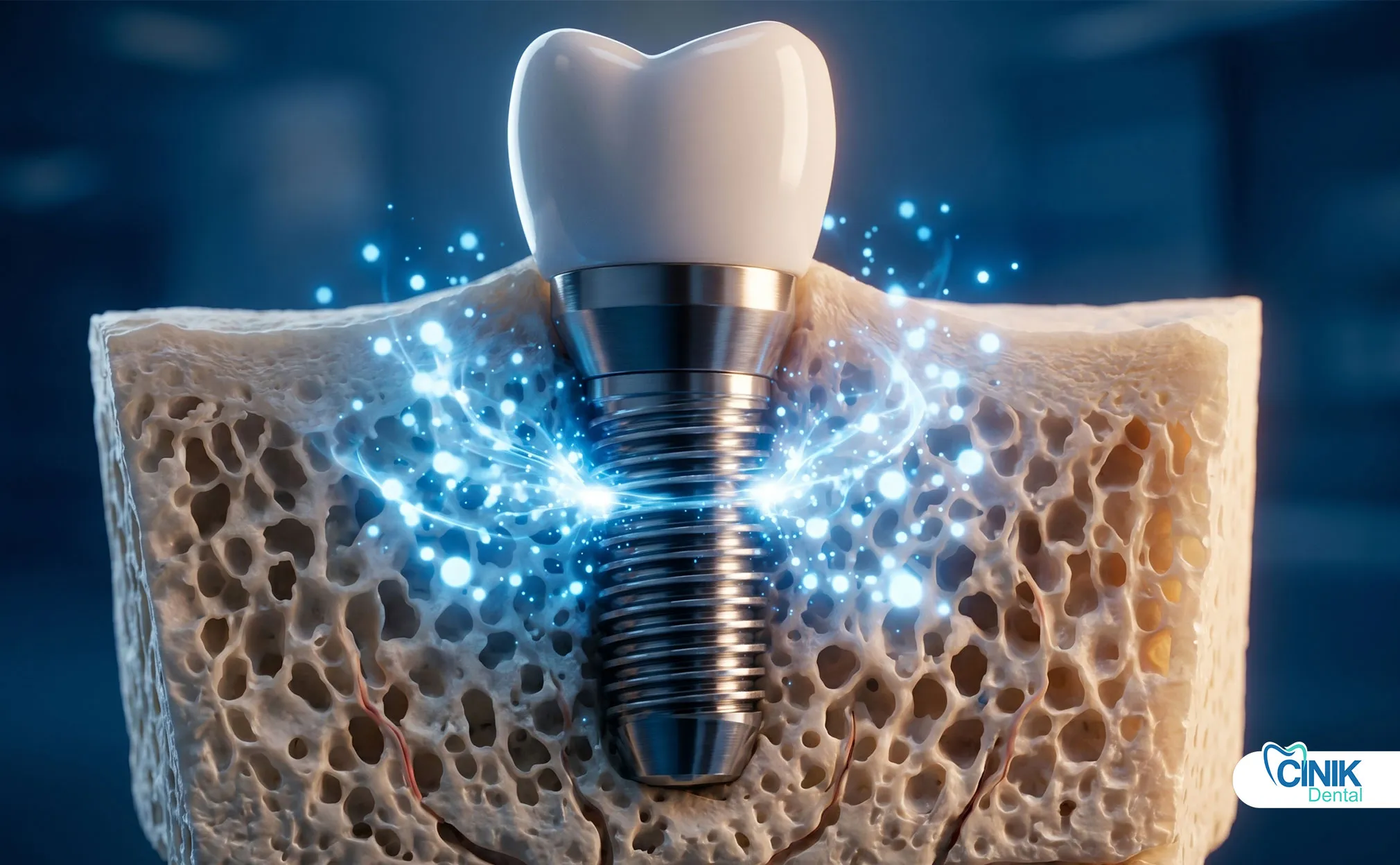
What Is Exosome Therapy and Why Does It Matter for Dental Implants?
Exosome therapy represents a breakthrough in regenerative dentistry. This cell-free treatment uses tiny vesicles to accelerate bone healing, reduce inflammation, and improve implant success rates. Unlike traditional stem cell approaches, exosome therapy delivers growth factors without living cells, eliminating risks of rejection or tumor formation.
Dental implants serve as the gold standard for tooth replacement. However, clinicians face persistent challenges. Some patients experience delayed healing. Others suffer from peri-implant inflammation or insufficient bone density. These complications compromise implant stability and longevity.
Regenerative dentistry now turns to exosomes as a solution. These nanoscale particles act as biological messengers. They carry proteins, RNA, and lipids that stimulate natural repair processes. Research shows they enhance osseointegration, the critical fusion between implant and bone (Valadi et al., 2007). This article examines how exosome therapy transforms implant dentistry through scientific mechanisms, clinical applications, and future potential.
What Are Exosomes and How Do They Function in Tissue Repair?
Exosomes are extracellular vesicles measuring 30 to 150 nanometers in diameter. Cells release these bubbles to communicate with neighboring tissues. They originate from the endosomal pathway through a process called multivesicular body fusion. Think of them as biological text messages. One cell sends instructions. Another cell receives the signal and changes its behavior.
Table 1: Core Components of Exosomes and Their Functions
Component | Function | Therapeutic Impact |
Proteins | Cell signaling | Activate repair pathways |
miRNA | Gene regulation | Control inflammation and bone growth |
mRNA | Protein synthesis | Direct tissue regeneration |
Lipids | Membrane structure | Ensure stability and cell fusion |
The composition varies by source cell. Mesenchymal stem cell-derived exosomes (MSC-exosomes) carry over 850 proteins including transforming growth factor-β and insulin growth factor (Zhang et al., 2020). Dental pulp stem cells release exosomes enriched with osteogenic miRNAs. This specialized cargo explains why exosomes from different sources produce distinct healing effects.
Exosomes solve major problems associated with stem cell therapy. Stem cells can trigger immune reactions. They may form tumors. They require strict storage conditions. Exosomes bypass these issues entirely. They offer low immunogenicity, high biocompatibility, and reduced safety concerns (Shi et al., 2021). Patients receive the regenerative benefits without the cellular risks.
How Do Exosomes Promote Bone Formation Around Dental Implants?
What Mechanisms Drive Osteogenesis Enhancement?
Exosomes activate multiple pathways to build bone. They stimulate osteoblast differentiation. They increase bone matrix deposition. They boost mineralization throughout the healing site.
Research by Furuta et al. (2016) demonstrates that MSC-exosomes promote fracture healing in mouse models. The exosomes elevate alkaline phosphatase (ALP) activity. This enzyme serves as an early marker of bone formation. Osteocalcin (OCN) levels rise as well. This protein indicates mature bone matrix development.
Three primary signaling pathways drive these effects:
BMP/Smad Pathway: Exosomes deliver bone morphogenetic proteins. These proteins bind to cell surface receptors. They activate Smad transcription factors. Runx2 and Osterix expression increases. Bone formation accelerates.
Wnt/β-catenin Pathway: Exosomes stabilize β-catenin in recipient cells. This molecule enters the nucleus. It activates genes responsible for cell proliferation and differentiation. Zhang et al. (2020) found that human umbilical cord MSC-exosomes reduce bone loss through this mechanism.
PI3K/AKT Pathway: Exosomes trigger survival signals in target cells. This prevents apoptosis during the critical early healing phase. Studies show that inhibiting this pathway blocks exosome-induced bone formation (Chen et al., 2019).
How Do Exosomes Improve Blood Supply to Implant Sites?
Angiogenesis proves essential for successful osseointegration. Bone tissue needs oxygen and nutrients. Without adequate vascularization, implants fail.
Exosomes stimulate vascular endothelial growth factor (VEGF) production. They encourage endothelial cells to form tube-like structures. Qi et al. (2016) observed that hiPS-MSC-exosomes combined with β-TCP scaffolds enhanced both bone regeneration and angiogenesis in rat models. The vessels penetrated deeper into the bone graft material. This dual action, bone building plus vessel creation, creates a favorable environment for implant integration.
What Role Do Exosomes Play in Controlling Inflammation?
Inflammation destroys implants. Peri-implantitis affects up to 20% of dental implant patients. Traditional antibiotics help but create resistance problems. Exosomes offer a biological solution.
Dental pulp stem cell-derived exosomes (DPSC-EXO) suppress pro-inflammatory cytokines. They inhibit IL-1β and TNF-α production. They block the IL-6/JAK2/STAT3 signaling pathway (Li et al., 2023). This pathway drives destructive inflammation in periodontal tissues.
Macrophages change their behavior after exosome exposure. Pro-inflammatory M1 macrophages transform into anti-inflammatory M2 macrophages. This polarization shift reduces tissue damage. It creates a pro-healing environment around the implant (Shen et al., 2020).
Where Can Clinicians Apply Exosome Therapy in Implant Dentistry?
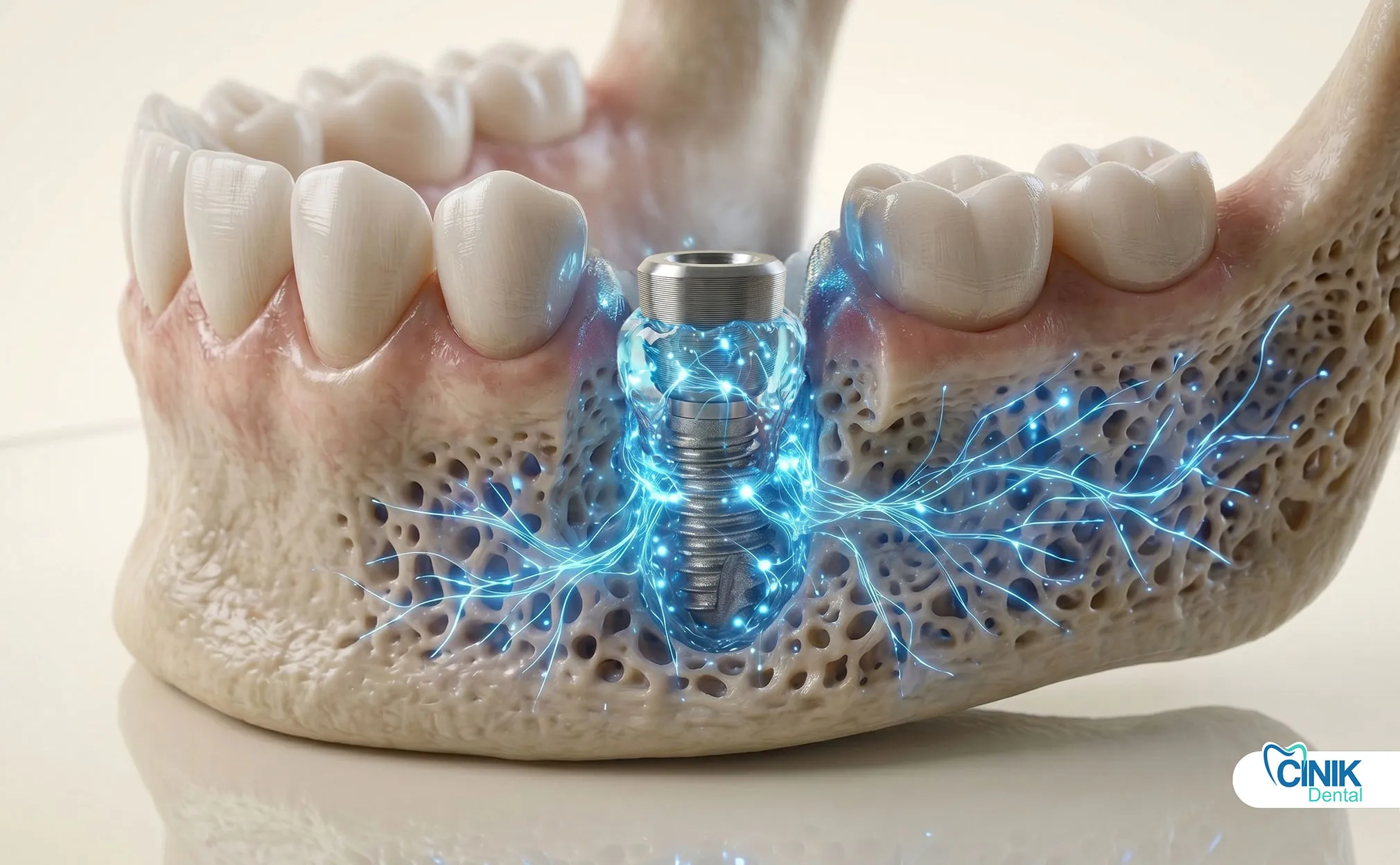
Can Exosomes Accelerate Osseointegration in Standard Implant Cases?
Yes. Exosomes improve bone-to-implant contact significantly. They speed up integration timelines. Traditional osseointegration requires three to six months. Exosome therapy may reduce this period by 30 to 40% based on preclinical data.
Wang et al. (2020) developed a self-healing hydrogel containing umbilical cord MSC-exosomes. The material promoted bone regeneration in critical-sized defects. The bone volume fraction increased compared to control groups. This suggests faster and more robust implant integration when exosomes are present.
Do Exosomes Help Patients with Insufficient Bone?
Absolutely. Alveolar bone regeneration represents a major application. Many patients lack adequate bone for immediate implant placement. Exosomes enhance bone grafting procedures. They improve ridge augmentation outcomes. They prevent bone resorption after extraction.
Table 2: Exosome Sources and Their Regenerative Properties
Source | Osteogenic Potential | Immunomodulatory Strength | Accessibility |
Bone Marrow MSCs | High | Moderate | Invasive |
Dental Pulp Stem Cells | Very High | Very High | Minimally invasive |
Periodontal Ligament | High | High | Moderate |
Gingival MSCs | Moderate | Very High | Easy |
Dental stem cells provide superior exosomes for oral applications. They express specific markers like CD24 and CD140a. These cells proliferate faster than bone marrow alternatives. They resist senescence during culture expansion. Most importantly, they naturally adapt to the oral environment (Kotova et al., 2021).
Can Exosomes Heal Soft Tissues Around Implants?
Soft tissue seals prevent bacterial invasion. They protect the underlying bone. Exosomes accelerate gingival wound healing. They stimulate fibroblast migration and collagen production.
Zhou et al. (2022) demonstrated that exosome-functionalized scaffolds enhanced soft tissue integration. The gingival epithelium healed more completely. This reduced post-surgical complications. It improved final aesthetic outcomes for anterior implant restorations.
Are Exosomes Effective Against Peri-Implant Diseases?
Research strongly supports this application. Peri-implantitis involves bacterial infection and inflammatory bone loss. Exosomes provide dual protection. They modulate immune responses. They also carry antimicrobial peptides.
Lei et al. (2022) showed that stem cell-derived exosomes treated inflammatory bone loss in periodontitis models. The bone volume fraction improved significantly. Tartrate-resistant acid phosphatase (TRAP)-positive osteoclasts decreased. This indicates reduced bone destruction.
What Sources Provide the Best Exosomes for Dental Applications?
Mesenchymal stem cells remain the primary source. However, dental tissues offer unique advantages.
Dental Pulp Stem Cells (DPSCs): These cells reside inside tooth structures. They demonstrate high proliferative rates. They maintain strong osteogenic potential even after multiple passages. DPSC-exosomes contain specific miRNAs that promote angiogenesis and neuroprotection.
Periodontal Ligament Stem Cells (PDLSCs): These cells connect teeth to bone. They naturally regulate periodontal homeostasis. Their exosomes excel at soft tissue regeneration and bone-ligament interface formation.
Stem Cells from Human Exfoliated Deciduous Teeth (SHEDs): These cells come from baby teeth. They show exceptional plasticity. They express early stem cell markers longer than other sources. SHED-exosomes may offer superior neuroregenerative properties.
Engineered Exosomes: Scientists now load exosomes with specific cargo. They add HIF-1α to boost angiogenesis. They incorporate miR-375 to enhance osteogenesis (Chen et al., 2019). This customization allows targeted therapy for specific implant complications.
What Clinical Benefits Do Patients Receive from Exosome Therapy?
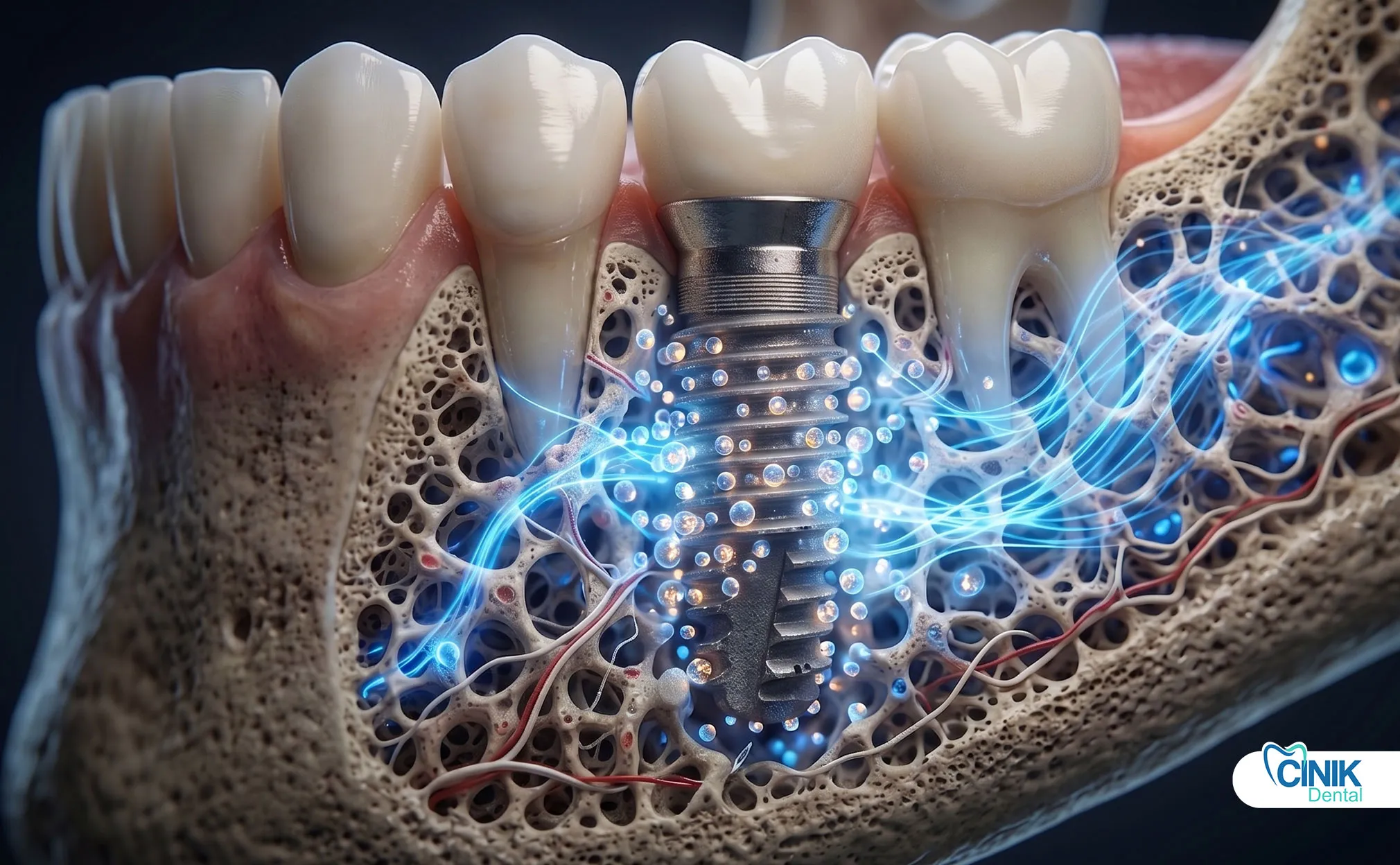
Patients experience measurable improvements:
Faster Healing: Exosome-treated sites show earlier bone mineralization. Soft tissues close more rapidly. This reduces the time between implant placement and final restoration.
Less Pain and Swelling: The anti-inflammatory action reduces post-operative discomfort. Patients report lower pain scores. They require fewer analgesic medications.
Higher Success Rates: Early integration prevents micromotion. This reduces implant failure. Exosomes may prove especially valuable for patients with diabetes, osteoporosis, or smoking histories, groups traditionally considered high-risk.
Minimally Invasive Delivery: Clinicians apply exosomes through hydrogels, collagen membranes, or direct injection. No additional surgery is required. The therapy integrates seamlessly into standard implant protocols.
Personalized Possibilities: Future treatments may use patient-specific exosomes. Cells harvested from extracted wisdom teeth could provide personalized regenerative therapies.
What Limitations and Challenges Currently Exist?
Why Isn't Exosome Therapy Widely Available Yet?
Evidence Gaps: Most studies remain preclinical. Researchers have conducted extensive animal trials. Human clinical trials lag behind. Long-term data on implant survival rates with exosome therapy does not yet exist.
Standardization Problems: No universal protocol exists for exosome isolation. Differential ultracentrifugation remains popular but produces variable yields. Precipitation methods increase quantity but reduce purity. Microfluidic technologies promise consistency but require expensive equipment (Miron et al., 2025).
Regulatory Hurdles: Regulatory agencies classify exosomes as biological products. They require extensive safety testing. Mass production must meet Good Manufacturing Practice standards. These requirements slow clinical adoption.
Technical Barriers: Exosomes degrade during storage. They require specific temperature conditions. They lose activity if mishandled. Delivery systems must protect exosomes until they reach target tissues. Current scaffolds and hydrogels provide partial solutions. Better carriers are needed.
How Do Exosomes Compare to Other Regenerative Treatments?
Table 3: Comparison of Regenerative Therapies
Feature | Exosomes | Stem Cells | PRP | Bone Graft Materials |
Cell-free | Yes | No | Partial | Yes |
Immunogenicity | Very low | Moderate | Low | Very low |
Tumor risk | None | Low | None | None |
Growth factor concentration | Very high | Moderate | Moderate | Low |
Handling complexity | Moderate | High | Low | Low |
Cost | Moderate | High | Low | Variable |
Exosomes outperform stem cells in safety. They avoid the commitment risk. They eliminate concerns about unpredictable cell differentiation in vivo. They provide three times the growth factor concentration of adult stem cells according to recent analyses.
Compared to platelet-rich plasma (PRP), exosomes offer greater consistency. PRP quality varies by patient age and health status. Exosomes from cultured stem cells maintain standardized potency. They deliver predictable therapeutic effects.
Bone graft materials provide structural support. Exosomes provide biological instruction. The combination proves superior. β-TCP scaffolds loaded with exosomes regenerate bone faster than scaffolds alone (Ying et al., 2020).
What Future Developments Will Shape Exosome Therapy?
Personalized Exosome Therapies: Clinicians will extract stem cells from patient dental tissues. They will culture these cells and harvest exosomes. This autologous approach eliminates all rejection risks. It maximizes therapeutic compatibility.
Smart Biomaterial Integration: 3D-printed implants will incorporate exosome reservoirs. These scaffolds will release vesicles gradually. They will provide sustained stimulation throughout the healing period.
Gene-Loaded Exosomes: Scientists will engineer exosomes carrying specific genetic instructions. They will target peri-implantitis pathways. They will accelerate nerve regeneration in implant sites.
AI-Driven Treatment Planning: Machine learning algorithms will predict optimal exosome concentrations. They will determine ideal delivery timing. They will personalize protocols based on patient genetics and bone quality.
How Should Clinicians Implement Exosome Therapy?
Patient Selection: Ideal candidates include patients with low bone density. Smokers and diabetics benefit particularly. Patients requiring immediate implant placement in extraction sites show improved outcomes.
Contraindications: Patients with active infections require treatment first. Those with bleeding disorders need careful evaluation. Pregnant patients should wait until postpartum due to limited safety data.
Integration Protocols: Clinicians should incorporate exosomes during implant placement. They can apply them to the osteotomy site before implant insertion. They can soak collagen membranes in exosome solutions. They can mix exosomes with bone graft materials for sinus lift procedures.
Cost Considerations: Currently, exosome therapy adds $500 to $2,000 to implant procedures. Prices will decrease as production scales. Insurance coverage remains limited. Patients should understand this represents an out-of-pocket investment in faster healing.
Conclusion
Exosome therapy for dental implants offers a powerful regenerative tool. These cell-free vesicles accelerate bone formation. They reduce inflammation. They improve implant stability. They avoid the risks associated with living cell therapies.
Current evidence supports their use for enhancing osseointegration. They show particular promise for bone regeneration in deficient sites. They offer solutions for peri-implant disease management. They integrate smoothly with advanced implant techniques.
However, clinicians must acknowledge limitations. Long-term human clinical trials remain necessary. Standardization efforts must continue. Regulatory frameworks need development.
The field advances rapidly. DPSC-exosomes demonstrate superior potential for oral applications. Engineering techniques improve targeting and potency. Delivery systems become more sophisticated.
For patients, this means faster healing. It means reduced complications. It means broader candidacy for implant treatment. For the profession, it represents a shift toward biological rather than merely mechanical implant integration.
Exosome therapy stands at the intersection of cell biology and clinical dentistry. It bridges laboratory discovery and patient care. While not yet routine, it soon will be. Clinicians who understand these mechanisms now will lead implant dentistry tomorrow.
References
Chen, Shiyi, et al. "Exosomes Derived from miR-375-Overexpressing Human Adipose Mesenchymal Stem Cells Promote Bone Regeneration." Cell Proliferation, vol. 52, no. 5, 2019, doi:10.1111/cpr.12669.
Fan, Linlin, et al. "Exosome-Functionalized Polyetheretherketone-Based Implant with Immunomodulatory Property for Enhancing Osseointegration." Bioactive Materials, vol. 6, no. 9, 2021, pp. 2754–66, doi:10.1016/j.bioactmat.2021.02.005.
Furuta, T., et al. "Mesenchymal Stem Cell-Derived Exosomes Promote Fracture Healing in a Mouse Model." Stem Cells Translational Medicine, vol. 5, no. 12, 2016, pp. 1620–30, doi:10.5966/sctm.2015-0285.
Kotova, A., et al. "Comparative Analysis of Dental Pulp and Periodontal Stem Cells: Differences in Morphology, Functionality, Osteogenic Differentiation and Proteome." Biomedicines, vol. 9, no. 11, 2021, p. 1606, doi:10.3390/biomedicines9111606.
Lei, Fengyang, et al. "Treatment of Inflammatory Bone Loss in Periodontitis by Stem Cell-Derived Exosomes." Acta Biomaterialia, vol. 141, 2022, pp. 333–43, doi:10.1016/j.actbio.2021.12.035.
Li, Mei, et al. "Dental Pulp Stem Cell-Derived Exosomes Regulate Anti-Inflammatory and Osteogenesis in Periodontal Ligament Stem Cells and Promote the Repair of Experimental Periodontitis in Rats." Frontiers in Bioengineering and Biotechnology, vol. 11, 2023, doi:10.3389/fbioe.2023.10441659.
Miron, Richard J., et al. "Isolation Methods of Exosomes Derived from Dental Stem Cells." International Journal of Oral Science, 2025, doi:10.1038/s41368-025-00370-y.
Qi, X., et al. "Exosomes Secreted by Human-Induced Pluripotent Stem Cell-Derived Mesenchymal Stem Cells Repair Critical-Sized Bone Defects through Enhanced Angiogenesis and Osteogenesis in Osteoporotic Rats." International Journal of Biological Sciences, vol. 12, no. 7, 2016, pp. 836–49, doi:10.7150/ijbs.14809.
Shen, Zhenhua, et al. "Chitosan Hydrogel Incorporated with Dental Pulp Stem Cell-Derived Exosomes Alleviates Periodontitis in Mice via a Macrophage-Dependent Mechanism." Bioactive Materials, vol. 5, no. 4, 2020, pp. 1113–26, doi:10.1016/j.bioactmat.2020.07.002.
Shi, Qin, et al. "MSC-Derived Exosomes: A Novel Promising Therapy for Osteoporosis." Frontiers in Cell and Developmental Biology, vol. 9, 2021, p. 723803, doi:10.3389/fcell.2021.723803.
Valadi, Hadi, et al. "Exosome-Mediated Transfer of mRNAs and microRNAs Is a Novel Mechanism of Genetic Exchange between Cells." Nature Cell Biology, vol. 9, no. 6, 2007, pp. 654–59, doi:10.1038/ncb1596.
Wang, Ling, et al. "A New Self-Healing Hydrogel Containing hucMSC-Derived Exosomes Promotes Bone Regeneration." Frontiers in Bioengineering and Biotechnology, vol. 8, 2020, p. 564731, doi:10.3389/fbioe.2020.564731.
Ying, Chang, et al. "BMSC-Exosomes Carry Mutant HIF-1α for Improving Angiogenesis and Osteogenesis in Critical-Sized Calvarial Defects." Frontiers in Bioengineering and Biotechnology, vol. 8, 2020, p. 565561, doi:10.3389/fbioe.2020.565561.
Zhang, Shiqing, et al. "MSC Exosomes Alleviate Temporomandibular Joint Osteoarthritis by Attenuating Inflammation and Restoring Matrix Homeostasis." Biomaterials, vol. 200, 2019, pp. 35–47, doi:10.1016/j.biomaterials.2019.02.006.
Zhou, Ye, et al. "Polydopamine-Coated Biomimetic Bone Scaffolds Loaded with Exosomes Promote Osteogenic Differentiation of BMSC and Bone Regeneration." Regenerative Therapy, vol. 23, 2023, pp. 25–36, doi:10.1016/j.reth.2023.03.005.