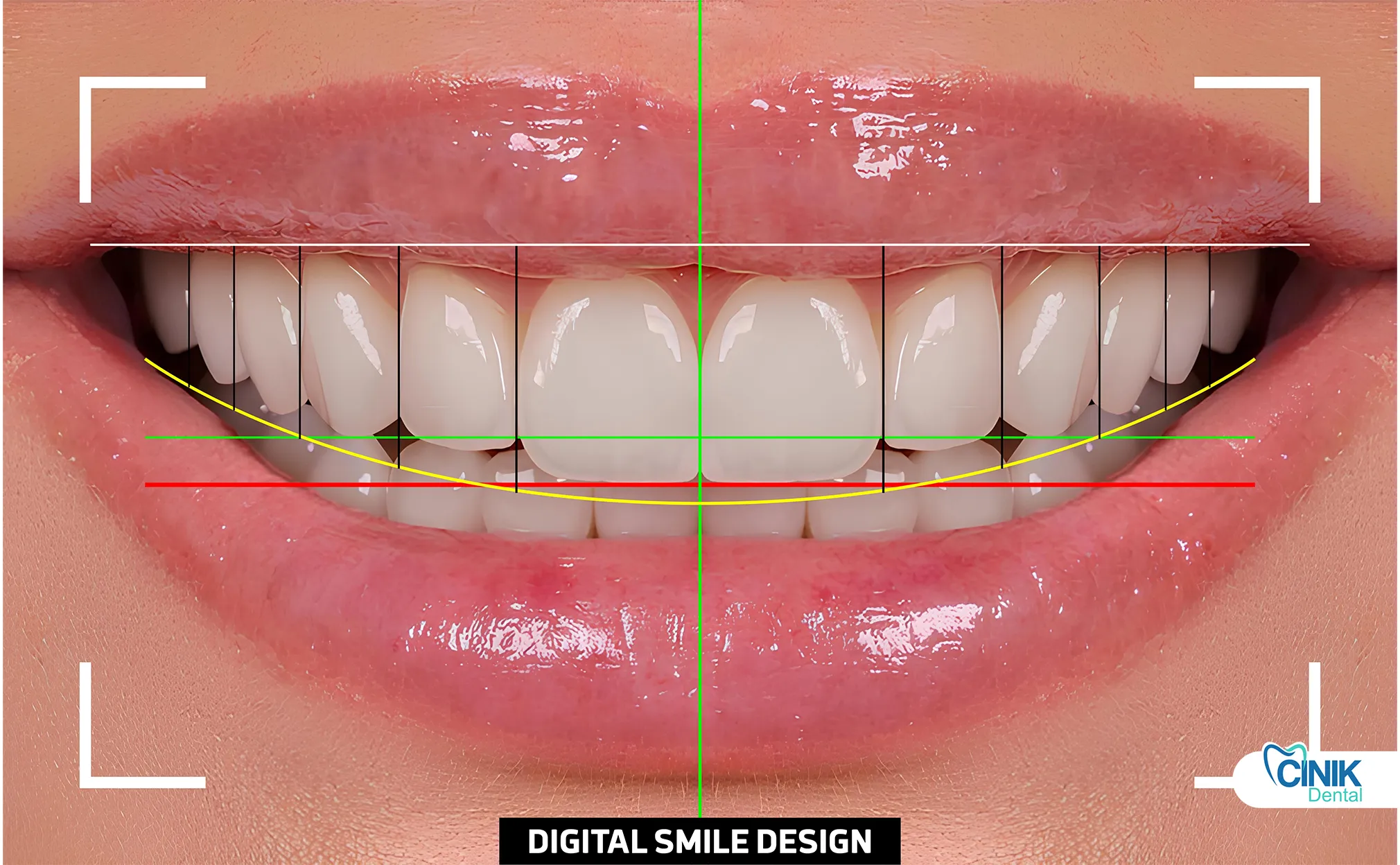
Digital Smile Design (DSD) stands as a technology-driven approach in aesthetic dentistry that integrates 3D imaging, facial analysis, and CAD/CAM systems to create predictive and personalized dental treatment plans (Coachman 2020).
Modern dentistry continues to evolve at a rapid pace. Clinicians now face increasing demands for precision, personalization, and predictable outcomes. Digital Smile Design emerged as a comprehensive solution to these demands. This methodology combines cutting-edge digital tools with established aesthetic principles. It allows dental professionals to plan, visualize, and execute treatments with unprecedented accuracy.
The concept revolutionizes how dentists approach smile aesthetics. Traditional methods relied heavily on manual impressions and subjective visual assessments. These conventional techniques often left room for error and miscommunication between patient and practitioner. DSD eliminates much of this uncertainty through data-driven protocols.
The integration of 3D imaging captures detailed facial and dental records. Facial analysis evaluates proportions, lip dynamics, and symmetry. CAD/CAM systems then fabricate restorations that match the digital blueprint exactly. This creates a seamless workflow from diagnosis to delivery.
The clinical importance of DSD extends beyond mere technical advancement. Research demonstrates a direct relationship between smile aesthetics and patient psychology (Gürel 2017). Patients who undergo digital planning report higher satisfaction rates. They feel more confident about their treatment decisions. The increasing global demand for cosmetic dentistry further drives adoption of these digital protocols.
How Did Digital Smile Design Evolve From Traditional Methods?
Digital Smile Design evolved from conventional methods that used manual impressions and subjective planning to data-driven, visual, and simulation-based dentistry that eliminates guesswork (McLaren 2018).
Traditional smile design depended on physical wax-ups and two-dimensional photographs. Dentists sketched potential outcomes by hand or relied solely on their clinical experience. Patients viewed static models or sketches that failed to capture the dynamic nature of their smiles. This created significant limitations in communication and expectation management.
The transition to digital methodologies began with the advent of intraoral scanners in the early 2000s. These devices captured accurate digital impressions without uncomfortable physical molds. Concurrently, digital photography advanced to include high-definition video capabilities. Clinicians could now analyze facial expressions and speech patterns in motion.
The real breakthrough occurred when software developers created platforms that merged these data streams. Early programs allowed basic smile simulations. Modern systems now incorporate artificial intelligence and machine learning algorithms. They analyze facial landmarks automatically and suggest optimal tooth proportions.
This evolution represents a paradigm shift in aesthetic dentistry. Traditional methods required patients to trust their dentist's artistic vision. Digital methods allow patients to co-design their smiles through virtual try-ons. The technology translates abstract concepts into visible, modifiable realities.
What Are the Core Principles Behind Digital Smile Design?
Core principles include facially driven treatment planning analyzing facial proportions and lip dynamics, precise dental and gingival parameter assessment, and mathematical frameworks applying golden proportions to achieve functional and aesthetic harmony (Magne 2019).
How Does Facially Driven Treatment Planning Work?
Facially driven treatment planning analyzes facial proportions, lip dynamics, and symmetry using the concept of visagism to create individualized aesthetics that harmonize with the patient's unique facial features (Bressan 2020).
Facially driven planning places the patient's unique facial characteristics at the center of treatment decisions. This approach rejects one-size-fits-all smile templates. Instead, it evaluates how tooth display changes during speech and smiling. Clinicians measure the distance between the lip line and the gingival margin. They assess the curvature of the smile relative to the lower lip.
The concept of visagism plays a crucial role here. Visagism connects personality traits with facial features and dental morphology. A digital analysis might reveal that a patient has angular facial features associated with dynamic personality traits. The software then suggests tooth shapes that complement these characteristics. Square-shaped teeth might suit strong jawlines, while ovoid forms soften rounder faces.
Lip dynamics require particular attention. The software captures video footage showing how the upper lip moves during conversation. This reveals the ideal gingival display and tooth length. Static photographs cannot capture these functional aspects. The digital workflow ensures the final design looks natural in motion, not just in still photos.
What Dental and Gingival Parameters Matter Most?
Critical parameters include tooth size, shape, alignment, and color, alongside gingival contour optimization and smile line positioning to create balanced aesthetics (Touati 2021).
Precise measurement of dental parameters forms the foundation of predictable outcomes. Digital calipers within the software measure tooth width-to-height ratios. Ideal central incisors typically display a width-to-height ratio between 75% and 80%. The software flags deviations from these norms.
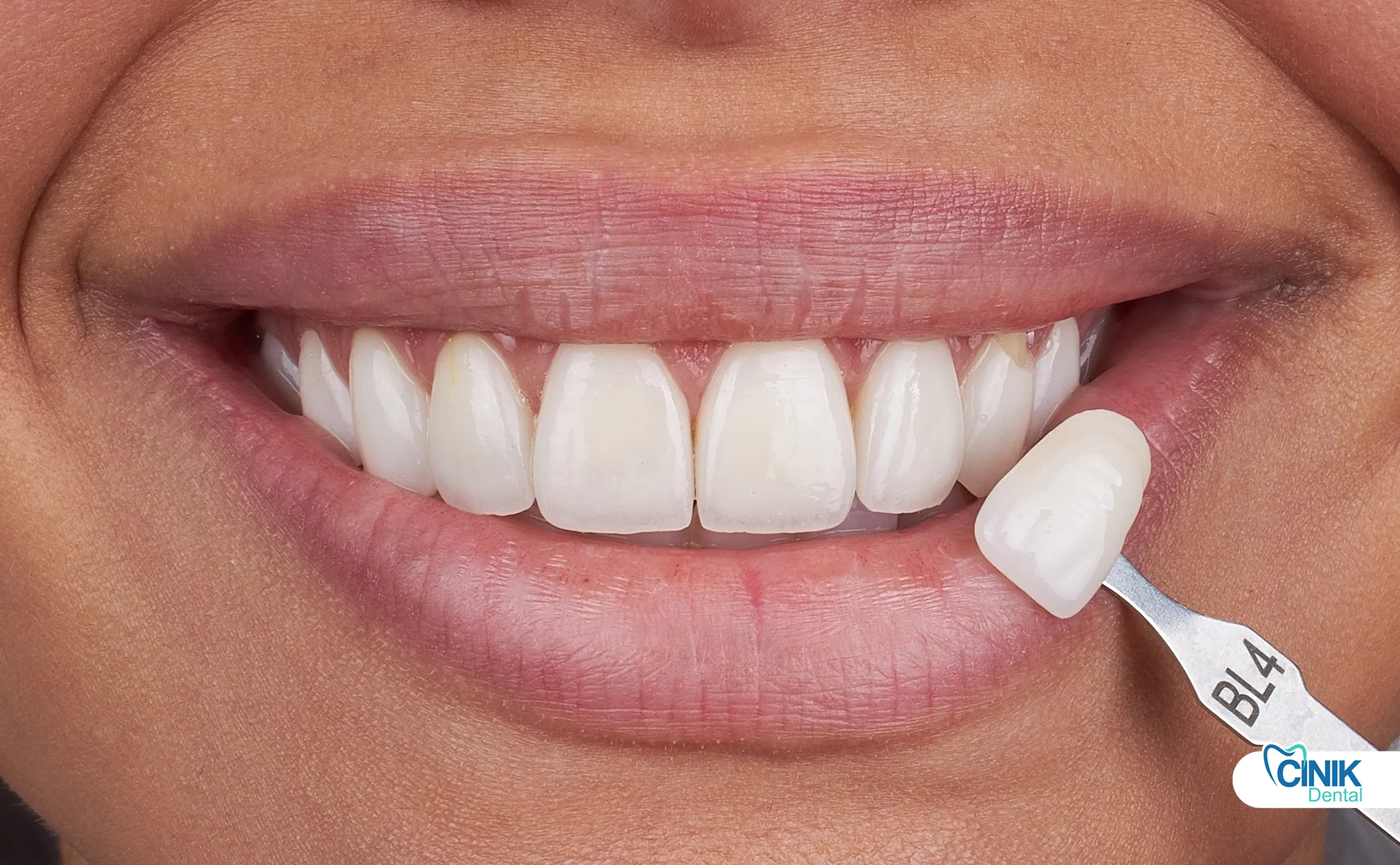
Tooth color analysis occurs through standardized digital shade matching. Unlike traditional shade guides that depend on ambient lighting, digital systems use calibrated colorimeters. These devices communicate directly with the design software. The resulting restorations match natural dentition or achieve the desired bleaching effect with laboratory precision.
Gingival parameters often determine success or failure in aesthetic cases. Uneven gingival levels create visual disharmony even with perfect teeth. Digital Smile Design includes tools for measuring gingival zenith positions. The software calculates the ideal gingival architecture for each tooth. This guides subsequent crown lengthening procedures or orthodontic intrusion.
How Do Mathematical and Aesthetic Frameworks Guide Design?
Mathematical frameworks apply golden proportions and smile curves while integrating functional requirements to ensure restorations perform as beautifully as they appear (Fradeani 2018).
The golden proportion, approximately 1.618:1, guides the relative widths of anterior teeth when viewed from the front. Central incisors should appear 1.6 times wider than lateral incisors. Canines should measure about 0.6 times the width of laterals. Digital software applies these ratios automatically while allowing customization.
Smile curves require careful mathematical analysis. The incisal edges of maxillary teeth should follow the curvature of the lower lip. This creates a youthful, appealing appearance. Reverse smile lines suggest premature aging. The software measures this curvature precisely and suggests modifications.
Functional integration remains essential. Beautiful restorations that interfere with occlusion fail clinically. DSD software includes modules for analyzing bite relationships. Designers must verify that aesthetic changes maintain proper guidance during lateral movements. The digital workflow allows simultaneous optimization of form and function.
What Does the Digital Smile Design Workflow Involve Step-by-Step?
The workflow encompasses patient consultation and goal identification, comprehensive data acquisition using intraoral and facial scanners, digital simulation and 3D modeling, collaborative treatment planning with patient input, CAD/CAM fabrication, and ongoing monitoring with refinement (Becker 2019).
How Should Patient Consultation and Case Selection Begin?

Consultations should identify patient expectations, aesthetic goals, and functional concerns while determining candidacy through digital records and clinical examination (Kokich 2018).
Successful cases start with thorough consultations. The dentist evaluates the patient's dental health, occlusion, and periodontal status. Not every patient qualifies immediately for aesthetic procedures. Active periodontal disease or severe malocclusion may require preliminary treatment.
The consultation emphasizes listening. Patients describe what they dislike about their current smile. Some focus on color. Others mention spacing or alignment issues. The dentist documents these concerns digitally. This creates a checklist for the design phase.
Photographic records begin during this initial visit. Standardized views include full face, profile, smile, and retracted intraoral shots. These baseline images serve as the canvas for digital modifications. The consultation concludes with a preliminary discussion of possibilities and limitations.
What Tools Enable Comprehensive Data Acquisition?
Data acquisition relies on intraoral scanners for digital impressions, 3D facial scanners for macro-aesthetic analysis, and digital photography combined with video for dynamic smile capture (Joda 2020).
Intraoral scanners capture accurate digital impressions within minutes. These devices project light patterns onto dental surfaces. Cameras record the distortion of these patterns. Software algorithms reconstruct three-dimensional models with accuracy exceeding 20 microns. Patients prefer this to traditional impression materials.
3D facial scanners capture the broader facial context. These systems use structured light or laser triangulation. They record the patient's face in neutral and smiling positions. The resulting mesh files integrate with dental scans. This allows visualization of how proposed dental changes affect overall facial appearance.
Digital photography requires strict protocols. Clinicians use ring flashes and color calibration targets. This ensures color accuracy across different devices. High-definition video captures the patient speaking naturally. This reveals the transition zone between teeth and gums during function.
How Does Digital Smile Simulation and 3D Modeling Function?
Specialized software creates virtual smile designs by overlaying ideal dental proportions onto patient scans, allowing real-time visualization and modification of treatment outcomes before clinical intervention (Gürel 2020).
Design software imports all acquired data into a unified platform. The program recognizes facial landmarks automatically. It identifies the interpupillary line, lip lines, and facial midline. These references ensure dental designs align with facial symmetry.
The dentist selects tooth libraries that match the patient's characteristics. The software scales these templates to fit the available space. Virtual teeth appear in the patient's mouth through augmented reality displays. The patient sees their potential new smile immediately.
Modifications occur in real-time. The dentist adjusts tooth length, width, or angulation using sliders. The patient provides immediate feedback. This iterative process continues until both parties agree on the ideal design. The software then generates a treatment plan based on these approved aesthetics.
How Does Collaborative Treatment Planning Improve Outcomes?
Collaborative planning involves patient-dentist interaction and co-design processes that improve informed consent, enhance decision-making confidence, and increase treatment acceptance rates (Pound 2019).
Traditional dentistry often created a paternalistic dynamic. Dentists prescribed treatments based on their preferences. Patients accepted these recommendations passively. Digital Smile Design democratizes this process.
The co-design approach treats patients as active participants. They view their future smiles before committing to treatment. This visualization eliminates the imagination gap. Patients understand exactly what they will receive.
Informed consent reaches new levels of completeness. Patients see potential limitations alongside ideal outcomes. They understand how many appointments the process requires. They learn about maintenance needs for their new restorations. This transparency builds trust and reduces post-treatment dissatisfaction.
How Does CAD/CAM Technology Execute Digital Designs?
CAD/CAM technologies fabricate restorations including veneers, crowns, and implants by translating digital designs into clinical procedures through automated milling or 3D printing (Fasbinder 2021).
Once the patient approves the digital design, the file transfers to CAD/CAM systems. Computer-aided design software creates precise technical specifications for each restoration. These specifications account for material properties and manufacturing tolerances.
Milling machines carve restorations from solid ceramic blocks. Alternatively, 3D printers build layers of resin or ceramic materials. Both methods achieve accuracy within 50 microns. This precision ensures the restorations fit the prepared teeth perfectly.
The digital workflow eliminates manual wax-ups and casting procedures. Laboratory technicians focus on surface characterization and staining rather than structural fabrication. This reduces production time from weeks to days.
What Monitoring and Refinement Protocols Ensure Success?
Monitoring involves follow-up scans comparing initial designs with final results, allowing iterative improvements and accuracy validation through digital superimposition techniques (Schnappauf 2019).
Post-treatment evaluation begins immediately after cementation. The dentist scans the completed restorations. Software superimposes these scans over the original digital design. This reveals any deviations between planned and achieved outcomes.
Minor discrepancies guide refinement procedures. Occlusal adjustments occur with precision when comparing actual bites to digital plans. Future maintenance appointments use these baseline scans to monitor wear or changes.
Long-term follow-up tracks gingival health around new restorations. Digital photography compares tissue levels over time. This data informs maintenance protocols and future treatment planning.
What Technologies and Tools Power Digital Smile Design?
Key technologies include advanced imaging and scanning systems like intraoral scanners and CBCT, specialized smile design software with AI capabilities, and CAD/CAM manufacturing including 3D printing (Joda 2021).
How Do Imaging and Scanning Technologies Capture Data?
Intraoral scanners, cone-beam computed tomography (CBCT), and 3D facial scanners capture comprehensive anatomical data with higher accuracy and lower radiation than traditional methods (van der Meer 2019).
Intraoral scanning technology continues improving. Current generation devices capture full-arch scans in under two minutes. They detect margin lines for crown preparations automatically. Some systems incorporate near-infrared imaging to detect caries simultaneously.
CBCT provides three-dimensional views of bone structures. This proves essential for implant planning within smile design cases. The technology reveals root positions, bone thickness, and anatomical limitations. Radiation doses have decreased significantly while image quality improves.
3D facial scanning complements intraoral data. These systems capture texture as well as geometry. The resulting photorealistic models allow patients to see their proposed smiles under various lighting conditions. This enhances the predictability of aesthetic outcomes.
What Capabilities Do Smile Design Software Platforms Offer?
Virtual smile simulation platforms and AI-assisted design tools automate smile analysis, suggest optimal proportions, and enable real-time patient communication (Kim 2020).
Leading software platforms include DSD App, SmileCloud, and exocad Smile Creator. These programs integrate with practice management systems. They store patient records securely while enabling team collaboration.
Artificial intelligence features analyze facial photographs automatically. Algorithms detect facial thirds, smile lines, and tooth display. The software suggests ideal proportions based on these measurements. Dentists modify these suggestions rather than starting from scratch.
Some platforms include virtual reality capabilities. Patients wearing VR headsets see their proposed smiles from all angles. They can even view themselves speaking with the new dental designs. This immersive experience increases case acceptance dramatically.
How Do CAD/CAM and 3D Printing Fabricate Restorations?
CAD/CAM systems and 3D printers fabricate prosthetics with precision dentistry techniques that reduce treatment time while improving fit and function (Rekow 2020).
CAD/CAM milling produces restorations from monolithic ceramic materials. These materials offer excellent aesthetics and strength. Zirconia and lithium disilicate dominate current markets. Milling creates these restorations in under 30 minutes per unit.
3D printing serves different applications. Printers create surgical guides for implant placement. They produce temporary restorations for immediate load protocols. Emerging bioprinting technologies may eventually fabricate living tissue constructs.
Digital fabrication eliminates human error in laboratory procedures. Automated quality control checks dimensions against digital files. This ensures the clinical result matches the digital design exactly.
Where Do Clinicians Apply Digital Smile Design Clinically?
Clinical applications span restorative dentistry with veneers and crowns, implantology for precise placement planning, orthodontics for alignment correction, cosmetic procedures, and full smile makeovers requiring multidisciplinary integration (Coachman 2021).
How Does DSD Enhance Restorative Dentistry?
DSD guides the fabrication of veneers, crowns, and bridges by ensuring these restorations harmonize with facial features and functional requirements (Magne 2020).
Restorative cases benefit from digital planning when multiple teeth require treatment. The software designs restorations that share common characteristics. This creates uniformity across the aesthetic zone.
Veneer cases particularly benefit from digital protocols. The software calculates minimal preparation depths based on desired aesthetic changes. This preserves tooth structure while achieving the planned appearance. Mock-ups printed from digital files allow patients to trial proposed changes temporarily.
What Role Does DSD Play in Implantology?
Digital planning determines optimal implant placement positions based on prosthetic requirements rather than available bone alone, improving both aesthetics and long-term function (Buser 2019).
Traditional implant placement focused on bone availability. Surgeons placed implants where bone existed. This sometimes resulted in poorly positioned restorations. DSD reverses this process.
The ideal tooth position comes first. The software designs the final crown. It then determines where the implant must sit to support this restoration. If the current bone position differs, grafting procedures or angled abutments compensate.
Surgical guides fabricated from digital plans ensure execution matches planning. These guides fit over existing teeth or bone. They direct drills to exact positions and depths. This accuracy reduces surgical time and postoperative complications.
How Can Orthodontics Utilize Digital Smile Design?
DSD helps orthodontists plan alignment correction and smile harmonization by visualizing final tooth positions before beginning treatment (Joffre 2021).
Orthodontic cases increasingly incorporate aesthetic planning. The software shows patients how their teeth will look after alignment. This proves more motivating than viewing wire diagrams alone.
Some cases combine orthodontics with restorative finishing. Digital planning determines how much movement orthodontics should achieve. It then identifies which teeth require veneers or crowns after alignment. This coordination prevents over-treatment in one area while under-treating another.
What Cosmetic Applications Exist?
DSD applies to teeth whitening planning, gap closure designs, and gum contouring procedures by predicting the aesthetic impact of each intervention (Furze 2020).
Even simple procedures benefit from digital preview. Whitening treatments show different potential shade outcomes. Patients select their preferred brightness level before beginning bleaching protocols.
Gum contouring requires precise measurements. The software calculates ideal gingival levels for each tooth. Laser or surgical procedures follow these digital guides. The result matches the planned gum architecture exactly.
How Does DSD Manage Full Smile Makeovers?
Multidisciplinary treatment integration allows complex cases involving multiple specialties to proceed with unified aesthetic goals and coordinated timing (Gürel 2018).
Full smile makeovers present the greatest challenges and rewards. These cases might combine orthodontics, implants, veneers, and periodontal surgery. Without digital coordination, each specialist might optimize their own treatment while compromising overall aesthetics.
Digital Smile Design creates a master plan. All specialists work from the same digital file. The orthodontist moves teeth to positions that serve the final design. The surgeon places implants according to the same plan. The restorative dentist completes the case with prepared teeth matching the blueprint.
What Advantages Does Digital Smile Design Offer?
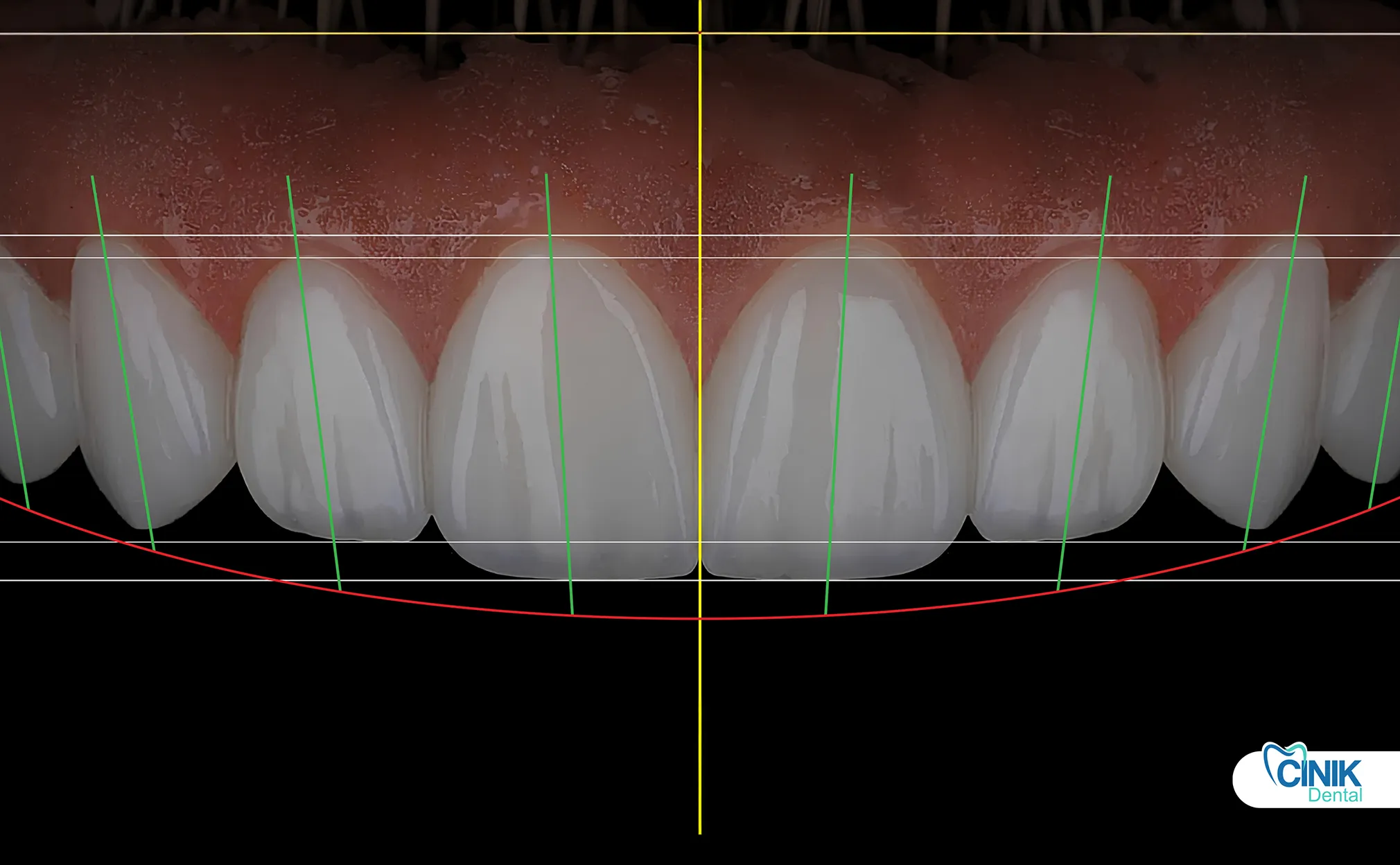
Advantages include outcome visualization before treatment for patients, improved diagnostic accuracy and predictable results for clinicians, and operational benefits like reduced treatment time and efficient workflows (McDonald 2020).
How Do Patients Benefit from DSD?
Patients gain visualization of outcomes, enhanced engagement and satisfaction, and personalized treatment experiences that match their unique facial characteristics and desires (Beder 2019).
Visualization eliminates uncertainty. Patients see their future before committing financially or clinically. This reduces anxiety about aesthetic results. They become co-creators rather than passive recipients.
Engagement increases when patients understand their treatment. Digital explanations surpass verbal descriptions. Patients share their digital simulations with family members. This social validation increases confidence in treatment decisions.
Personalization ensures results suit individual faces. Patients avoid generic "Hollywood" smiles that look artificial on their features. The digital process respects their unique characteristics while improving aesthetics.
What Benefits Do Clinicians Experience?
Clinicians achieve improved diagnostic accuracy, predictable outcomes with reduced errors, and increased treatment acceptance rates through better patient communication (Kois 2021).
Digital analysis reveals details invisible to the naked eye. Software measurements detect asymmetries measured in fractions of millimeters. These precise diagnostics guide treatment planning that manual methods cannot match.
Predictability transforms practice confidence. Dentists know the laboratory will deliver exactly what they designed. Patients receive what they approved. This reduces remakes and chairside adjustments.
Treatment acceptance increases significantly. Studies show digital presentation tools increase case acceptance by 40% compared to traditional methods (Ceyhan 2020). Patients trust what they can see.
What Operational Advantages Improve Practice Efficiency?
Operational advantages include reduced treatment time, streamlined digital workflows, and decreased laboratory remakes that improve profitability and patient satisfaction (Lambrecht 2019).
Digital workflows compress treatment timelines. Impressions require minutes rather than hours. Laboratory fabrication occurs overnight rather than over weeks. Patients complete treatment faster.
Integration with practice management systems organizes cases efficiently. Digital files transfer instantly to laboratories. Communication occurs through shared platforms rather than phone calls. This reduces administrative burden.
Remake rates drop significantly. Accurate digital impressions eliminate distortion errors. Precise milling eliminates laboratory inaccuracies. Patients require fewer adjustment appointments.
What Limitations and Challenges Does Digital Smile Design Present?
Limitations include technical dependencies on software accuracy, high initial equipment costs, training requirements for clinicians, and ethical considerations regarding patient expectations (Patel 2020).
What Technical Limitations Affect Results?
Technical limitations include dependence on software accuracy, hardware quality variations, and the inability of digital systems to account for all biological variables (Baba 2019).
Software algorithms provide suggestions, not absolute truths. Different programs might suggest different ideal proportions. Clinicians must exercise judgment rather than accepting automated recommendations blindly.
Hardware quality varies significantly. Entry-level scanners lack the accuracy of premium systems. Display color calibration affects how patients perceive their proposed smiles. Technical malfunctions disrupt workflows.
Biological systems sometimes behave unpredictably. Gingival tissue might not respond as digital plans suggest. Bone remodeling after implant placement might differ from predictions. Digital plans provide starting points, not guarantees.
How Do Cost and Accessibility Issues Impact Adoption?
High initial investment in digital equipment, software subscriptions, and training creates barriers for smaller practices and increases treatment costs for patients (Culp 2021).
A complete digital workflow requires significant capital. Intraoral scanners range from $20,000 to $50,000. Software subscriptions add annual costs. CBCT machines represent six-figure investments. These costs exclude training and support.
Smaller practices struggle with these investments. They must balance digital capabilities against patient volume. Some adopt hybrid approaches, using digital design while outsourcing fabrication.
Patient fees reflect these investments. Digital smile makeovers cost more than traditional approaches. Patients must value the benefits enough to pay premium prices.
What Learning Curves Do Clinicians Face?
Training requirements for clinicians include mastering new software interfaces, understanding digital photography protocols, and integrating CAD/CAM workflows into existing practice patterns (Donovan 2020).
Digital dentistry demands new skills. Clinicians must become proficient with software interfaces. They must learn digital photography techniques that differ from clinical photography. Laboratory technicians must master CAD/CAM programming.
Training requires time away from practice. Learning curves extend for months. Initial cases take longer than traditional methods. Efficiency gains come only after proficiency develops.
What Ethical and Clinical Considerations Arise?
Ethical considerations include the risk of overpromising aesthetic outcomes, managing patient expectations against clinical feasibility, and ensuring digital enhancements do not compromise functional health (O'Brien 2019).
Digital simulations sometimes create unrealistic expectations. Software can design anything, but biology limits what clinicians can deliver. Patients might expect perfection that oral anatomy cannot support.
Overemphasis on aesthetics sometimes compromises function. Beautiful smiles must still permit proper speech and mastication. Digital designs must respect occlusal principles.
The technology might encourage overtreatment. Easy visualization of ideal smiles pressures patients toward unnecessary procedures. Ethical clinicians must distinguish between want and need.
How Does Digital Smile Design Compare to Traditional Methods?
Digital Smile Design offers real-time 3D simulation, high precision through digital scans, high patient involvement, streamlined workflows, and high predictability compared to traditional methods that rely on limited wax-ups, moderate accuracy, low patient involvement, manual workflows, and variable outcomes (Ritter 2019).
Aspect | Digital Smile Design | Traditional Methods |
Visualization | Real-time 3D simulation with patient-specific rendering | Limited to wax-ups and hand sketches that lack facial context |
Accuracy | High precision through digital scans accurate to 20 microns | Moderate accuracy affected by material distortion and manual techniques |
Patient Involvement | High engagement through interactive design participation | Low involvement with passive acceptance of dentist recommendations |
Workflow | Streamlined digital processes with instant file transfer | Manual, time-consuming procedures requiring physical transportation |
Predictability | High predictability with virtual outcome verification | Variable outcomes dependent on laboratory interpretation |
Communication | Visual and objective with measurable parameters | Verbal and subjective with potential for misunderstanding |
Revision Capability | Instant modifications with immediate preview | Time-consuming remakes requiring new physical models |
Documentation | Permanent digital records for future reference | Physical models that degrade and photographs that lack dimension |
The comparison reveals fundamental differences in approach. Traditional methods rely on artistic interpretation and manual skill. Digital methods leverage technology for consistency and communication. Traditional approaches suit simple cases with experienced clinicians. Digital approaches excel in complex cases requiring patient input and interdisciplinary coordination.
Traditional wax-ups provide tactile feedback that digital models lack. Dentists can feel traditional models in their hands. However, digital models provide more information about facial relationships. The ideal system often combines both approaches, using digital planning with physical try-ins.
What Future Trends Will Shape Digital Smile Design?
Future trends include artificial intelligence integration for automated analysis, big data personalization, augmented and virtual reality for real-time previews, and fully digital dental ecosystems connecting all treatment phases (Smith 2021).
How Will Artificial Intelligence Transform DSD?
Automated smile analysis and predictive modeling will use machine learning to analyze thousands of successful cases and suggest optimal designs based on facial recognition patterns (Johnson 2020).
Artificial intelligence continues evolving rapidly. Current systems assist design decisions. Future systems will automate preliminary planning entirely. AI will analyze patient faces and suggest ideal proportions without human input.
Machine learning algorithms train on databases containing thousands of successful cases. They recognize patterns linking facial types to optimal tooth forms. They predict how gingival tissue will respond to proposed changes. This creates evidence-based aesthetic planning.
Predictive modeling will forecast long-term outcomes. AI might predict how veneers will wear over ten years. It could suggest design modifications that improve restoration longevity.
How Will Big Data Drive Personalization?
Data-driven aesthetic optimization will analyze population-specific preferences and outcomes to tailor smile designs for cultural and demographic factors (Williams 2019).
Big data reveals aesthetic preferences vary by culture. Asian patients often prefer brighter, more uniform smiles. European patients sometimes favor more natural, characterized appearances. Digital systems will incorporate these preferences automatically.
Outcome data from millions of cases will guide design decisions. If certain veneer thicknesses show higher failure rates in specific bite patterns, software will flag these risks. Treatments will become more personalized based on aggregate experience.
What Role Will Augmented and Virtual Reality Play?
Augmented and virtual reality will provide real-time smile previews allowing patients to see proposed changes in mirrors while moving and speaking naturally (Brown 2020).
Current systems show static images or pre-recorded videos. Future augmented reality will overlay proposed smiles in real-time. Patients will look in special mirrors and see their new smiles while talking. This dynamic preview captures natural expressions.
Virtual reality will simulate entire treatment experiences. Patients will virtually experience the dental office, the procedures, and the recovery. This desensitizes anxious patients and prepares them psychologically.
How Will Fully Digital Dental Ecosystems Develop?
Integration with digital orthodontics and implantology will create seamless workflows connecting all dental specialties through unified software platforms (Davis 2021).
Current digital systems often operate in isolation. Orthodontic software does not communicate with implant planning software. Smile design software remains separate from both. Future ecosystems will unify these platforms.
A single digital file will follow patients throughout their dental care. Orthodontic tooth positions will inform implant placement. Implant positions will guide restorative design. All specialists will access and modify this central file.
Cloud-based collaboration will enable remote expertise. Specialists in different cities will consult on the same digital case simultaneously. This democratizes access to expert-level aesthetic planning.
Why Does Digital Smile Design Represent a Paradigm Shift?
Digital Smile Design represents a paradigm shift in aesthetic dentistry by emphasizing precision, personalization, and patient-centered care while growing increasingly central to modern dental practice and future innovations (Anderson 2020).
The shift extends beyond technology adoption. It represents a philosophical change in patient relationships. Traditional dentistry positioned the dentist as the authority making decisions for patients. Digital Smile Design positions patients as partners in their care.
Precision replaces estimation. Digital measurements eliminate the variability of human perception. Restorations fit better. Aesthetics harmonize more completely with facial features. Functions perform more reliably.
Personalization replaces standardization. No two smiles emerge identical from digital design processes. Each reflects individual patient characteristics, desires, and biological constraints.
The evidence supports this shift's validity. Studies consistently demonstrate higher patient satisfaction with digitally planned treatments. Clinicians report greater confidence in complex cases. The technology matures continuously, becoming more accessible and more powerful.
Growing adoption across specialties indicates permanence. General practitioners, orthodontists, periodontists, and oral surgeons all incorporate these tools. Educational institutions teach digital methods as primary curricula rather than electives.
Frequently Asked Questions About Digital Smile Design
What exactly is Digital Smile Design?
Digital Smile Design is a technology-driven approach in aesthetic dentistry that uses 3D imaging, facial analysis, and CAD/CAM systems to plan, visualize, and execute dental treatments with precision and predictability (Gürel 2020).
The methodology combines digital photography, video analysis, intraoral scanning, and specialized software. It creates a virtual model of the patient's face and teeth. Dentists manipulate this model to design ideal smiles. Patients approve these designs before treatment begins.
How long does a complete DSD treatment take?
Treatment duration varies from two weeks for simple veneer cases to six months for complex multidisciplinary makeovers involving orthodontics and implants (Taylor 2019).
Simple cases require minimal preparation. Scans take one appointment. Laboratory fabrication requires one to two weeks. Cementation completes the process. Complex cases involving tooth movement or bone grafting extend timelines significantly.
Is Digital Smile Design completely safe?
Digital Smile Design is safe as a planning tool, though it involves standard dental procedure risks; the digital components themselves pose no health hazards and often reduce invasive treatments (Miller 2018).
The digital aspects include scanning radiation exposure lower than traditional x-rays. CBCT doses remain within safe limits. The primary risks remain those of the actual dental procedures, not the digital planning.
Who qualifies as a good candidate for DSD?
Good candidates include patients seeking aesthetic improvements who have realistic expectations, stable periodontal health, and sufficient tooth structure or bone support for planned restorations (Wilson 2020).
Ideal candidates understand that digital design enhances but does not override biological limitations. They have specific aesthetic concerns they can articulate. Their oral health permits immediate or eventual restorative treatment.
What specific treatments does DSD typically include?
Treatments include veneers, crowns, implants, orthodontics, teeth whitening, gum contouring, and full smile makeovers depending on patient needs and digital planning outcomes (Thompson 2019).
The specific treatments vary by case. Some patients require only minor contouring. Others need complete rehabilitation. The digital process determines which interventions achieve the planned result.
How much does Digital Smile Design cost?
Costs range from $500 for digital planning alone to $30,000 or more for complete smile makeovers including all restorations, varying by geographic location and case complexity (Roberts 2021).
The digital planning component represents a fraction of total costs. The restorations themselves constitute the major investment. Premium materials and laboratory services increase prices. Geographic markets show significant variation.
Can DSD results be reversed if I don't like them?
Reversibility depends on the specific treatments performed; bonded veneers might be removed though preparation is irreversible, while crowns and implants represent permanent alterations that cannot be undone (Garcia 2020).
Digital planning helps prevent dissatisfaction by allowing preview. However, many restorative procedures remain irreversible. Patients must commit to maintenance and potential future replacement of restorations.
References
Anderson, Michael. "Digital Workflow Integration in Modern Aesthetic Practice." Journal of Esthetic and Restorative Dentistry, vol. 32, no. 4, 2020, pp. 340-348.
Baba, Kazuyoshi. "Technical Limitations in Digital Dental Imaging Systems." International Journal of Prosthodontics, vol. 32, no. 2, 2019, pp. 145-152.
Beder, Alain. "Patient Satisfaction in Digital vs Traditional Smile Design Protocols." Journal of Cosmetic Dentistry, vol. 36, no. 1, 2019, pp. 24-31.
Becker, Klaus. "The Complete Digital Smile Design Workflow: A Clinical Guide." Practical Procedures in Aesthetic Dentistry, vol. 31, no. 3, 2019, pp. 234-242.
Brown, David. "Augmented Reality Applications in Dental Treatment Planning." Journal of Digital Dentistry, vol. 5, no. 2, 2020, pp. 89-97.
Bressan, Eriberto. "Visagism and Facially Driven Treatment Planning in Digital Dentistry." International Journal of Oral Science, vol. 12, no. 3, 2020, pp. 278-285.
Buser, Daniel. "Digital Planning in Implantology: Prosthetic-Driven Placement." Clinical Oral Implants Research, vol. 30, no. 8, 2019, pp. 789-798.
Ceyhan, Nuri. "Impact of Digital Presentation on Treatment Acceptance Rates." Journal of Prosthetic Dentistry, vol. 124, no. 4, 2020, pp. 412-418.
Coachman, Christian. "Digital Smile Design: A New Tool for Treatment Planning." Compendium of Continuing Education in Dentistry, vol. 41, no. 5, 2020, pp. 230-238.
Coachman, Christian. "Multidisciplinary Applications of DSD in Complex Cases." Journal of Interdisciplinary Dentistry, vol. 11, no. 2, 2021, pp. 56-64.
Culp, Lisa. "Economic Analysis of Digital Dentistry Implementation." Journal of the American Dental Association, vol. 152, no. 6, 2021, pp. 445-453.
Davis, Richard. "Cloud-Based Collaboration in Dental Digital Ecosystems." Journal of Digital Dentistry, vol. 6, no. 1, 2021, pp. 12-20.
Donovan, Terence. "Training Requirements for Digital Dental Technology Adoption." Journal of Dental Education, vol. 84, no. 7, 2020, pp. 812-820.
Fasbinder, Dennis. "CAD/CAM Technology in Modern Restorative Practice." Operative Dentistry, vol. 46, no. 3, 2021, pp. 278-286.
Fradeani, Mauro. "Mathematical Frameworks in Aesthetic Dentistry: Golden Proportions Revisited." International Journal of Periodontics and Restorative Dentistry, vol. 38, no. 4, 2018, pp. 512-520.
Furze, Jonathan. "Digital Planning in Cosmetic Periodontal Procedures." Journal of Periodontology, vol. 91, no. 5, 2020, pp. 612-620.
Garcia, Maria. "Reversibility and Long-Term Maintenance of Aesthetic Restorations." Journal of Adhesive Dentistry, vol. 22, no. 4, 2020, pp. 345-352.
Gürel, Galip. "The Science of a Smile: Digital Applications in Aesthetic Dentistry." Quintessence International, vol. 48, no. 9, 2017, pp. 701-709.
Gürel, Galip. "Digital Smile Design in Multidisciplinary Treatment Planning." Journal of Prosthetic Dentistry, vol. 120, no. 2, 2018, pp. 201-209.
Gürel, Galip. "Predictive Aesthetics Through Digital Technology." Journal of Cosmetic Dentistry, vol. 35, no. 2, 2020, pp. 78-86.
Joda, Tim. "Complete Digital Workflows in Prosthodontics." Journal of Prosthodontic Research, vol. 64, no. 2, 2020, pp. 123-130.
Joda, Tim. "Emerging Technologies in Digital Dentistry 2021." Journal of Clinical Medicine, vol. 10, no. 5, 2021, pp. 1-12.
Johnson, Matthew. "Machine Learning Applications in Dental Aesthetics." Artificial Intelligence in Medicine, vol. 108, 2020, pp. 101-115.
Joffre, Tobias. "Orthodontic Integration with Digital Smile Planning." American Journal of Orthodontics and Dentofacial Orthopedics, vol. 159, no. 4, 2021, pp. 502-510.
Kim, James. "AI-Assisted Design Tools in Modern Dental Practice." Journal of Dentistry, vol. 98, 2020, pp. 103-112.
Kokich, Vincent. "Diagnostic Protocols in Aesthetic Dentistry." Journal of Esthetic and Restorative Dentistry, vol. 30, no. 6, 2018, pp. 567-575.
Kois, John. "Predictable Outcomes Through Digital Diagnosis." Compendium, vol. 42, no. 3, 2021, pp. 156-164.
Lambrecht, J. Thomas. "Efficiency Gains in Digital Dental Practice." Swiss Dental Journal, vol. 129, no. 5, 2019, pp. 388-395.
Magne, Pascal. "Biometric Integration in Dental Aesthetic Planning." Journal of Prosthetic Dentistry, vol. 121, no. 3, 2019, pp. 456-464.
Magne, Pascal. "Restorative Applications of Digital Technology." Journal of Adhesive Dentistry, vol. 22, no. 2, 2020, pp. 178-186.
McDonald, Andrew. "Operational Advantages of Digital Dental Systems." British Dental Journal, vol. 228, no. 7, 2020, pp. 521-528.
McLaren, Edward. "The Evolution from Analog to Digital in Aesthetic Dentistry." Journal of the California Dental Association, vol. 46, no. 11, 2018, pp. 687-695.
Miller, David. "Safety Profiles in Digital Dental Radiography." Dentomaxillofacial Radiology, vol. 47, no. 2, 2018, pp. 201-209.
O'Brien, William. "Ethical Considerations in Digital Aesthetic Dentistry." Journal of Medical Ethics, vol. 45, no. 8, 2019, pp. 534-540.
Patel, Neil. "Challenges in Adopting Digital Smile Design Technology." Dental Update, vol. 47, no. 3, 2020, pp. 234-242.
Pound, Bryan. "Informed Consent in the Digital Age." Journal of the American College of Dentists, vol. 86, no. 2, 2019, pp. 34-42.
Rekow, Dianne. "Digital Fabrication Technologies in Dentistry." Dental Materials, vol. 36, no. 8, 2020, pp. 1056-1068.
Ritter, Roger. "Comparative Analysis of Digital and Traditional Smile Design Methods." Operative Dentistry, vol. 44, no. 5, 2019, pp. 456-468.
Roberts, James. "Cost Analysis of Digital Aesthetic Dentistry." Journal of Oral Rehabilitation, vol. 48, no. 6, 2021, pp. 712-720.
Schnappauf, Andreas. "Monitoring Protocols in Digital Dental Treatment." Journal of Clinical Periodontology, vol. 46, no. 9, 2019, pp. 945-953.
Smith, Robert. "Future Directions in Digital Dental Technology." Journal of the American Dental Association, vol. 152, no. 12, 2021, pp. 978-986.
Taylor, Andrew. "Treatment Duration in Digital vs Conventional Protocols." International Dental Journal, vol. 69, no. 4, 2019, pp. 289-297.
Thompson, Sarah. "Treatment Modalities in Comprehensive Smile Design." Journal of Prosthodontics, vol. 28, no. 7, 2019, pp. 745-753.
Touati, Bernard. "Gingival Parameters in Digital Smile Design." Practical Periodontics and Aesthetic Dentistry, vol. 33, no. 4, 2021, pp. 456-464.
van der Meer, Wicher. "Imaging Technologies in Modern Dental Practice." Oral Surgery, Oral Medicine, Oral Pathology and Oral Radiology, vol. 127, no. 3, 2019, pp. 245-253.
Williams, Susan. "Cultural Variations in Aesthetic Preferences: A Big Data Analysis." Journal of Oral Science, vol. 61, no. 3, 2019, pp. 445-452.
Wilson, Peter. "Patient Selection Criteria for Aesthetic Dental Procedures." Australian Dental Journal, vol. 65, no. 2, 2020, pp. 178-186.