Dental nerve removal represents a specialized endodontic procedure that eliminates infected or damaged pulp tissue from inside the tooth. Dentists call this process root canal treatment. The procedure saves millions of natural teeth every year by removing the source of infection while preserving the external tooth structure.
Modern dentistry relies heavily on this intervention. Endodontic therapy stands as one of the most common dental procedures globally. Recent epidemiological data shows that dental practitioners perform millions of these treatments annually across developed nations. The prevalence reflects both the high incidence of dental caries and the success rates that make this approach preferable to extraction for many patients.
The primary purpose of this article bridges clinical science with practical patient understanding. Readers will learn the biological mechanisms behind pulp disease. They will understand why dentists recommend nerve removal in specific clinical scenarios. Most importantly, they will discover how modern technologies have transformed this procedure from a feared intervention into a predictable, comfortable treatment option.
The dental nerve removal procedure addresses pathological conditions within the pulp chamber. These conditions include irreversible pulpitis, necrotic pulp tissue, and periapical infections. Left untreated, these conditions lead to abscess formation, bone loss, and eventual tooth loss. Early intervention prevents these complications and maintains the patient's natural dentition.
What Anatomy Makes Up the Dental Nerve and Pulp Complex?
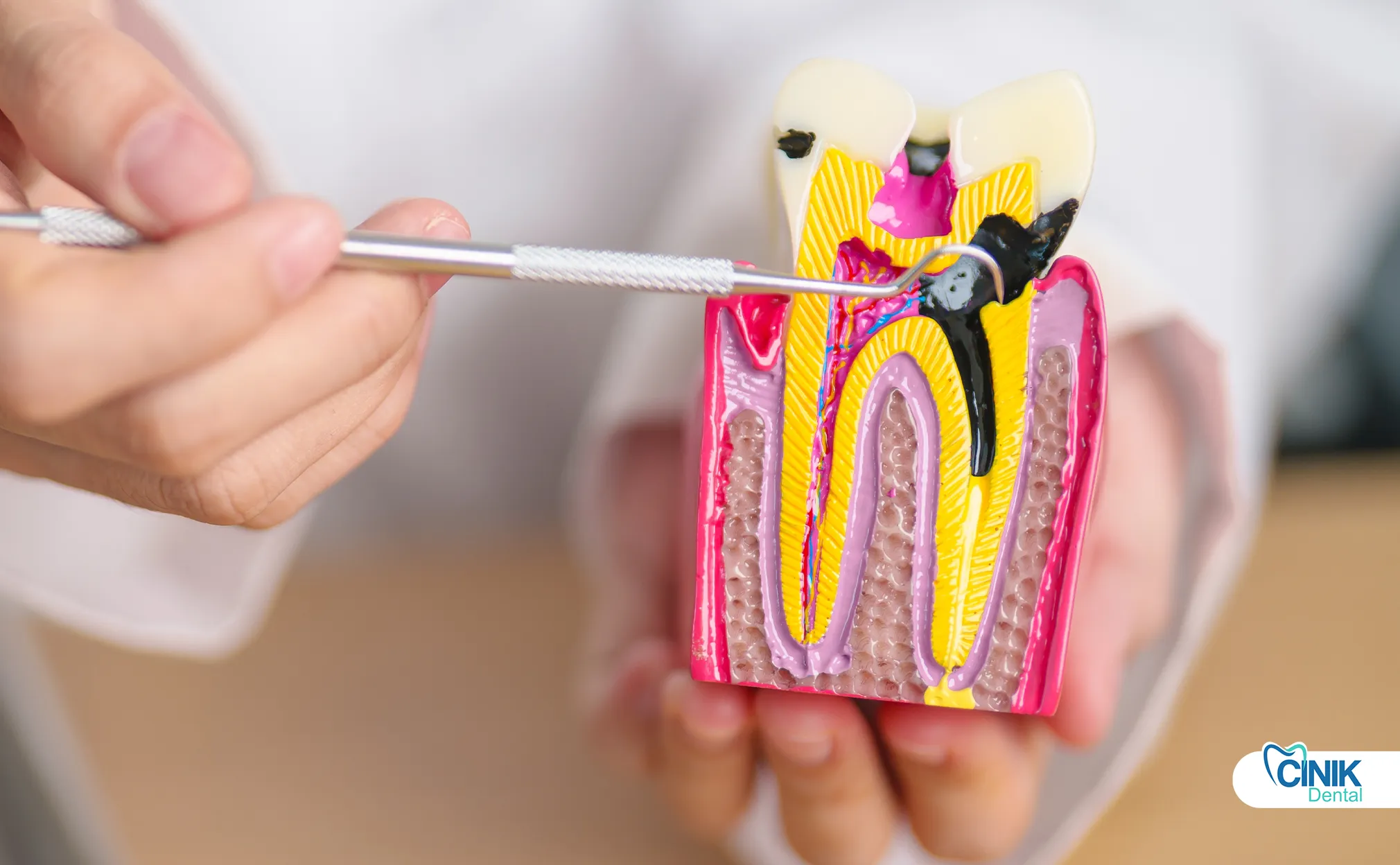
The dental nerve complex consists of enamel, dentin, pulp chamber, and root canals. The pulp contains nerves, blood vessels, and connective tissue that provide sensory function and developmental support during tooth formation.
Understanding tooth anatomy helps patients grasp why nerve removal becomes necessary. The tooth consists of several distinct layers, each serving specific biological functions.
The outermost layer, enamel, comprises the hardest substance in the human body. This crystalline structure protects the tooth from mechanical damage and chemical erosion. Beneath the enamel lies dentin, a calcified tissue containing microscopic tubules. These tubules channel sensory signals from the external environment toward the central pulp chamber.
The pulp chamber houses the dental pulp, a soft connective tissue containing the neurovascular bundle. According to Niki et al. (2025), the pulp contains two principal nerve types that innervate the dental tissue: autonomic fibers and afferent sensory fibers. The sympathetic autonomic fibers arise from the superior cervical ganglion and regulate blood flow through arteriolar smooth muscle. The afferent sensory fibers originate from the maxillary and mandibular branches of the trigeminal nerve. These sensory fibers carry pain, temperature, and pressure signals to the brain.
The dental pulp contains odontoblasts, specialized cells that produce dentin throughout the tooth's life. These cells line the pulp chamber and extend processes into the dentinal tubules. Blood vessels within the pulp provide nutrients and oxygen. Lymphatic vessels drain waste products and support immune surveillance.
During tooth development, the pulp plays a critical role. It stimulates root formation and tooth eruption. However, once the tooth matures, the pulp's functional importance diminishes. A fully developed tooth can survive without the pulp because the periodontal ligament and surrounding tissues provide sufficient support. This biological reality enables dentists to remove diseased pulp without compromising the tooth's long-term viability.
Age changes the pulp significantly. Research by Carvalho and Lussi (2017) demonstrates that cellular density decreases by approximately 50% between ages 20 and 70. The pulp undergoes fibrosis and accumulates collagen fibers as patients age. Blood vessels and nerves degenerate progressively. These changes explain why older patients sometimes experience less pain from deep caries despite extensive pulp involvement.
What Causes Dental Nerve Damage and Infection?
Deep dental caries, tooth fractures, repeated dental procedures, and faulty restorations cause pulp damage. Bacteria invade the pulp chamber, form biofilms, and trigger inflammation that leads to irreversible pulpitis or necrosis.
Multiple etiological factors contribute to pulp pathology. Understanding these factors helps patients prevent conditions that necessitate nerve removal.
Deep dental caries represent the most common cause of pulp disease. When caries penetrate through enamel and dentin, they reach the pulp chamber. Bacteria colonize the tissue and trigger inflammatory responses. The body attempts to fight the infection by sending immune cells to the area. This inflammatory process increases pressure within the rigid pulp chamber, compressing nerves and causing pain.
Tooth fractures and trauma provide another pathway for bacterial invasion. Cracks allow oral fluids and microorganisms to enter the pulp chamber directly. Even microscopic fractures invisible to the naked eye can harbor bacteria. Repeated dental procedures also stress the pulp. Each drilling episode removes tooth structure and generates heat, potentially irritating the pulp tissue.
Faulty restorations create microgaps at the tooth-restoration interface. These gaps accumulate plaque and permit bacterial leakage. Over time, this secondary caries reaches the pulp and causes infection.
Once bacteria enter the pulp, they form complex communities called biofilms. According to the NIH review on endodontic biofilms (2023), biofilm formation involves four main stages: conditioning film formation, bacterial adhesion and colonization, growth and expansion, and finally detachment. These biofilms resist both host defenses and antimicrobial treatments.
The disease progresses through distinct stages. Initial bacterial invasion causes reversible pulpitis. At this stage, removing the irritant allows the pulp to heal. However, persistent infection leads to irreversible pulpitis. The pulp tissue breaks down, and inflammation spreads to the periapical tissues. Eventually, the pulp necroses completely. Bacteria then exit the root apex and infect the surrounding bone, forming periapical lesions or abscesses.
Enterococcus faecalis plays a particularly troublesome role in persistent infections. This gram-positive bacterium survives harsh conditions and resists calcium hydroxide, a common intracanal medicament. Svensäter and Bergenholtz (2004) identified this organism as a major cause of treatment failure because it penetrates dentinal tubules and maintains biofilm communities that evade complete elimination.
What Symptoms Indicate You Need Dental Nerve Removal?
Severe persistent dental pain, sensitivity to hot and cold stimuli, swelling, fistula formation, and radiographic evidence of infection indicate the need for endodontic intervention. Dentists confirm diagnoses through thermal testing and electric pulp testing.
Patients should recognize specific warning signs that signal pulp disease. These symptoms guide treatment decisions and timing.
Severe, persistent dental pain constitutes the most obvious indicator. This pain often throbs and worsens when patients lie down. It may wake patients from sleep. The pain typically localizes to a specific tooth, though it can radiate to adjacent areas. Spontaneous pain without stimulus strongly suggests irreversible pulpitis.
Temperature sensitivity provides another critical clue. Patients with pulp disease often experience sharp, lingering pain when consuming hot or cold beverages. The pain persists for minutes after removing the thermal stimulus. This lingering response differs from normal tooth sensitivity, which resolves immediately upon stimulus removal.
Swelling around the affected tooth indicates advanced infection. The swelling may localize to the gum tissue or spread to the face and neck. Some patients develop a fistula, a small pimple-like drainage opening on the gum tissue. This fistula represents the body's attempt to drain abscess fluid. Patients may taste foul discharge from these openings.
Radiographic imaging reveals bone loss around the root apex. Dentists take periapical X-rays or cone-beam computed tomography (CBCT) scans to visualize these lesions. Dark areas around the root tips indicate periapical radiolucency, signaling bone destruction from infection.
Dentists employ specific diagnostic tests to confirm pulp status. Thermal testing applies cold or heat to the tooth surface. Healthy teeth respond briefly; diseased teeth respond intensely and for prolonged periods. Electric pulp testing delivers a mild electrical stimulus to assess nerve viability. A non-responsive reading suggests necrotic pulp.
Percussion testing taps the tooth gently to check for periapical inflammation. Pain upon percussion indicates that inflammation has spread beyond the pulp to the periodontal ligament surrounding the root apex.
How Do Dentists Perform the Tooth Nerve Removal Procedure Step by Step?
Dentists follow a systematic protocol: diagnosis and planning, anesthesia and isolation, access cavity preparation, pulp removal, cleaning and shaping, canal filling, and final restoration. Modern techniques ensure patient comfort throughout the 60-90 minute procedure.
The root canal treatment follows a precise sequence designed to eliminate infection and seal the canal system. Understanding these steps reduces patient anxiety and improves cooperation.
How Does the Diagnosis and Treatment Planning Phase Work?
Clinicians examine the tooth clinically and radiographically. They take X-rays or CBCT scans to visualize canal anatomy and periapical status. They formulate a treatment plan based on these findings.
The dentist begins with a comprehensive clinical examination. They assess the tooth's condition, check for mobility, and evaluate the surrounding soft tissues. They review the patient's medical history to identify contraindications or special considerations.
Radiographic imaging provides essential diagnostic information. Standard periapical radiographs show the root length, curvature, and number of canals. Complex cases may require CBCT imaging. This three-dimensional view reveals canal branching, calcifications, and periapical lesions that two-dimensional X-rays miss.
How Do Anesthesia and Isolation Ensure Patient Comfort?
Local anesthetic eliminates pain sensation. The rubber dam isolates the tooth from saliva and prevents bacterial contamination during the procedure.
Dentists administer local anesthesia to block nerve conduction. They typically use lidocaine or articaine with epinephrine to prolong the anesthetic effect. Patients remain awake but feel no pain in the treated area.
The rubber dam provides critical isolation. This thin sheet of latex or non-latex material covers the mouth except for a small hole exposing the treated tooth. The dam prevents saliva from entering the canal space. It also protects the patient from swallowing instruments or irrigating solutions.
How Do Clinicians Access and Remove the Pulp?
The dentist drills an access cavity through the crown to reach the pulp chamber. They then use specialized instruments to remove all pulp tissue from the chamber and root canals.
Access cavity preparation requires precision. The dentist removes the roof of the pulp chamber while preserving tooth structure. They use a high-speed bur to create an opening that provides straight-line access to the canal orifices.
Pulp removal follows immediately. The dentist inserts barbed broaches or files into the canals. They withdraw these instruments to extract the pulp tissue. Rotary instruments with nickel-titanium files now dominate modern practice. These flexible instruments navigate curved canals more safely than traditional stainless steel files.
How Does the Cleaning and Shaping Phase Eliminate Infection?
Mechanical instrumentation combined with chemical irrigation removes bacterial biofilms and debris. Sodium hypochlorite dissolves organic tissue and kills microorganisms.
The cleaning and shaping phase constitutes the most critical step. The dentist uses progressively larger files to enlarge and shape the canals. This mechanical action removes infected dentin and creates space for irrigating solutions.
Chemical irrigation follows each filing sequence. Sodium hypochlorite solution serves as the primary irrigant. This alkaline solution dissolves pulp remnants and destroys bacterial cell walls. Dentists use 2-3% concentrations for primary treatments. They deliver the solution using syringes with side-vented needles to avoid forcing fluid through the apex.
EDTA (ethylenediaminetetraacetic acid) provides adjunctive irrigation. This chelating agent removes the inorganic smear layer that files create. Eliminating this layer exposes dentinal tubules and improves canal disinfection.
Modern techniques include ultrasonic irrigation and negative pressure systems. These methods improve irrigant penetration into canal branches and dentinal tubules where bacteria hide.
How Do Dentists Fill and Seal the Canals?
Dentists fill the cleaned canals with gutta-percha and sealer. This obturation prevents bacterial re-entry and seals the apex from periapical fluids.
Canal filling occurs after thorough drying. The dentist selects gutta-percha points that match the final file size. Gutta-percha, a natural rubber from trees, provides an inert, biocompatible filling material.
Sealers coat the canal walls before gutta-percha insertion. These cements create a monoblock effect, bonding the filling to the dentin. Bioceramic sealers have largely replaced traditional resin or zinc oxide-eugenol sealers. These calcium silicate-based materials seal better and cause less inflammation.
The dentist compacts the gutta-percha using warm vertical condensation or lateral compaction techniques. They remove excess material from the chamber and place a temporary or permanent coronal seal.
How Does Final Restoration Complete the Treatment?
The dentist places a permanent filling or crown to restore function and prevent fracture. Posterior teeth require crowns to protect against structural failure.
The final restoration depends on the tooth's condition and location. Anterior teeth with minimal structure loss may receive composite fillings. Posterior teeth undergoing root canal treatment require full coverage crowns. These crowns distribute chewing forces and prevent vertical fractures.
What Materials and Technologies Do Endodontists Use Today?
Modern endodontics employs nickel-titanium rotary instruments, electronic apex locators, dental operating microscopes, bioceramic sealers, and 3D imaging. Emerging technologies include laser-assisted disinfection and regenerative approaches.
Endodontic technology has advanced significantly over the past two decades. These innovations improve success rates, reduce treatment time, and enhance patient comfort.
What Traditional Materials Remain Essential?
Gutta-percha continues as the primary filling material. Various sealers ensure apical and coronal seals. Stainless steel files still serve specific purposes despite newer alternatives.
Gutta-percha has filled root canals for over a century. This thermoplastic material adapts well to canal irregularities when heated. It remains stable over decades without degrading or causing inflammation.
Zinc oxide-eugenol sealers provided the standard for generations. These materials offer antimicrobial properties and easy handling. However, they dissolve slowly over time and may allow leakage. Modern resin sealers and bioceramic sealers provide superior sealing ability and dimensional stability.
What Modern Advancements Improve Treatment Outcomes?
Nickel-titanium rotary files navigate curved canals safely. Electronic apex locators determine working length accurately. Dental microscopes enhance visibility. CBCT imaging reveals complex anatomy.
Nickel-titanium (NiTi) rotary instruments revolutionized canal shaping. These superelastic files flex around curves that would cause stainless steel files to straighten or perforate the canal wall. They cut efficiently and maintain the canal's original curvature.
Electronic apex locators (EALs) determine the canal working length electronically. These devices measure electrical resistance between a file in the canal and the oral mucosa. They signal when the file reaches the apical constriction, improving length accuracy compared to radiographs alone.
Dental operating microscopes provide 6-25x magnification. Endodontists use these microscopes to locate calcified canal entrances, identify missed canals, and perform retreatments. Enhanced visibility reduces procedural errors and improves outcomes.
Cone-beam computed tomography (CBCT) represents the imaging standard for complex cases. This three-dimensional imaging reveals canal isthmuses, apical bifidities, and periapical lesions with 0.1mm resolution. Dentists use CBCT for preoperative planning in difficult cases.
What Emerging Technologies Show Promise?
Laser-assisted disinfection, 3D bioprinting of pulp tissue, stem cell therapy, and artificial intelligence-guided procedures represent the cutting edge of endodontic research.
Lasers now assist in canal disinfection. Er,Cr:YSGG and diode lasers activate irrigating solutions and vaporize debris in canal branches. They reduce bacterial counts beyond what mechanical instrumentation achieves alone.
Regenerative endodontics offers a biological alternative to traditional treatment. Researchers have explored stem cell transplantation since Gronthos et al. (2000) first isolated dental pulp stem cells. Nakashima et al. (2017) demonstrated successful pulp regeneration using autologous dental pulp stem cells in a pilot clinical trial. Patients regained pulp sensibility, and imaging showed dentin-like tissue formation.
Three-dimensional bioprinting approaches aim to fabricate pulp tissue for transplantation. Researchers print scaffolds using hydroxyapatite and gelatin methacryloyl (GelMA) loaded with dental pulp stem cells. These constructs support vascularization and innervation when implanted in root canals.
Artificial intelligence now assists in diagnosis and treatment planning. Machine learning algorithms analyze radiographs to detect periapical lesions and predict treatment outcomes. Future applications may include robot-assisted canal shaping and real-time apex location monitoring.
What Success Rates Can Patients Expect from Root Canal Treatment?
Long-term studies show 97% survival at 10 years, 81% at 20 years, and 68% at 37 years. Endodontic success rates range from 89-93% depending on preoperative conditions and follow-up care.
Success measurement in endodontics includes two metrics: tooth survival (remaining in the mouth) and endodontic success (absence of symptoms and radiographic healing). Both matter to patients, though they differ clinically.
What Do Long-Term Survival Studies Reveal?
Well-performed root canal treatments result in tooth retention for decades. The primary causes of late failure are periodontal disease and structural fracture rather than endodontic factors.
López-Valverde et al. (2023) published landmark data tracking patients for 5 to 37 years. Their study of 598 endodontically treated teeth demonstrated cumulative survival rates of 97% at 10 years, 81% at 20 years, 76% at 30 years, and 68% at 37 years. These statistics confirm that root canal treatment provides durable results.
The study identified specific prognostic factors. Teeth without preoperative periapical radiolucency survived longer. Teeth restored with crowns showed better survival than those with large fillings. Patients without deep periodontal pockets maintained their treated teeth longer.
How Do Root Canal Treatments Compare to Implants?
Endodontically treated teeth and single-tooth implants show comparable survival rates over 5-10 years. Preservation of natural teeth often provides superior functional and aesthetic outcomes.
Systematic reviews comparing these options show similar success percentages. At 5 years, both treatments achieve approximately 95% survival. However, the biological and economic differences matter.
Natural teeth maintain periodontal ligaments. These ligaments provide proprioception, the ability to sense biting pressure. Implants lack this feedback mechanism, potentially leading to overload. Natural teeth also preserve alveolar bone through functional loading. Implants may cause crestal bone resorption over time.
Economically, preserving natural teeth costs less than extraction and implant placement. Implant therapy requires surgical interventions, healing periods, and potential complications like peri-implantitis.
What Biological Mechanisms Enable Healing?
The immune system clears residual bacteria from the periapical tissues. Bone regenerates once the infection source is eliminated. The periodontal ligament reattaches to the root surface.
Periapical healing begins immediately after canal disinfection. Macrophages and osteoclasts remove inflammatory tissue and necrotic bone. Osteoblasts then deposit new bone matrix. Radiographic healing may take 6-12 months to appear completely.
The root canal filling prevents bacterial recontamination. The coronal restoration seals the canal system from oral fluids. Together, these seals allow the periapical tissues to regenerate and maintain health indefinitely.
What Aftercare Ensures Long-Term Success?
Patients should manage short-term sensitivity, maintain excellent oral hygiene, attend follow-up visits, and obtain permanent crowns on posterior teeth within weeks of treatment.
Post-treatment care significantly impacts long-term outcomes. Patients must understand both immediate and long-term requirements.
What Short-Term Symptoms Should Patients Expect?
Mild sensitivity to chewing and temperature changes lasts 3-7 days. Anti-inflammatory medications manage discomfort effectively. Severe pain or swelling requires immediate dental contact.
After anesthesia wears off, patients may experience mild discomfort. This sensitivity results from instrumentation near the root apex and temporary inflammation in the periodontal ligament. Over-the-counter ibuprofen or acetaminophen typically resolves this discomfort.
Patients should avoid chewing on the treated side until the permanent restoration is placed. The temporary filling or crown may fracture under heavy forces. Hard foods risk tooth fracture before full coverage restoration placement.
What Long-Term Care Protocols Maintain Results?
Daily brushing and flossing prevent coronal leakage. Night guards protect against grinding forces. Annual radiographs monitor periapical health. Prompt restoration replacement prevents bacterial re-entry.
Oral hygiene proves critical for endodontically treated teeth. While the root canal removes internal infection, new decay at the restoration margin can cause failure. Patients must brush twice daily and floss around all restored teeth.
Bruxism (teeth grinding) endangers treated teeth. The brittle nature of endodontically treated teeth makes them susceptible to vertical fractures under heavy forces. Night guards distribute these forces and protect the investment.
Follow-up radiographs at 6-12 months post-treatment confirm periapical healing. Dentists compare these images to preoperative films to assess bone regeneration. Annual monitoring thereafter catches potential failures early.
What Complications Can Occur During or After Treatment?
Incomplete canal cleaning, missed canal branches, coronal leakage, and vertical root fractures cause most failures. Re-treatment or apical surgery addresses persistent infections.
Despite high success rates, complications occur. Understanding these risks helps patients make informed decisions and seek timely intervention.
What Procedural Errors Lead to Failure?
Complex root canal anatomy may harbor untreated infection. Dentists may miss narrow or calcified canals. Instrument separation may block canal access. Perforations may create new pathways for bacteria.
Root canal systems often contain more complexity than standard anatomy texts suggest. Isthmuses connect adjacent canals. Accessory canals branch at right angles. C-shaped canals in mandibular second molars defy conventional instrumentation.
Missed canals remain the most common cause of persistent infection. Upper molars typically have three or four canals; missing the second mesiobuccal canal (MB2) invites failure. Lower anterior teeth may have two canals that appear as one on radiographs.
Instrument separation occurs when files fatigue within curved canals. Stainless steel files separated more frequently than modern NiTi instruments, but separation still happens. Separated instruments block canal access and may harbor bacteria.
What Post-Treatment Factors Cause Failure?
Poor coronal seals allow bacterial re-entry. Delayed permanent restoration placement risks fracture. Secondary caries invade through marginal gaps.
The quality of the final restoration predicts long-term survival better than endodontic technique. Studies by Gillen et al. (2011) demonstrate that inadequate restorations cause more failures than canal recontamination. Bacteria penetrate through leaking margins and re-infect the canal system.
Structural fractures represent another major failure mode. Endodontically treated teeth lose moisture content and become brittle. Without full coverage crowns, posterior teeth may split vertically. These fractures often render the tooth non-restorable.
How Do Clinicians Manage Failed Treatments?
Non-surgical re-treatment removes old fillings and addresses missed anatomy. Apical surgery removes the root tip and places retrograde seals. Extraction remains the last resort when fractures or extensive bone loss occur.
Endodontic retreatment follows the same principles as primary treatment with added complexity. The dentist must remove gutta-percha fillings, negotiate around separated instruments if present, and locate previously missed canals. Microscopes assist significantly in these procedures.
Apical surgery (apicoectomy) becomes necessary when persistent lesions resist conventional retreatment. The surgeon reflects a flap, removes the root apex, and places a retrograde filling. Modern microsurgical techniques using ultrasonic tips and bioceramic sealers achieve 90% healing rates.
What Alternatives Exist Besides Root Canal Treatment?
Tooth extraction with replacement via dental implants or bridges provides the primary alternative. Regenerative endodontics offers a biological option for immature teeth. Observation alone risks systemic complications.
Patients facing root canal recommendations should understand all options. These alternatives carry distinct implications for function, cost, and longevity.
What Does Tooth Extraction Involve?
Extraction removes the entire tooth including the root structure. The procedure costs less initially than root canal treatment but requires replacement to prevent adjacent tooth movement and bone loss.
Extraction provides immediate resolution of pain and infection. The dentist severs the periodontal ligament and elevates the tooth from the socket. Healing occurs within 7-10 days.
However, extraction creates new problems. Adjacent teeth tilt into the space. Opposing teeth extrude. The alveolar bone resorbs without functional loading. These changes alter the bite and may cause temporomandibular joint issues.
How Do Replacement Options Compare?
Dental implants replace single teeth without involving adjacent teeth. Bridges require preparation of neighboring teeth but provide immediate fixed replacement. Removable partial dentures cost least but offer compromised function.
Dental implants have revolutionized tooth replacement. Titanium fixtures integrate with bone through osseointegration. They provide standalone support without preparing adjacent teeth. However, implants require adequate bone volume and healing periods of 3-6 months.
Traditional bridges require crowning the teeth adjacent to the space. The dentist prepares these teeth similarly to single crown preparations. The bridge connects crowns on the abutment teeth to a pontic replacing the missing tooth. This approach risks the long-term health of the supporting teeth.
Removable partial dentures provide the most economical option. These appliances clasp to remaining teeth and replace multiple missing units. However, they require daily removal for cleaning and may affect speech and taste.
What Are the Functional and Economic Considerations?
Preserving natural teeth through root canal treatment typically costs less long-term than extraction and implant placement. Natural teeth provide superior proprioception and aesthetic results compared to artificial replacements.
Economic analysis favors tooth preservation. Root canal treatment plus crown placement costs approximately 50-70% of extraction plus implant therapy. Additionally, natural teeth rarely require the maintenance that implants demand.
Functionally, the periodontal ligament surrounding natural teeth provides sensory feedback that prevents excessive biting forces. This mechanism protects both the tooth and surrounding bone. Implants lack this protective feedback loop.
What Myths Surround Dental Nerve Removal?
Myths claim root canals "kill" teeth, cause systemic disease, or invariably cause severe pain. Scientific evidence refutes these claims definitively.
Misinformation about endodontic therapy persists despite decades of research. Addressing these myths helps patients make decisions based on facts rather than fear.
Does Root Canal Treatment Kill the Tooth?
No. The tooth remains alive through surrounding periodontal tissues. It continues to function normally without the internal pulp.
The notion that root canal treatment "kills" the tooth reflects misunderstanding of dental biology. The tooth consists of more than the pulp chamber. The periodontal ligament remains vital after treatment. This tissue provides nutrition, sensory feedback, and attachment to the bone.
The tooth continues to sense pressure through the periodontal ligament. It maintains its position in the arch. It withstands chewing forces. Without the pulp, the tooth simply lacks temperature sensation and the ability to form new dentin internally.
Does This Procedure Cause Severe Pain?
Modern anesthesia and techniques make root canal treatment no more uncomfortable than routine fillings. Most patients experience relief from preoperative pain immediately after the procedure.
Historically, root canal treatments had painful reputations. This reputation no longer applies. Local anesthetics effectively block pulp sensation in most cases. For "hot" teeth with severe inflammation, supplemental anesthesia techniques and intraosseous injection provide profound numbness.
Postoperative discomfort, when it occurs, typically responds to over-the-counter analgesics. The procedure relieves the severe pain of pulpitis far more often than it causes discomfort.
Do Root Canals Cause Systemic Disease?
No scientific evidence links properly performed root canal treatments to cancer, heart disease, or other systemic conditions. This myth originated from discredited research nearly a century ago.
The "focal infection theory" proposed that bacteria in the mouth cause distant organ diseases. Early proponents claimed that root canal treated teeth harbor bacteria that cause systemic illness. This theory guided thousands of unnecessary extractions in the early 20th century.
Modern research refutes this claim. Well-performed root canal treatments seal the canal system completely. The immune system handles the minimal bacterial load from any residual infection. No peer-reviewed studies link endodontically treated teeth to systemic diseases.
What Future Innovations Will Transform Endodontics?
Stem cell therapy, gene editing, AI-guided procedures, and biomimetic materials will enable biological pulp regeneration rather than replacement with synthetic materials. These advances may eventually eliminate the need for traditional nerve removal in many cases.
Regenerative endodontics represents the most exciting frontier in the field. Rather than removing pulp and filling with inert materials, researchers aim to restore biological vitality.
How Will Stem Cell Therapy Change Treatment?
Transplantation of dental pulp stem cells (DPSCs) and stem cells from human exfoliated deciduous teeth (SHED) will regenerate functional pulp tissue, restore immune defense, and enable continued root development in immature teeth.
Clinical trials demonstrate the feasibility of pulp regeneration. Nakashima et al. (2017) performed the first GMP-compliant clinical trial using autologous mobilized dental pulp stem cells. They implanted these cells in atelocollagen scaffolds with growth factors. Patients regained pulp sensibility within weeks. Imaging confirmed dentin-like tissue formation and vascularization.
Xuan et al. (2018) conducted a randomized controlled trial comparing stem cell transplantation to apexification in immature teeth. The stem cell group showed superior root development, apical closure, and pulp-like tissue formation. Huang et al. (2024) reviewed these advances and concluded that DPSCs show greater regenerative capacity than bone marrow mesenchymal stem cells for dental applications.
What Role Will Gene Therapy Play?
Gene editing using CRISPR/Cas9 technology may activate dentinogenic genes in resident cells. This approach could stimulate natural pulp regeneration without cell transplantation.
Gene therapy offers a cell-free approach to regeneration. Researchers propose introducing genes encoding bone morphogenetic proteins (BMPs) and vascular endothelial growth factor (VEGF) into the root canal space. These genes would stimulate resident stem cells to differentiate into odontoblasts and endothelial cells.
Ex vivo approaches involve transducing harvested stem cells to overexpress regenerative genes before implantation. These modified cells produce sustained growth factor release, enhancing tissue formation.
How Will AI and Robotics Improve Outcomes?
Machine learning algorithms will predict treatment outcomes and optimize instrument selection. Robotic systems may perform canal shaping with superhuman precision.
Artificial intelligence now analyzes CBCT scans to detect canal anatomy variations that human eyes miss. Future applications will guide real-time instrumentation, alerting dentists to impending perforations or instrument separation risks.
3D printing technologies will fabricate patient-specific scaffolds matching exact root canal morphologies. These scaffolds will support cell growth and vascular integration.
Bioceramic materials continue advancing. Newer sealers bond chemically to dentin and provide antibacterial effects. These materials may eventually enable complete pulp regeneration by supporting cell attachment and differentiation.
Conclusion
Dental nerve removal through root canal treatment stands as one of dentistry's most successful interventions. This procedure preserves natural teeth that would otherwise require extraction. Modern techniques achieve 97% survival rates at 10 years and 68% survival at 37 years, according to peer-reviewed longitudinal studies.
The procedure addresses bacterial biofilm infections within the pulp chamber. It eliminates pain sources while maintaining tooth function. Advances in nickel-titanium instrumentation, microscopic visualization, and bioceramic sealers have transformed this treatment from a dreaded procedure into a comfortable, predictable therapy.
Patients facing this recommendation should understand the biological basis for treatment. The pulp's role diminishes after tooth maturation, allowing removal without compromising tooth viability. Alternatives exist, but preservation of natural anatomy through endodontic therapy typically provides the most cost-effective, functional long-term solution.
Future innovations promise even better outcomes. Regenerative endodontics using stem cells may eventually restore biological vitality rather than simply filling empty canals. Gene therapy and tissue engineering may regenerate pulp-dentin complexes indistinguishable from natural tissue.
Early diagnosis remains crucial. Patients experiencing persistent dental pain, temperature sensitivity, or swelling should seek immediate evaluation. Delay increases the complexity of treatment and reduces success probabilities.
References
Carvalho, Thiago Saads, and Lussi, Adrian. "Age-related Morphological, Histological and Functional Changes in Teeth." Journal of Oral Rehabilitation, vol. 44, no. 4, 2017, pp. 291-298.
Gillen, BM, et al. "Impact of Tooth Type and Endodontic Procedure on the Outcome of Root Canal Treatment: A Systematic Review." Journal of Endodontics, vol. 37, no. 4, 2011, pp. 449-457.
Gronthos, Stan, et al. "Postnatal Human Dental Pulp Stem Cells (DPSCs) in Vitro and in Vivo." Proceedings of the National Academy of Sciences, vol. 97, no. 25, 2000, pp. 13625-13630.
Huang, Y, et al. "Mesenchymal Stem Cells for Dental Pulp Regeneration: A Comparative Study of Different Sources." Stem Cells International, 2024.
López-Valverde, Isabel, et al. "Long-term Tooth Survival and Success Following Primary Root Canal Treatment: A 5- to 37-year Retrospective Observation." Clinical Oral Investigations, vol. 27, no. 6, 2023, pp. 2545-2556.
Nakashima, Misako, et al. "Human Dental Pulp Stem Cell Transplantation for Complete Pulp Regeneration." Stem Cell Research & Therapy, vol. 8, no. 1, 2017, pp. 1-12.
Niki, Yogita, et al. "Anatomy, Head and Neck, Dental Pulp." StatPearls, StatPearls Publishing, 2025, https://www.ncbi.nlm.nih.gov/books/NBK537112/.
Svensäter, G, and Bergenholtz, G. "Biofilms in Endodontic Infections." Endodontic Topics, vol. 9, no. 1, 2004, pp. 27-36.
Xuan, K, et al. "Deciduous Autologous Tooth Stem Cells Regenerate Dental Pulp after Implantation into Injured Teeth." Science Translational Medicine, vol. 10, no. 455, 2018, eaaf3227.