Dental bone grafting is a procedure used to restore or preserve jawbone lost due to tooth extraction, gum disease, trauma, or congenital conditions. Adequate bone is essential for the stability of dental implants and the maintenance of facial structure. Different grafting techniques, such as block grafts, sinus lifts, and socket preservation, are chosen based on the location and severity of bone loss. The procedure involves careful assessment, placement of graft material, and a healing period of several months before further treatment. While generally safe, bone grafting carries minor risks and varying costs depending on complexity, but it plays a key role in improving implant success and long-term oral health.
1. What is a dental bone grafting procedure?
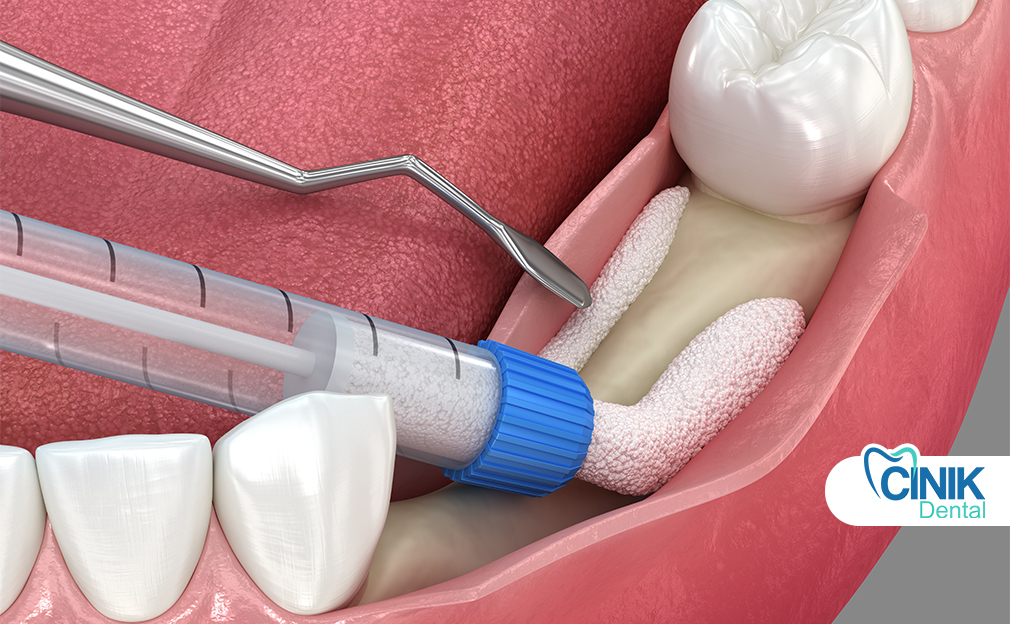
Quick Answer: Dental bone grafting is a surgical procedure that restores or preserves jawbone to support dental implants and maintain oral structure after tooth loss, disease, or injury.
Dental bone grafting is a surgical procedure carried out to repair damaged bone. An example of its application is in dentistry when a tooth has fallen out, which, if untreated, may lead to jaw bone loss, making the installation of an implant difficult (R. Megalaa, 2018). As defined by the American Academy of Periodontology, the goal of dental bone grafting is to augment, preserve, or regenerate the bone around a tooth and lengthen the clinical crown of a tooth.
Sufficient jaw bone is indispensable to ensure that implants are stable and capable of functioning like natural teeth. When a tooth falls out, it is probable that bone loss will occur over time. Dental bone grafting aims to ensure that sufficient bone is still present to allow the installation of an implant after a tooth has fallen out. Bone loss is continuous throughout life, and grafting is a preventative measure that maintains bone volume for future dental requirements. Other reasons for dental bone grafting are to repair damage from trauma or accidents, congenital bone loss or growth disorders, or severe periodontal disease causing loss of both bone and teeth.
2. What are the types of dental bone grafts?
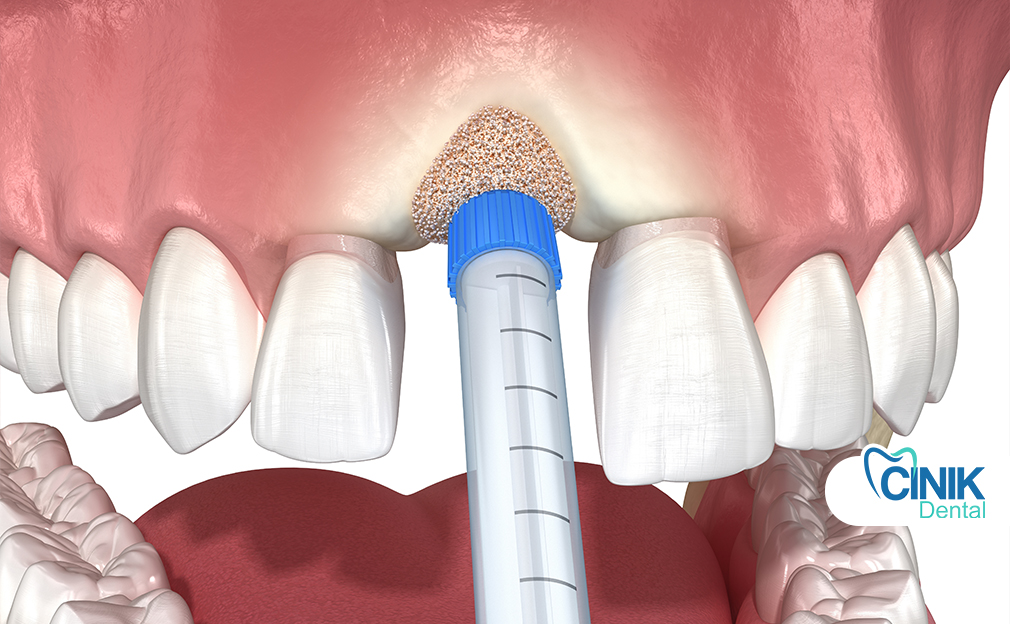
Quick Answer: The main types of dental bone grafts are block bone grafting for severe bone loss, sinus augmentation to increase bone height in the upper jaw, and socket preservation to prevent bone shrinkage after tooth extraction.
Block Bone Grafting
This technique uses a solid section of bone harvested from another area of the jaw to rebuild regions with advanced bone deficiency. It is especially useful in areas where bone volume has significantly diminished and where strong structural support is required before further dental treatment.
Sinus Augmentation
Sinus augmentation is used when the upper jaw lacks sufficient bone height due to sinus expansion following tooth loss. The procedure gently lifts the sinus membrane and adds bone beneath it, creating a stable foundation for future restorations.
Socket Preservation Graft
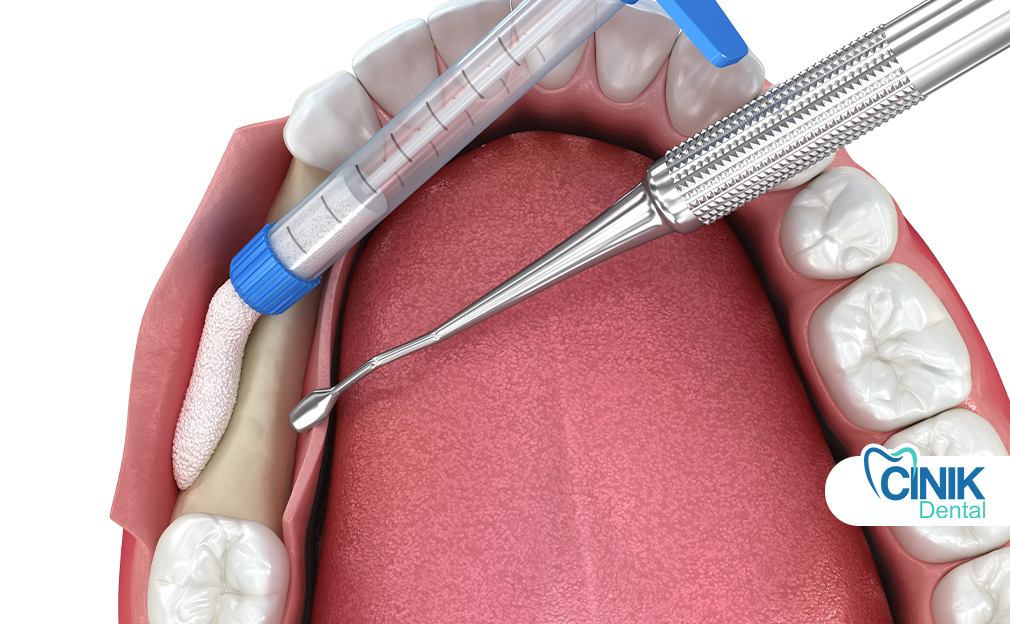
Socket preservation is performed immediately after a tooth is removed to minimize bone shrinkage. By placing grafting material into the empty socket, the natural shape of the jaw is maintained, supporting healthier bone levels for later dental procedures.
3. What are the reasons a dental bone graft may be necessary?
Quick Answer: A dental bone graft is needed to restore lost bone, support implants, maintain facial structure, or repair damage from trauma or congenital conditions.
When a tooth is extracted, the bone surrounding it may deteriorate. The neighboring teeth could drift into the gap. Over time, the surrounding facial bones may collapse, creating changes in the facial profile. An implant is stable only when surrounded by adequate bone. A bone graft fills in where bone has been lost, restoring contours and improving the success of the implant with better aesthetics. A bone graft may also be needed to repair damage from trauma or congenital absorption conditions (R. Megalaa, 2018).
4. How a dental bone graft is carried out
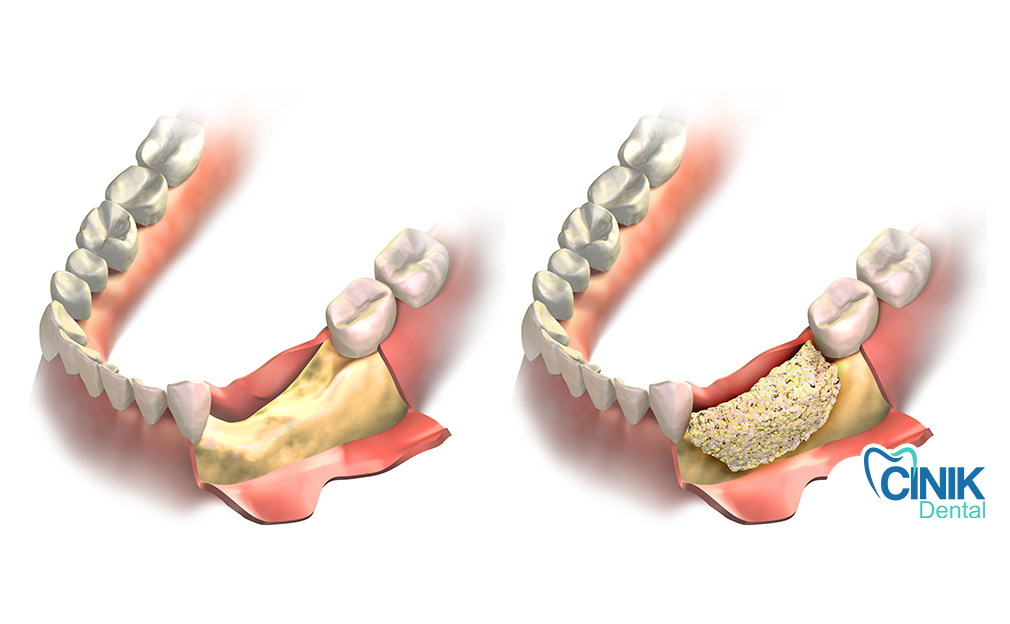
Quick Answer: A dental bone graft involves placing graft material into the jawbone after clinical evaluation to restore lost bone and support healing.
Before the graft can be placed, several prior steps are necessary. The process begins with a thorough dental assessment. The clinician evaluates the patient’s medical history, current medication, and the extent of existing dental work. Preoperative imaging studies demonstrate the condition of the graft site and adjacent structures. Common modalities include standard periapical and panoramic radiographs, cone-beam computed tomography (CBCT), and computerized tomography (CT). The clinician also determines the most appropriate approach for grafting.
During the procedure, the dentist typically administers local anesthetic. A surgical flap exposes the graft site in either the maxilla or mandible. An appropriately sized amount of the grafting material is shaped and placed into the graft site, and the flap is positioned to cover the graft. Certain situations may require the use of devices, such as screws, plates, or membranes, for stabilization. In extensive cases, specialists such as an oral surgery team may be consulted (R. Megalaa, 2018).
5. What is the healing process and post-procedure care?
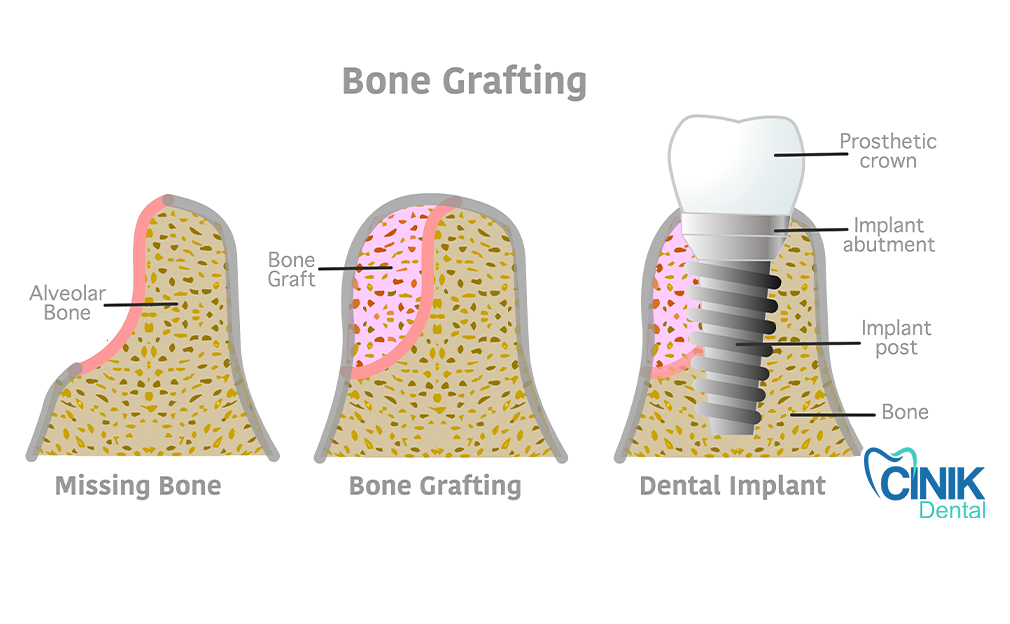
Quick Answer: Healing after a dental bone graft varies by graft type and patient factors, but typically takes several months before implant placement. Post-procedure care includes managing swelling, attending follow-up visits, using prescribed pain relief, maintaining gentle oral hygiene, and monitoring for signs of complications.
The healing and integration of a bone graft varies according to the type of graft used and the characteristics of the tissue where it is placed. Healing timelines are influenced by factors such as bone type, density, volume, and vascularity of the recipient site; metabolic state and age of the patient; occlusal support; systemic diseases (such as diabetes); and associated medications (such as antiresorptive drugs, bisphosphonate drug therapy, or antihypertensives) (R. Megalaa, 2018).
After placement of a bone graft, the healing process requires at least 4 months before an implant can be installed in the grafted area. Nevertheless, stable bone filling is often achieved before this period, as it depends on the type of graft or biomaterial used, the osseointegration process, and the surrounding bone characteristics. In cases with insufficient occlusal support or if an implant needs to be installed, it is advisable to wait 3-6 months before placing the implant.
Initial patient follow-ups are generally scheduled for 1 week and then again after 3 weeks. After that, the duration between follow-ups can vary between 3 and 6 months, depending on the scheduled treatment (Adrian Raţiu et al., 2020). For socket preservation, ridge augmentation, and lateral sinus lift procedures, preoperative and postoperative radiographs are recommended to further assess the healing process.
After the procedure, swelling is frequent on the operated area, lasting 2 to 3 days. A follow-up appointment can be scheduled for 7 days post-surgery to assess swelling and the need for analgesics; if no stitches are involved, an additional appointment is unnecessary. Only one week is considered sufficient for normal postoperative follow-up. Regarding analgesics, paracetamol and most anti-inflammatories are usually prescribed, avoiding narcotics that could lead to dependency or constipation. It is advisable to elevate the head with pillows during the first nights to limit swelling and facilitate drainage.
In the case of a block graft, a special restriction on mouth opening can also be indicated. In the event of persistent swelling or bleeding on the days following surgery, the patient should be instructed to contact the dental professional. To diminish the risk of peri-implantitis or further complications, a breath spray and mouthwash without alcohol, dyes, or flavors may be recommended, together with brushing and disinfection with a soft toothbrush or a water flosser, daily for a few minutes.
6. What are the possible risks and side effects?
Quick Answer: Risks of dental bone grafting include infection, swelling, bleeding, delayed healing, and rare nerve or sinus complications.
Dental bone grafting carries several possible risks and side effects, although serious complications are uncommon. Many of the associated risks apply to the harvesting of graft material, which may be performed from the upper or lower jaw. Improper technique can lead to injury of the nerves and blood vessels near the harvesting site (Bayram et al., 2024). Likewise, graft exposure, significant bleeding, swelling, and prolonged healing time represent common but manageable issues when the graft tissue is artificially produced or acquired from another person (Titsinides et al., 2019). The occurrence of these risks can be minimized by thoroughly discussing the procedure and clarifying any doubts during the preparatory consultation.
Infection around the graft site remains the main risk, irrespective of the graft’s origin. Non-absorbable sutures used during the procedure can act as a surface for bacterial growth and facilitate the development of peri-graft infections. Other potential complications include blockage of the sinus cavity, unexpected resorption of graft material, and displacement of graft into the sinus after the procedure (R. Megalaa, 2018). Patients are encouraged to seek immediate medical attention if they detect any abnormal signs, such as excessive swelling, bleeding, or discharge of pus from the graft site. Following the dentist’s advice on medication, oral care, chewing, and general activity also contributes significantly to minimizing any complications.
7. What is the cost of dental bone grafting?
Quick Answer: The cost of dental bone grafting varies based on the graft material used, procedure complexity, type of anesthesia, and required follow-up care.
The price of dental bone grafting depends on a number of factors. Bone grafting materials, the dentist’s technique, and the care following the procedure all impact the total cost (R. Megalaa, 2018).
1. Material. The material selected for the graft influences price. Anesthetics and additional materials can also be needed.
2. Procedure. Bone grafting creates new bone in specific sites in the mouth, and the area requiring treatment impacts the cost. Bone grafting is used during maxillary sinus lifts, guided bone regeneration in the anterior mandible, horizontal ridge augmentations, and vertical ridge augmentations. Fracture stabilization and ridge preservation after tooth removal are other applications. Complex grafting approaches take longer and increase expenses. Dozy patient cooperation prolongs grafting time.
3. Anesthesia. Anesthesia type, whether local or general, modifies the bill. Local anesthesia is simpler, faster, and less costly than general anesthesia. Accompanying procedures like tooth extraction that add time, materials, or anesthesia increase expenses. Other preparatory treatments that influence total grafting price can include cone beam computed tomography scans and preparation for oral bacterial contamination.
4. Follow-up care. Post-treatment assessments after a maximal number of weeks and months require further investment.
8. Who needs a dental bone graft
Quick Answer: A dental bone graft is needed for patients with bone loss who require implants, bone preservation after extraction, or jaw repair due to injury or disease.
A dental bone graft may be needed to prevent, remedy, or reconstruct bone loss in specific areas of the mouth. One common group of candidates are those who seek dental implants but lack sufficient bone mass or quality in the implant site. If a tooth is lost and a dental implant is not placed immediately thereafter, an additional procedure called ridge preservation may be required to maintain the underlying bone volume. This technique is especially important if the missing tooth is located in the upper front area of the mouth and is critical for both functional and esthetic reasons. Finally, individuals with previous trauma or injury to the jaw, or with congenital bone defects caused by conditions such as ectodermal dysplasia, may need bone augmentation to restore normal anatomy and function.
Dental bone grafting is not only performed in these well-defined situations. A dental bone graft may also be indicated as a preventive measure. For instance, it may be planned to augment the alveolar ridge of a patient undergoing extraction of a periodontally-involved tooth. Since the dimensions of the bone overlying the maxillary sinuses tend to diminish in height after loss of a molar in this region, a bone graft to the floor of the maxillary sinus may be performed to provide sufficient bone volume for dental implants after healing.
9. Conclusion
A dental bone graft helps restore bone tissue damaged by tooth loss, disease, trauma, or congenital conditions. After analysis, the dentist creates a plan to rebuild lost bone. Grafting aims to facilitate a dental implant (R. Megalaa, 2018) or preserve bone shape after an extraction. Bone grafts stabilize implants, restore smile aesthetics, and provide necessary support after injury or disease.
References:
R. Megalaa, A. "Bone grafting and its effect on stablilty of the jaw on extraction patients: a systematic review." 2018. [PDF]
Titsinides, S., Agrogiannis, G., and Karatzas, T. "Bone grafting materials in dentoalveolar reconstruction: A comprehensive review()." 2019. ncbi.nlm.nih.gov
Adrian Raţiu, C., Adela Raţiu, I., Cavalu, S., Bianca Boşca, A., and Ciavoi, G. "Successful management of spontaneous bone regeneration after jaws cystectomy using PRGF approach; case series." 2020. ncbi.nlm.nih.gov
Bayram, F., Göçmen, G., and Özkan, Y. "Evaluating risk factors and complications in mandibular ramus block grafting: a retrospective cohort study." 2024. ncbi.nlm.nih.gov