Dental fillings form the cornerstone of restorative dentistry in the functional and aesthetic restoration of tooth tissue damaged by decay or traumatic injury. These artificial materials serve as a biological barrier that protects the pulp tissue from thermal, chemical, and mechanical irritations while restoring the anatomical form of the tooth. However, there is a critical fact: fillings are not permanent structures. They can deteriorate over time due to biological, chemical, and mechanical factors.
Early diagnosis plays a decisive role in preventing tooth loss and advanced invasive treatments. This article aims to define the clinical and subjective signs of a faulty filling in light of scientific foundations. It provides a practical diagnostic guide for patients and practitioners.
What is a Dental Filling and How Does It Work?
A dental filling is a restorative structure composed of biocompatible materials used to fill cavities formed after the removal of decay lesions. This structure serves two primary functions: ensuring mechanical integrity and maintaining biological protection.
Mechanically, the filling protects the structural integrity of the tooth by distributing chewing forces. Biologically, it prevents secondary caries by blocking bacterial infiltration. A successful filling must create a leak-proof seal at the tooth-filling interface at the micro level (Khurana et al., 2025).
What Filling Materials Are Used and What Are the Differences Between Them?
In modern restorative dentistry, three main filling materials stand out:
Material | Composite Resin | Amalgam | Ceramic/Glass Ionomer |
Aesthetic | Excellent (tooth color) | Weak (silver color) | Good-Very Good |
Durability | 5-15 years | 10-15 years | 7-10 years |
Annual Failure Rate | %0.94-9.43 | %0.16-2.83 | ~%7 |
Chemical Bonding | Yes (adhesive) | No (mechanical) | Yes (ionomer) |
Polymerization Shrinkage | %1.5-4.3 | No | Minimal |
In the retrospective study of 400 patients by Khurana and colleagues (2025), composite restorations accounted for 69.5% of total failures, while amalgam was at 24.25% and glass ionomer at 6.25%. This distribution reflects the more widespread use of composites and aesthetic expectations; however, it also indicates the need for technical precision.
What is the Lifespan of Fillings and What Determines It?
The lifespan of a filling varies depending on the type of material, cavity size, oral hygiene, and chewing forces. Amalgam restorations show a survival rate of 94.4% at 7 years of follow-up, while composite restorations have a survival rate of 85.5% (Opdam et al., 2004). However, these are average values; individual variations can differ significantly.
Why Do Fillings Fail?
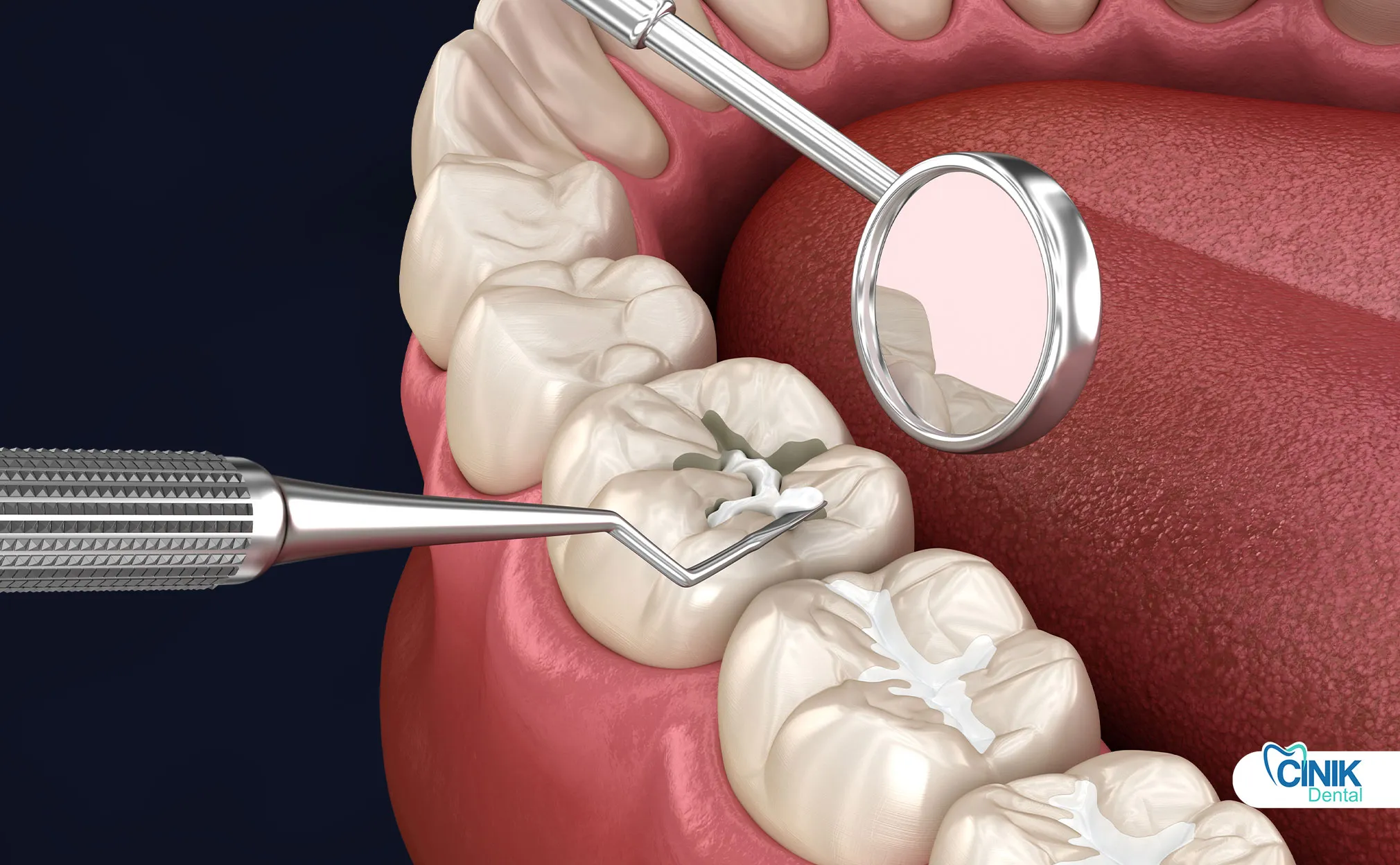
Chewing forces, especially in the posterior teeth, can reach pressures of 150-200 psi (pounds per square inch) on restorations. The repetitive application of these forces leads to material fatigue and micro-cracking.
Teeth grinding (bruxism) contributes significantly to this mechanical stress. In a comprehensive screening study by Al-Talib and colleagues (2025), it was shown that bruxism is a significant risk factor for both direct and indirect restoration failures. The meta-analysis by Tabassum and the team (2025) revealed that the risk of ceramic restoration failure significantly increased in patients with sleep bruxism.
Hard foods (ice, hard candies, nut shells) and traumatic events (sports injuries, accidents) can cause filling fractures or cracks in the tooth structure by applying high forces instantaneously.
How Do Chemical and Thermal Effects Threaten Filling Integrity?
Differences in the thermal expansion coefficients between dental tissue and restorative materials lead to stress formation in the marginal area after hot-cold cycles. The thermal expansion coefficient of composite resins (~30-40 × 10⁻⁶/°C) is significantly higher than that of enamel and dentin (~11 × 10⁻⁶/°C).
Acidic environments (gastric reflux, consumption of acidic beverages) contribute to the wear of filling surfaces and the degradation of marginal integrity. This chemical erosion prepares the ground for the formation of microscopic gaps and bacterial infiltration.
Biological Factors and Secondary Caries Formation
Secondary caries (recurrent caries) are new carious lesions that develop around or beneath an existing filling. In a study by Khurana and colleagues (2025), secondary caries ranked first among the reasons for failure at a rate of 73.5%. This rate is 95.65% in amalgam restorations and 93.28% in composites.
Microorganisms (Streptococcus mutans, Lactobacillus species) infiltrate the marginal gaps at the filling-tooth interface and produce acid. These acids lead to demineralization of enamel and dentin. Microleakage is the main mechanism of bacterial and fluid infiltration; it was detected at a rate of 99.25% among the reasons for failure in Khurana's study.
How Does Aging and Material Fatigue Manifest Over Time?
All restorative materials undergo physical and chemical changes over time. In composite resins, post-polymerization reactions of remaining monomers after polymerization shrinkage lead to the accumulation of internal stress. In amalgam, corrosion and darkening can be observed.
Material fatigue progresses through the growth and merging of micro-cracks due to repetitive chewing forces. This process increases the brittleness of the restoration and leads to ultimate failure.
What Are the Clinical Symptoms of Defective Fillings?
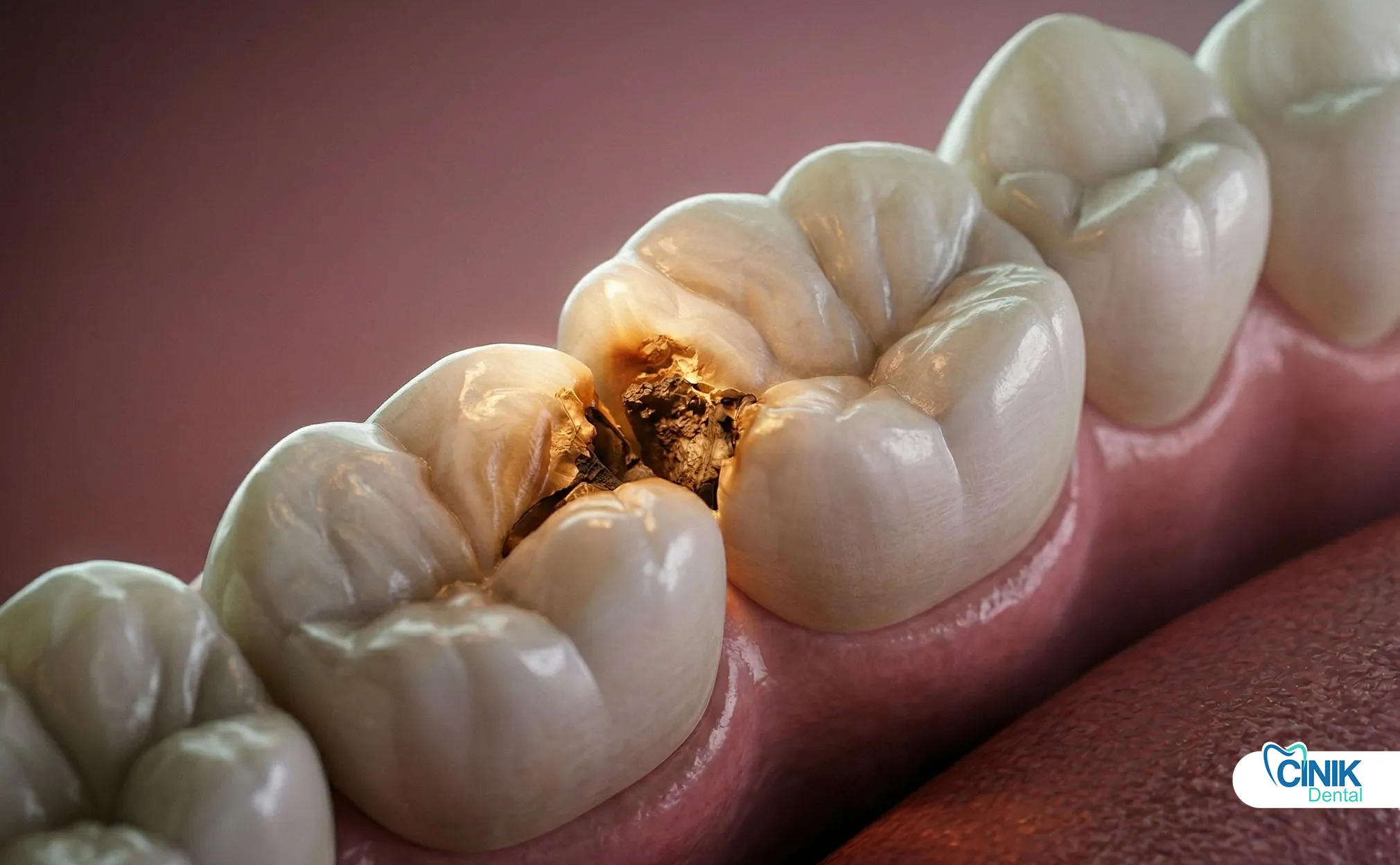
The disruption of the filling's marginal seal exposes the dentinal tubules and pulp tissue to thermal stimuli. Sudden, sharp pains after consuming hot coffee or cold ice cream indicate the loss of the filling's seal.
This sensitivity is related to increased dentin permeability and even pulp irritation. In the study by Khurana and colleagues (2025), thermal sensitivity holds a significant place among failure indicators. The onset of pain weeks or months after placement suggests that the restoration is deteriorating.
What Does Pain or Pressure Sensitivity During Chewing Mean?
Pain felt during biting or chewing may indicate three fundamental pathologies:
Cracking or loosening of the filling: Loss of mechanical integrity disrupts force distribution
High filling: Occlusal mismatch creates excessive pressure on the periodontal ligament
Deep caries or pulp involvement: Pulp inflammation due to secondary caries or microleakage
This symptom should be taken seriously, especially if it manifests as localized pain when force is applied to a specific tooth.
How Should Continuous or Intermittent Tooth Pain Be Interpreted?
Progressive secondary caries or bacterial infiltration under the filling can lead to irreversible inflammation in the pulp tissue. This condition presents itself as spontaneous pain, nighttime pain, or prolonged thermal pain.
The character of the pain is important:
Mild, transient sensitivity: Reversible pulp irritation
Severe, spontaneous, increased nighttime pain: Indication of irreversible pulpitis or apical periodontitis
How Is Visible Damage in the Filling Defined?
The following findings are noteworthy during visual examination with a mirror:
Finding | Possible Reasons | Clinical Importance |
Surface cracks | Material fatigue, trauma | Bacterial infiltration risk |
Edge fractures | Occlusal forces, bruxism | Loss of marginal adaptation |
Color change (darkening) | Secondary decay, pigment accumulation | Active carious lesion |
Surface wear | Abrasion, erosion | Functional loss |
When is the loosening or falling of the filling urgent?
The movement or complete detachment of the filling indicates that the bonding mechanism of the restoration has completely failed. This situation requires urgent treatment because:
The internal structure of the tooth (dentin tubules) is exposed
Bacterial infiltration accelerates
The risk of thermal and chemical irritation increases
The risk of tooth fracture rises
In the study by Khurana and colleagues (2025), bonding failure was identified as a reason for failure at a rate of 69.75%.
Why is Surface Roughness or Sharp Edges Important?
The tongue perceives tissue changes in the oral cavity with extreme sensitivity. The roughness felt on the filling surface is an early indicator of cracking or wear. Sharp edges can cause irritation and ulceration on the tongue and soft tissues.
How to Interpret Color Change and Staining?
The darkening seen in the enamel or dentin around the filling (gray, brown, or black spots) may be a radiographic finding of secondary caries. In Brouwer and colleagues' (2016) meta-analysis, the average sensitivity for the visual detection of secondary carious lesions was determined to be 0.50-0.59, and specificity 0.78-0.83.
What Causes Bad Breath and Bad Taste that May Indicate Filling Failure?
Bacterial colonies accumulating under the filling produce volatile sulfur compounds. These compounds cause characteristic bad breath and a metallic taste. Odor that cannot be alleviated by normal oral hygiene procedures (brushing, flossing) suggests microbial accumulation beneath the restoration.
What Does Food Accumulation and Impaction Between Teeth Mean?
Marginal gaps at the edges of the filling cause food particles to become trapped. This condition:
Increases interdental plaque accumulation
Raises the risk of interproximal caries
May lead to periodontal ligament irritation
Gives a sensation of tearing or impaction during flossing
Subjective Symptoms: Signs the Patient May Notice
Proprioception (the conscious perception of body position) is also effective in the mouth. The patient usually does not feel the presence of the filling; however, if the filling is high, loosened, or has lost its anatomical form, the tongue and occlusal proprioceptors perceive this change.
When Should Changes in Bite Sensation Raise Suspicion?
Changes in occlusal sensation indicate variations in the height of the filling or in the position of the tooth. The patient may report a subjective complaint such as, "my tooth contacts differently than before." This is an early sign of excessive pressure on the periodontal ligament.
Why is a High or Incompatible Filling a Risk?
A high filling applies traumatic occlusal forces on the periodontal ligament. This situation:
Leads to hyperemia of the periodontal ligament (increased blood flow)
Causes painful chewing
Can lead to periodontal ligament expansion and mobility in the long term
How is a Gap or Cavity Feeling Defined by the Tongue?
A gap felt with the tip of the tongue may indicate that the filling has started to drop or has broken. The cavity feeling is the subjective perception of enamel and dentin loss due to secondary decay.
What are the Clinical Examination and Diagnostic Methods?
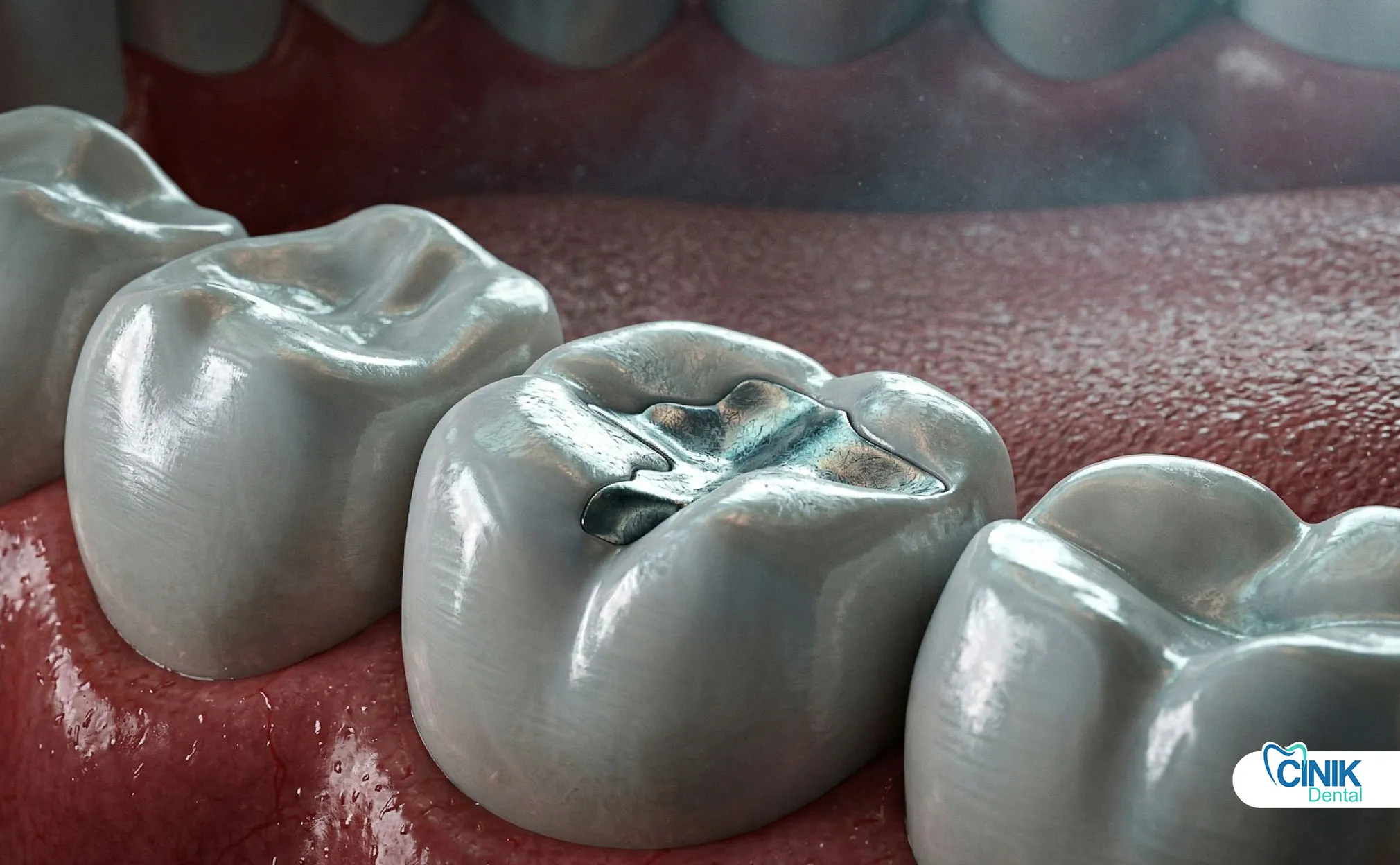
The clinician evaluates the following parameters using a dental mirror and probe:
Marginal adaptation: Step or gap felt with the tip of the probe at the filling-tooth interface
Color and opacity: Changes in restoration and surrounding tissues
Surface integrity: Signs of cracks, fractures, or wear
Contact points: Interdental fit and food packing
How Does Radiographic Examination Show Secondary Caries and Substructure Damage?
The radiographs placed in the mouth while taking dental X-rays are the gold standard for assessing secondary caries in interproximal areas. Radiographic findings:
Radiolucent (dark) appearance under or around the restoration
Uncertainty at the filling-tooth interface
Cavitation or dentin loss
In the study by Espelid and colleagues (1991), the radiopacity of the filling material affects the diagnosis of secondary caries; slightly higher radiopacity than enamel is the best diagnostic criterion.
How Does Occlusal Analysis Assess Bite Forces?
Occlusal contact points are determined using articulating paper. High fillings show a distinct dark contact point. Additionally, occlusal analysis may be necessary for evaluating torsional forces.
What Are the Possible Complications of Faulty Fillings?
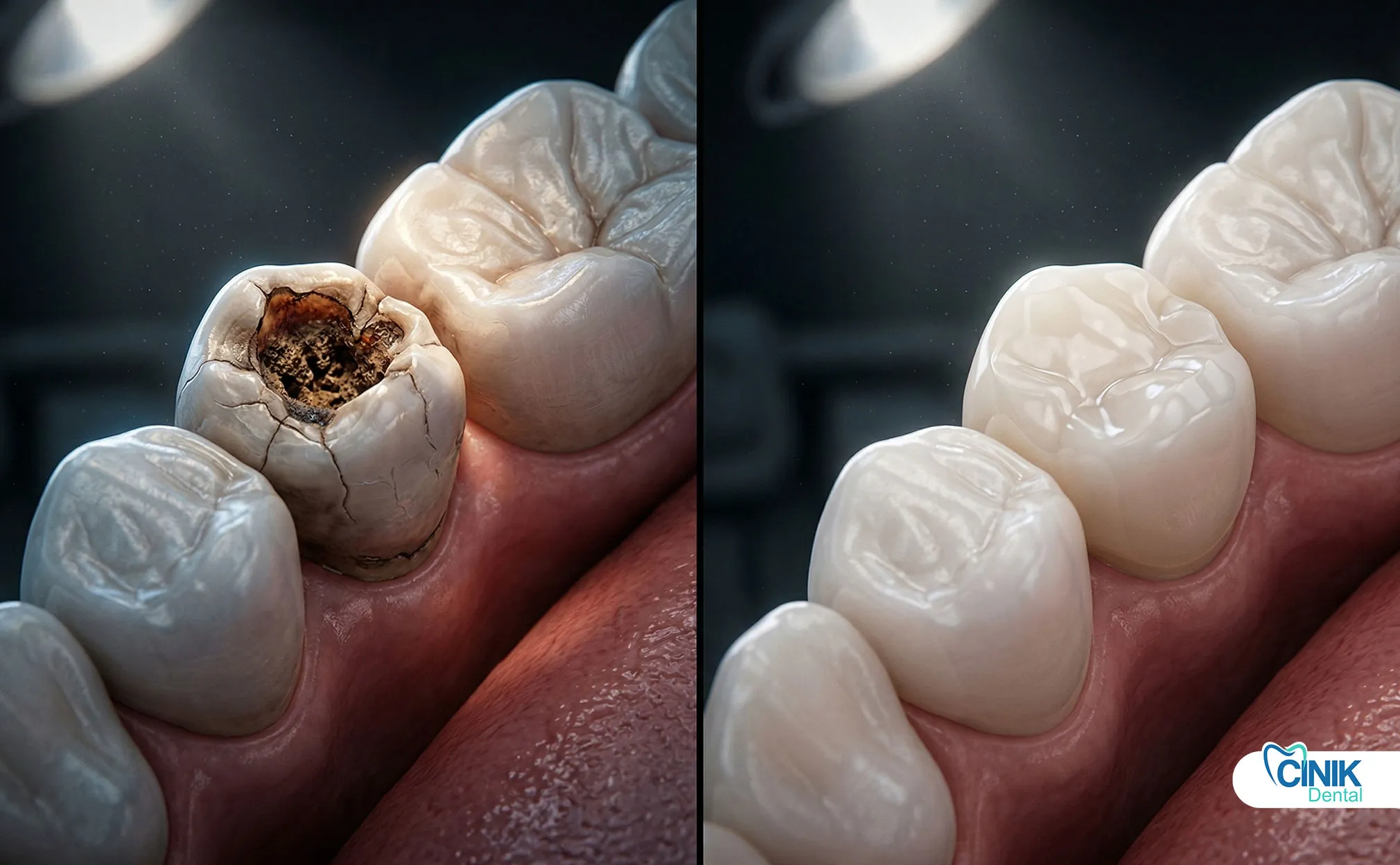
Secondary caries begin below a filling or in the marginal area and progress towards the pulp. In Khurana's (2025) study, secondary caries account for 73.5% of failures. If left untreated:
Enamel and dentin demineralization
Pulp cavity and pulpitis
Periapical infection and abscess
When Does Pulp Infection and Abscess Develop?
Bacterial infiltration under the filling leads to pulp necrosis. This condition:
Spontaneous, severe pain
Long-lasting pain response to thermal stimulation
Periapical radiolucency (root tip infection)
Abscess formation (swelling, pain, trismus)
How Does the Risk of Tooth Fracture Increase?
A loose or cracked filling loses support from the remaining tooth structure. This situation, especially in posterior teeth, can lead to cusp fractures or vertical tooth fractures.
How Do Periodontal Problems Emerge?
Marginal openings and food impaction contribute to interdental plaque accumulation and the development of gingivitis/periodontitis.
When Should One Consult a Dentist?
The following situations require urgent or non-urgent dental evaluation:
Symptom | Urgency | Action |
Severe spontaneous pain | Urgent | Immediate visit |
Filling loss | Urgent | Within 24-48 hours |
Thermal sensitivity (new) | Not urgent | Within a week |
Food blockage | Not urgent | Within a week |
Surface crack | Not urgent | Within two weeks |
Bad taste/smell | Not urgent | Within a week |
What are the treatment approaches?
Small marginal defects or surface cracks can be repaired with composite resin. However, this approach is a temporary solution if the underlying degradation mechanism (microleakage, secondary caries) has not been resolved.
How is filling renewal carried out?
The existing filling is completely removed, the cavity is re-prepared, and a new restoration is placed. This is the preferred approach in the presence of secondary decay or material fatigue.
What are the alternative restorative options?
Option | Indication | Advantage | Disadvantage |
Inlay/Onlay | Large cavities, solid walls | Superior marginal adaptation | Cost, time |
Crown | Wide restorations, after endodontic treatment | Full protection, aesthetic | Invasive, cost |
Composite (direct) | Small-medium cavities | Conservative, economical | Durability limit |
Preventive and Protective Approaches
Brushing with fluoride toothpaste twice a day
Interdental cleaning once a day (dental floss or interproximal brush)
Antiseptic rinses (chlorhexidine) as needed
Why are Regular Dental Check-ups Critical?
Check-ups performed every 6-12 months allow for the diagnosis of early marginal deterioration and secondary caries. Radiographs placed in the mouth during dental X-rays reveal clinically undetectable interproximal lesions.
How to Regulate Diet and Habits?
Avoiding hard foods (ice, hard candies)
Limiting carbonated beverages and using straws
Using a night guard in the presence of bruxism
Avoiding smoking and heavy alcohol consumption (Al-Talib, 2025)
Conclusion
Noticing early signs of faulty dental fillings is crucial for preserving the tooth and preventing invasive treatments. Clinical findings such as thermal sensitivity, chewing pain, visible damage, food impaction, and bad breath should be assessed by the patient and clinician.
Scientific evidence shows that secondary caries and microleakage are the main reasons for failure (Khurana et al., 2025). Therefore, regular check-ups and early intervention play a key role in restorative dentistry. Patient education and proprioceptive awareness help in the early detection of failures.
References
Al-Talib, Tanya, et al. "Bruxism and direct and indirect restorations failure: A scoping review." Journal of Dentistry, vol. 145, 2025, pp. 105470. https://doi.org/10.1016/j.jdent.2025.105470
Brouwer, F., et al. "Detecting Secondary Caries Lesions: A Systematic Review and Meta-analysis." Journal of Dental Research, vol. 95, no. 2, 2016, pp. 143-151. https://doi.org/10.1177/0022034515611041
Espelid, I., et al. "Radiopacity of restorations and detection of secondary caries." Dental Materials, vol. 7, no. 2, 1991, pp. 114-117. https://doi.org/10.1016/S0109-5641(05)80005-8
Khurana, Surbhi, et al. "Incidence of restoration failure and its etiology: A retrospective study." Journal of Conservative Dentistry and Endodontics, vol. 28, no. 1, 2025, pp. 23-29. https://doi.org/10.4103/JCDE.JCDE_123_24
Opdam, N. J., et al. "Longevity of restorations: The 'death spiral'." Dental Materials, vol. 20, no. 9, 2004, pp. 840-843. https://doi.org/10.1016/j.dental.2004.03.001
Tabassum, Rubina, et al. "Ceramic Dental Restorations And Sleep Bruxism: Failure Rates And Clinical Implications: A Systematic Review And Meta-Analysis." South Eastern European Journal of Public Health, 2025, pp. 126-141. https://doi.org/10.70135/seejph.vi.7025