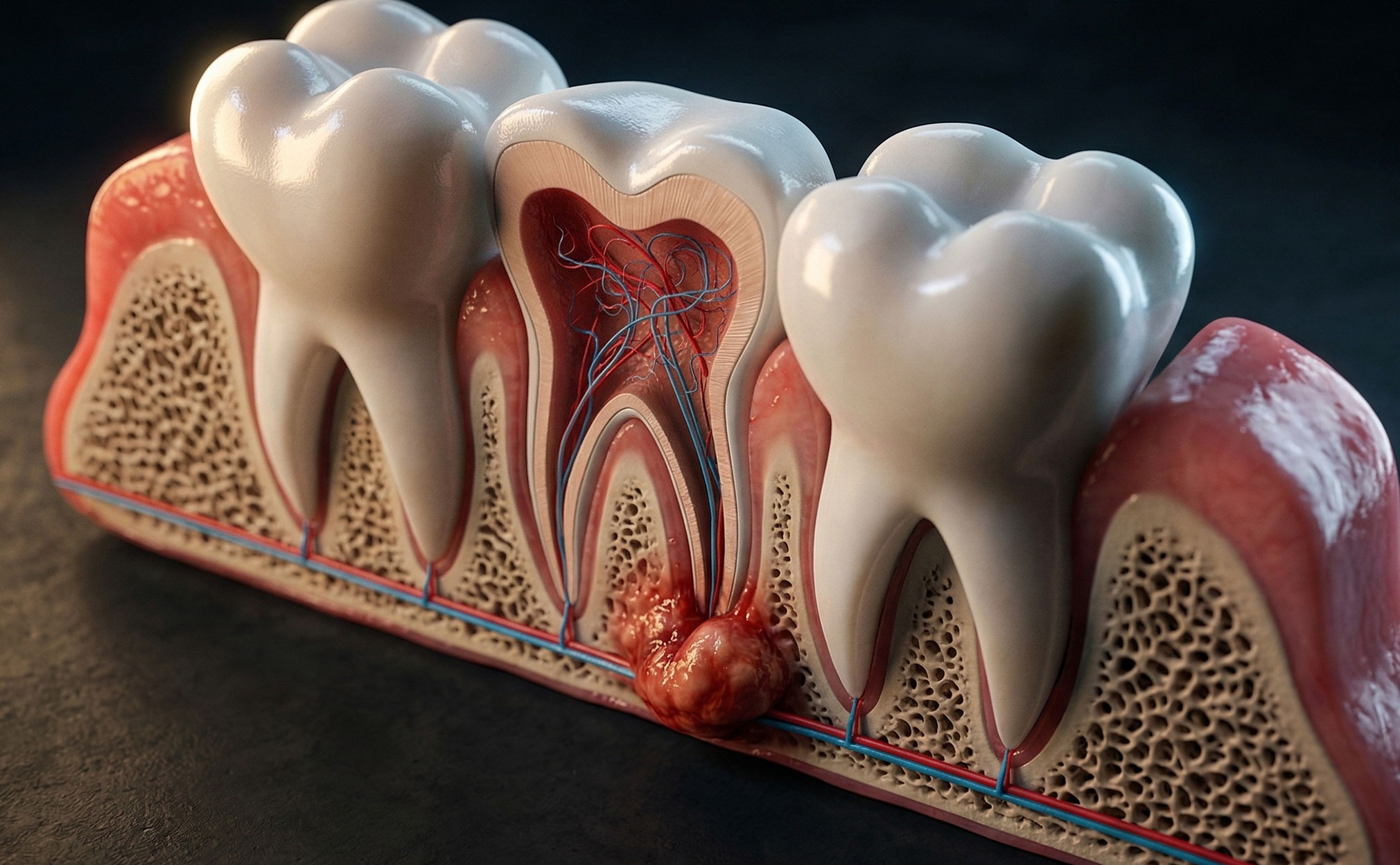
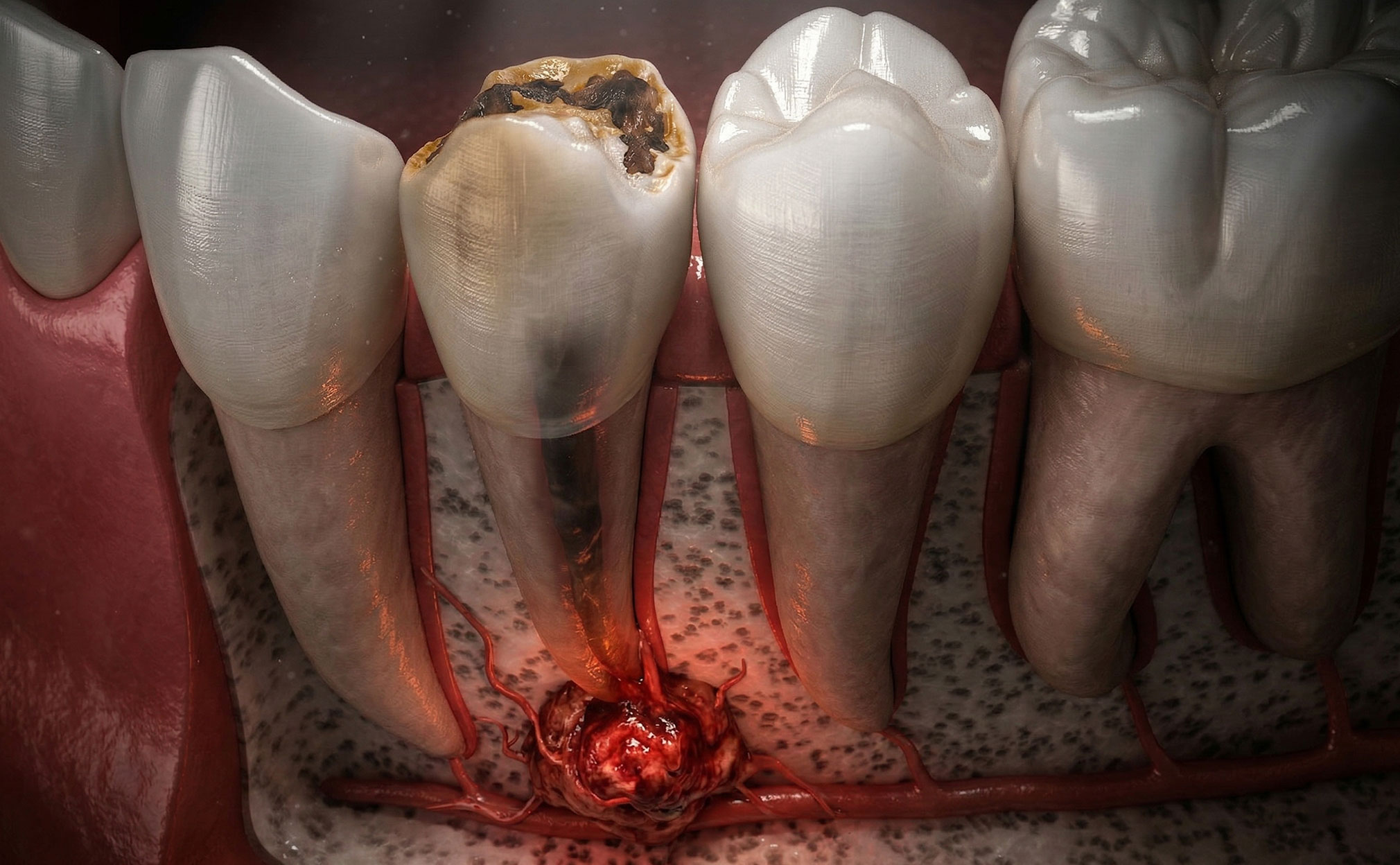
Dental cysts are abnormal, fluid-filled cavities that can form in the jawbone, in association with teeth, or within soft tissues of the mouth. They are most often seen at the roots of teeth that have not properly developed, died, or been weakened by previous trauma or infection. Problems that lead to the formation of cysts include untreated tooth decay or abscess, protein build-up from failed tooth emergence, tooth grating, and severe jawbone fractures. Developmental cysts can also appear around healthy teeth and remain asymptomatic for years. Cysts generally have an ordinary growth pattern. When a diseased or dying tooth comes to the attention of a dental professional, the cyst may be diagnosed early, allowing primary treatment of the cyst while preserving the tooth. Unfortunately, early detection is not always achievable, leading to potential rupturing of cyst walls, necrosis of surrounding bony areas, significant swelling, and drainage of infectious material (Bhardwaj et al., 2016) (Ruslin et al., 2022).
1. What are the main reasons to develop dental cysts?
Quick Answer: Dental cysts mainly develop due to pulp necrosis, dental trauma, infection during tooth development, abnormal tooth eruption in children, and failed or old root canal treatments.
Dental cysts can develop for multiple reasons:
Cause / Condition | Resulting Cyst Type | Description |
Pulp necrosis from caries, trauma, periodontal disease, or tooth fracture | Radicular cyst | Dead pulp tissue triggers cyst formation at the tooth root. |
Dental trauma (fracture, avulsion, luxation, tooth mobility) | Radicular cyst | Physical injury initiates inflammatory cyst development. |
Infection during tooth development (pulp necrosis, caries, periodontal inflammation) | Radicular or dentigerous cyst | Cyst type depends on the stage of tooth development. |
Ectopic eruption of permanent teeth in children | Dentigerous cyst | Abnormally positioned teeth become surrounded by cystic tissue. |
Persistent pulp necrosis after old root canal filling | Radicular cyst | Incomplete or failed endodontic treatment leads to cyst formation. |
2. What are the common signs and warning symptoms?
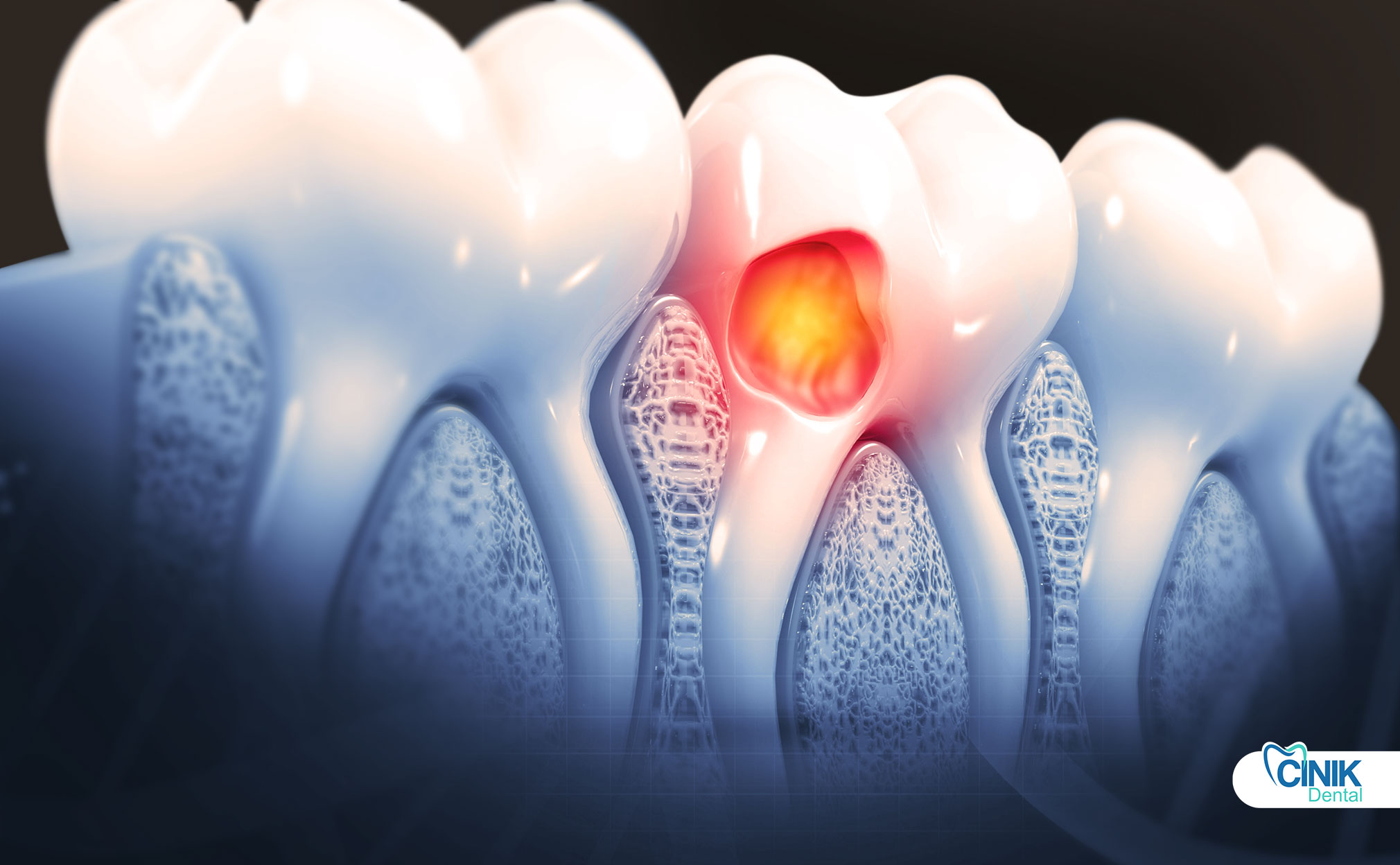
Quick Answer: Dental cysts often cause no symptoms at first but may present with swelling, pain, tooth mobility, bite changes, or drainage. Severe pain and swelling usually indicate infection and prompt diagnosis.
Dental cysts often do not cause visible signs of problems in their early stages. However, certain warning symptoms may indicate the presence of a cyst (Ruslin et al., 2022). The most common early warning signs include swelling, pain, tooth mobility, changes in the bite, and drainage. Warning signs tend to remain mild when a cyst is still small. Many cysts are even discovered incidentally on X-rays when all other components of the dental examination are unremarkable. Most alarming early warning signs, particularly intense pain, swelling, and drainage, suggest the cyst has become infected, which is the most frequent reason to seek medical attention.
Swelling of the gum or face near a tooth is one of the earliest signs of a dental cyst. The swelling may be barely visible or readily apparent and may not occur if the cyst is in a hard tissue area such as the jawbone. Swelling is often accompanied by discomfort. Some patients note generalized sensitivity to touch, while others report sharp pains that may radiate to nearby teeth or muscles, sometimes feeling like earache or blocked sinuses. In the lower jaw, cyst-related swelling may also cause difficulty in opening the mouth. Cysts affecting teeth that are already loose or deemed hopeless during the examination may cause little or no initial discomfort or swelling.
3. Do dental cysts pose health risks?
Quick Answer: Dental cysts are usually harmless but may become dangerous if infected or, rarely, cancerous.
Dental cysts can pose health risks for both jawbone and overall health. In most cases, however, they cause few problems beyond initial discomfort. Cysts usually only pose serious health effects in two situations. First, having a cyst can carry the risk that the cyst will become infected, especially if left untreated. Second, in rare cases, cysts can become cancerous and may need to be removed for that reason (Kothari et al., 2024).
4. What are the methods used to detect dental cysts?
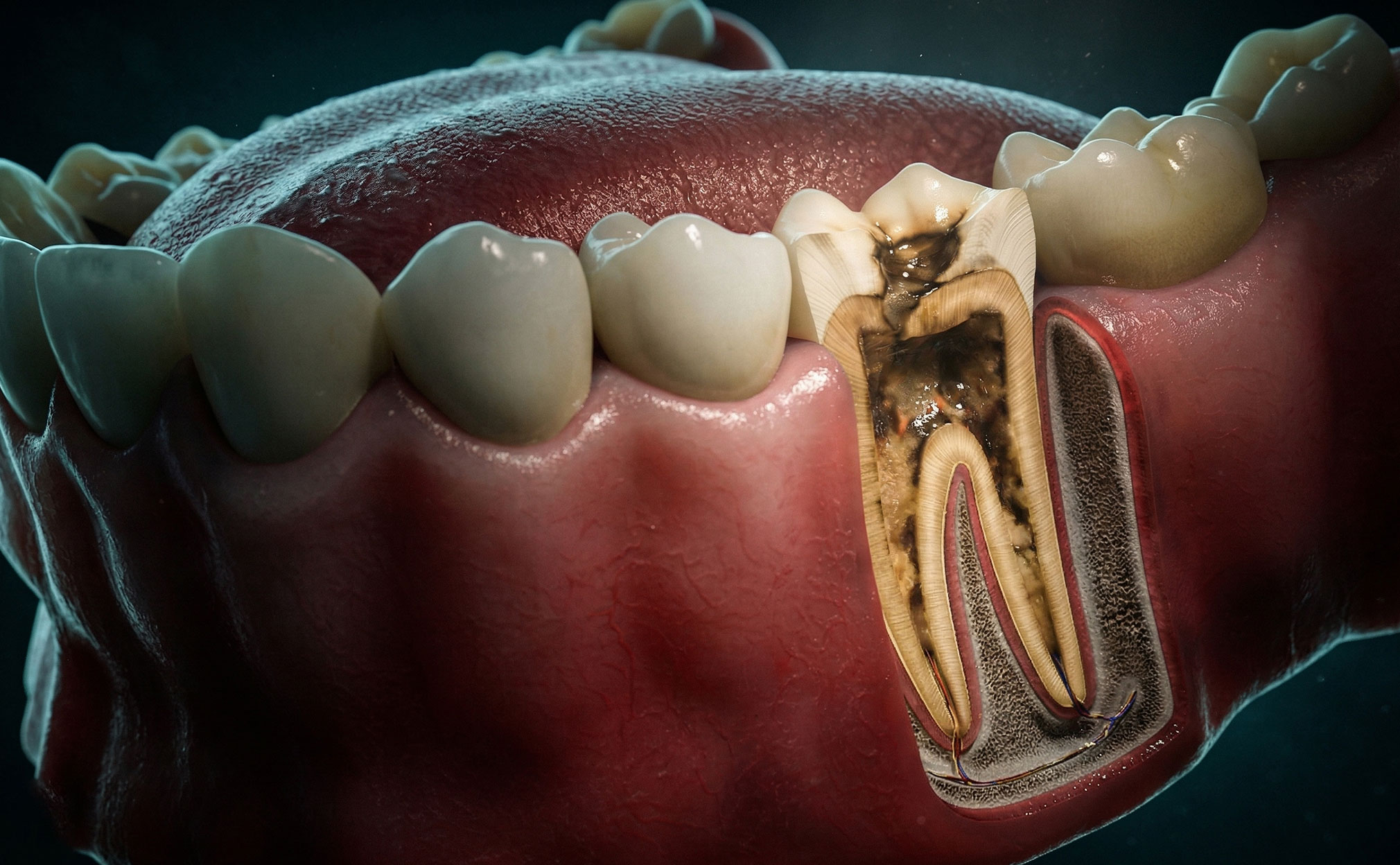
Quick Answer: Dental cysts are detected through dental exams and imaging such as X-rays, panoramic or periapical scans, and sometimes CT scans or biopsy if the lesion appears suspicious.
A dental exam can often identify cysts in the mouth. The dentist may look for puffiness, drainage, or tooth mobility. Changes in the bite may indicate problems below the gums. Cyst-like growths that turn up in routine checks are still worth monitoring.
X-rays can show the size of the cyst and its exact position. Most dental practices use panoramic X-rays, which capture the whole mouth. Periapical X-rays focus on one or two specific areas. Cysts appearing on panoramic images often match the final diagnosis. If X-rays do not clarify the condition, a CT scan may help. These tests take only a few minutes and provide instant results. Lesions that seem dangerous can lead to a biopsy.
5. What are the available treatment options for dental cysts?
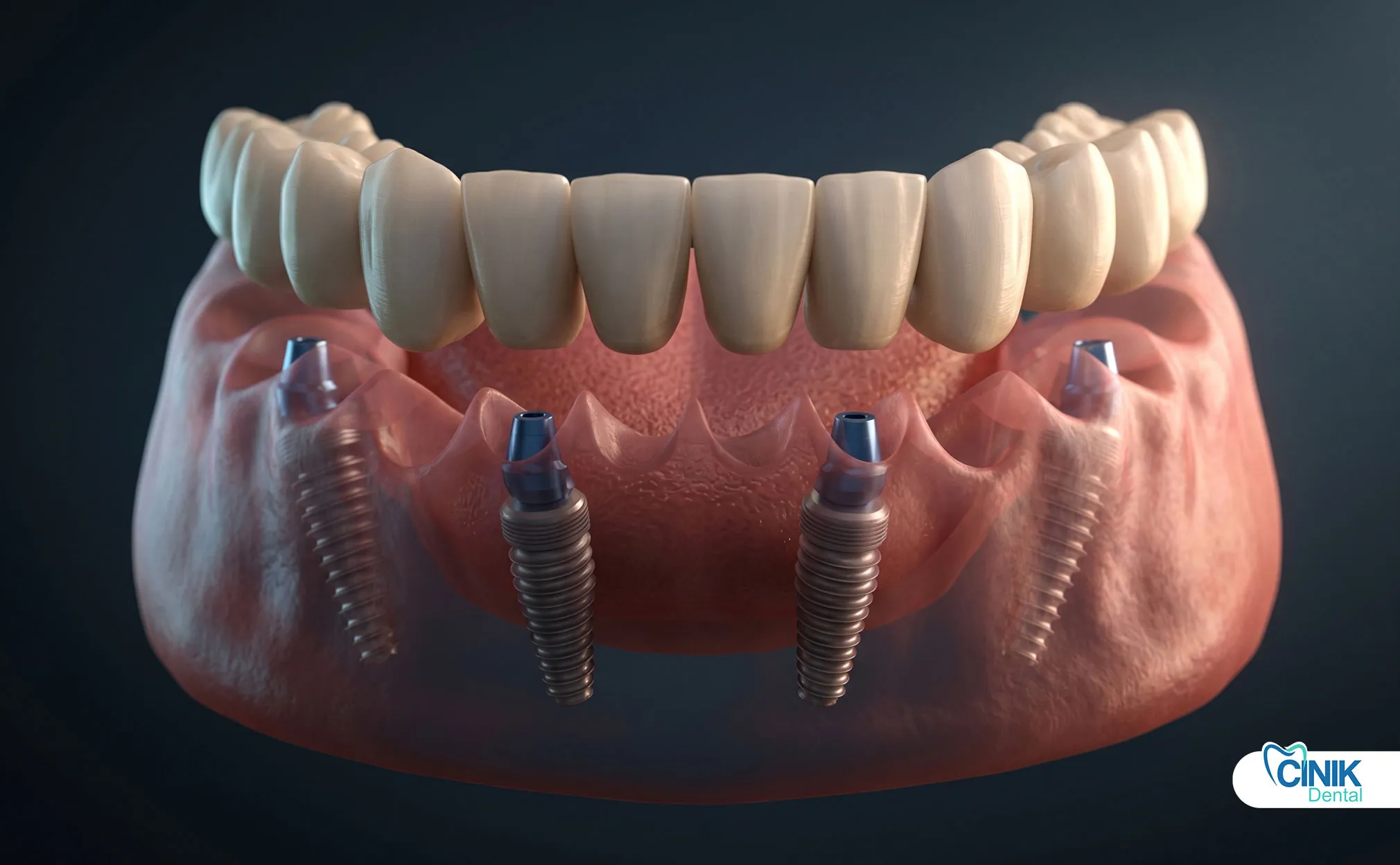
Quick Answer: Dental cysts are treated by surgical removal or drainage, often combined with root canal treatment to save the tooth, and antibiotics are used only if infection is present.
Dental cysts can be treated through various options, often involving a dental professional's evaluation and possible referral to a specialist. For simple cysts, surgical removal is frequently recommended, with integumentary lesions being entirely excised, and remaining cavities may be drained or packed with antibacterial foam. If tooth pulp is compromised due to infection, root canal treatment may be necessary to restore functionality and aesthetics. The primary treatment goals are to remove the cyst and save the tooth, which is crucial for maintaining oral health. Complications can arise from cysts related to tooth decay or trauma. Another option is to drain and disinfect the cyst cavity, especially in cases of progressed oral periapical cysts. Inadequately treated intra-bone teeth can contribute to cyst growth. Endodontic preparation aids in cleaning and disinfecting the root canal. Protecting the tooth with sterile dressings is essential to prevent contamination. If the cyst shows signs of infection, direct drainage through a muco-buccal flap may be considered, allowing for better access. Continuous drainage through absorbable sutures helps manage the cyst and reduces surgical risks. Antibiotics may be used if an acute infection is present, but asymptomatic cysts allowing root apex clearance can proceed with endodontic treatment without them. (Fidele Nyimi et al., 2019)(Niu et al., 2024)
6. What are the ways to reduce the risk of tooth root complications?
Quick Answer: To reduce the risk of tooth root complications, maintain good oral hygiene, attend regular dental checkups, treat decay or injuries early, monitor at-risk teeth with X-rays, and follow a healthy diet low in sugar.
To limit the chance of complications in a tooth’s root, patients can take a number of preventive steps. First, maintain good oral hygiene. Clean teeth and gums habitually by brushing twice a day, flossing daily, and using an antimicrobial mouthwash regularly. Professional teeth cleaning and oral checkups also help protect dental health. Ideally, see a dentist every six months or as often as recommended. During checkups, dentists evaluate mouth, teeth, and gums, check for decay or other problems and diagnose conditions early. Detecting tooth decay or infection early is essential. Treatments are usually easy, inexpensive, and effective. At the first sign of decay, discoloration, sensitivity, or other troublesome symptoms, consult a dentist (Kothari et al., 2024). Treat teeth carefully after trauma. Injuries to teeth or other parts of the mouth can damage or expose tooth roots and lead to complications. After any dental impact, fracture, or other trauma, have an oral assessment done. For teeth at risk of cyst development, follow an added practice. Timely radiographs evaluated every six to twelve months can assess the size and condition of teeth involved in a cyst. Keep a healthy lifestyle. Eat balanced and nutritious-based meals. Avoid excessive sugar and hard snacks. Limit between-meal snacks to aid in cavity control.
7. Conclusion
Dental cysts can occur in up to 40% of the population during their lifetime (Ruslin et al., 2022).
Odontogenic cysts are a variety of dental cysts with origins in the tissues. Odontogenic cysts may appear as painless hard lumps associated with teeth, and they sometimes cause tooth mobility or discomfort following challenges such as filling the cavity and may be incidental findings of radiographic examinations. Most odontogenic cysts develop at the naive stage of tooth formation following injury to the tooth bud or pulp. Because odontogenic cysts develop from dental structures, they cannot be treated by extracting the associated tooth; other locally invasive treatments may be indicated (Fidele Nyimi et al., 2019).
References:
Bhardwaj, B., Sharma, S., Chitlangia, P., Agarwal, P., Bhamboo, A., and Rastogi, K. "Mandibular Dentigerous Cyst in a 10-Year-Old Child." 2016. ncbi.nlm.nih.gov
Ruslin, M., N. van Trikt, K., Yusuf, A. S. H., Tajrin, A., Fauzi, A., Rasul, M. I., Boffano, P., and Forouzanfar, T. "Epidemiology, treatment, and recurrence of odontogenic and non-odontogenic cysts in South Sulawesi, Indonesia: A 6-year retrospective study." 2022. ncbi.nlm.nih.gov
Kothari, A., V Shinde, V., Ingale, M., and Devi Putta, S. "Dentigerous Cyst in a Pediatric Patient: A Case Report." 2024. ncbi.nlm.nih.gov
Fidele Nyimi, B., Yifang, Z., and Liu, B. "The Changing Landscape in Treatment of Cystic Lesions of the Jaws." 2019. ncbi.nlm.nih.gov
Niu, G., Zhang, G. H., Chen, J., Wang, T., Wu, Y., Lu, Y. G., and Lin, L. "A 3-year follow-up clinical study on the preservation for vitality of involved tooth in jaw cysts through an innovative method." 2024. ncbi.nlm.nih.gov