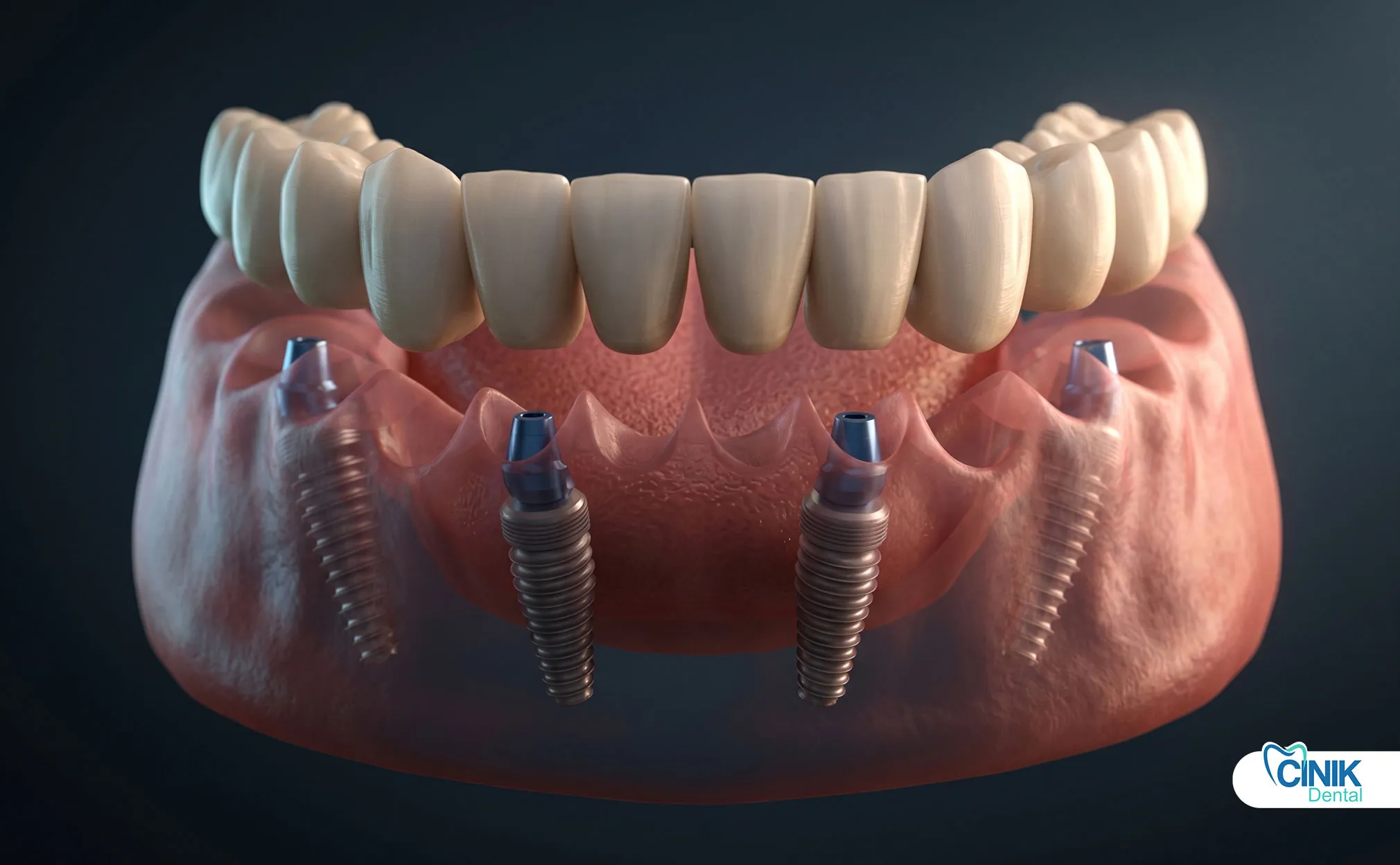
Dental implants offer superior long-term function, bone preservation, and durability. Removable dentures provide a lower-cost, non-surgical alternative. The best choice depends on your bone health, budget, and personal priorities. This article explains the clinical evidence behind both options.
What Is Edentulism and Why Does Tooth Loss Matter?
Edentulism means complete tooth loss. It reduces chewing power, alters speech, shrinks jawbone volume, and lowers quality of life.
Edentulism describes the condition of having no natural teeth in one or both jaws. Partial edentulism refers to the loss of some teeth. Both conditions affect millions of adults worldwide. Tooth loss directly impacts masticatory function. Patients with missing teeth cannot chew food effectively. This limitation reduces nutritional intake and digestive health.
Tooth loss also alters facial aesthetics. The jawbone needs daily mechanical stimulation from tooth roots. Without this stimulation, the bone undergoes resorption. The face loses vertical dimension. The chin moves closer to the nose. Lips appear sunken. These changes make patients look older than their actual age.
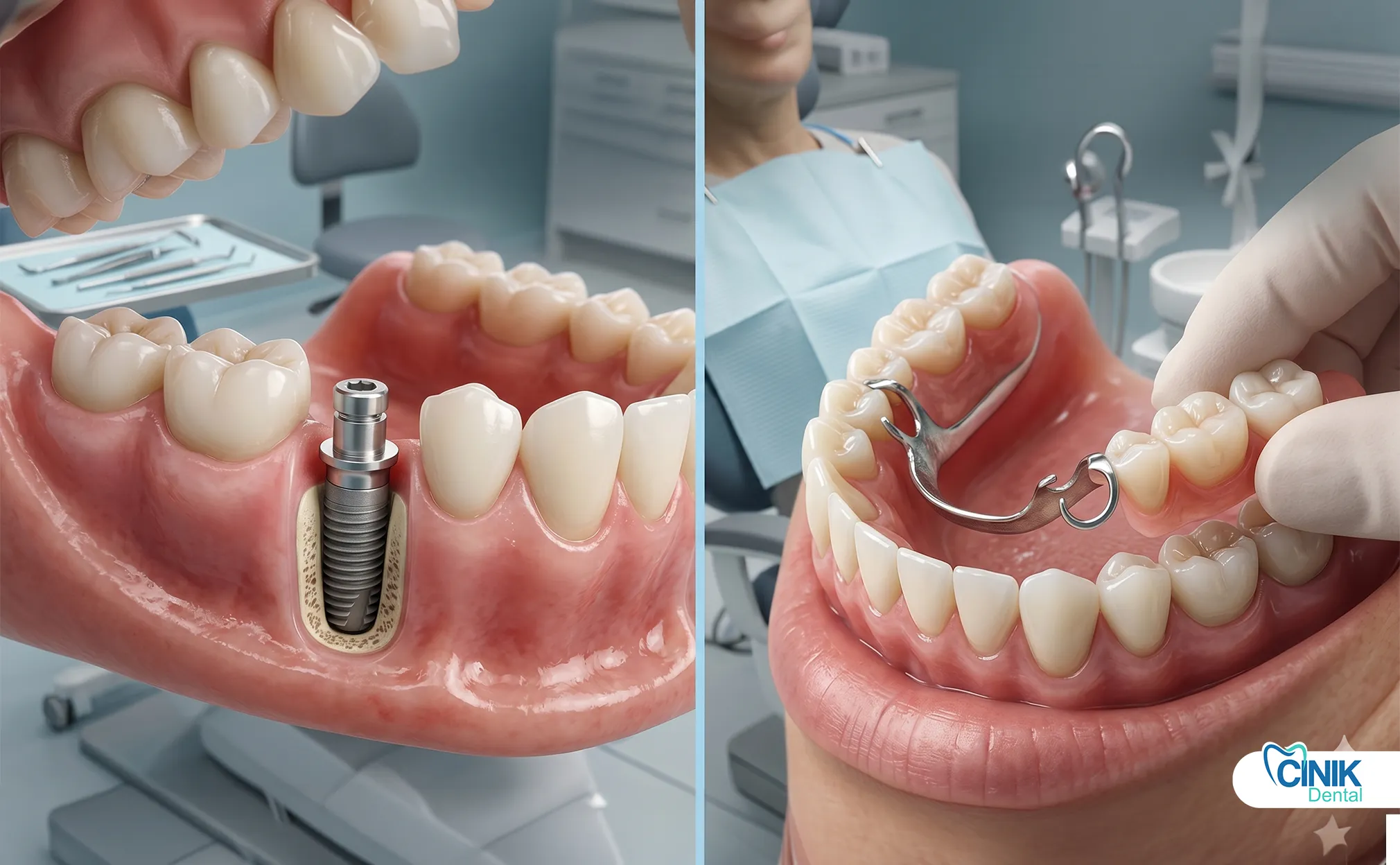
Modern prosthodontics offers two primary solutions. Dental implants replace tooth roots with titanium fixtures. Removable dentures replace the visible crowns but rest on soft tissue. Both options restore appearance. However, they differ drastically in function, longevity, and biological impact. Clinicians must evaluate each patient individually. No single treatment fits every case.
What Are Dental Implants and How Do They Work?
Dental implants are titanium posts that surgeons place into the jawbone. The bone fuses with the implant through osseointegration. This fusion creates a permanent anchor for artificial teeth.
What Makes Up a Dental Implant?
A dental implant has three parts: a titanium screw, an abutment, and a prosthetic crown.
The titanium screw acts as an artificial root. Titanium ranks as the material of choice because it integrates with living bone. Branemark and his team discovered this phenomenon in the 1960s. They named it osseointegration (Branemark 1977). The abutment connects the screw to the crown. The crown replicates the visible tooth. Modern crowns use zirconia or layered porcelain. These materials mimic natural enamel color and light reflection.
What Types of Dental Implants Can Patients Receive?
Patients can choose single-tooth implants, implant-supported bridges, or full-arch implants.
Single-tooth implants replace one missing tooth. The surgeon places one fixture and tops it with one crown. This approach preserves neighboring teeth. Unlike traditional bridges, it requires no grinding of adjacent healthy teeth.
Implant-supported bridges replace multiple teeth. The dentist places two or more implants. These implants support a bridge of connected crowns. This option suits patients who lack three or more teeth in a row.
Full-arch implants replace an entire jaw of teeth. The All-on-Four protocol uses four strategically angled implants to support a full fixed bridge. Nagni and colleagues confirmed high survival rates for this approach. Their retrospective study reported a 98.09% implant survival rate over six years (Nagni 2023). Some protocols use six implants for additional support.
Who Qualifies for Dental Implants?
Patients with adequate bone density, healthy gums, and stable general health qualify for implants.
The jawbone must measure enough width and height to house the implant. The bone also needs sufficient density. Soft, porous bone cannot anchor the fixture firmly. Patients with severe diabetes, uncontrolled hypertension, or heavy smoking habits face higher failure risks. However, age alone does not disqualify anyone. Many patients in their seventies and eighties receive implants successfully.
What Are Removable Dentures and How Do They Function?
Removable dentures are acrylic or resin bases that hold artificial teeth. Patients take them out for cleaning and sleep. They rely on suction, adhesives, or metal clasps for retention.
What Types of Removable Dentures Exist?
Complete dentures replace all teeth in one arch. Partial dentures replace some teeth and clasp onto remaining natural teeth.
Complete dentures rest on the gum ridge. The upper denture covers the entire palate. It creates suction against the roof of the mouth. The lower denture covers the horseshoe-shaped ridge. It relies more on gravity and adhesive paste because the tongue constantly displaces it.
Partial dentures fill gaps between existing teeth. A metal framework holds the acrylic base. Small metal clasps wrap around natural teeth for stability. Some modern versions use flexible nylon instead of metal. These flexible partials offer better aesthetics but provide less rigid support.
How Do Dentures Stay in Place?
Upper dentures use suction and saliva seal. Lower dentures need adhesives and muscle control. Partial dentures use metal clasps on adjacent teeth.
The upper jaw offers a broad surface area. The palate provides a seal. Saliva acts as a natural adhesive. This suction keeps the upper denture reasonably stable during normal speech. The lower jaw presents a bigger challenge. The tongue occupies significant space. The lower ridge absorbs less surface area. Patients often struggle with lower denture stability. Denture adhesives improve retention temporarily. However, adhesives cannot overcome poor fit or severe bone loss.
What Are the Core Differences Between Implants and Removable Dentures?
Implants anchor into bone and function like natural teeth. Dentures rest on gums and require daily removal. Implants demand surgery. Dentures need no surgery.
How Do Structure and Function Differ?
Implants replace roots and crowns. Dentures replace only crowns. Implants transfer bite force into bone. Dentures press on soft tissue.
Dental implants replicate the entire tooth structure. The titanium screw embeds into the jawbone. It transmits chewing forces directly to the bone. This stimulation preserves bone volume. Removable dentures sit on the mucosa. The gum tissue and underlying bone bear all pressure. This pressure accelerates bone resorption over time. Carlsson described this process in his research on jawbone responses to stress (Carlsson 2004).
Why Does One Require Surgery and the Other Does Not?
Implants need surgical placement into bone. Dentures need only impressions and fitting.
Implant treatment involves multiple surgical steps. The surgeon exposes the bone. He drills a precise osteotomy. He inserts the titanium fixture. He closes the gum tissue. The patient waits three to six months for osseointegration. Then the surgeon attaches the abutment. Finally, the dentist places the crown. Some protocols allow immediate loading. Sánchez-Torres and colleagues studied immediately loaded full-arch prostheses. Their cohort showed 100% implant survival over a mean follow-up of fifty-two months (Sánchez-Torres 2021). However, immediate loading requires excellent primary stability and strict patient selection.
Denture fabrication requires no incisions. The dentist takes alginate impressions. A dental lab casts models. Technicians set artificial teeth in wax bases. The dentist tries a wax version. After approval, the lab processes the final acrylic denture. The patient receives the denture in a single fitting appointment.
Which Option Provides Better Stability?
Implants provide rigid, immovable stability. Dentures shift during eating and speaking.
Osseointegration creates a biomechanical bond between metal and bone. This bond rivals the periodontal ligament of natural teeth. Patients can bite into apples. They can chew steak. They can speak without fear of slippage. Removable dentures depend on soft tissue support. They lift when the patient yawns. They shift when the patient bites down on hard foods. Many patients fear embarrassing moments in public. This fear reduces social confidence.
How Do Implants and Dentures Affect Daily Function?
Implants restore near-natural chewing and speech. Dentures reduce chewing efficiency and may cause clicking sounds.
Which Option Restores Better Chewing Power?
Implants restore nearly 100% of natural bite force. Dentures restore only 25% to 50%.
Natural teeth generate approximately 150 to 200 pounds of bite force per square inch. Dental implants restore this capacity almost completely. Patients eat raw vegetables. They chew nuts. They maintain a balanced diet. Removable dentures drastically reduce this power. Studies show that complete denture wearers generate only 25% to 50% of natural bite force. This limitation forces patients toward softer foods. Many denture wearers avoid fiber-rich fruits, crunchy vegetables, and tough proteins. Over time, this dietary shift affects overall nutrition and gastrointestinal health.
Elboraey and colleagues compared fixed implant-retained prostheses with removable implant-supported overdentures. They found that fixed prostheses demonstrated significantly higher masticatory efficiency. Both options improved muscle activity and occlusal balance. However, the fixed modality delivered superior clinical outcomes (Elboraey 2024).
Which Option Protects Natural Speech?
Implants allow normal phonetics. Dentures may cause lisping or clicking.
The tongue contacts the back of the upper front teeth during speech. It forms specific sounds like "s" and "th." Dental implants maintain this anatomical relationship. The crown sits at the same position as the natural tooth. Speech remains unchanged. Upper dentures cover the palate. This coverage alters tongue placement. Many new denture wearers develop a slight lisp. The denture base may also click during conversation. Patients must learn to speak more slowly. Some never fully adapt.
Which Option Feels More Comfortable?
Implants feel like natural teeth. Dentures often create sore spots and pressure points.
Patients with implants rarely notice their artificial teeth. The crown emerges from the gum like a natural tooth. No bulky acrylic covers the palate. No metal clasps wrap around other teeth. Removable dentures require daily adaptation. The acrylic base presses against the gum ridge. This pressure creates ulcers and sore spots. The dentist must adjust the denture flange repeatedly. Even well-fitted dentures cause minor irritation. Patients remove dentures at night specifically to let the gums rest.
How Do These Options Affect Jawbone Health?
Implants stimulate bone and prevent shrinkage. Dentures accelerate bone loss over time.
The alveolar bone exists solely to support teeth. When teeth disappear, the bone loses its purpose. The body resorbs the mineral content. It redirects calcium to other skeletal sites. This process continues throughout life. Patients wearing conventional dentures experience this resorption most severely. The denture base compresses the blood vessels in the gum tissue. This compression reduces blood flow to the bone. The bone shrinks faster.
Dental implants interrupt this cycle. The titanium post transmits occlusal forces into the surrounding bone. These forces trigger mechanoreceptors in the bone cells. Osteoblasts deposit new mineral matrix. The bone maintains its volume and density. Adell and his team documented this preservation in their landmark fifteen-year study. They observed stable bone levels around osseointegrated implants in edentulous jaws (Adell 1981).
Bone loss affects more than oral health. It alters the facial profile. The nose and chin move closer together. The lips turn inward. Wrinkles deepen around the mouth. These changes create a prematurely aged appearance. Implants preserve the youthful facial structure. Dentures cannot.
Which Option Lasts Longer?
Implants last twenty years or more. Dentures need replacement every five to ten years.
How Long Do Dental Implants Survive?
Well-maintained implants often last a lifetime. The crown may need replacement after fifteen to twenty years.
Pjetursson and colleagues conducted a systematic review of implant-supported fixed prostheses. They analyzed studies with at least five years of follow-up. They found high survival rates and noted that technical complications occurred but rarely caused failure (Pjetursson 2012). With proper oral hygiene and regular check-ups, the titanium fixture itself can last indefinitely. The porcelain crown endures wear. It may chip or stain after a decade or two. Replacing a crown costs far less than replacing the entire implant.
How Long Do Removable Dentures Last?
Dentures typically require relining every two years and full replacement every five to ten years.
The acrylic resin in dentures wears down. The artificial teeth flatten. The gum tissue underneath the denture shrinks. This shrinkage creates a loose fit. The dentist adds new acrylic to the denture base. This procedure is called relining. Most patients need relining every two to three years. After five to ten years, the denture teeth wear significantly. The acrylic becomes porous and stained. At this point, the lab must fabricate an entirely new denture. Each replacement requires new impressions, new fittings, and new adaptation periods.
What Are the Cost Differences Between Implants and Dentures?
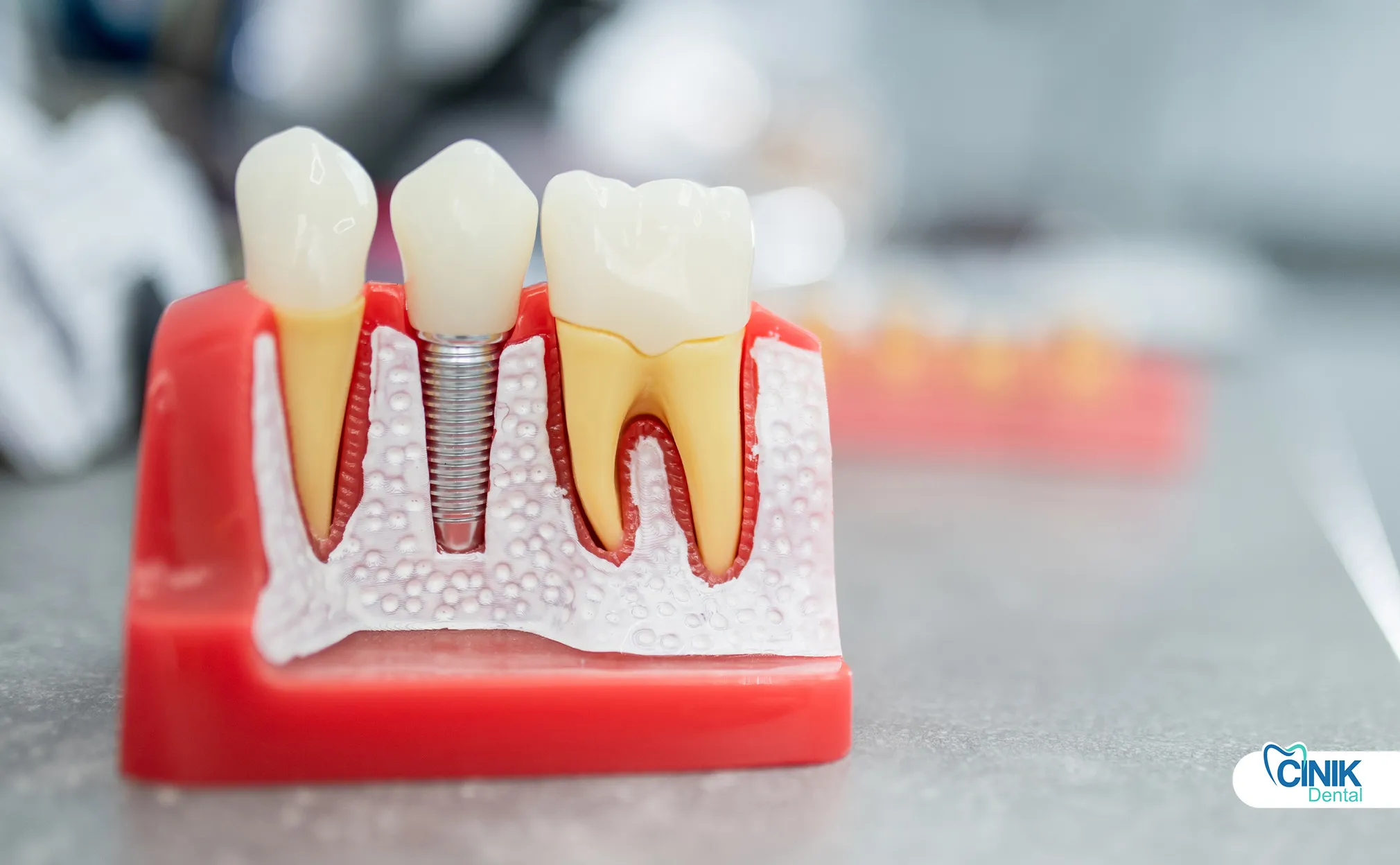
Dentures cost less upfront. Implants cost more initially but offer better long-term value.
What Are the Initial Costs?
A full set of dentures costs significantly less than a full-arch implant restoration. Single implants cost more than partial dentures.
A conventional upper or lower denture typically costs a fraction of a single implant. A full-arch implant restoration, such as All-on-Four, requires multiple implants, surgical fees, abutments, and a fixed bridge. The total initial investment runs much higher. However, patients must consider the full financial picture.
Which Option Saves Money Over Time?
Implants require fewer replacements and less maintenance. Dentures generate recurring costs for adhesives, relining, and remakes.
Denture wearers purchase adhesive paste monthly. They pay for relining every few years. They replace dentures every five to ten years. These costs accumulate over decades. Implants need only standard brushing and flossing. The patient visits the dentist for routine cleanings. The implant itself rarely needs replacement. Over a twenty-year period, the total cost of denture maintenance often approaches or exceeds the initial implant investment.
What Maintenance Does Each Option Require?
Dentures need daily removal, soaking, and adhesive application. Implants need only regular brushing, flossing, and dental check-ups.
How Do Patients Care for Removable Dentures?
Patients remove dentures every night. They brush the acrylic base. They soak the denture in a cleaning solution.
Dentures accumulate plaque and bacteria just like natural teeth. However, patients cannot brush them while wearing them. They must take the denture out. They scrub it with a soft brush and non-abrasive paste. They soak it overnight in a denture cleanser. This soaking kills odor-causing bacteria. Patients also clean their gums with a soft toothbrush. They apply denture adhesive every morning. They avoid sleeping with dentures in place. Nighttime removal allows the gum tissue to recover from daytime pressure.
How Do Patients Care for Dental Implants?
Patients brush implants twice daily. They floss around the abutment. They visit the dentist every six months.
Implant maintenance mirrors natural tooth care. The patient uses a soft-bristle toothbrush. He brushes along the gumline. He flosses between implants and natural teeth. Some patients use interdental brushes for hard-to-reach areas. The dentist checks implant stability during routine visits. He measures gum pocket depth. He removes any calculus buildup. He examines the bite to ensure even force distribution. Buser and his colleagues emphasized that ideal implant placement and maintenance protocols optimize long-term outcomes (Buser 2017).
What Are the Advantages and Disadvantages of Each Option?
Implants offer natural function and bone preservation but require surgery and higher cost. Dentures offer affordability and speed but provide less stability and accelerate bone loss.
What Are the Pros and Cons of Dental Implants?
Implants look natural, preserve bone, and last decades. They require surgery, cost more, and need healing time.
Advantages:
Implants restore nearly natural chewing power.
They prevent jawbone shrinkage.
They do not cover the palate.
They allow normal speech.
They do not slip or click.
They last twenty years or longer with proper care.
Disadvantages:
Surgeons must place them through invasive surgery.
They cost more than dentures initially.
They require three to six months of osseointegration.
Patients with severe bone loss may need grafting first.
Smoking and uncontrolled diabetes increase failure risk.
What Are the Pros and Cons of Removable Dentures?
Dentures cost less, require no surgery, and restore smiles quickly. They slip, reduce chewing power, and speed up bone loss.
Advantages:
Dentures cost less upfront.
Labs can fabricate them within weeks.
Patients avoid surgical risks.
Dentures work for patients with severe bone loss.
Technicians can modify or reline dentures easily.
Disadvantages:
Dentures provide only 25% to 50% of natural bite force.
They may shift during meals or conversations.
They cover the palate and alter taste sensation.
They accelerate alveolar bone resorption.
They require frequent adjustments and replacements.
Adhesives can be messy and unreliable.
What Are Implant-Supported Dentures?
Implant-supported dentures, also called overdentures, snap onto two or more implants. They combine implant stability with removability.
This hybrid solution offers a middle ground. The surgeon places two to four implants in the jaw. The lab fabricates a removable denture with special attachments underneath. The denture snaps onto the implants. The implants provide retention and stability. The patient removes the denture for cleaning.
Feine and colleagues championed this approach in the McGill Consensus Statement. They declared that the two-implant overdenture should become the first-choice standard of care for edentulous mandibles (Feine 1998). Martín-Ares and colleagues compared conventional dentures, fixed prostheses, and implant-supported overdentures. They found that implant-supported options delivered superior satisfaction and function compared to conventional dentures. Fixed prostheses showed the best function. Overdentures offered easier hygiene. Both surpassed conventional dentures in patient-reported outcomes (Martín-Ares 2016).
Dinu and colleagues recently reviewed implant-assisted removable partial dentures. They found that these devices showed favorable implant survival and lower rates of adjacent tooth loss compared to conventional removable partial dentures. However, they noted that long-term data remains limited (Dinu 2025). Kuroshima and colleagues also reviewed clinical applications. They concluded that implant-assisted removable partial dentures show promise but need more research (Kuroshima 2024).
Implant-supported overdentures cost less than full fixed bridges. They also allow patients to clean the prosthesis thoroughly. However, the attachments wear out. Patients must replace the nylon inserts every six to twelve months.
Which Patients Should Choose Implants?
Patients with adequate bone, good general health, and a desire for permanent solutions should choose implants.
When Do Dentists Recommend Implants?
Dentists recommend implants for patients with sufficient bone density, healthy gums, and no medical contraindications.
The ideal implant candidate possesses a thick, tall alveolar ridge. He maintains good oral hygiene. He does not smoke heavily. He controls chronic conditions like diabetes. He wants a solution that feels like natural teeth. He accepts the higher initial cost and surgical process. Younger patients often prefer implants because the long-term benefits outweigh the upfront investment.
Which Patients Should Choose Dentures?
Patients with medical contraindications, limited budgets, or immediate needs should choose dentures.
When Do Dentists Prefer Dentures?
Dentists prefer dentures for patients who cannot undergo surgery, need rapid restoration, or lack bone for implants.
Some patients take blood thinners. Others have uncontrolled heart conditions. Surgery poses unacceptable risks for these individuals. Dentures provide a safe alternative. Some patients need teeth immediately after extraction. An immediate denture restores appearance the same day. Bone grafting and implant healing would take months. Patients with severe financial constraints also benefit from dentures. The lower upfront cost makes tooth replacement accessible.
What Risks and Complications Should Patients Consider?
Implants carry surgical risks like infection and nerve damage. Dentures cause poor fit, speech issues, and progressive bone loss.
What Complications Can Implants Cause?
Implants may fail to integrate, become infected, or damage nearby nerves. Technical issues include screw loosening and crown fracture.
Surgical complications include bleeding, infection, and nerve injury. The inferior alveolar nerve runs through the mandible. A misplaced implant can compress this nerve. The patient may experience numbness in the lip and chin. Peri-implantitis poses a biological threat. This condition resembles gum disease. Bacteria colonize the implant surface. They destroy the surrounding bone. Without treatment, the implant loosens and fails.
Technical complications affect the prosthesis itself. Sánchez-Torres and Nagni both reported screw loosening and veneering fractures in fixed full-arch restorations (Sánchez-Torres 2021; Nagni 2023). However, these complications rarely caused complete failure. Patient satisfaction remained high despite technical issues.
What Problems Can Dentures Cause?
Ill-fitting dentures create ulcers, alter speech, and accelerate bone shrinkage. They may also cause fungal infections.
A poorly fitting denture rubs against the gum tissue. It creates painful sores. These sores can become infected. Denture stomatitis, a fungal condition, develops under the acrylic base. The yeast Candida albicans thrives in the warm, moist space between denture and gum. Patients must maintain strict hygiene to prevent this. Dentures also change speech patterns. The clicking noise embarrasses many wearers. The progressive bone loss under dentures complicates future implant placement. The patient may need extensive bone grafting if he later chooses implants.
How Should Patients and Dentists Make the Final Decision?
The dentist must evaluate oral health, bone density, lifestyle needs, and budget. The patient must share his expectations and concerns.
What Factors Matter Most?
Bone volume, general health, daily habits, financial resources, and personal expectations guide the decision.
The dentist takes a panoramic X-ray. He may order a cone-beam CT scan. These images reveal bone height and width. They show the location of nerves and sinuses. The dentist reviews the patient's medical history. He asks about smoking, diabetes, and medications. He discusses the patient's diet. Does the patient want to eat steak and apples? Does he mainly eat soft foods? He discusses social needs. Does the patient give public speeches? Does he fear denture slippage during meetings? He explains the financial timeline. He compares the upfront implant cost against the recurring denture costs.
Why Does the Dentist Consultation Matter?
Only a trained clinician can assess bone quality, surgical feasibility, and prosthetic design.
Self-diagnosis leads to poor outcomes. Patients cannot measure their own bone density. They cannot evaluate their gum health accurately. The dentist performs a comprehensive examination. He measures pocket depths. He assesses bite alignment. He evaluates the opposing arch. He may collaborate with an oral surgeon or periodontist. This team approach ensures safe, predictable results.
What Does the Future Hold for Tooth Replacement?
Digital planning, immediate-load protocols, advanced ceramics, and hybrid solutions will dominate future prosthodontics.
Computer-guided surgery improves implant placement accuracy. Dentists use 3D scans to plan the exact implant position. They print surgical guides. These guides direct the drill to the precise angle and depth. Immediate-load implants continue to evolve. More patients qualify for same-day teeth. Advanced ceramics like zirconia offer superior aesthetics and biocompatibility. Hybrid solutions like implant-supported overdentures will likely increase. They balance cost, function, and maintenance. Molinero-Mourelle and colleagues confirmed that tooth-implant-supported removable partial dentures represent a viable clinical option, especially for strategic abutment preservation (Molinero-Mourelle 2022).
What Is the Bottom Line in This Comparison?
Implants outperform dentures in function, bone preservation, and longevity. Dentures remain a valid choice for patients who need affordability or cannot undergo surgery.
Dental implants represent the gold standard for tooth replacement. They restore natural function. They preserve facial bone structure. They last decades. However, they demand a higher initial investment. They require surgery. They need adequate bone volume.
Removable dentures provide an accessible, non-surgical alternative. They restore smiles quickly. They cost less upfront. However, they reduce chewing power. They accelerate bone loss. They need frequent replacement.
The optimal choice depends on the individual. A healthy sixty-year-old with strong bone should consider implants. A frail eighty-year-old on blood thinners may benefit more from dentures. A middle-aged patient with moderate bone loss might choose an implant-supported overdenture.
Every patient deserves a personalized treatment plan. The dentist must lead this decision. He must weigh clinical evidence against patient values. He must explain the long-term implications of each option. The patient must ask questions. He must understand maintenance requirements. Together, they select the solution that best serves the patient's health, function, and quality of life.
Frequently Asked Questions
Are Implants Better Than Dentures?
Yes, implants generally provide better function, stability, and bone preservation. However, "better" depends on the patient's health, bone, and budget.
How Long Do Removable Dentures Last?
Dentures typically last five to ten years before requiring full replacement. Patients need relining every two to three years.
Can Dentures Convert to Implants?
Yes, many patients start with dentures and later upgrade to implants. However, prolonged denture use may cause bone loss that requires grafting.
Are Implants Painful?
Surgeons use local anesthesia during implant placement. Most patients experience mild soreness for a few days. Over-the-counter pain relievers manage this discomfort.
Which Option Looks More Natural?
Both options look natural. However, implants emerge from the gum like real teeth. Dentures may show acrylic borders or metal clasps.
Comparison Table: Implants vs Removable Dentures
Feature | Dental Implants | Removable Dentures |
Surgical Need | Yes, minor surgery required | No surgery needed |
Bone Preservation | Stimulates and preserves bone | Accelerates bone resorption |
Chewing Efficiency | Restores ~100% of natural force | Restores 25%–50% of natural force |
Stability | Fixed and immovable | May shift or lift |
Speech Impact | No change | May cause lisp or click |
Comfort | Feels like natural teeth | May cause sore spots |
Initial Cost | Higher | Lower |
Long-Term Cost | Lower maintenance costs | Higher cumulative costs |
Lifespan | 20+ years or lifetime | 5–10 years |
Daily Maintenance | Brush and floss normally | Remove, brush, soak nightly |
Palate Coverage | None | Upper denture covers palate |
Treatment Time | 3–6 months (or same-day) | 2–4 weeks |
Candidacy | Requires adequate bone and health | Works for most patients |
References
Adell, R., et al. "A 15-Year Study of Osseointegrated Implants in the Treatment of the Edentulous Jaw." International Journal of Oral Surgery, vol. 10, no. 6, 1981, pp. 387-416.
Branemark, Per-Ingvar, et al. "Osseointegrated Implants in the Treatment of the Edentulous Jaw." Scandinavian Journal of Plastic and Reconstructive Surgery, vol. 13, no. 1, 1977, pp. 1-10.
Buser, Daniel, et al. "Long-Term Stability of Early Implant Placement with Contour Augmentation." Journal of Clinical Periodontology, vol. 44, no. 12, 2017, pp. 1237-1247.
Carlsson, Gunnar E. "Responses of the Jawbone to Stress." Anatomy and Physiology, 2004.
Dinu, Robert-Cosmin, et al. "Clinical Performance and Longevity of Implant-Assisted Removable Partial Dentures Compared to Other Removable Prosthesis Types: A Systematic Review." Dentistry Journal, vol. 13, no. 9, 2025, p. 389.
Elboraey, A., et al. "Fixed Implant-Retained vs Removable Mandibular Implant-Supported Overdenture." Journal of Prosthodontics, 2024.
Feine, Jocelyn S., et al. "The McGill Consensus Statement on Overdentures." International Journal of Prosthodontics, vol. 11, no. 4, 1998, pp. 307-308.
Kuroshima, Shinichiro, et al. "Implant-Assisted Removable Partial Dentures: Part I. A Scoping Review of Clinical Applications." Journal of Prosthodontic Research, vol. 68, 2024, pp. 20-39.
Martín-Ares, M., et al. "Patient Satisfaction, Functional Satisfaction, Oral Hygiene Maintenance, and OHRQoL with CD, FP, and OD." Gerodontology, 2016.
Molinero-Mourelle, P., et al. "Clinical Performance of Tooth Implant-Supported Removable Partial Dentures: A Systematic Review and Meta-Analysis." Clinical Oral Investigations, vol. 26, 2022, pp. 6003-6014.
Nagni, M., et al. "Fixed Full-Arch Implant Prosthesis: A Retrospective Study." Journal of Clinical Medicine, 2023.
Pjetursson, Bjarni E., et al. "A Systematic Review of the Survival and Complication Rates of Implant-Supported Fixed Dental Prostheses after an Observation Period of at Least 5 Years." Clinical Oral Implants Research, vol. 23, no. 6, 2012, pp. 22-38.
Sánchez-Torres, A., et al. "Immediately Loaded Complete-Arch Implant-Supported Prostheses: A Retrospective Cohort Study." Journal of Oral Rehabilitation, 2021.