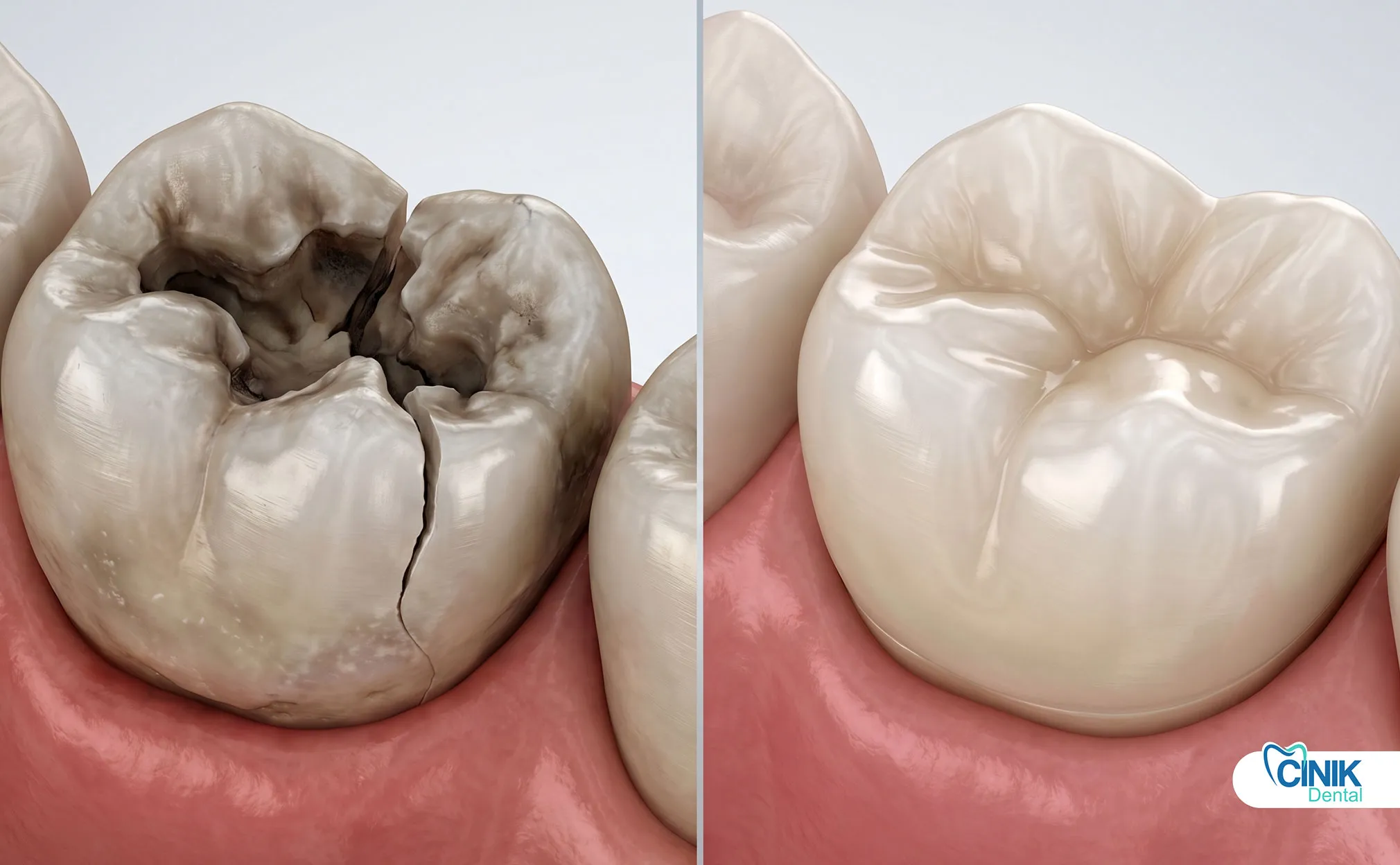
Gingival (gum) recession occurs when gum tissue pulls away from the teeth, exposing the roots and increasing the risk of sensitivity, decay, infection, and tooth instability. It is common in adults and becomes more prevalent with age, influenced by factors such as aggressive brushing, gum disease, genetics, aging, and improper oral habits. Early signs include sensitive teeth, longer-looking teeth, exposed roots, discomfort, and changes in bite or denture fit. While mild recession can often be managed with proper home care such as gentle brushing and fluoride use advanced cases may require professional treatments like scaling, gum grafts, or regenerative therapies. Beyond aesthetics, gum recession affects tooth support and overall health, as poor gum health is linked to systemic conditions including cardiovascular disease. Early detection, preventive care, and timely dental intervention are essential to slow progression, protect oral structures, and maintain long-term oral and general health.
1. How to understand Gingival Recession
Quick Answer: Gingival recession is the loss of gum tissue that exposes tooth roots, raising the risk of sensitivity and decay. It is common with age and is often caused by hard brushing, gum disease, genetics, and natural aging.
Gingival recession occurs when gum tissue moves away from teeth and exposes tooth roots. It can also leave teeth that look longer, creates gaps between teeth, and leads to greater risk of cavity and infection. The condition affects adults across the world, with the risk increasing with age. Studies show that gum recession has a high prevalence, with an estimated 58% of adults aged 30 and up experiencing at least 1 millimeter of it (M Kassab et al., 2010). The loss of periodontal tissue does not begin at a specific age and may develop well into senior years.
Many factors contribute to gingival recession. One of the most common is brushing too hard, especially when using a hard-bristled toothbrush, because the gums will recede before the enamel will wear away. Other oral health issues, such as gum disease or gingivitis, cause tissues to wear away. Genetics can play a role as well. The condition may arise as part of natural aging because tissue strength tends to diminish in older adults.
1.1. What is gingival recession
Quick Answer: Gingival recession is when gums pull back from teeth, exposing the roots and making teeth look longer.
Gum recession is a common dental problem. It happens when gum tissue pulls back from the teeth. This leaves the roots of the teeth exposed. Gum recession can cause major oral health issues. Yet it often goes unnoticed until it is advanced (Pradeep et al., 2012).
Gum recession appears in several ways. The roots of teeth become visible. Teeth look longer than normal. The gaps between teeth change. In severe cases, the tissue above the tooth may shrink.
Gingival recession is defined as the apical migration of the gingival margin to the cementoenamel junction. Periodontal disease, immovable large-rooted teeth, improper flossing, inflammatory lesions, aggressive tooth brushing, incorrect occlusal relationships, orthodontic treatment, and dominant teeth affecting interdental papillae can all contribute (M Kassab et al., 2010). Recession can be localized or generalized and may or may not involve loss of attached tissue. It is prevalent among adults; at least 58% of individuals aged 30 or older considered sought dental care and met the clinical criteria, followed by 40% of those aged 18 to 29.
1.2. Why gums recede
Quick Answer: Gums recede due to factors such as aggressive brushing, gum disease, aging, and genetics. The condition becomes more common with age and can progress unpredictably over time.
Gingival recession is when gum tissue moves away from teeth. The gingival margin (the upper limit of the gum tissue) migrates apically, exposing the root, or the part of the tooth normally covered by the gum. The tooth then appears longer.
Various factors contribute to gingival recession. The most common include improper brushing techniques (particularly too much pressure or using a hard toothbrush), periodontal disease of any kind, aging, and heredity (Pradeep et al., 2012). According to a large American health survey, 88% of the population show some degree of gum recession. The prevalence of recession increases with age. More than half of adults over 30, and three quarters of those over 70, show at least one millimeter of receded gum tissue, and men and African Americans tend to suffer more. Since the causes are not always obvious, recession can continue to progress unpredictably, even in apparently stable mouths (M Kassab et al., 2010).
1.3. How it shows up in your mouth
Quick Answer: Gingival recession shows up as exposed tooth roots, longer-looking teeth, and wider gaps between teeth. It may cause sensitivity, pain, bite changes, or denture fit problems as it progresses.
Gingival recession occurs when the gum tissue pulls away from the tooth. This exposes more of the tooth’s root. It also makes the teeth appear longer. The gum line can also change when it upwardly moves up between teeth, spacing opens between the teeth. Saliva that should be cleaning between teeth flow becomes restricted. Gum disease, brushing too hard, and genetic factors can cause the tissue to recede (Pradeep et al., 2012). More detailed treatment options may be needed when the recession continues, causing sensitivity, tooth pain, discomfort, changing the fit of a denture, or changing the bite.
2. What are the Common Signs You Shouldn’t Ignore?

Quick Answer: Common signs of gum recession include tooth sensitivity, longer-looking teeth, exposed roots, and pain as damage progresses.
Sensitive teeth are commonly associated with exposed dentin, the layer beneath the enamel that's vulnerable to temperature and touch. When gums recede, cementum doesn't protect exposed dentin, making teeth sensitive.
Longer looking teeth are an indication of gum recession. With the receding gums, the portion of the tooth above the gum line appears in greater length and consequently the tooth seems longer. Gum tissues around the teeth shorten over time, causing longer-looking teeth, as they’re losing their supportive tissues.
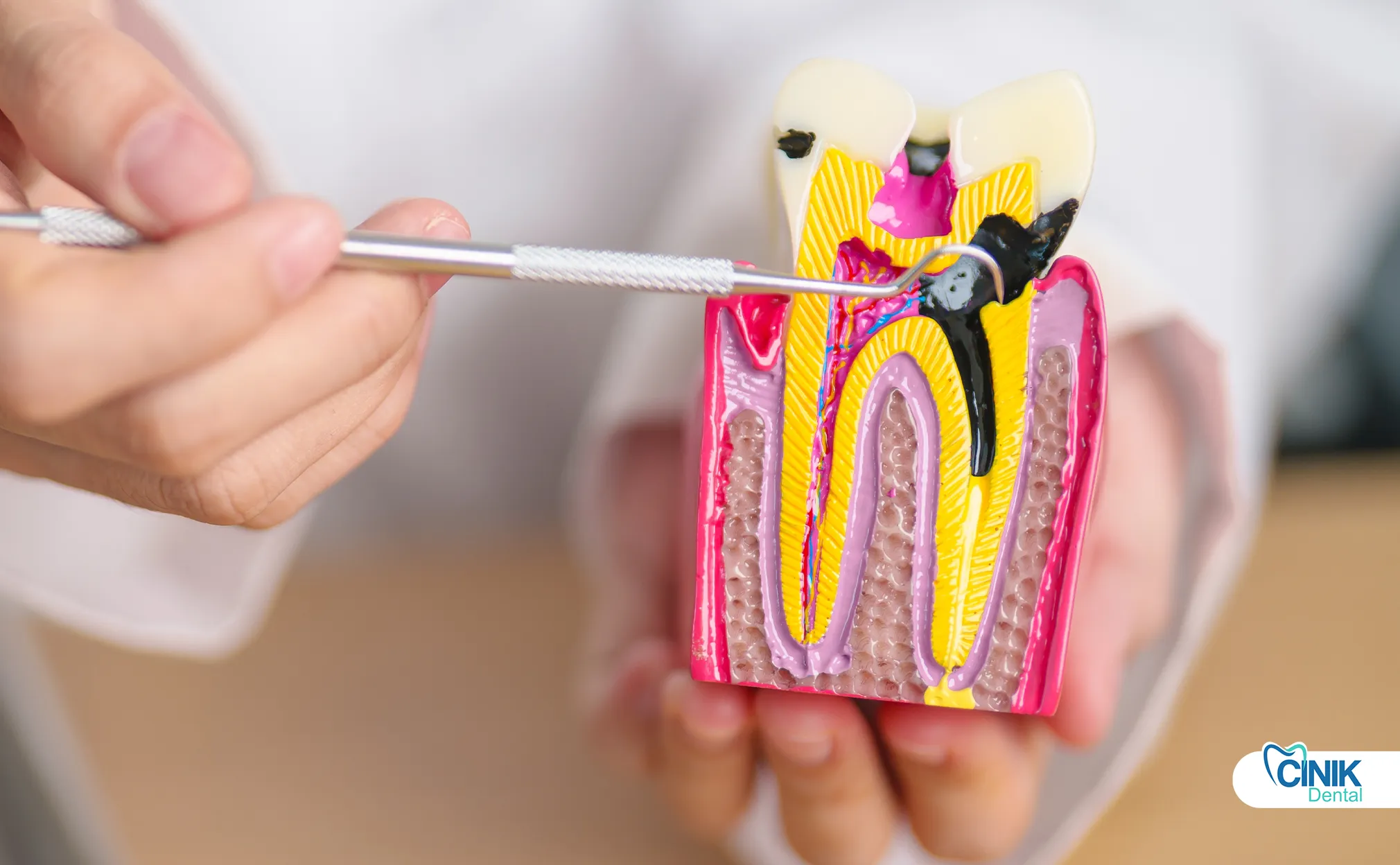
As the polystratic supporting gum tissues recede away from the cementum of teeth, the thinner uncontrolled cementum material gets exposed. The exposed cementum can suffer damage and will not be protected as it is when it's covered by healthy gingival tissues. If gum recession continues further, the underlying bone surrounding the teeth may also be exposed and can dissolve.
If the primary lamina of the tooth is also lost, the bacteria at that location may enter into it. These bacteria may damage other tissues making it hurt in some specific cases or even lead to pulp death.
2.1. What are sensitive teeth?
Quick Answer: Sensitive teeth occur when receding gums expose the dentin, allowing heat, cold, or touch to trigger discomfort. Teeth may also appear longer as the gum line moves downward.
Gingival recession often becomes noticeable through tooth sensitivity. When gum tissue retracts from the teeth, it exposes the dentin layer underneath. This layer contains tiny openings that lead to the nerve pathways inside teeth. Once a person loses the protective enamel shield on the crown or the cementum cover on the root, thermal, tactile, or chemical stimulation can cause discomfort in response to cold, heat, sweet, sour, or acidic substances. Generally, patients with generalized gingival recession develop sensitive areas on the facial or lingual surfaces of the incisors, canines, or premolars (Pradeep et al., 2012).
The teeth may also appear longer. A careful examination may reveal that the crown remains unchanged in dimension while the gum has moved down. The transition contour between the tooth and the gum is longer than in the adjacent teeth.
2.2. What are longer looking teeth?
Quick Answer: Longer-looking teeth occur when gums recede, exposing more of the tooth and making it appear elongated.
In addition to sensitivity, longer looking teeth can indicate gum recession. The tissue that surrounds the tooth wears away, elongateding the appearance of teeth. Unlike most other conditions that only affect the tooth, gum tissue recession affects the space between teeth. Instead of brushing teeth as needed, the addition of “gums” restores normal appearance. (Pradeep et al., 2012)
2.3. What are exposed roots?
Quick Answer: Exposed roots occur when receding gums uncover the tooth roots, leading to sensitivity, higher risk of decay, discoloration, and a longer-looking tooth.
Gingival recession, also known as gum recession, occurs when the gums pull away from the teeth, exposing the tooth roots. Roots are not normally visible but become a concern when they are exposed (Pradeep et al., 2012). The exposed root surfaces can develop decay, leading to further destruction of the tooth. Recession may also expose sensitive root surfaces, increasing discomfort when consuming cold drinks or sweets. The tooth appears longer, giving an unpleasing smile. In the form of a localized area, the exposed root can become discolored from staining, drawing even more attention to it. Recession may worsen over time and may not be necessarily an irreversible condition.
2.4. What is toothache or discomfort?
Quick Answer: Toothache or discomfort is pain or sensitivity when chewing or consuming hot or cold foods, often caused by irritation or damage to the tooth pulp and sometimes requiring root canal treatment.
Some people can feel sensitivity and/or pain while chewing food. In more serious cases, it's also possible to have pain when eating or drinking hot or cold food and beverages. All these symptoms could happen because the tooth's pulp is affected. If a tooth's pulp becomes affected by tooth decay, is exposed to the outside environment, or if the pulp's blood vessels are compressed because of another cause, it could result in pain and require endodontic therapy. If the tooth's pulp becomes necrotic, it could be a reason for a dental abscess and require endodontic therapy.
2.5. What are the changes in bite or fit of dentures?
Quick Answer: Changes in bite or denture fit happen when gum tissue is lost, causing teeth or dentures to shift or loosen.
Gingival recession leads to loss of tissue around teeth, eventual loss of teeth, and a major public health issue. Changes in denture fit can indicate tissue loss or other oral health problems. (Coulthwaite and Verran, 2007) (Kalina et al., 2022)
3. What are the Available Treatment Approaches?
Quick Answer: Gingival recession is treated with gentle home care, professional cleaning, and, in advanced cases, gum grafts or regenerative therapies.
Gingival recession can be detected by certain signs. You may feel sensitive teeth due to exposed dentin. The teeth may appear longer because of gum loss. Exposed roots may cause discomfort and should be taken seriously. Some patients report toothache, particularly in cold weather, or discomfort that may indicate sensitivity issues. A change in bite or denture fit can also indicate tissue loss. Teeth may drift apart, leading to shifts in how upper and lower teeth contact during chewing.
Preventive measures can be taken at home. Using a soft-bristled toothbrush and a gentle brushing technique can help. Using a fluoride rinse after regular brushing is recommended. A fluoride treatment at the dentist may help strengthen teeth, especially in exposed areas.
Gingival recession may require further attention from a dental professional. If gingival recession is suspected, arrange a visit. During a typical exam, the dentist will visually inspect the gums and roots around the teeth. The clinician may also ask about teeth that feel sensitive or uncomfortable. A determination then follows regarding whether any treatment is necessary. Treatment options vary and depend on multiple factors.
When a professional is involved, some minor cleaning is often performed beforehand. A careful clean-up may help minimize further buildup that can cause sensitivity or decay. Another service, scaling, removes tartar and plaque buildup from roots below the gum line. When gum disease is present, scaling is done prior to other therapy.
Advanced options may include gum grafting or similar procedures that help prevent further recession. These procedures can maintain healthy tissues around teeth. Different grafts or flap techniques aim to cover roots, for example, when the surfaces are covered with composite resin to reduce sensitivity. These options are needed when the gum has already receded.
Regenerative procedures for further tissue-building rely on growth factors contained in the body’s own platelets. Another option available in select practices focuses on tissue-regeneration technology that helps build tissue in needed areas. During a visit, the dentist will examine tissue around teeth and may ask questions regarding any gum, tooth, or joint issues. Options can then be discussed, including preventive measures to limit further recession or treatments to help already-exposed roots.
3.1. How to care and prevent at home
Quick Answer: Home care focuses on gentle brushing with a soft toothbrush, minimal pressure, and proper technique to protect gums and prevent further recession.
Gums support teeth. When gum tissue recedes, roots become exposed. This changes how teeth fit together and increases sensitivity (Kumar et al., 2023).
Proper brushing helps prevent tissue loss. Always use a soft brush. Hold the brush at a 45-degree angle against gums. Apply minimal pressure. The best toothbrush is one the patient likes. Modern electric brushes are generally best, with gentle, oscillating movements. If hands are unsteady, grasp the brush like a pen and rest the wrist on the cheek.
3.2. What is professional cleaning and scaling?
Quick Answer: Professional cleaning and scaling remove plaque and tartar to improve gum health.
Periodontal disease produces a variety of clinical manifestations. Among these is loss of soft and hard tissue, which must be characterized to identify appropriate treatment needs. The objective of scaling is to enhance the patients’ gingival health status (Kumar et al., 2023).
3.3. What are gum grafts and advanced options?
Quick Answer: Gum grafts restore lost gum tissue and cover exposed roots, while advanced options use regenerative therapies to rebuild support.
Growing evidence indicates receding gums often accompany periodontal disease, either in the first stage or in a more advanced form, known as periodontitis, characterized by loss of attachment. Both things generally occur together (Mary George et al., 2012). Grazing of the hard surface on the crown of the tooth leads to pronounced malaise. At this stage, the gums may also exhibit a change in color and tone.
Corrective resistance measures are therefore usually followed by prescriptions, including gum grafts, which different professionals call “tissue grafting” or “soft-tissue grafting.” The same professionals, however, also call connective-tissue grafts “gum grafts” (M Kassab et al., 2010). Alternatives are regenerative treatments incorporating growth factors (platelet-derived growth factor or enamel-matrix proteins) or therapies employing cell-therapy approaches mixed with growth factors or other tissue-engineering principles.
3.4. What are regeneration and modern therapies?
Quick Answer: Regeneration and modern therapies aim to rebuild lost gum and bone tissue using growth factors, cell-based methods, and tissue-engineering techniques to restore tooth support.
Periodontal tissues play essential roles in supporting teeth, and periodontal disease, one of the major oral health problems, causes these tissues to deteriorate around teeth. Therefore, regeneration of the periodontal tissues lost to disease is a crucial focus in periodontology. A variety of methods such as mechanically controlled delivery of cells (tooth-driven cell therapy), tooth movement, local application of growth factors, and strategic use of tissue-engineering concepts (scaffolds plus growth factors) are under investigation. Furthermore, methods that align with the self-repair capacity of damaged periodontal tissues and recruit progenitor/stem cells residing in neighboring tissues are actively being developed.
The need for periodontal regeneration can arise when tissues have been lost due to periodontal disease, when the mucogingival complex is insufficient to maintain marginal gingiva around free mucosal grafted sites, or when localized gingival recession occurs. Current materials and techniques for periodontal tissue regeneration achieve variable outcomes and exhibit some limitations. Therefore, research continues to clarify the biological basics of periodontal regeneration and to provide clinical solutions. The clinical needs can also be classified as restoration of the regenerative capacity of the periodontal tissues, alleviation of gingival recession, and the treatment of oral and periodontal diseases, which occur as complications of various pathological conditions. In each category, a spectrum of desirable materials is being explored, and the construction and verification of biological evidence to achieve these goals is an area of developmental focus (M Kassab et al., 2010).
3.5. What to expect in a visit to the dentist
Quick Answer: A dental visit involves an exam and symptom review to plan treatment, as untreated gum recession can cause sensitivity, decay, and gum disease.
A visit to the dentist often begins with a thorough clinical examination and a review of the patient’s medical history. It is helpful to inform the dental practitioner about oral hygiene habits, specific dental concerns, and any discomfort. These details facilitate an accurate diagnosis, assist in developing a personalized treatment plan, and guide the selection of preventive and therapeutic interventions.
Gingival recession carries several undesirable consequences that extend beyond mere esthetic concerns. If the problem remains neglected, gingival recession may lead to the retention of plaque around the tooth, the initiation of periodontal disease, and an increase in the quantity and severity of gingival bleeding. In addition, the exposure of the cervical dentine commonly associated with gingival recession renders the tooth hypersensitive to thermal or osmotic stimuli. Such discomfort constitutes a sharp, fleeting sensation of short duration generally triggered by exposure to cold stimuli or by contact with tooth paste or mouth rinses (Pradeep et al., 2012). Exposed root surfaces adjacent to teeth that have undergone periodontal maintenance further predispose the individual to root caries, dentin hypersensitivity, and, potentially, periodontal disease activity.
4. Why Gum Health Matters More Than Appearance

Quick Answer: Gum health matters because receding gums expose vulnerable tooth roots, increasing the risk of decay, sensitivity, tooth loss, and overall health problems.
Gingival recession allows plaque and bacteria to thrive in the space between teeth and gums. As tissue recedes, dental roots, which are softer and more porous than enamel, become exposed, increasing the risk of decay, sensitivity, and tooth loss (Pradeep et al., 2012). Tooth loss and dental instability can severely impact aesthetic appearance and overall health.
4.1. How to protect tooth support
Quick Answer: Tooth support is protected by preventing gum recession, which otherwise exposes roots, loosens teeth, increases plaque buildup, sensitivity, and the risk of decay and bone loss.
Gingival recession exposes root surfaces that compromise tooth support, causing teeth to loosen and move. Jawbone and gum tissue can vanish without support. Spacing between teeth also widens, predisposing to plaque accumulation that leads to decay and gum inflammation. Unattractive tooth appearance results, and recession also serves as a plaque retention site, leading to bleeding. Exposed cervical dentine generates sharp, short-term hypersensitivity often triggered by cold stimuli. These surfaces elevate root-caries risk, especially with multiple exposures. Periodontal-maintained patients exhibit lesions on exposed roots (Pradeep et al., 2012).
4.2. How to prevent further loss
Quick Answer: Further loss is prevented through early intervention, good oral care, and ongoing treatment to slow recession, protect exposed roots, and reduce risks to overall health.
Gum recession can cause more than cosmetic concerns; it threatens the foundation that supports teeth and dentures. Receding gums expose root surfaces, which lack protective enamel and can lead to decay, abscess, and loss of stability (Pradeep et al., 2012). Advanced stages also reveal bone tissues; once gone, they cannot be restored, though certain treatments can stimulate regeneration.
Gingival tissue continues to recede after the first instance. Early intervention can slow this progression, and ongoing care helps maintain results and prevent further loss. Gum problems in childhood can indicate a risk that may persist throughout life, but preventive measures can limit damage.
The mouth connects to other systems; poor oral health can increase susceptibility to respiratory diseases, heart conditions, and complications during pregnancy.
4.3. How overall health links to gum recession
Quick Answer: Gum health affects overall health, as bacteria from gum disease can enter the bloodstream and impact the heart and other systems.
Unquestionable links connecting gum health to overall wellness have been established. The mouth acts as a potent gateway to the body, both positively and negatively. When inflammatory gum disease is present, oral pathogens can enter the bloodstream, carrying harmful bacteria to the heart (Kumar et al., 2023). Early-stage gum disease, reversible with improved home care, may nevertheless cause tooth-supporting bone to recede. Once lost, bone and soft tissue never return independently. Moreover, adherence to effective oral hygiene practices can diminish the negative impact of periodontal bacteria on the heart (Schwarz et al., 2023).
Research suggests a connection between periodontal diseases and other chronic health issues. Studies have evidenced a two-way link between gum health and systemic disorders. Furthermore, the presence of specific systemic diseases may expand the local periodontal microbiome, promoting a detour into systemic health problems (S. Lipsky et al., 2024).
5. Conclusion

Gingival recession exposes potentially vulnerable areas of the teeth. It can arise from a number of causes. Protecting or restoring tissues around the teeth is therefore an important aspect of maintaining oral health. The gingiva protects the roots of the teeth, the bone around the teeth, and the periodontal attachment. Loss of gingival tissue that was once attached to the teeth leads to increased exposure of the root surface, an elongated clinical crown, or a change in the bite (Pradeep et al., 2012). Once gingival recession has begun, further loss may occur over time. Therefore, reducing gingival inflammation, improving oral hygiene, and achieving adequate clinical attachment are essential steps to take at the earliest sign of recession (Nwhator, 2014). Studies show links between oral and general health. Oral conditions can also lead to symptoms elsewhere in the body.
References:
M Kassab, M., Badawi, H., and R. Dentino, A. "Treatment of Gingival Recession." 2010. [PDF]
Pradeep, K., Rajababu, P., Satyanarayana, D., and Sagar, V. "Gingival Recession: Review and Strategies in Treatment of Recession." 2012. ncbi.nlm.nih.gov
Coulthwaite, L. and Verran, J. "Potential pathogenic aspects of denture plaque." 2007. [PDF]
Kalina, E., Grzebyta, A., and Zadurska, M. "Bone Remodeling during Orthodontic Movement of Lower Incisors—Narrative Review." 2022. ncbi.nlm.nih.gov
Kumar, A., Grover, V., Satpathy, A., Jain, A., Singh Grover, H., Khatri, M., Kolte, A., Dani, N., Melath, A., Singh Chahal, G., Thomas, B., Raju Pradeep, A., Pandit, N., Radhamoni Madhavan Pillai, B., G. Shiva Manjunath, R., Nandkeoliar, T., Puri, K., Singhal, R., Dodwad, V., Bhardwaj, A., Thakur, R., Jalaluddin, M., Boyapati, R., Kumar Singh, M., and Bansal, M. "ISP good clinical practice recommendations for gum care." 2023. ncbi.nlm.nih.gov
Mary George, A., S. Rajesh, K., Hegde, S., and Kumar, A. "Two stage surgical procedure for root coverage." 2012. ncbi.nlm.nih.gov
Schwarz, C., Ioan Hajdu, A., Dumitrescu, R., Sava-Rosianu, R., Bolchis, V., Anusca, D., Hanghicel, A., Doris Fratila, A., Oancea, R., Jumanca, D., Galuscan, A., and Leretter, M. "Link between Oral Health, Periodontal Disease, Smoking, and Systemic Diseases in Romanian Patients." 2023. ncbi.nlm.nih.gov
S. Lipsky, M., Singh, T., Zakeri, G., and Hung, M. "Oral Health and Older Adults: A Narrative Review." 2024. ncbi.nlm.nih.gov
Nwhator, S. O. "Gingival Recession in a Child-Patient; Easily Missed Etiologies: Case Report with Video." 2014. ncbi.nlm.nih.gov