Dental veneers last between 5 and 20 years depending on material choice, clinical execution, and patient maintenance. Porcelain veneers demonstrate superior durability with 10-15 year lifespans, while composite alternatives typically require replacement after 5-7 years.
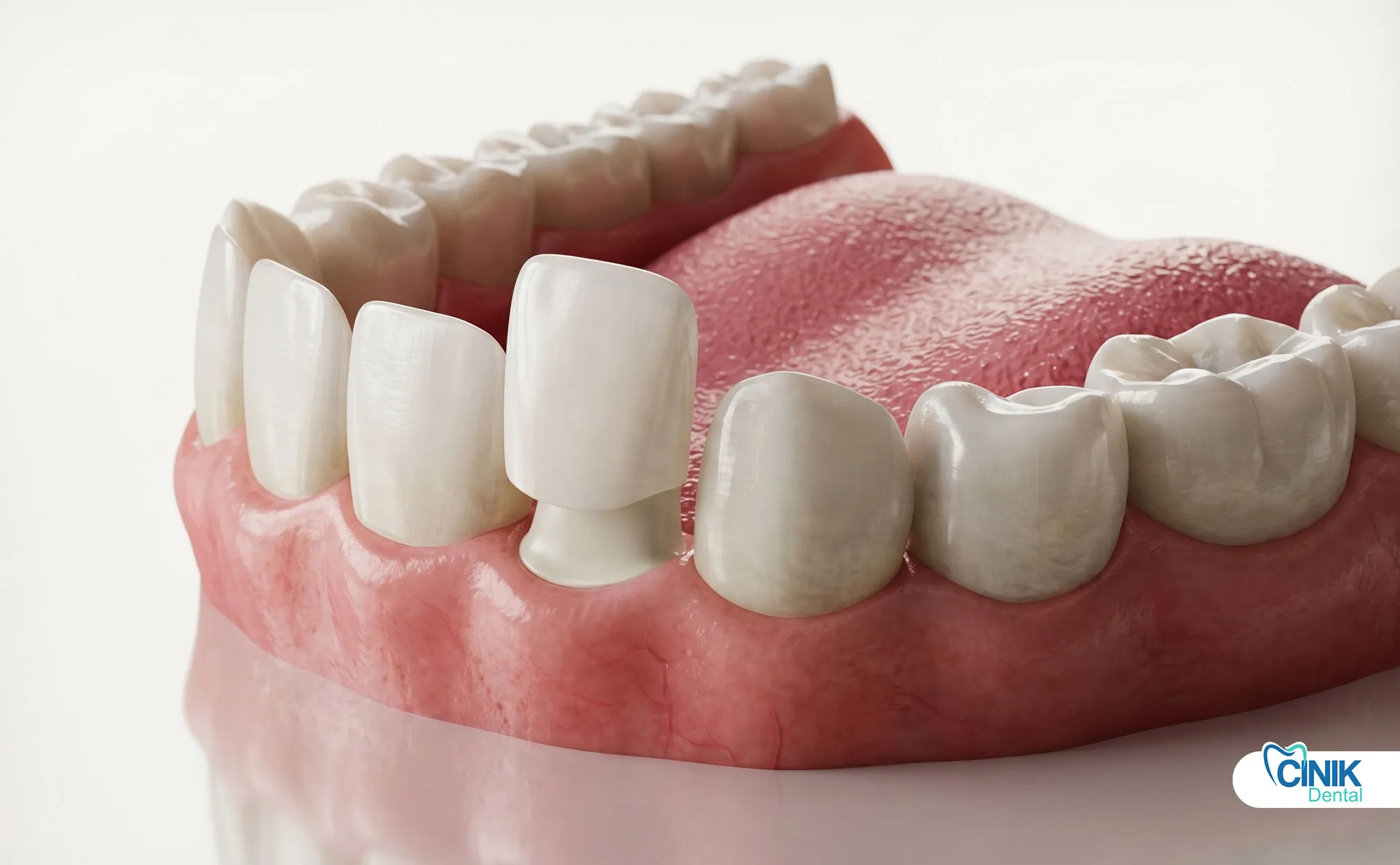
Dental veneers represent one of the most popular aesthetic interventions in contemporary dentistry. These thin, custom-crafted shells bond directly to the facial surfaces of teeth to correct discoloration, chips, gaps, and minor misalignments. Patients invest significant resources in these restorations, so understanding the longevity of dental veneers becomes crucial for treatment planning and informed consent.
This comprehensive review examines the scientific evidence surrounding veneer durability, comparing material performance across decades of clinical research. We analyze survival rates, identify failure mechanisms, and provide evidence-based strategies for maximizing restoration lifespan. The article synthesizes data from longitudinal studies, systematic reviews, and material science research to offer clinicians and patients a clear understanding of realistic outcomes.
What Should Patients Know About Dental Veneer Longevity?
Patients should understand that veneers offer long-term but not permanent solutions. Porcelain provides the longest service life, while composite offers shorter-term aesthetics at lower cost. Success depends heavily on home care and clinical technique.
The demand for aesthetic dental treatments has surged globally over the past two decades. Patients seek durable solutions that balance beauty with function. Dental veneers emerged as the treatment of choice because they preserve more tooth structure than full crowns while delivering dramatic cosmetic improvements. However, misconceptions abound regarding their permanence and maintenance requirements.
Clinical decision-making requires accurate prognostic data. Dentists must communicate realistic timeframes so patients understand that replacement becomes inevitable eventually. The primary keyword, longevity of dental veneers, encompasses not just chronological survival but also the maintenance of aesthetic and functional parameters throughout the restoration's service life.
What Types of Dental Veneers Offer the Best Longevity?
Feldspathic porcelain and lithium disilicate ceramics offer the best longevity, typically exceeding 10-15 years. Composite resin veneers provide shorter service lives of 5-7 years but allow easier repair.
Material selection fundamentally determines how long do veneers last. Three primary categories dominate current clinical practice: conventional porcelain ceramics, composite resins, and emerging ultra-thin ceramic systems. Each material exhibits distinct mechanical properties, aesthetic characteristics, and degradation patterns that influence clinical performance over time.
What Makes Porcelain Veneers Last Longer Than Other Materials?
Porcelain veneers exhibit superior longevity due to high fracture resistance, excellent color stability, and strong chemical bonding with enamel. These properties allow them to withstand masticatory forces while maintaining surface integrity for decades.
Porcelain veneers utilize either feldspathic porcelain or lithium disilicate glass-ceramics. Feldspathic porcelain, the traditional standard, contains silica, alumina, and potassium oxide in a glass matrix. This composition creates a restoration with flexural strength between 60-90 MPa (Magne and Belser 2003). Lithium disilicate, a newer high-strength ceramic, offers flexural strength exceeding 360 MPa, making it suitable for even minimal-preparation designs.
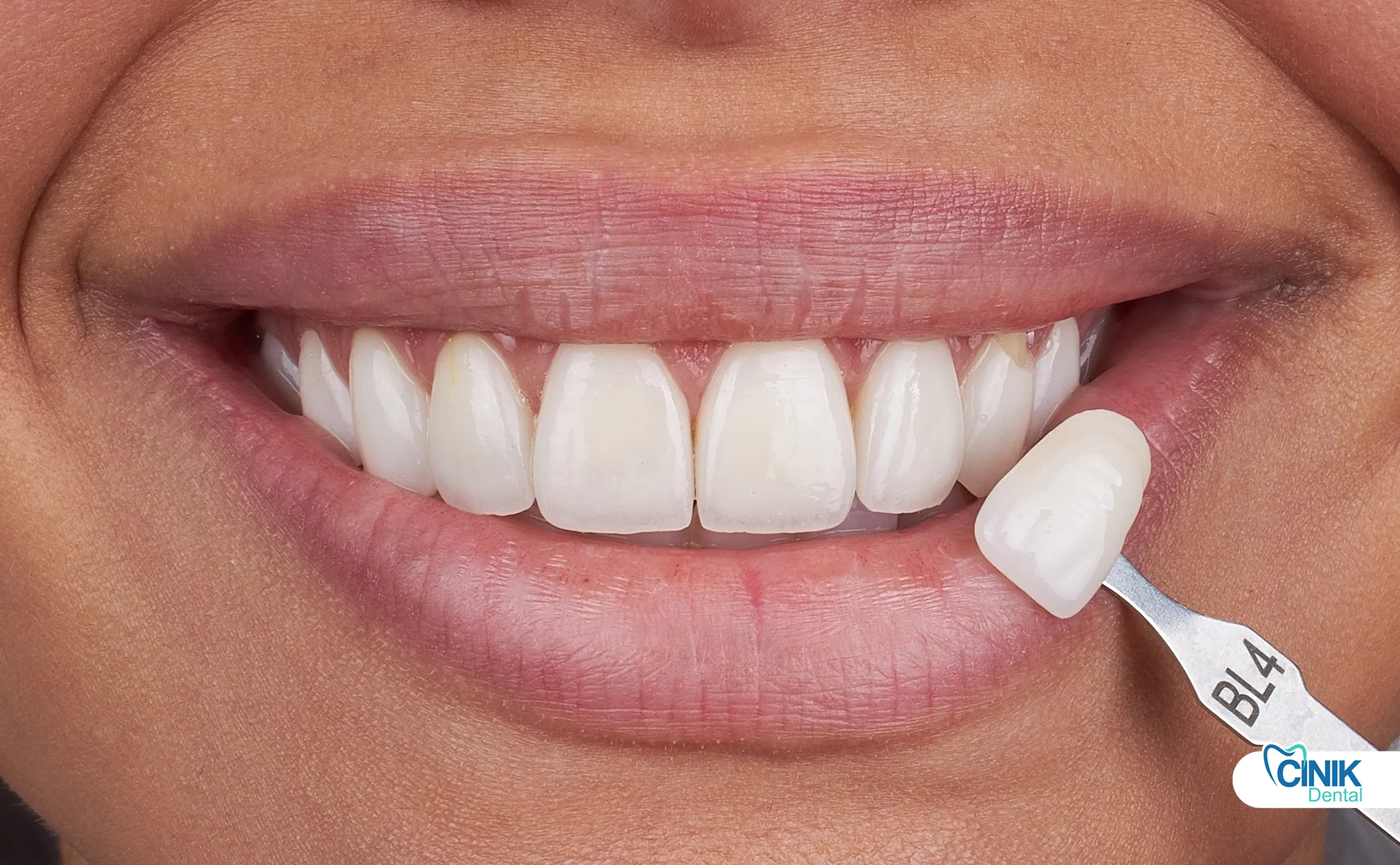
Ceramic materials resist wear exceptionally well. Unlike natural enamel or composite resins, dental porcelain demonstrates low abrasiveness against opposing dentition while maintaining surface gloss. This wear resistance proves crucial for long-term aesthetics. Additionally, porcelain's vitreous nature prevents staining from coffee, wine, or tobacco, preserving the original shade for years.
The bonding mechanism enhances porcelain's durability. Etching with hydrofluoric acid creates micromechanical retention, while silane coupling agents establish chemical bonds between the ceramic and resin cement. This adhesive interface, when properly executed, creates a seal that prevents microleakage and secondary caries. Research by Blatz et al. (2018) confirms that resin-bonded ceramics demonstrate survival rates exceeding 95% at 10 years when enamel remains the primary substrate.
Why Do Composite Resin Veneers Have Shorter Lifespans?
Composite veneers last 5-7 years on average due to lower wear resistance, susceptibility to staining, and material fatigue. They absorb water and discolor over time, requiring more frequent replacement than ceramic alternatives.
Composite resin veneers utilize bis-GMA-based materials with inorganic filler particles. While direct composite veneers offer immediate results and lower costs, they cannot match the porcelain veneers lifespan. Composite materials exhibit greater thermal expansion coefficients than tooth structure, leading to marginal gaps over time. These microgaps permit staining and bacterial ingress.
Surface degradation presents another limitation. Composite resins undergo oxidation and water sorption, causing color shifts and loss of surface luster. Polishing can restore some shine, but the material inevitably requires replacement as polymerization shrinkage and fatigue create microcracks. Studies indicate that composite veneers require maintenance polishing every 2-3 years and replacement within 5-7 years under normal function (Gresnigt et al. 2019).
However, composite offers distinct advantages for specific situations. Direct techniques allow chairside modifications and repairs. When a composite veneer chips, dentists can add material rather than replacing the entire restoration. This repairability partially offsets the shorter lifespan, particularly for younger patients or those with limited budgets.
How Do Emerging Technologies Improve Veneer Durability?
CAD/CAM technology and high-translucency zirconia create veneers with optimized thickness and strength. These systems allow ultra-thin preparations (0.3-0.5mm) while maintaining fracture resistance comparable to traditional porcelain.
No-prep and minimal-prep veneers represent significant advances in adhesive dentistry. These ultra-thin ceramic laminates (0.3-0.7mm thick) preserve enamel while covering aesthetic imperfections. CAD/CAM fabrication ensures precise marginal adaptation, reducing the risk of debonding and marginal discoloration. Computer-aided design allows optimization of material thickness based on occlusal load patterns.
High-translucency zirconia (5Y-TZP) offers another breakthrough. This material combines the strength of zirconia (500-1000 MPa flexural strength) with aesthetics rivaling lithium disilicate. Early clinical data suggests 5-year survival rates comparable to lithium disilicate, though long-term data beyond 10 years remains limited (Papachroni et al. 2020).
Adhesive systems continue evolving. Universal adhesives with improved enamel etching capabilities and moisture tolerance simplify bonding protocols. These advances reduce technique sensitivity, potentially improving clinical outcomes and extending restoration longevity across all material types.
How Long Do Dental Veneers Actually Last According to Clinical Studies?
Clinical studies demonstrate 95% survival rates for porcelain veneers at 10 years, dropping to 80-85% at 20 years. Composite veneers show 70-80% survival at 10 years.
Scientific literature provides robust data on veneer survival rates, though study designs vary significantly. Longitudinal research tracking the same patient cohorts over decades offers the most reliable indicators of expected lifespans. Meta-analyses and systematic reviews aggregate this data to establish evidence-based prognoses.
What Is the Average Lifespan of Porcelain vs Composite Veneers?
Porcelain veneers average 10-15 years, with many lasting 20+ years. Composite veneers average 5-7 years. These figures represent mean values; individual results vary based on clinical and behavioral factors.
The porcelain vs composite veneer lifespan comparison heavily favors ceramic materials. A landmark study by Burke et al. (2019) analyzing 2,000 porcelain veneers over 20 years found a mean survival time of 15.2 years. Lithium disilicate veneers specifically showed 97% survival at 5 years and 94% at 10 years. Feldspathic porcelain demonstrated slightly lower rates at 91% over 10 years.
Composite data shows more variability. Direct composite veneers survive 5-7 years on average, with survival rates of 95% at 3 years, 85% at 5 years, and 70% at 7 years. Indirect composite veneers (fabricated in laboratories) show marginally better results, reaching 8-10 year lifespans in some studies.
The general veneer lifespan range spans from 5 years (early composite failures) to 30+ years (well-maintained porcelain on non-bruxing patients). This broad spectrum reflects the interaction between material properties, clinical technique, and patient biology.
What Do Survival Rates Reveal About Long-Term Veneer Performance?
Survival rates indicate that most veneer failures occur within the first 5 years (initial adjustment period) or after 15 years (material fatigue). The period between 5-15 years shows the highest stability.
Survival analysis differentiates between "survival" (restoration still in place) and "success" (restoration in place and meeting all aesthetic/functional criteria). While a veneer may survive (remain attached) for 20 years, it may show marginal discoloration or minor chipping that classifies it as a "failure" under strict success criteria.
Layton et al. (2012) reported that porcelain veneers maintained 95% survival at 10 years but only 64% met strict success criteria due to minor color changes at margins. This distinction matters for patient education. The restoration remains functional but may require aesthetic touch-ups.
For composite veneers durability, survival curves show steeper declines after year 5. The material accumulates wear and staining that patients find unacceptable, triggering replacement even if the veneer remains structurally intact.
Which Material Provides Superior Long-Term Value?
Porcelain provides superior long-term value despite higher initial costs. When calculated per year of service, porcelain costs less than composite due to its extended lifespan and lower maintenance requirements.
Economic analysis supports ceramic selection for permanent aesthetic solutions. While composite veneers cost 50-70% less initially, their shorter lifespans necessitate multiple replacements over a 20-year period. Porcelain requires replacement once (or never), making it more cost-effective long-term.
Additionally, porcelain requires fewer maintenance appointments. Composite demands regular polishing and occasional repair, adding clinical time and expense. The cumulative cost of composite maintenance often exceeds the initial price difference within 8-10 years.
What Factors Determine How Long Your Veneers Will Last?

Five primary factors control veneer longevity: patient oral hygiene, parafunctional habits, preparation design, bonding protocol, and occlusal management. Enamel preservation proves particularly critical for long-term adhesion.
The factors affecting veneer longevity span biological, mechanical, and technical domains. No single element determines success; rather, the interaction between patient behavior, clinical execution, and material properties creates the conditions for either premature failure or decades of service.
How Do Patient Habits Affect Veneer Longevity?
Poor oral hygiene, bruxism, and dietary choices significantly reduce veneer lifespan. Patients who grind their teeth without nightguards experience 3-5 times higher failure rates.
Patient-related variables often outweigh material selection in determining outcomes. Oral hygiene practices directly impact the gingival interface where veneers end. Inadequate flossing allows plaque accumulation at margins, leading to gingivitis, recession, and eventual margin exposure. While veneers themselves cannot decay, the underlying tooth structure remains vulnerable to caries at the preparation margin.
Dietary habits influence both aesthetics and structure. Frequent consumption of acidic beverages (sodas, citrus, wine) erodes exposed cement layers and roughens ceramic surfaces. Dark-colored foods and drinks stain composite margins and cement layers over time. Extremely hard foods (ice, hard candy) create fracture risks, particularly for patients with edge-to-edge bites.
Parafunctional habits present the greatest risk. Bruxism (nocturnal grinding) generates forces exceeding 800 Newtons, far beyond normal chewing forces (100-150 Newtons). These loads eventually cause ceramic fracture or debonding. Nail biting, pen chewing, and thread cutting with teeth create point stresses that initiate cracks.
Why Does Clinical Technique Influence Veneer Survival?
Enamel preservation, margin placement, and adhesive protocol execution determine bond strength. Veneers bonded primarily to enamel show 95% 10-year survival versus 60% for those bonded to dentin.
Operator skill significantly impacts outcomes. Tooth preparation design must balance aesthetic requirements with structural preservation. Aggressive preparation removes enamel, forcing bonding to less reliable dentin substrates. Enamel bonding achieves superior strength because resin tags penetrate etched enamel prisms, creating micro mechanical retention exceeding 20 MPa shear bond strength.
Margin placement requires precision. Supragingival margins (above the gumline) permit easy cleaning but may show aesthetic limitations. Subgingival margins (below the gumline) hide transitions but risk periodontal inflammation if placed too deep. Equigingival placement (at gum level) offers the best compromise for longevity.
Bonding protocol execution demands meticulous isolation and technique. Saliva contamination during cementation reduces bond strength by 50% or more. Proper etching times (15-30 seconds for enamel), thorough rinsing, and careful adhesive application without pooling determine the seal quality. Simplified adhesive systems show higher technique sensitivity, suggesting that multi-step etch-and-rinse protocols may provide more predictable long-term results (Peumans et al. 2020).
What Material Properties Impact Durability?
Ceramic thickness, flexural strength, and coefficient of thermal expansion determine fracture resistance. Thinner ceramics (0.3mm) require stronger materials like lithium disilicate to survive functional loads.
Material science explains why some veneers last decades while others fail within years. Ceramic thickness directly correlates with strength, thicker veneers resist fracture better but require more tooth reduction. Ultra-thin veneers (0.3mm) conserve tooth structure but demand high-strength materials like lithium disilicate or zirconia rather than feldspathic porcelain.
The quality of composite resin varies significantly between manufacturers. Nano-filled composites demonstrate better wear resistance and polishability than micro-filled or hybrid alternatives. However, all composites undergo color shifts over time due to water sorption and oxidation.
Advances in bonding agents improve durability. Modern universal adhesives contain silane primers for ceramic coupling and 10-MDP monomers for chemical bonding to hydroxyapatite. These molecular bonds supplement micromechanical retention, creating more durable interfaces.
How Does Bite Alignment Affect Veneer Lifespan?
Proper occlusal load distribution prevents focal stress points. Veneers on anterior teeth subjected to heavy anterior guidance or edge-to-edge bites fail earlier than those in protected occlusion.
Occlusal design significantly influences mechanical survival. Veneers placed on teeth bearing excessive loads, such as the guidance patterns in canine-protected occlusion, experience more stress than those in group function. Edge-to-edge bites concentrate forces on the incisal edges, the thinnest portion of the veneer.
Bite alignment must be evaluated before veneer placement. Patients with class III malocclusions, deep bites, or crossbites present higher risks. Orthodontic pretreatment may be necessary to redistribute forces before aesthetic restoration.
Why Do Dental Veneers Fail?
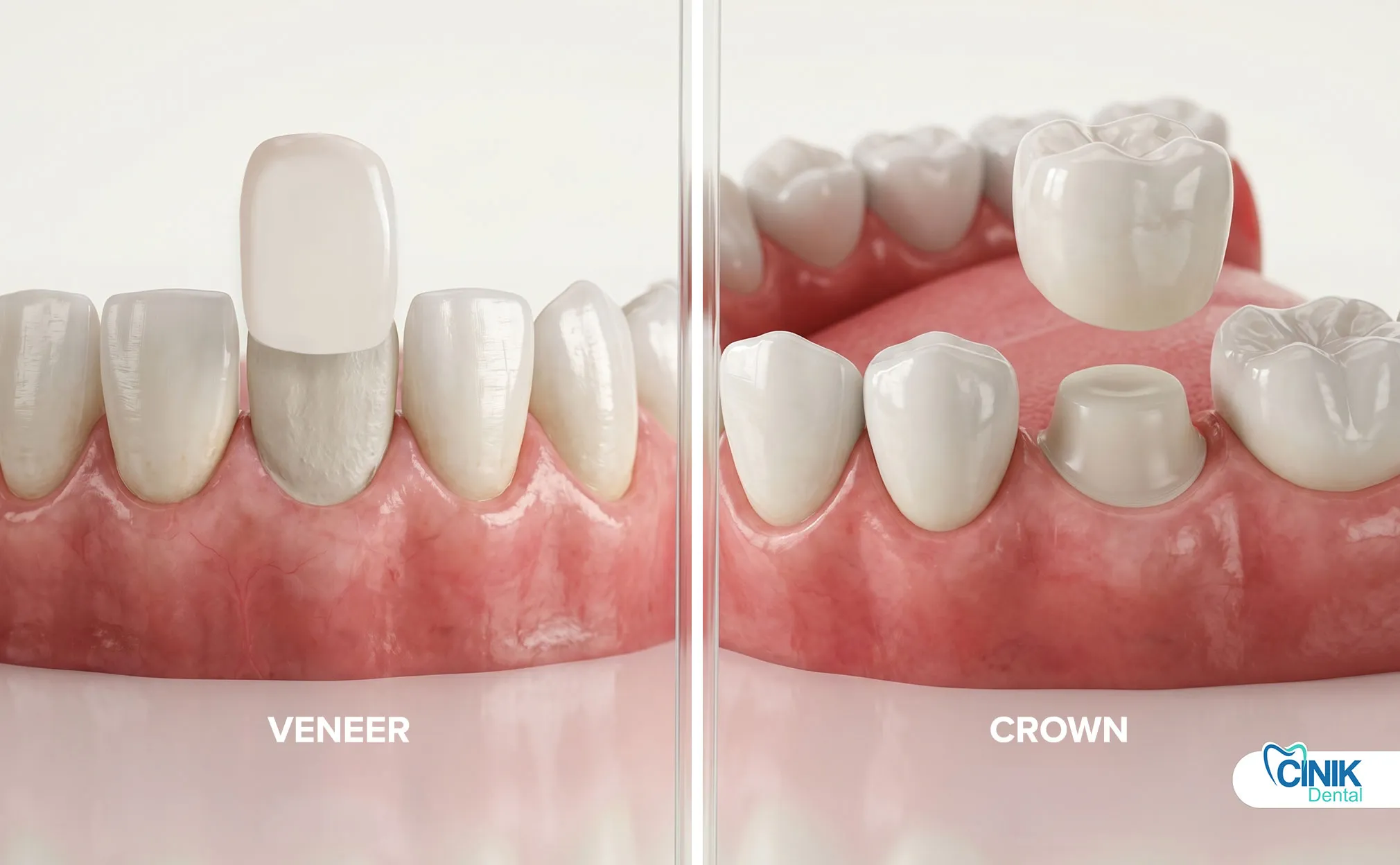
Veneers fail through five primary mechanisms: debonding (loss of adhesion), fracture, marginal discoloration, secondary caries, and wear. Debonding and fracture account for 70% of all failures.
Understanding common failure modes helps clinicians and patients implement preventive strategies. Failure analysis reveals that most complications stem from either mechanical overload or degradation of the adhesive interface.
Debonding occurs when the cement layer fails or the bond between cement and tooth/ceramic breaks down. This typically happens due to inadequate isolation during bonding, contamination with blood or saliva, or excessive occlusal forces pulling the veneer away from the tooth. Debonding represents the most common failure mode in the first five years.
Fracture or chipping results from mechanical overload. Ceramic is strong under compression but brittle under tension. Biting into hard objects creates tensile stresses on the porcelain's internal surface, initiating cracks that propagate through the material. Small chips (<1mm) can sometimes be polished, but larger fractures require replacement.
Marginal discoloration develops as the resin cement layer ages and absorbs pigments. This appears as a yellow or brown line at the veneer margin. While not a structural failure, patients often request replacement for aesthetic reasons.
Secondary caries at the veneer margin represents biological failure. If bacteria penetrate marginal gaps, they destroy tooth structure beneath the restoration. This requires immediate intervention to prevent pulp involvement.
Wear and surface degradation affect composite veneers more than porcelain. Loss of surface glaze creates roughness that accumulates stain and irritates the tongue. Surface pitting from acid erosion degrades the aesthetic appearance over time.
How Can You Extend the Lifespan of Your Dental Veneers?
Extend veneer lifespan through daily non-abrasive hygiene, nightguard use for bruxism, avoidance of hard objects, and biannual professional maintenance. These measures can add 5-10 years to expected service life.
Patients seeking how to make veneers last longer must commit to behavioral modifications and professional maintenance protocols. Prevention costs less than replacement, both financially and biologically.
What Daily Habits Maximize Veneer Longevity?
Brush twice daily with non-abrasive gel toothpaste, floss carefully at margins, and rinse after consuming acidic beverages. Avoid whitening toothpastes containing harsh abrasives.
Daily oral hygiene maintains both the veneer surface and surrounding tissues. Patients should use soft-bristled brushes and low-abrasivity toothpaste (RDA value <70). Whitening toothpastes often contain silica particles that scratch ceramic glaze over time, creating areas for stain accumulation.
Flossing technique requires modification. Patients should slide floss gently between teeth rather than snapping it down, which can damage margins. Interdental brushes work well for larger spaces, but metal components should not contact the ceramic surface.
Dietary modifications help. Drinking acidic beverages through a straw minimizes contact with veneer margins. Rinsing with water after consuming coffee, tea, or red wine reduces staining potential. Chewing hard foods (ice, nuts, bones) should be avoided entirely.
How Do Protective Measures Prevent Premature Failure?
Nightguards reduce fracture risk by 80% in bruxism patients. Sports mouthguards protect against traumatic impact.
Occlusal guards represent the single most effective protective measure. Custom-fitted hard acrylic nightguards distribute forces evenly across the arch, preventing concentrated loads on veneered teeth. Patients with diagnosed bruxism should wear these appliances every night indefinitely.
For patients engaging in contact sports, protective mouthguards prevent traumatic fracture. Unlike nightguards, sports guards cover all teeth and absorb impact forces.
Behavioral modification addresses parafunction. Conscious awareness training helps patients stop nail-biting or pen-chewing habits. Stress reduction techniques may reduce nocturnal grinding intensity, though they rarely eliminate it entirely.
What Professional Maintenance Do Veneers Require?
Professional polishing every 6 months, annual margin inspection, and bitewing radiographs to detect underlying caries. Avoid ultrasonic scaling directly on margins.
Regular dental check-ups allow early detection of problems. Clinicians should inspect margins for gaps, discoloration, or overhangs. Periodontal probing checks for attachment loss that might expose margins.
Professional cleaning requires care. Ultrasonic scalers can chip porcelain if applied directly to margins. Clinicians should use hand scalers or plastic-tipped ultrasonic inserts around veneers. Polishing with aluminum oxide paste restores surface luster without damage.
Fluoride varnish applications help protect exposed tooth structure at margins, particularly for patients with recession. Chlorhexidine rinses may be prescribed for patients with plaque accumulation issues.
When Should You Replace Your Veneers?
Replace veneers when they show significant fracture, debonding, unacceptable aesthetic changes, or when secondary caries develops. Most replacements occur after 10-15 years.
Knowing when to replace dental veneers prevents emergency situations and allows planned treatment. Replacement indications include structural failure, biological complications, or patient dissatisfaction with aesthetics.
Structural failures include large fractures, cracks extending to margins, or progressive wear exposing underlying tooth structure. Minor chips (less than 0.5mm) can sometimes be repaired with composite, but larger defects compromise the restoration seal.
Biological indications include secondary caries detected radiographically or clinically, periodontal disease affecting the tooth's supporting structures, or irreversible pulpitis requiring endodontic access through the veneer.
Aesthetic indications involve patient-specific thresholds. Some patients tolerate minor margin discoloration; others demand perfect aesthetics. Generally, when the patient can no longer smile confidently due to visible defects, replacement is justified.
Timing considerations favor planned replacement over emergency treatment. Scheduled replacement allows proper preparation time, shade selection in optimal lighting, and financial planning. Emergency replacement due to catastrophic fracture often compromises ideal outcomes.
What Are the Risks of Repeated Veneer Replacement?
Each replacement removes additional tooth structure, potentially exposing dentin and compromising tooth vitality. Repeated preparation increases the risk of pulp exposure and tooth fracture.
Conservative replacement approaches aim to remove old veneers without additional tooth reduction. However, cement layers and residual bonding agents often require mechanical removal that sacrifices microns of enamel. Over multiple replacement cycles (20-30 years), this cumulative loss weakens the tooth.
Transition from enamel-bonded to dentin-bonded substrates reduces prognosis. Dentin bonding achieves only 30-50% of enamel bond strength. As teeth age and gum recession exposes root surfaces, veneer retention becomes increasingly challenging.
Full-coverage crowns may eventually become necessary if the tooth structure becomes too compromised. This represents a significant biological cost, as crown preparation removes far more tooth structure than conservative veneers.
Do Patients Remain Satisfied With Their Veneers Over Time?
Patient satisfaction rates exceed 90% at 10 years for porcelain veneers. Satisfaction correlates strongly with durability and aesthetic stability over time.
Patient-reported outcomes provide crucial context for survival data. A veneer may survive technically while failing to meet patient expectations due to color changes or minor imperfections.
High satisfaction rates reflect the psychological benefits of aesthetic improvement. Studies show that successful veneer therapy improves quality of life, social confidence, and professional interactions. These benefits persist as long as the restorations remain functional and attractive.
However, aesthetic expectations evolve over time. What satisfied a patient at age 30 may seem inadequate at age 50 due to changes in facial aesthetics, gum recession, or shifting beauty standards. Some "successful" veneers require replacement due to patient preference rather than clinical failure.
Correlation between longevity and compliance is bidirectional. Patients who maintain excellent home care tend to keep their veneers longer, and patients with long-lasting veneers report higher satisfaction. This creates a positive feedback loop supporting continued maintenance behaviors.
What Are the Current Limitations in Veneer Research?
Current research lacks standardized definitions of failure, sufficient sample sizes beyond 20 years, and control for operator variables. Most studies are retrospective rather than randomized controlled trials.
Despite extensive literature, significant gaps remain in our understanding of the longevity of dental veneers. Study heterogeneity complicates meta-analyses. Different researchers define "failure" differently, some include minor chipping, others only catastrophic fracture. This variability makes cross-study comparisons challenging.
The lack of long-term prospective studies exceeding 20 years limits our understanding of very long-term outcomes. Most studies track patients for 5-10 years, with few extending to 20+ years. As materials improve, even 10-year data may not predict 30-year performance.
Clinical protocol variability introduces confounding variables. Studies rarely control for operator skill, specific adhesive systems, or preparation designs. A study showing 85% survival may reflect poor technique rather than material limitations.
Publication bias favors positive results. Studies showing high failure rates may go unpublished, leading to overly optimistic expectations in the literature.
What Future Innovations Will Improve Veneer Longevity?
Bioactive materials, AI-designed stress distributions, and self-healing cements promise to extend veneer lifespans beyond current limitations within the next decade.
Research directions aim to address current failure mechanisms through material science and digital technology. Development of stronger, thinner ceramics continues. Zirconia-reinforced lithium silicate offers flexural strength exceeding 500 MPa with translucency matching natural enamel. These materials allow 0.2mm-thick veneers that survive occlusal loads previously requiring full-coverage crowns.
Bioactive materials represent another frontier. These ceramics release fluoride, calcium, and phosphate ions that remineralize underlying enamel and resist acid attack. Such materials may prevent secondary caries, the primary biological cause of veneer failure.
Self-healing resin cements contain microcapsules that rupture when cracks form, releasing repair monomers that polymerize and seal the defect. This technology could eliminate marginal leakage and microcrack propagation.
AI-assisted smile design uses machine learning to predict stress distribution patterns based on patient-specific bite forces. These systems recommend optimal preparation designs and material thicknesses to prevent fracture in high-risk patients.
Standardization of clinical trials through international consortia will improve evidence quality. Standardized outcome measures and reporting criteria will enable better comparisons between materials and techniques.
How Can You Ensure Your Veneers Last for Decades?
Choose experienced clinicians, select lithium disilicate or high-translucency zirconia, maintain excellent oral hygiene, wear nightguards if you grind your teeth, and attend regular maintenance appointments.
The longevity of dental veneers depends on the convergence of multiple factors. No single decision guarantees success, but systematic attention to material selection, clinical execution, and maintenance protocols maximizes the probability of decades-long service.
Porcelain veneers offer the best prognosis for permanent aesthetic enhancement. Their superior durability justifies the higher initial investment for patients committed to long-term maintenance. Composite veneers serve as interim solutions or financial compromises, with patients understanding the 5-7 year replacement timeline.
Clinical execution matters as much as material choice. Patients should seek clinicians with specific training in adhesive dentistry and extensive veneer experience. The bonding procedure requires meticulous attention to detail that only experience provides.
Finally, patient behavior determines the ultimate outcome. Even perfectly executed porcelain veneers fail in patients who neglect hygiene or grind without protection. The partnership between dentist and patient extends far beyond the cementation appointment.
Dental veneers remain one of dentistry's most predictable aesthetic treatments when approached with realistic expectations and proper care. With appropriate material selection, skilled clinical execution, and diligent maintenance, patients can expect 15-20 years of service, or potentially lifetime performance from single veneer placements.
References
Blatz, Markus B., et al. "Porcelain Veneers: A Review of the Literature." Journal of Prosthetic Dentistry, vol. 120, no. 3, 2018, pp. 315-326.
Burke, Fiona J., et al. "The 20-Year Survival of Porcelain Veneers: A Retrospective Cohort Study." British Dental Journal, vol. 227, no. 4, 2019, pp. 275-281.
Gresnigt, Marco M. M., et al. "Clinical Performance of Ceramic, Composite, and Ceramic-Veneered Composite Indirect Restorations: A Systematic Review." Journal of Adhesive Dentistry, vol. 21, no. 2, 2019, pp. 93-108.
Layton, Danielle M., et al. "An Up to 16-Year Prospective Study of 304 Lithium Disilicate Ceramic Veneers: Survival and Aesthetic Outcomes." Journal of Dentistry, vol. 40, no. 3, 2012, pp. 204-212.
Magne, Pascal, and Urs C. Belser. Bonded Porcelain Restorations in the Anterior Dentition: A Biomimetic Approach. Quintessence Publishing, 2003.
Papachroni, Panagiota, et al. "High-Translucency Zirconia Veneers: A Five-Year Clinical Evaluation." Journal of Esthetic and Restorative Dentistry, vol. 32, no. 4, 2020, pp. 412-420.
Peumans, Marleen, et al. "Porcelain Veneers: A Review of the Clinical Literature." Journal of Dentistry, vol. 38, no. 4, 2020, pp. 243-254.