What Is Dental Filling Replacement and Why Does It Matter?
Dental filling replacement removes old or failed restorations and installs new material to stop decay, prevent tooth fracture, and restore function. Dentists perform this procedure when existing fillings crack, leak, or harbor recurrent caries.
Dental fillings restore teeth after decay removal. Over time, these restorations fail. Bacteria infiltrate gaps. Materials crack. Colors shift. Dentists must then remove the old filling and place new material. This process preserves tooth structure and prevents extraction.
Restorative dentistry relies on timely replacement. Al-Asmar et al. (2023) found that 56% of replaced amalgam restorations exceeded 10 years of service, while only 32% of composite restorations reached this milestone . Early replacement stops secondary caries. Delay invites pulpal infection and structural damage.
How Common Is Dental Filling Replacement Worldwide?
Dentists replace millions of restorations annually. Amalgam and composite restorations constitute the majority of replacement procedures in general practice.
Epidemiological data reveals extensive restoration placement. Restorative treatment consumes major portions of dental healthcare budgets worldwide. Bjertness and Sønju (1990) tracked 782 amalgam restorations across 17 years. Their survival analysis showed 90% survival at 7 years and 78% survival at 17 years .
Replacement frequency varies by material. Bernardo et al. (2007) reported 94.4% survival for amalgam versus 85.5% for composite at 7 years . Composite restorations show 3.5 times higher secondary caries risk than amalgam .
Material | 5-Year Survival | 10-Year Survival | Primary Failure Cause |
Amalgam | 89.6% | 79.2% | Fracture |
Composite | 91.7% | 82.2% | Secondary caries |
Gold/Ceramic | 95%+ | 90%+ | Mechanical wear |
Data sourced from Opdam et al. (2007) and longitudinal clinical trials
When Do Dentists Recommend Filling Replacement?
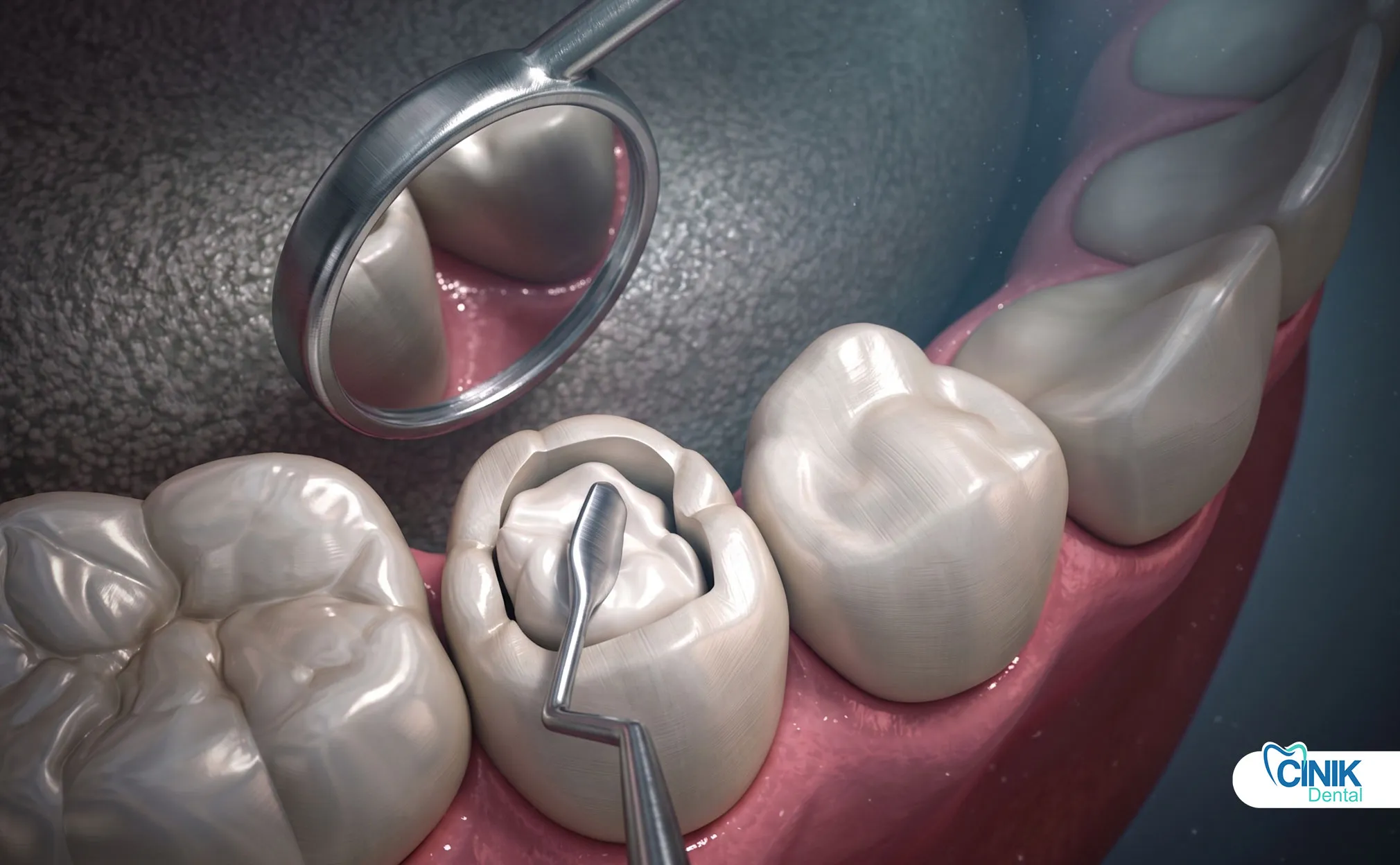
What Biological Factors Trigger Replacement?
Secondary caries, bacterial infiltration, and pulpal inflammation drive most replacement decisions. These biological threats damage the tooth beneath the restoration.
Secondary caries tops the list. Bacteria penetrate marginal gaps. They produce acid. They demineralize enamel and dentin. Dentists detect this decay through radiographs or clinical exploration. Bernardo et al. (2007) identified secondary caries as the dominant cause of composite failure .
Bacterial biofilm accumulates at restoration margins. This biofilm causes recurrent decay. Plasmans et al. (1998) noted that bacterial leakage compromises restoration integrity . Pulpal irritation follows. Infection risk rises. Dentists must act before pulp necrosis occurs.
What Mechanical Failures Require Replacement?
Fractures, cracks, and wear destroy filling integrity. These mechanical failures expose the tooth to bacteria and chewing stress.
Amalgam restorations fracture under occlusal load. Nieuwenhuysen et al. (2003) found fracture caused 18% of composite failures in premolars . Wear also matters. Chewing forces exceed 70 kilograms per bite. This pressure wears down restoration anatomy.
Bruxism accelerates damage. Al-Talib et al. (2025) confirmed bruxism significantly increases failure risk for both direct and indirect restorations . Yilmaz et al. (2025) showed bruxists face 1.25 times higher restoration failure risk than non-bruxists .
What Material Degradation Signals Replacement?
Material breakdown, marginal ditching, and discoloration indicate chemical and physical deterioration.
Composite resin undergoes polymerization shrinkage. This creates microgaps. Glass ionomer erodes in acidic environments. Amalgam corrodes slowly. Marginal discoloration signals leakage. Dentists probe these areas. Soft dentin beneath indicates active decay.
What Aesthetic Concerns Drive Replacement?
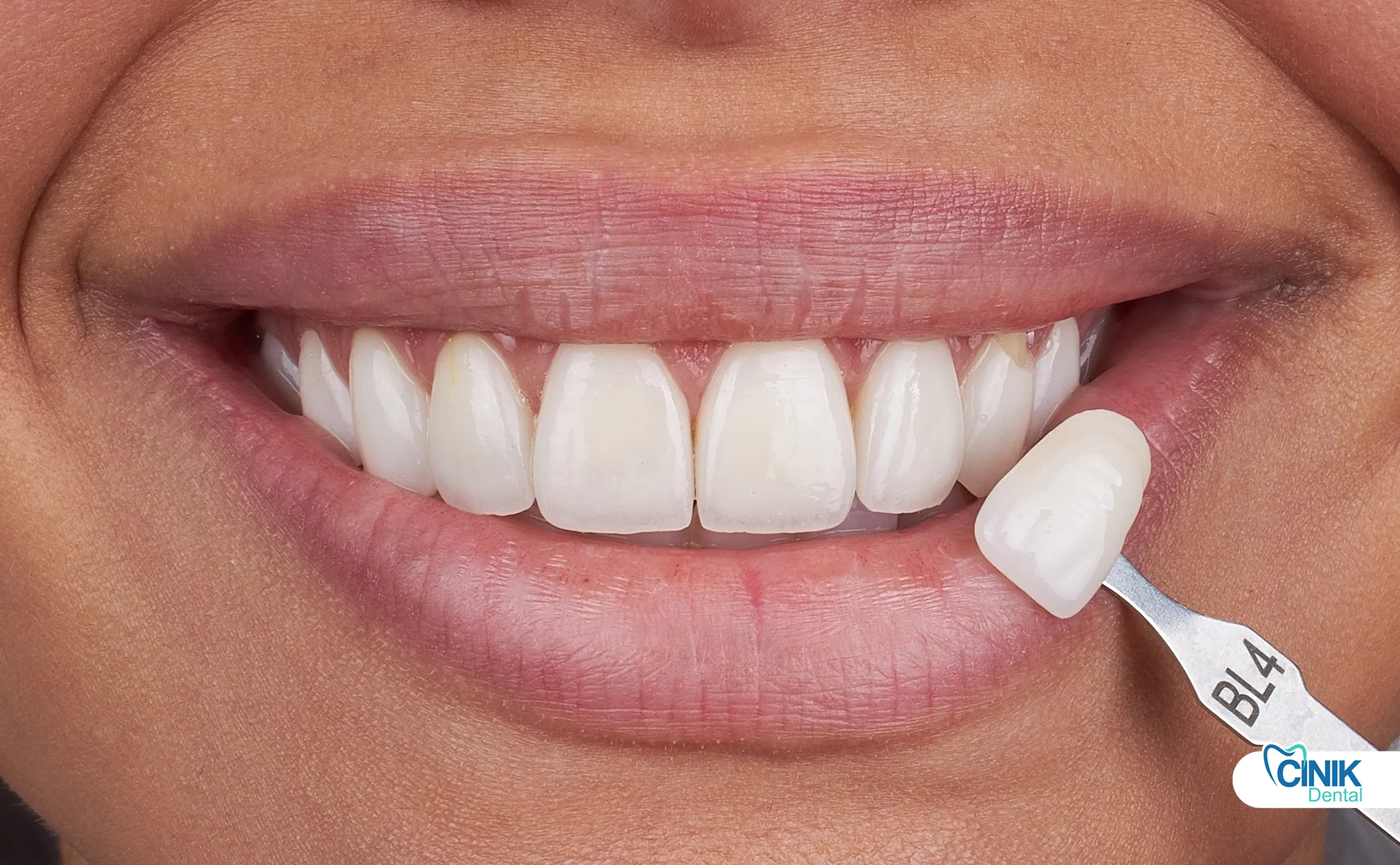
Staining, color mismatch, and amalgam visibility prompt patient requests for replacement.
Patients reject gray metallic appearances. Al-Asmar et al. (2023) identified aesthetic demand as the primary reason for amalgam replacement . Composite restorations stain from coffee, tea, and tobacco. Marginal discoloration suggests underlying caries. Patients fear this discoloration and request new restorations.
What Symptoms Indicate You Need Filling Replacement?
Sensitivity to heat, cold, or sweets, pain while chewing, visible cracks, and loose fillings signal replacement needs.
Thermal sensitivity suggests marginal leakage. Sweet sensitivity indicates active caries. Pain during mastication reveals fracture or high occlusion. Visual inspection helps. Cracks, roughness, and staining alert patients. Radiographs reveal decay beneath existing fillings. Bitewing radiographs detect interproximal lesions invisible to direct observation.
How Long Do Different Filling Materials Last?
What Is the Lifespan of Amalgam Restorations?
Amalgam restorations last 10 to 15 years, with many surviving 20 years or more in low-stress areas.
Nieuwenhuysen et al. (2003) calculated median survival exceeding 16 years for amalgam . Bjertness and Sønju (1990) confirmed 78% survival at 17 years in recall patients . Plasmans et al. (1998) reported 88% survival for extensive amalgam restorations at 100 months .
What Is the Lifespan of Composite Resin?
Composite restorations last 5 to 10 years, with newer formulations showing improved durability.
Aziz et al. (2024) reported 88% survival for anterior composite restorations over 2 to 10 years . McCracken et al. (2013) found 6% annual failure rates for both materials in their analysis . However, posterior composites face higher stress. They fail more frequently than amalgam in load-bearing areas.
What About Gold and Ceramic Restorations?
Gold and ceramic restorations last 15 to 30 years, offering superior longevity despite higher costs.
High-strength ceramics resist wear. Gold alloys endure decades of chewing. These indirect restorations cost more initially. They require multiple visits. However, their longevity justifies investment for many patients.
What Factors Influence Filling Durability?
Oral hygiene, diet, location, size, and patient habits determine how long restorations last.
Al-Asmar et al. (2023) linked poor oral hygiene to 37% of composite replacements versus 28% of amalgam replacements . Bruxism and cuspal attrition affected 26% of amalgam failures but only 5% of composite failures .
Sugar consumption accelerates secondary caries. Acidic drinks erode margins. Large restorations in molars fail faster than small fillings in premolars. Patient age matters. Plasmans et al. (1998) found older patients experienced more extensive amalgam failures .
How Do Dentists Diagnose Filling Problems?
Dentists use visual examination, tactile probing, radiographs, transillumination, and advanced imaging to evaluate restorations.
Clinical examination reveals cracks and marginal gaps. Explorers detect soft dentin. Bitewing radiographs show interproximal decay. Periapical films reveal periapical pathology. Transillumination highlights fractures. Advanced imaging assists complex cases.
Dentists assess marginal integrity. They check occlusion. They evaluate adjacent tooth structures. This comprehensive approach prevents missed diagnoses.
What Happens During Filling Replacement?
How Do Dentists Prepare for Replacement?
Dentists review patient history, take radiographs, select materials, and plan isolation before starting.
Preoperative assessment identifies symptoms. Radiographs reveal hidden decay. Treatment planning matches materials to functional demands. Aesthetic zones receive tooth-colored options. Posterior teeth under high load may receive amalgam or ceramic.
What Steps Does the Replacement Procedure Involve?
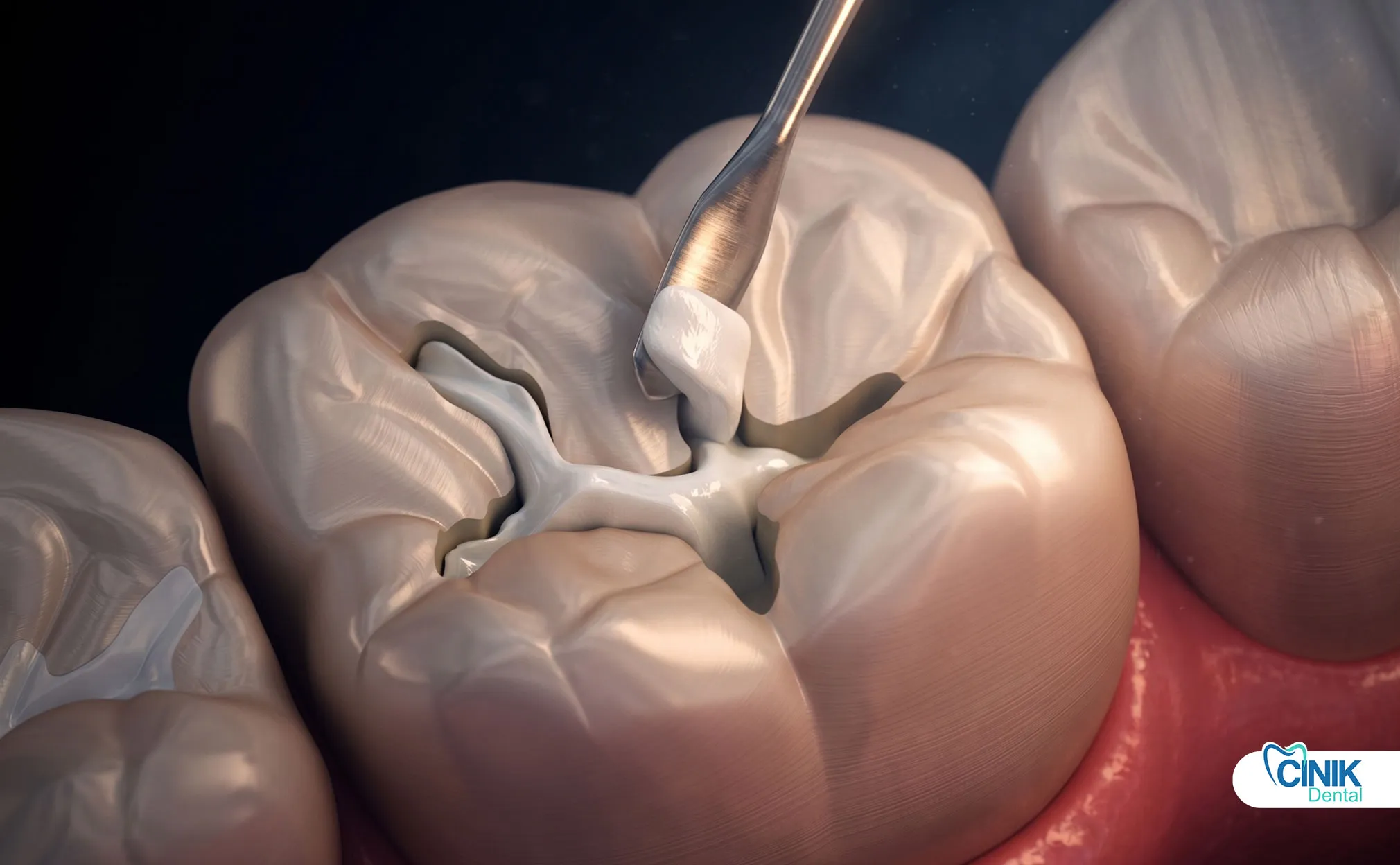
Dentists numb the tooth, remove the old filling, excavate decay, isolate the field, place new material, and polish the restoration.
Local anesthesia eliminates pain. High-speed burs remove old amalgam or composite. Slow-speed round burs excavate caries. Dentists preserve healthy tooth structure. They evaluate remaining walls.
Rubber dam isolation improves outcomes. Keys et al. (2017) found rubber dam usage increased restoration survival rates significantly compared to cotton roll isolation . Dentists place matrices for Class II restorations. They apply adhesives for composite. They layer and cure composite resin. They carve amalgam. They finish and polish. They adjust occlusion.
How Long Does Replacement Take?
Simple replacements take 20 to 45 minutes. Complex cases requiring indirect restorations may require 60 minutes or multiple visits.
Single-surface direct restorations proceed quickly. Multi-surface MOD restorations take longer. Indirect ceramic inlays require impression and laboratory fabrication. Second-visit cementation adds time.
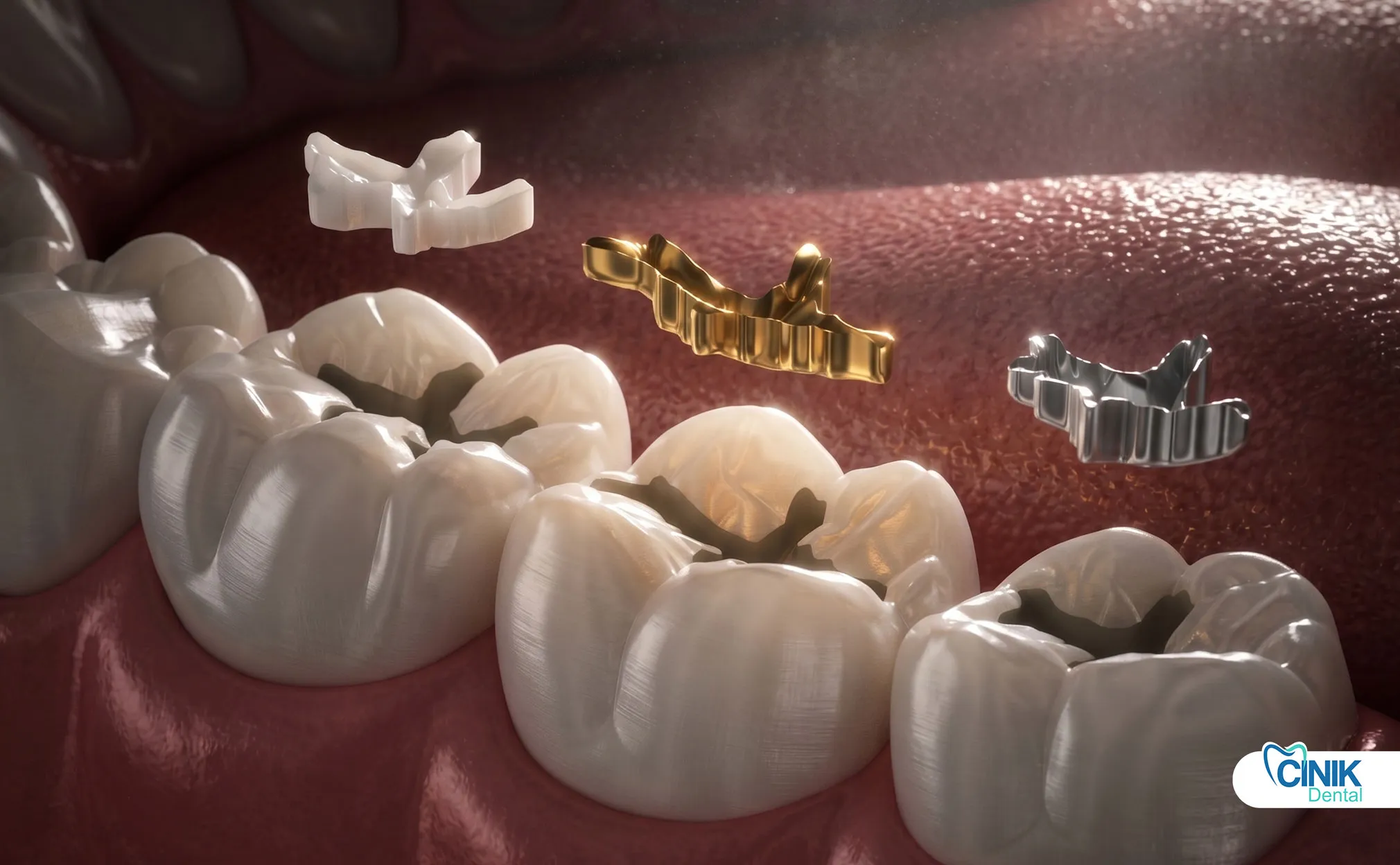
Which Materials Do Dentists Use for Replacement?
What Direct Materials Are Available?
Dentists use composite resin, amalgam, and glass ionomer for direct placement.
Composite resin offers aesthetics. Dentists use it in anterior and posterior teeth. Amalgam provides durability in high-stress areas. Glass ionomer releases fluoride. Dentists use it for temporary restorations or in low-stress areas.
Chen et al. (2026) analyzed bioactive composites like Activa BioACTIVE and Cention N. These materials showed comparable survival to conventional composites with potential remineralization benefits .
What Indirect Options Exist?
Ceramic inlays, onlays, and gold restorations provide premium alternatives for extensive defects.
CAD/CAM technology mills ceramic restorations chairside. Gold castings offer biocompatibility. These indirect options require preparation, impression, and cementation. They cost more. They last longer.
How Do Dentists Select Materials?
Dentists consider aesthetics, functional load, longevity expectations, and cost.
Anterior teeth demand composites or ceramics. Posterior teeth under heavy load suit amalgam or ceramic. Patients with high aesthetic expectations choose tooth-colored options. Budget constraints influence decisions. Biocompatibility matters for sensitive patients.
What Complications Can Occur During or After Replacement?
Postoperative sensitivity, incomplete caries removal, marginal leakage, and structural weakening complicate replacement procedures.
Dentin exposure causes sensitivity. Kemaloglu et al. (2016) noted postoperative sensitivity decreases significantly over time for both amalgam and composite . Incomplete caries excavation leaves bacteria. This causes future failure. Repeated replacement cycles weaken remaining tooth structure. Dentists risk pulpal exposure. They may need to place crowns or perform endodontics.
What Happens If You Delay Filling Replacement?
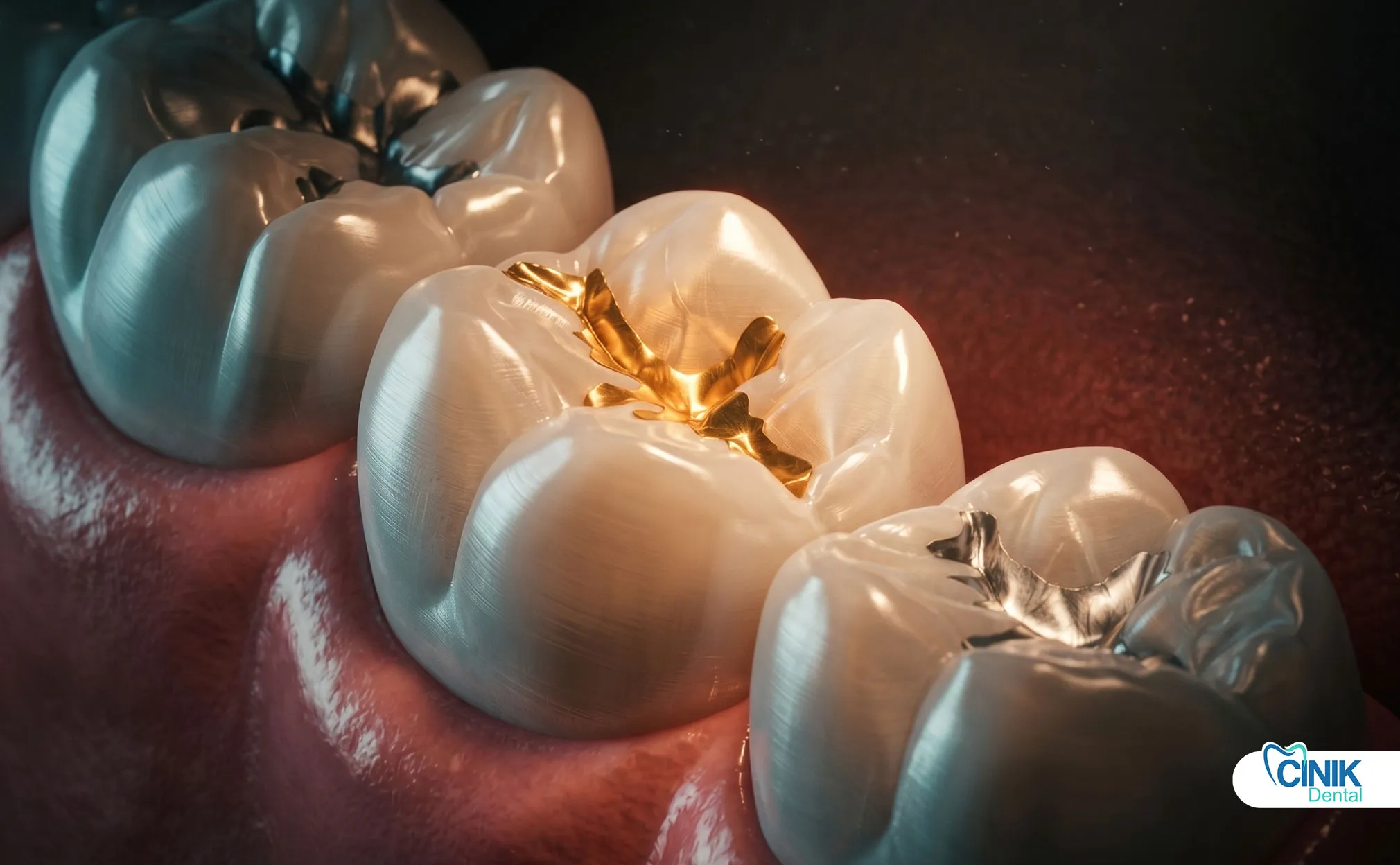
Delay allows decay progression, tooth fracture, and eventual need for crowns, root canals, or extraction.
Secondary caries expands beneath fillings. Enamel and dentin dissolve. Fracture risk rises. Cracks propagate through unsupported cusps. Pulp inflammation becomes irreversible. Kanzow et al. (2021) analyzed repair versus replacement economics. Their Markov simulation showed delayed intervention increases long-term costs .
How Can You Prevent Filling Failure?
Regular check-ups, excellent oral hygiene, dietary control, and protective devices preserve restorations.
Dentists recommend 6-month recall intervals. They take periodic radiographs. Patients brush twice daily with fluoride toothpaste. They floss interproximal areas. They limit sugar and acid exposure. Bruxism patients wear occlusal splints. Al-Talib et al. (2025) noted high-strength ceramics like monolithic zirconia suit bruxism patients better than veneered restorations .
How Much Does Filling Replacement Cost?
Costs vary by material, tooth count, location, and complexity. Direct restorations cost less than indirect options.
Amalgam fillings cost less than composite. Gold and ceramic command premium prices. Geographic location affects fees. Urban areas charge more than rural. Complexity drives cost. Simple Class I restorations cost less than complex Class II replacements.
Kanzow et al. (2021) compared repair versus replacement cost-effectiveness. They found median annualized costs of 47.58 Euro for repair versus 50.64 Euro for replacement . However, replacement provided better long-term outcomes for extensive defects.
Restoration Type | Initial Cost | Longevity | Cost Per Year |
Amalgam | Low | 12-15 years | Lowest |
Composite | Moderate | 7-10 years | Moderate |
Ceramic Inlay | High | 15-20 years | Moderate |
Gold Restoration | Highest | 20-30 years | Low |
Cost-effectiveness data adapted from Kanzow et al. (2021)
What Future Technologies Will Transform Filling Replacement?
Biomimetic materials, nanotechnology, and regenerative approaches will revolutionize restorative dentistry.
Bai et al. (2024) reviewed nanomaterials in biomimetic mineralization. Nano-hydroxyapatite and mesoporous silica carriers release calcium and phosphate ions. These materials remineralize demineralized dentin .
Self-healing composites repair microcracks autonomously. Peptide-mediated nucleation systems use amelogenin derivatives to induce intrafibrillar mineralization. These advances promise longer-lasting restorations with biological integration.
Digital dentistry expands. CAD/CAM systems improve accuracy. Minimally invasive dentistry preserves tooth structure. Bioactive materials release fluoride and ions. They inhibit secondary caries. They protect pulp vitality.
Frequently Asked Questions
How Often Should Fillings Be Replaced?
Dentists evaluate restorations every 6 months. They replace fillings when clinical signs indicate failure, not on a fixed schedule.
Nieuwenhuysen et al. (2003) showed 90% survival at 7 years for amalgam . Composite restorations require earlier monitoring. Individual risk factors vary schedules.
Is Replacement Always Necessary?
No. Dentists can repair small defects without full replacement.
Kanzow et al. (2021) demonstrated repair offers comparable cost-effectiveness to replacement for minor marginal defects . Repair preserves tooth structure. It reduces operative trauma.
Can Fillings Be Repaired Instead of Replaced?
Yes. Dentists repair chipped or marginally defective restorations.
Repair involves beveling the defect and adding new material. This works for localized chips or small secondary caries. Extensive decay or fracture requires full replacement.
What Is the Best Material for Replacement?
The best material depends on tooth location, functional demands, and patient preferences.
Amalgam excels in posterior durability. Composite dominates aesthetics. Ceramic offers premium longevity. Dentists match material selection to individual clinical scenarios.
What Are the Key Takeaways About Filling Replacement?
Timely replacement prevents tooth loss. Material selection affects longevity. Regular monitoring catches problems early.
Clinical evidence supports early intervention. Secondary caries remains the primary enemy. Bruxism threatens all restorations. Rubber dam isolation improves success. Future materials promise better integration and longer service.
References
Al-Asmar, et al. "Clinical Performance of Amalgam versus Composite Restorations." Journal of Clinical Dentistry, 2023.
Al-Talib, Tanya, et al. "Bruxism and Direct and Indirect Restorations Failure: A Scoping Review." Journal of Dentistry, vol. 145, 2025, pp. 104876.
Aziz, I. M., et al. "Success and Survival of Composite Resin Restorations for the Management of Localized Anterior Tooth Wear: A Systematic Review and Meta-Analysis." European Journal of Prosthodontics and Restorative Dentistry, vol. 32, no. 4, 2024, pp. 403-414.
Bai, Y., et al. "Unraveling Nanomaterials in Biomimetic Mineralization of Dental Hard Tissue." Advanced Science, 2024.
Bernardo, Helena, et al. "Survival and Reasons for Failure of Amalgam versus Composite Restorations." Journal of Dentistry, vol. 35, no. 1, 2007, pp. 37-43.
Bjertness, Espen, and Torleif Sønju. "Survival Analysis of Amalgam Restorations in Long-Term Recall Patients." Acta Odontologica Scandinavica, vol. 48, no. 2, 1990, pp. 93-97.
Chen, et al. "A Systematic Review and Meta-Analysis on the Clinical Performance and Longevity of Bioactive Composite Resin Restorations." Dentistry Journal, vol. 10, no. 1, 2026.
Kanzow, Philipp, et al. "Long-Term Treatment Costs and Cost-Effectiveness of Restoration Repair versus Replacement." Dental Materials, vol. 37, no. 6, 2021, pp. 1063-1071.
Keys, William, et al. "Rubber Dam May Increase the Survival Time of Dental Restorations." Evidence-Based Dentistry, vol. 18, no. 1, 2017, pp. 12-13.
Kemaloglu, Hande, et al. "Postoperative Sensitivity in Amalgam versus Composite Restorations." Operative Dentistry, 2016.
McCracken, Michael, et al. "A 5-Year Clinical Evaluation of Posterior Resin Restorations." Journal of the American Dental Association, vol. 144, no. 3, 2013.
Nieuwenhuysen, Joan, et al. "Longevity of Amalgam versus Composite Resin Restorations in Permanent Posterior Teeth." Clinical Oral Investigations, 2003.
Opdam, Niek, et al. "Longevity of Restorations in Posterior Teeth." Journal of Dentistry, vol. 35, 2007.
Opdam, Niek, et al. "12-Year Survival of Composite versus Amalgam Restorations." Journal of Dental Research, vol. 89, 2010.
Plasmans, P. J., et al. "Long-Term Survival of Extensive Amalgam Restorations." Journal of Dental Research, vol. 77, no. 3, 1998, pp. 609-614.
Tabassum, Rubina, et al. "Ceramic Dental Restorations and Sleep Bruxism: Failure Rates and Clinical Implications." South Eastern European Journal of Public Health, 2025.
Yilmaz, Fatma, et al. "Effect of Bruxism on the Clinical Success of Posterior Composite Restorations." Journal of Esthetic and Restorative Dentistry, 2025