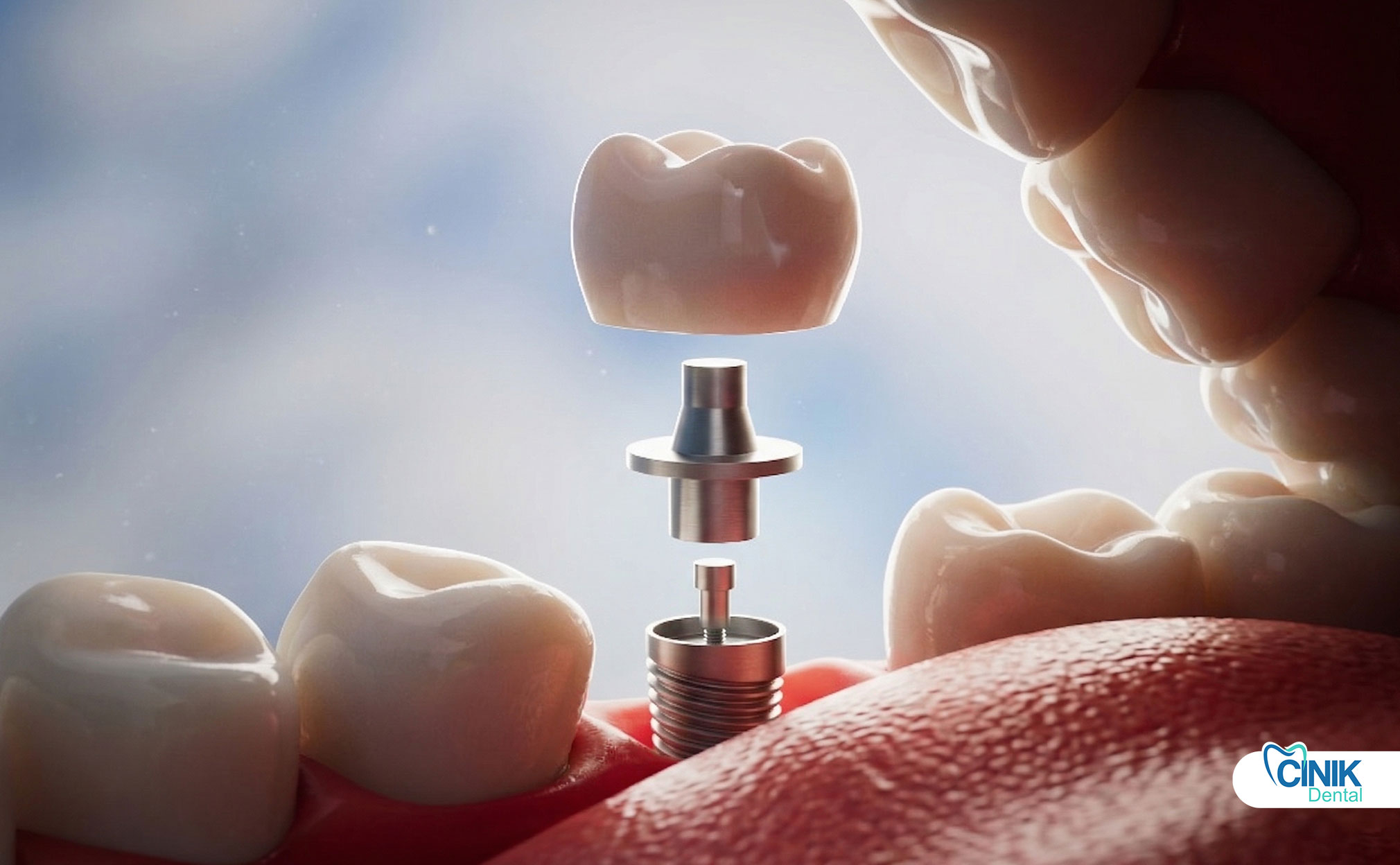
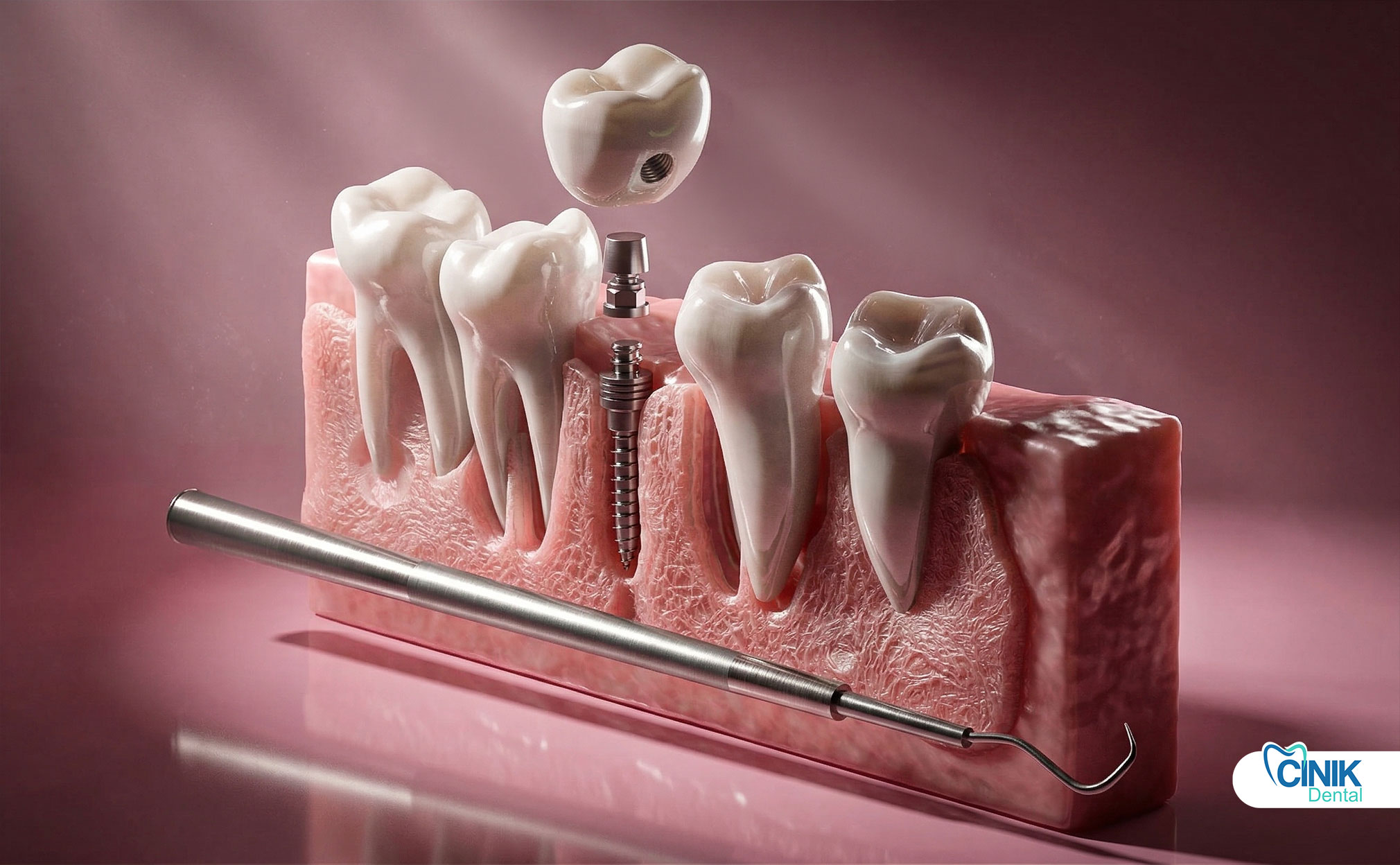
A dental implant abutment is a connector component that links the implant fixture (in the bone) to the prosthetic restoration such as a crown, bridge, or denture. It serves as the critical intermediary structure that transfers chewing forces, maintains soft tissue architecture, and ensures long-term stability of the entire implant system.
What Is a Dental Implant Abutment in Implantology?
It is the intermediate structure that provides retention, stability, and load transfer between implant and prosthesis. The abutment emerges through the gum tissue and creates the foundation for the visible tooth replacement.
Core Definition and Terminology
The dental implant abutment functions as the connector between the implant fixture embedded in the jawbone and the final prosthetic crown visible in the mouth. Positioned above the gum line, this component acts as the "neck" of the implant system. The term "abutment" originates from engineering architecture, where it describes a structural support that bears weight and transfers loads between two elements.
In modern implantology, the abutment serves three primary functions. First, it provides mechanical retention for the prosthetic restoration. Second, it transfers occlusal forces from the chewing surface down through the implant fixture and into the surrounding bone. Third, it shapes the soft tissue emergence profile, creating a natural-looking transition between the implant and the gum tissue.
Components of a Dental Implant System
A complete dental implant restoration consists of three distinct components working in harmony:
Component | Location | Primary Function |
Implant Fixture | Embedded within the jawbone | Acts as an artificial root, providing anchorage through osseointegration |
Abutment | Protrudes through the gum tissue | Connects the implant to the prosthesis, transfers loads, shapes soft tissue |
Prosthesis | Visible above the gum line | Restores chewing function and aesthetics (crown, bridge, or denture) |
The implant fixture typically consists of titanium or titanium alloy, featuring a threaded design that maximizes surface area for bone integration. The abutment attaches to this fixture through various connection mechanisms. The prosthetic crown then attaches to the abutment either through cementation or screw retention.
Biological and Mechanical Role
The abutment performs critical biological and mechanical functions that determine implant success. Mechanically, it distributes chewing forces to the surrounding bone. Research demonstrates that proper load distribution prevents stress concentrations that could lead to bone resorption or component failure (Nie et al., 2023) .
Biologically, the abutment shapes the soft tissue emergence profile. This emergence profile refers to the contour of the gum tissue as it transitions from the narrow implant platform to the wider crown dimensions. A properly designed emergence profile mimics natural tooth anatomy and prevents food impaction while maintaining aesthetic harmony with adjacent teeth.
The abutment also maintains the biological seal, the barrier between the oral environment and the underlying bone. A stable implant-abutment connection minimizes microleakage, which reduces bacterial infiltration and protects the peri-implant tissues from inflammation.
Why Is the Abutment Critical for Implant Success?

The abutment determines long-term stability, aesthetics, and biomechanical performance of the implant. Poor abutment selection leads to mechanical failures, biological complications, and compromised treatment outcomes.
Mechanical Stability and Load Transfer
The abutment serves as the primary load transfer mechanism in the implant system. When you chew, forces travel from the crown through the abutment and into the implant fixture. The screw-joint mechanism at the implant-abutment interface must withstand these forces without loosening or fracturing.
Research using finite element analysis reveals that connection design significantly affects stress distribution. Internal connections demonstrate superior biomechanical efficiency compared to external connections, offering better stress distribution and enhanced stability (Dave, 2023) . The Morse taper connection, featuring a conical interface with precise friction fit, creates a "cold-welded" effect that minimizes micromovement and reduces stress concentrations at the crestal bone level.
Stress distribution patterns vary based on loading conditions. Axial loads (straight down) distribute relatively evenly across all connection types. However, oblique loads (angled forces common during chewing) create significantly higher stress concentrations. Studies show that internal connections handle off-center loading more effectively than external hex designs, reducing the risk of screw loosening and bone resorption.
Prosthetic Retention and Fit
The abutment determines how the final crown attaches to the implant system. Two primary retention mechanisms exist:
Cement-Retained Abutments: These abutments feature a prepared post (similar to a natural tooth prepared for a crown) that allows the prosthesis to cement permanently into place. This approach offers superior aesthetics because no screw access hole interrupts the occlusal surface. However, cement remnants below the gum line pose a documented risk factor for peri-implant inflammation.
Screw-Retained Abutments: These abutments incorporate a screw channel that passes through the abutment and crown. The prosthesis screws directly onto the abutment, enabling easy retrievability for maintenance or repair. The trade-off involves a visible screw access hole, typically filled with composite resin, which may compromise aesthetics in certain locations.
Modern abutments often incorporate anti-rotational features, geometric designs that prevent the abutment from rotating relative to the implant. These features include hexagonal, octagonal, or star-shaped internal connections that transfer rotational forces away from the retaining screw.
Biological Seal and Tissue Integration
The soft tissue interface around the abutment determines long-term biological stability. The abutment surface must promote healthy soft tissue attachment while resisting bacterial colonization. Research comparing titanium and zirconia abutments reveals that zirconia demonstrates lower plaque accumulation due to reduced surface energy, potentially contributing to better peri-implant tissue health (Pandey et al., 2019) .
The emergence profile created by the abutment shape influences soft tissue contouring. A properly contoured abutment supports the gingival margin and papilla (gum tissue between teeth), preventing recession and black triangles that compromise aesthetics. Custom abutments allow precise emergence profile optimization based on individual tissue thickness and tooth position.
Microleakage at the implant-abutment interface represents a significant biological concern. Even microscopic gaps allow bacterial infiltration, potentially triggering inflammation and bone loss. Connection designs featuring Morse taper or platform switching concepts minimize these microgaps, enhancing the biological seal.
What Are the Types of Dental Implant Abutments?
Abutments are classified based on design, fabrication method, retention, and clinical indication. The main categories include standard prefabricated abutments, custom CAD/CAM abutments, angled abutments, healing abutments, and multi-unit abutments for complex restorations.
Standard (Prefabricated) Abutments
Standard abutments are mass-produced components available in various sizes, angles, and cuff heights. Manufacturers produce these abutments to fit specific implant systems, offering cost-effective solutions for straightforward cases.
Advantages:
Lower cost compared to custom alternatives
Immediate availability (no laboratory fabrication time)
Proven designs with established clinical track records
Simplified inventory management for dental practices
Limitations:
Limited customization for unique clinical situations
Generic emergence profiles may not match patient anatomy
Fixed angles and cuff heights restrict application in challenging cases
Potential for visible metal margins in aesthetic zones
Standard abutments work well in posterior regions where aesthetic demands are lower and implant positioning is ideal. However, they often prove inadequate for anterior restorations requiring precise tissue management and optimal emergence profiles.
Custom Abutments (CAD/CAM)
Computer-aided design and computer-aided manufacturing (CAD/CAM) technology enables patient-specific abutment fabrication. Digital impressions capture the implant position and surrounding tissue architecture, allowing technicians to design abutments that match individual anatomical requirements.
Benefits of Custom Abutments:
Optimized emergence profile for natural tissue contouring
Corrected angulation for misaligned implants
Ideal margin placement (supragingival, equigingival, or subgingival)
Material selection based on aesthetic and functional needs
Better soft tissue adaptation and long-term stability
Research confirms that customized abutments yield comparable survival rates and aesthetic outcomes to prefabricated alternatives, with follow-up studies extending to 13 years (Alagarsamy et al., 2024) . The ability to position the crown margin precisely at or above the gum line simplifies cement removal and reduces biological complications.
Angled Abutments
Angled abutments correct implant misalignment without requiring surgical repositioning. These abutments feature pre-manufactured angles (typically 15°, 20°, or 30°) that redirect the prosthetic crown into proper alignment with adjacent teeth.
Clinical Applications:
Compensating for tilted implants in full-arch restorations
Correcting facial or lingual implant inclination
Aligning crowns in limited mouth opening situations
Aesthetic zone restorations requiring precise crown positioning
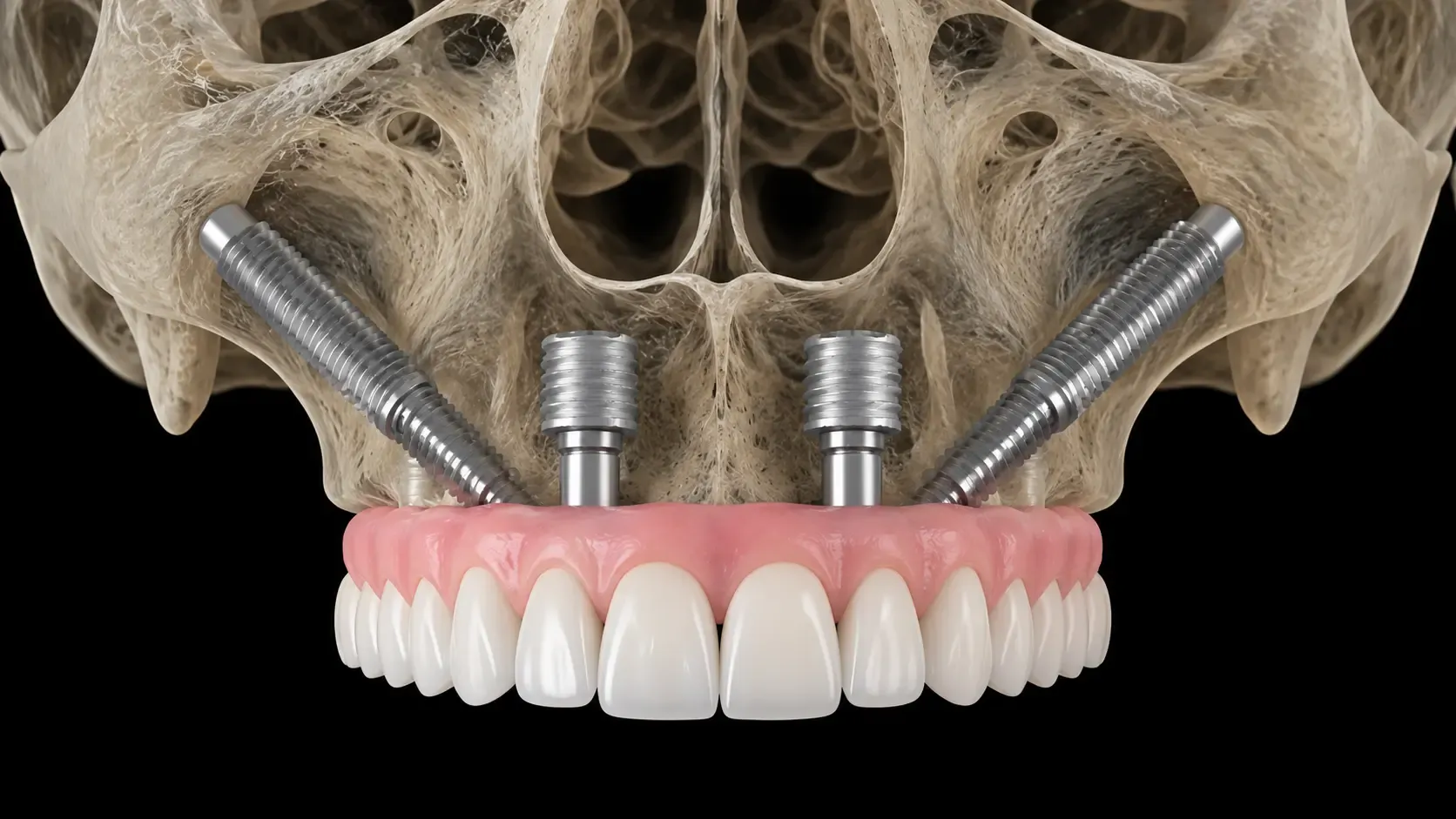
Angled abutments prove particularly valuable in the All-on-4 and All-on-6 treatment concepts, where posterior implants are intentionally tilted to maximize bone utilization and avoid anatomical structures. The angled abutment corrects this tilt, allowing the prosthesis to align properly with the opposing dentition.
Healing Abutments
Healing abutments are temporary components placed during the initial healing phase. These abutments are not designed to support final prostheses but rather to shape the soft tissue and protect the implant during osseointegration.
Functions:
Guide soft tissue healing around the implant
Prevent tissue collapse over the implant platform
Allow access for impression procedures
Maintain the pathway for final abutment placement
Healing abutments are typically shorter than final abutments and feature smooth, rounded contours that encourage healthy tissue formation. They are removed and replaced with definitive abutments once osseointegration is complete and the final restoration is ready for fabrication.
Multi-Unit Abutments
Multi-unit abutments are specialized components used in full-arch restorations such as All-on-4 and All-on-6 protocols. These abutments feature a standardized connection interface that accommodates a prefabricated prosthetic framework.
Key Characteristics:
Parallelized connection platform for prosthesis seating
Reduced number of components requiring precision fit
Simplified passive fit achievement for full-arch frameworks
Available in various angles (0°, 17°, 30°) for implant alignment correction
The multi-unit abutment system transforms multiple individual implant connections into a unified prosthetic platform, significantly simplifying the fabrication of full-arch restorations.
Hybrid and Specialized Abutments
Advanced prosthetic solutions include several specialized abutment types:
Ti-Base Abutments: These hybrid components combine a titanium base (for strength and implant connection) with a zirconia or ceramic upper structure (for aesthetics). The titanium provides reliable screw retention and mechanical stability, while the ceramic offers superior soft tissue integration and aesthetic outcomes.
Zirconia Abutments: Monolithic zirconia abutments provide excellent aesthetics, particularly in thin tissue biotypes where metal might show through. However, research indicates that zirconia abutments have lower fracture resistance compared to titanium, especially in posterior regions with high occlusal forces (Sanz-Martín et al., 2022) .
Castable Abutments: These plastic or wax patterns allow custom casting in precious or non-precious alloys. While less common with CAD/CAM prevalence, castable abutments remain useful for complex cases requiring specific alloy properties.
Classification Based on Retention Mechanism
Abutments differ in how they retain the prosthesis. The three main categories are cement-retained, screw-retained, and hybrid retention systems, each offering distinct advantages for specific clinical situations.
Cement-Retained Abutments
Cement-retained abutments function similarly to traditional crown preparations on natural teeth. The abutment features a tapered or parallel post that receives a permanently cemented crown.
Advantages:
Superior aesthetics (no screw access hole)
Easier to achieve passive fit on multi-unit restorations
Familiar cementation technique for most clinicians
Lower profile abutment design possible
Disadvantages:
Risk of subgingival cement remnants causing peri-implantitis
Difficult retrieval for maintenance or repair
Potential for cement washout over time
Challenges with margin location in deep subgingival situations
Research emphasizes the importance of supragingival or equigingival margin placement with cement-retained abutments. Subgingival cement remnants act as a nidus for bacterial accumulation, triggering inflammation and progressive bone loss. Careful cement application techniques and thorough removal protocols are essential for biological success.
Screw-Retained Abutments
Screw-retained abutments incorporate a screw channel that allows the prosthesis to attach mechanically without cement. The crown features a precision-milled intaglio surface that fits onto the abutment, secured by a prosthetic screw passing through both components.
Advantages:
Complete retrievability for maintenance or modification
No cement-related biological risks
Predictable retention force
Simplified repair procedures
Disadvantages:
Screw access hole compromises occlusal anatomy
Aesthetic challenges in anterior teeth
Potential for screw loosening over time
Requires adequate interocclusal space for screw head
Screw-retained restorations are particularly indicated for full-arch prostheses, long-span bridges, and situations requiring future retrievability. The ability to remove the prosthesis facilitates professional maintenance and simplifies future modifications.
Hybrid Retention Systems
Hybrid systems combine elements of both cement and screw retention. These approaches aim to maximize the advantages of each system while minimizing their respective drawbacks.
Common Hybrid Approaches:
Screw-retained abutments with cemented crowns (screw-accessible cemented restorations)
Ti-base abutments with screw retention through the ceramic structure
Overdenture attachments combining mechanical retention with tissue support
The screw-accessible cemented restoration represents a popular hybrid approach. The crown is cemented to a screw-retained abutment, but the screw channel remains accessible through the occlusal surface. This allows cement removal from the accessible abutment surface while maintaining retrievability through the screw access.
Materials Used in Implant Abutments
Common materials include titanium and zirconia, chosen for strength and biocompatibility. Gold alloys and cobalt-chromium serve specialized applications, while material selection depends on aesthetic requirements, functional loads, and tissue characteristics.
Titanium Abutments
Titanium abutments remain the gold standard for implant prosthetics. Commercially pure titanium (Grade IV) and titanium alloy (Ti-6Al-4V, Grade V) offer exceptional properties for implant applications.
Material Properties:
Excellent biocompatibility with osseointegration capability
High strength-to-weight ratio
Corrosion resistance in oral environment
Modulus of elasticity closer to bone than ceramics
Proven long-term clinical track record
Recent finite element analysis research demonstrates that titanium abutments exhibit favorable stress distribution patterns. Under oblique loading conditions, titanium's ductility allows it to absorb and redistribute loads, mitigating catastrophic failure (Alagarsamy et al., 2024) . The elastic modulus of titanium (110 GPa) more closely approximates bone (13-20 GPa) compared to zirconia (210 GPa), potentially reducing stress concentrations at the bone-implant interface.
Clinical Considerations:
Potential for grey line visibility in thin tissue biotypes
Surface treatment affects soft tissue response
Plasma argon cleaning reduces bone loss compared to steam cleaning
Suitable for all regions including high-load posterior areas
Zirconia Abutments
Zirconium dioxide (zirconia) abutments address aesthetic limitations of metal components. Yttria-stabilized tetragonal zirconia polycrystal (Y-TZP) offers high strength and biocompatibility with superior optical properties.
Aesthetic Advantages:
Tooth-colored appearance eliminates metal show-through
Better soft tissue color match compared to titanium
Light transmission similar to natural tooth structure
Reduced soft tissue discoloration in thin biotypes
Research comparing titanium and zirconia abutments reveals important biological differences. Studies demonstrate that zirconia abutments exhibit less plaque accumulation due to lower surface energy, potentially contributing to improved peri-implant tissue health (Pandey et al., 2019) . Additionally, zirconia promotes favorable microcirculatory dynamics in peri-implant mucosa, with blood flow patterns closer to natural teeth.
Mechanical Limitations:
Higher fracture risk compared to titanium, particularly in posterior regions
Reduced fracture toughness under humid conditions (oral environment)
Veneer chipping concerns with layered restorations
Higher modulus of elasticity may increase stress transmission to bone
Systematic reviews indicate that zirconia abutments show slightly higher biological complication rates compared to titanium, though the differences are not statistically significant in most studies (Sanz-Martín et al., 2022) . For high-load posterior applications, titanium remains the mechanically superior choice.
Gold and Alloy Abutments
Cast gold alloys and cobalt-chromium abutments serve specialized applications in implant dentistry.
Gold Alloy Abutments:
Excellent castability for complex custom shapes
Biocompatibility and tissue tolerance
Favorable wear characteristics against opposing dentition
Higher cost and limited indications in modern practice
Cobalt-Chromium Abutments:
High strength for narrow-diameter situations
Cost-effective alternative to precious metals
CAD/CAM milling compatibility
Potential for allergic reactions in sensitive patients
Recent research examining cobalt-chromium-molybdenum abutments suggests that soft-milled Co-Cr-Mo may offer favorable stress distribution characteristics, though titanium maintains superior overall performance (Alagarsamy et al., 2024) .
Material Selection Criteria
Selecting the appropriate abutment material requires balancing multiple factors:
Factor | Titanium Abutment | Zirconia Abutment |
Aesthetics | Moderate (metal color) | Excellent (tooth color) |
Strength | Excellent | Good (caution in posterior) |
Soft tissue response | Good | Excellent (less plaque) |
Bone preservation | Good | Slightly better (some studies) |
Cost | Moderate | Higher |
Retrievability | Excellent | Good (careful handling) |
Decision Guidelines:
Anterior zones with thin tissue: Zirconia preferred for aesthetics
Posterior high-load regions: Titanium recommended for strength
Full-arch restorations: Titanium or Ti-base for reliability
Patients with metal sensitivities: Zirconia or titanium (commercially pure)
Dental Implant Abutment Procedure (Step-by-Step)
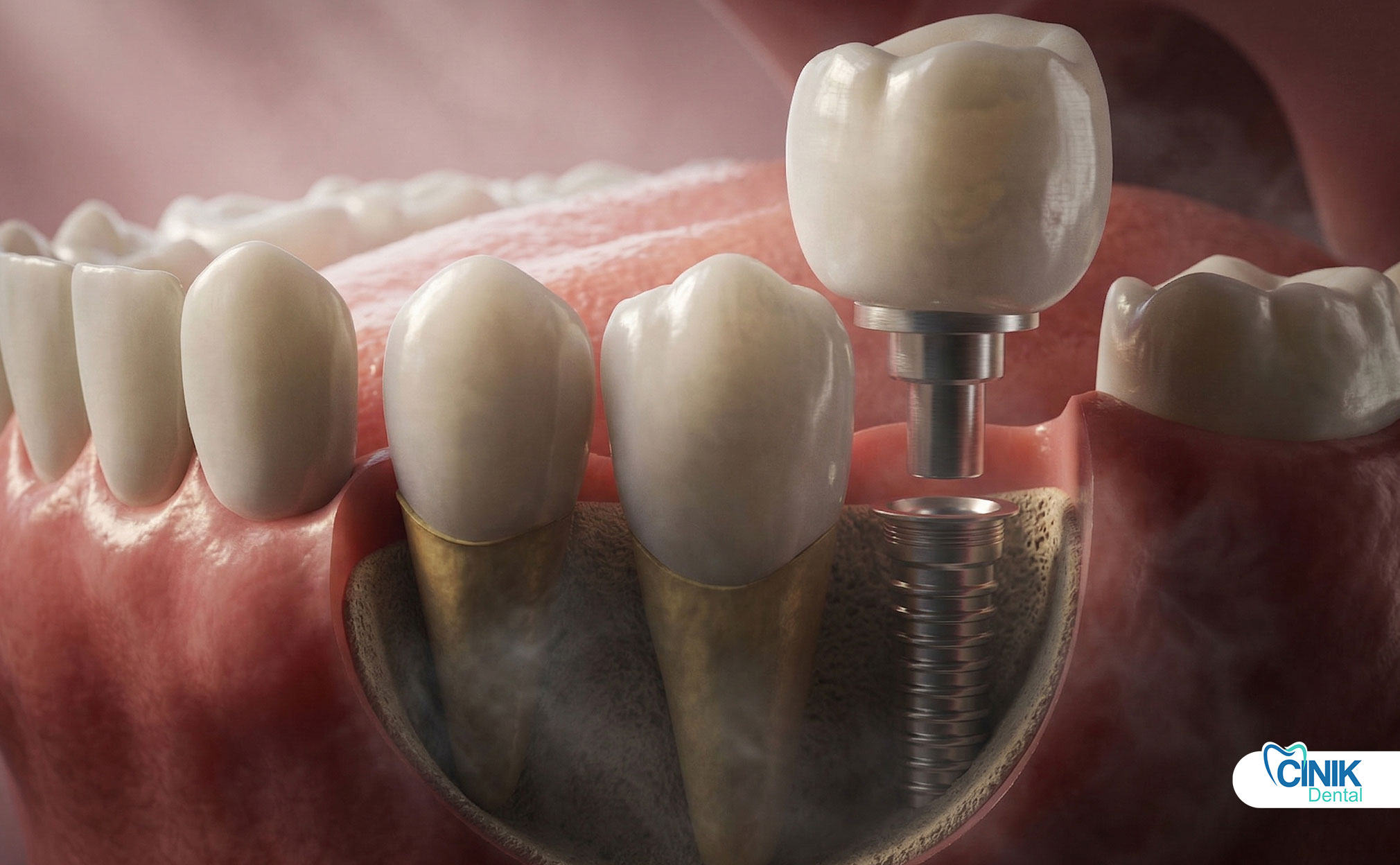
The abutment is placed after osseointegration and before the final crown placement. The procedure involves implant exposure, abutment attachment, soft tissue healing, and final impression for crown fabrication.
Timing of Abutment Placement
Abutment placement timing depends on the surgical protocol and healing requirements.
One-Stage Surgery:
Implant and healing abutment placed simultaneously
Eliminates second surgical procedure
Requires adequate primary stability at placement
Suitable for selected cases with good bone quality
Two-Stage Surgery:
Implant covered during initial healing (3-6 months)
Second surgery exposes implant and places healing abutment
Allows undisturbed osseointegration
Standard protocol for most clinical situations
The healing phase allows bone integration (osseointegration) to establish a solid foundation before functional loading. Premature loading risks implant failure and compromised stability.
Clinical Steps
Step 1: Implant Exposure (Two-Stage Protocol)
The clinician makes a small incision over the implant site to expose the implant cover screw. Local anesthesia ensures patient comfort during this minor surgical procedure. The cover screw is removed, revealing the internal implant connection.
Step 2: Healing Abutment Placement
A healing abutment is selected based on the tissue thickness and desired emergence profile. The abutment screws into the implant with predetermined torque (typically 10-15 Ncm). This component remains in place for 1-2 weeks while soft tissue heals around it.
Step 3: Soft Tissue Maturation
The gum tissue heals around the healing abutment, forming a "cuff" that will eventually receive the final abutment. This healing shapes the tissue architecture, creating the emergence profile for the final restoration. Proper tissue management during this phase determines the aesthetic outcome.
Step 4: Final Abutment Selection and Placement
Once tissue healing is complete, the clinician removes the healing abutment and places the definitive abutment. Selection criteria include:
Retention type (cement vs. screw)
Material (titanium vs. zirconia)
Angulation (straight vs. angled)
Cuff height (tissue thickness measurement)
Emergence profile design
The final abutment is torqued to manufacturer specifications (typically 20-35 Ncm) to ensure mechanical stability.
Step 5: Impression Procedures
With the final abutment in place, the clinician takes an impression to capture the exact position and orientation for laboratory fabrication. Digital scanning or traditional impression materials record the abutment position relative to adjacent teeth and opposing dentition.
Step 6: Crown Fabrication and Delivery
The dental laboratory fabricates the crown to fit the specific abutment design. Upon completion, the crown is either cemented onto the abutment or screwed into place, completing the restoration.
Healing and Recovery Timeline
Understanding the timeline helps patients set realistic expectations:
Phase | Duration | Activities |
Implant osseointegration | 3-6 months | Bone healing, no chewing on site |
Healing abutment placement | 1-2 weeks | Soft tissue shaping, minimal discomfort |
Final abutment placement | Same day | Abutment secured, impression taken |
Crown fabrication | 1-3 weeks | Laboratory manufacturing |
Final crown delivery | Single visit | Cementation or screw fixation |
Total treatment time from implant placement to final crown typically ranges from 4-9 months, depending on bone quality, healing response, and case complexity.
Implant–Abutment Connection Designs
Connection design affects stability, microleakage, and long-term success. Internal connections offer superior biomechanical performance compared to external designs, with Morse taper connections providing optimal bacterial sealing.
External Hex Connection
The external hex connection represents the original implant-abutment interface design. A hexagonal projection extends above the implant platform, engaging a corresponding hexagonal recess in the abutment.
Characteristics:
Simple design facilitating rotational torque transfer during placement
Visible hexagon above implant platform
Screw passes through abutment into implant body
Historically widespread but declining in modern systems
Limitations:
Smaller surface contact area compared to internal designs
Higher stress concentration on the screw
Greater microgap potential at the implant-abutment interface
Reduced resistance to lateral forces
Research using photoelastic stress analysis demonstrates that external connections concentrate stresses at the crestal bone level and implant components, potentially increasing the risk of mechanical complications (Dave, 2023) .
Internal Hex Connection
Internal hex connections reverse the geometry, placing the hexagonal feature inside the implant body. The abutment features a corresponding hexagonal projection that engages this internal feature.
Advantages:
Larger surface contact area improves stability
Screw is protected within the implant body
Better stress distribution to surrounding bone
Reduced screw loosening compared to external designs
The internal hex design represents a significant biomechanical improvement over external connections. The deeper engagement and protected screw position enhance long-term stability, particularly under off-center loading conditions common during mastication.
Morse Taper (Conical Connection)
The Morse taper connection features a conical interface with precise taper angles (typically 5-6 degrees) that create a friction-locked seal. This design combines the anti-rotational features of internal connections with the bacterial sealing properties of precision taper fits.
Biomechanical Benefits:
Cold-welded interface through high friction levels
Progressive tightening under functional loads (abutment settling)
Minimal microgap at the implant-abutment interface
Excellent bacterial seal reducing microleakage
Superior stress distribution compared to flat-platform designs
Finite element analysis research confirms that Morse taper connections demonstrate favorable stress patterns. Under compressive loading, abutment settling reduces the microgap, allowing the components to function as a single unit. This limits microleakage while improving resistance to rotation and bending torque (Alagarsamy et al., 2024) .
Studies comparing connection types reveal that Morse taper designs concentrate stresses away from the crestal bone, potentially preserving marginal bone levels over time. The conical interface redirects forces deeper into the implant body, reducing crestal stress concentrations.
Platform Switching Concept
Platform switching refers to using an abutment with a smaller diameter than the implant platform, creating a horizontal offset at the implant-abutment interface.
Biological Rationale:
Shifts the implant-abutment junction away from the bone crest
Reduces inflammatory cell infiltration toward bone
Maintains biological width with less crestal bone resorption
Improves soft tissue seal through horizontal offset
Research indicates that platform switching can reduce crestal bone loss by approximately 0.5-1.0 mm compared to platform-matched restorations. The offset moves the microgap, a potential pathway for bacterial infiltration, laterally away from the critical bone-implant interface.
Clinical Application:
Particularly beneficial in aesthetic zones
Useful for maintaining papilla height between implants
Applicable to most internal connection implant systems
Requires specific abutment selection relative to implant diameter
Complications Related to Implant Abutments
Complications are uncommon but may affect long-term outcomes. Mechanical issues include screw loosening and fracture, biological complications involve peri-implantitis, and aesthetic problems include tissue recession and improper emergence profiles.
Mechanical Complications
Screw Loosening:
Screw loosening represents the most common mechanical complication, occurring in 1-6% of cases depending on the connection type. Causes include inadequate torque application, occlusal overload, poorly fitting components, and external hex designs.
Prevention strategies include:
Precise torque application with calibrated drivers
Internal connection selection when possible
Occlusal load management (avoiding off-axis forces)
Regular maintenance and torque verification
Abutment or Screw Fracture:
Fracture rates range from 1.2% to 8% in clinical studies, with higher incidence in posterior regions and with zirconia abutments (Sanz-Martín et al., 2022) . Risk factors include:
Narrow-diameter implants in high-load areas
Zirconia abutments with thin walls or external connections
Platform switching designs (increased stress concentration)
Parafunctional habits (bruxism, clenching)
Component Misfit:
Microscopic gaps between components, even within manufacturer tolerances, can lead to micromovement, fretting corrosion, and biological complications. Precision manufacturing and verified component compatibility are essential.
Biological Complications
Peri-implantitis:
Peri-implantitis involves inflammation of the soft tissues with progressive bone loss around an osseointegrated implant. Abutment-related risk factors include:
Subgingival cement remnants (cement-retained restorations)
Rough abutment surfaces promoting plaque accumulation
Improper emergence profiles complicating hygiene access
Microleakage at the implant-abutment interface
Research comparing titanium and zirconia abutments shows that zirconia exhibits less plaque accumulation due to lower surface energy, potentially reducing biological complication risks (Pandey et al., 2019) . However, systematic reviews indicate no significant difference in long-term biological outcomes between materials when proper protocols are followed.
Soft Tissue Inflammation:
Mucositis (reversible inflammation) and peri-implantitis (irreversible bone loss) represent the spectrum of biological complications. Bleeding on probing is slightly more prevalent around titanium abutments compared to zirconia, though differences are often not statistically significant (Sanz-Martín et al., 2022) .
Esthetic Complications
Improper Emergence Profile:
An abutment that is too narrow or too wide for the clinical situation creates unnatural tissue contours. Narrow abutments allow tissue collapse, while overly wide abutments compress blood supply and cause recession.
Gum Recession:
Soft tissue recession exposes the implant-abutment junction or even the implant platform, creating aesthetic disasters and biological risks. Causes include:
Thin tissue biotypes with inadequate blood supply
Overly bulky abutments compressing tissue
Improper abutment angulation creating leverage forces
Inadequate soft tissue volume at placement
Metal Show-Through:
Titanium abutments in thin tissue biotypes may create a grey shadow visible through the gingiva. This "grey line" compromises aesthetics in the smile zone. Zirconia abutments or Ti-base designs with ceramic upper structures eliminate this concern.
Advantages of Proper Abutment Selection
Correct abutment choice improves function, aesthetics, and longevity. Benefits include enhanced prosthetic stability, better chewing efficiency, natural appearance, and long-term implant success.
Selecting the appropriate abutment for each clinical situation yields significant advantages across multiple domains:
Enhanced Prosthetic Stability:
Proper abutment selection ensures mechanical stability under functional loads. Internal connections and appropriate material choices minimize screw loosening and component fracture. Research demonstrates that Morse taper connections and titanium abutments in high-load areas provide optimal mechanical performance (Alagarsamy et al., 2024) .
Better Chewing Efficiency:
Optimal abutment design transfers occlusal forces efficiently to the implant and surrounding bone. Proper load distribution allows patients to chew with confidence, approaching the function of natural dentition. Biomechanical research confirms that well-designed implant-abutment connections handle masticatory forces (200-300 N in posterior regions) without excessive stress concentrations.
Natural Appearance:
Custom abutments with appropriate emergence profiles create restorations indistinguishable from natural teeth. Zirconia abutments in aesthetic zones eliminate metal visibility, while precisely contoured shapes support natural tissue architecture. Studies show that soft tissue color around zirconia abutments matches natural teeth better than titanium alternatives (Sanz-Martín et al., 2022) .
Long-Term Implant Success:
Proper abutment selection contributes to the documented 95-98% long-term survival rates of dental implants. By minimizing mechanical complications, biological inflammation, and aesthetic failures, appropriate abutment choice protects the patient's investment and oral health for decades.
Simplified Maintenance:
Screw-retained abutment selections allow future retrievability for professional maintenance, component replacement, or modification. This "serviceability" extends the functional lifespan of the restoration and reduces long-term costs.
Dental Implant Abutment vs Crown vs Implant (Key Differences)
Each component has a distinct role in the implant system. The implant acts as the root in the bone, the abutment serves as the connector above the gum, and the crown functions as the visible tooth replacement.
Component | Function | Location | Material Options | Longevity |
Implant Fixture | Acts as artificial root, provides bone anchorage | Inside jawbone (submerged or transgingival) | Titanium (commercially pure or alloy), Zirconia (ceramic) | 20+ years with proper care |
Abutment | Connects implant to prosthesis, transfers loads, shapes tissue | Above gum line, through soft tissue | Titanium, Zirconia, Gold alloy, Co-Cr | Typically matches implant lifespan |
Crown | Restores visible tooth anatomy, enables chewing, provides aesthetics | Above abutment, visible in mouth | Porcelain-fused-to-metal, All-ceramic, Zirconia, Composite | 10-15 years (replaceable) |
Functional Interdependence:
These three components function as an integrated system. The implant provides the foundation, but without the abutment, no prosthesis can attach. The abutment transfers forces, but without the crown, no chewing function is restored. The crown provides aesthetics, but without proper abutment support, it cannot survive functional loads.
Replacement Considerations:
Implant: Rarely replaced; requires surgical removal and new placement
Abutment: Replaceable if damaged or for aesthetic upgrade (screw-retained designs)
Crown: Routinely replaceable without disturbing the implant or abutment
Understanding these distinctions helps patients appreciate why the abutment selection is as critical as the implant brand or crown material.
Who Needs a Dental Implant Abutment?
Anyone receiving a dental implant restoration requires an abutment. This includes patients with single missing teeth, multiple missing teeth, and those requiring full-arch restorations.
Indications
Single Tooth Replacement:
Patients missing individual teeth due to trauma, decay, or congenital absence require implant-supported crowns. Each single-tooth restoration needs one implant, one abutment, and one crown. The abutment selection depends on the tooth position (aesthetic vs. posterior), tissue thickness, and occlusal requirements.
Multiple Missing Teeth:
Patients missing several teeth may receive implant-supported bridges. These restorations use multiple implants (typically one per missing tooth or strategic spacing) with abutments supporting a connected prosthesis. Multi-unit abutments may be employed to parallelize implant connections and simplify prosthesis fabrication.
Full-Arch Restorations:
Edentulous patients or those requiring full-arch rehabilitation benefit from implant-supported fixed or removable prostheses. The All-on-4 and All-on-6 protocols use 4-6 implants per arch with multi-unit abutments supporting a full-arch bridge. Each implant requires an abutment, though multi-unit designs reduce the complexity of individual component management.
Specific Clinical Scenarios Requiring Special Abutment Considerations:
Scenario | Abutment Consideration | Rationale |
High smile line | Zirconia or Ti-base abutment | Aesthetics critical, metal must not show |
Thin tissue biotype | Custom zirconia with concave profile | Preserve blood supply, prevent recession |
Implant malposition | Angled abutment (15°-30°) | Correct alignment for prosthesis |
Bruxism/Heavy occlusion | Titanium, wide-diameter | Mechanical strength priority |
Deep subgingival margin | Screw-retained design | Avoid cement remnants |
Limited interocclusal space | Low-profile abutment | Space constraints |
Contraindications for Immediate Abutment Placement:
Insufficient primary implant stability
Compromised bone quality requiring grafting
Active infection at the implant site
Uncontrolled systemic conditions affecting healing
Future Trends in Implant Abutment Technology
Digital dentistry is transforming abutment design and precision. Emerging trends include advanced CAD/CAM customization, AI-guided implantology, and innovative biomaterials with enhanced biocompatibility.
CAD/CAM Customization
Computer-aided design and manufacturing have revolutionized abutment fabrication. Current developments include:
Digital Impression Technology:
Intraoral scanners capture implant position and surrounding tissue architecture with micron-level accuracy. This digital workflow eliminates traditional impression materials, improving patient comfort and reducing laboratory variables.
Precision Manufacturing:
Milling centers fabricate custom abutments from solid blanks of titanium or zirconia with precision unattainable through casting. Five-axis milling creates complex emergence profiles and anatomical contours optimized for individual patients.
Virtual Treatment Planning:
Software platforms allow clinicians to visualize the final restoration before surgery, planning implant position and abutment selection for optimal outcomes. This "restoration-driven" approach ensures that implant placement supports the ideal abutment and crown position.
AI and Guided Implantology
Artificial intelligence applications are emerging in implant dentistry:
Predictive Analytics:
Machine learning algorithms analyze patient-specific factors (bone density, bite forces, tissue biotype) to recommend optimal abutment selection. These systems integrate clinical data with outcome databases to predict success probabilities for different abutment choices.
Robotic Placement:
Surgical robotic systems execute implant placement with precision beyond human capability. These systems plan abutment emergence position before surgery, ensuring that implant angulation matches the planned prosthetic outcome.
Automated Design:
AI-driven CAD software suggests abutment designs based on digital impressions, reducing design time and optimizing biomechanical parameters. These systems learn from successful cases to refine design recommendations continuously.
Biomaterials Innovation
Research continues into advanced materials for abutment fabrication:
Enhanced Biocompatibility:
Surface modifications including plasma argon cleaning, laser microtexturing, and bioactive coatings aim to improve soft tissue attachment and reduce bacterial adhesion. Studies show that plasma argon-treated titanium abutments exhibit less bone loss compared to steam-cleaned alternatives (Sanz-Martín et al., 2022) .
Reduced Bacterial Adhesion:
Materials science research focuses on surface properties that resist plaque accumulation. Zirconia's lower surface energy already demonstrates reduced plaque adherence compared to titanium. Future developments may incorporate antimicrobial surface treatments or nano-scale modifications that inhibit bacterial colonization.
Hybrid Material Systems:
Ti-base abutments represent the current state of hybrid technology, but future developments may include functionally graded materials that transition from metallic strength at the implant interface to ceramic aesthetics at the tissue level within a single component.
Smart Materials:
Research explores materials that respond to environmental conditions, self-healing ceramics, stress-adaptive alloys, or surfaces that release antimicrobial agents in response to bacterial challenge. While early in development, these innovations may transform abutment performance.
Frequently Asked Questions
Is the Abutment Placed During Implant Surgery?
Sometimes, but often after the healing phase. One-stage protocols place a healing abutment simultaneously with the implant, while two-stage protocols wait 3-6 months for osseointegration before abutment placement.
The timing depends on multiple factors:
Primary stability: Implants with high insertion torque can receive immediate abutments
Bone quality: Dense bone allows immediate loading; poor bone requires healing
Aesthetic demands: Immediate provisional abutments maintain tissue contour in visible areas
Patient factors: Systemic health, smoking status, and compliance influence decisions
Does Abutment Placement Hurt?
Minimal discomfort with local anesthesia. The procedure requires only soft tissue manipulation, not bone surgery, resulting in less postoperative discomfort than initial implant placement.
Patients typically report:
Pressure sensation during screw tightening
Mild soreness for 24-48 hours post-procedure
No significant swelling compared to implant surgery
Return to normal activities immediately
Over-the-counter analgesics manage any postoperative discomfort effectively.
How Long Does an Abutment Last?
Typically as long as the implant with proper care. Abutments are designed for permanent service, though they may require replacement if damaged or for aesthetic upgrades.
Longevity factors include:
Material selection (titanium rarely fractures; zirconia has lower fracture resistance)
Occlusal load management
Oral hygiene maintenance
Regular professional maintenance
Screw-retained designs allow replacement if needed
Studies demonstrate that CAD/CAM titanium abutments maintain stability and soft tissue health over 13-year follow-up periods (Alagarsamy et al., 2024) .
Can Abutments Be Replaced?
Yes, especially in case of damage or aesthetic revision. Screw-retained abutments are designed for retrievability, allowing replacement without disturbing the implant.
Replacement indications include:
Screw loosening that cannot be corrected by retightening
Abutment fracture or damage
Aesthetic upgrade (switching from titanium to zirconia)
Tissue changes requiring modified emergence profile
Prosthesis modification requiring different retention type
The replacement procedure is straightforward: the prosthetic screw is removed, the existing abutment is unscrewed, and the new abutment is placed with appropriate torque. The crown may require modification or remaking to fit the new abutment.
Conclusion: Why the Abutment Is the Key to Implant Success
The dental implant abutment is not just a connector, it is a critical determinant of biomechanical stability, aesthetic outcome, and long-term implant success.
The abutment represents the nexus between the hidden implant fixture and the visible restoration. Its selection influences every aspect of treatment outcomes:
Biomechanical Integrity: The abutment transfers chewing forces, distributes stresses, and maintains mechanical stability. Research confirms that connection design and material selection significantly affect stress patterns in surrounding bone and implant components. Internal connections, particularly Morse taper designs, offer superior biomechanical efficiency compared to external alternatives (Dave, 2023) .
Biological Harmony: The abutment shapes soft tissue architecture and maintains the biological seal protecting underlying bone. Material choices between titanium and zirconia involve trade-offs between mechanical strength and biological response, with current evidence supporting both materials when properly applied (Sanz-Martín et al., 2022) .
Aesthetic Integration: Custom abutment design creates natural emergence profiles that render restorations indistinguishable from natural dentition. In the aesthetic zone, zirconia abutments eliminate metal show-through, while precise contouring supports papilla maintenance and tissue harmony.
Long-Term Serviceability: Screw-retained abutment selections allow future retrievability for maintenance, modification, or component replacement. This "forward compatibility" protects the patient's investment and extends functional restoration lifespan.
As digital dentistry advances, abutment design continues evolving toward patient-specific optimization. CAD/CAM technology enables precision manufacturing tailored to individual anatomy, while biomaterials research pursues surfaces that enhance tissue integration and resist bacterial colonization.
For clinicians and patients alike, understanding the abutment's role transforms it from an afterthought into a critical decision point. The implant fixture may provide the foundation, but the abutment determines how successfully that foundation supports the final restoration. In the complex interplay of factors determining implant success, the abutment stands as the central component bridging biology, mechanics, and aesthetics.
References
Alagarsamy, S., et al. "Influence of different customized abutment materials on stress distribution of different internal implant-abutment connections: finite element analysis." BMC Oral Health, vol. 24, no. 1, 2024, p. 277.
Dave, Manas. "EBD spotlight: Bio-mechanical efficiency of different implant-abutment connections." Evidence-Based Dentistry, vol. 24, no. 3, 2023, pp. 84-85.
Nie, H., et al. "Influence of a new abutment design concept on the biomechanics of peri-implant bone, implant components, and microgap formation: a finite element analysis." BMC Oral Health, vol. 23, 2023, p. 277.
Pandey, R., et al. "Effect of different abutment materials (zirconia or titanium) on the crestal bone height in 1 year." Journal of International Society of Preventive and Community Dentistry, vol. 9, no. 6, 2019, pp. 574-579.
Sanz-Martín, I., et al. "Comparison of the Clinical Outcomes of Titanium and Zirconia Implant Abutments: A Systematic Review of Systematic Reviews." Journal of Clinical Medicine, vol. 11, no. 17, 2022, p. 5107.