Restorative dental treatment is a branch of dentistry focused on repairing, rebuilding, or replacing damaged or missing teeth to restore oral health, function, and aesthetics.
What Is Restorative Dental Treatment? (Scientific Definition)
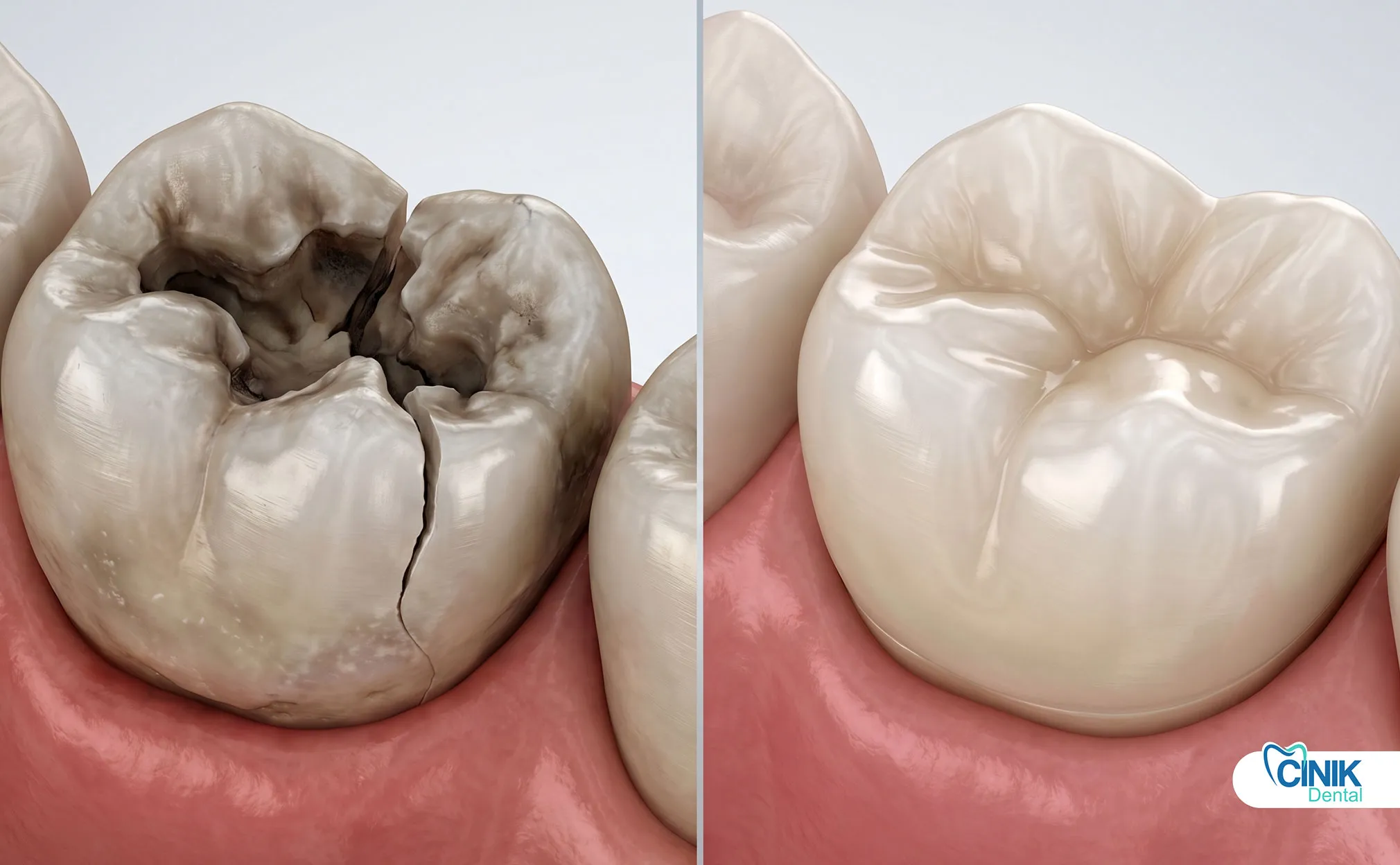
It restores the structure, integrity, and function of teeth affected by decay, trauma, or wear.
Restorative dental treatment refers to the clinical procedures that dental professionals use to repair or replace damaged, decayed, or missing teeth. The field encompasses a wide range of interventions that aim to restore the natural form and function of the dentition. According to Roberson (2019), restorative dentistry combines principles from multiple dental disciplines to achieve optimal patient outcomes.
The scientific foundation of restorative treatment rests on the understanding that oral health directly impacts systemic health. Research by Glick, Williams, and Kleinman (2015) demonstrates that untreated dental disease contributes to cardiovascular complications, diabetes management difficulties, and respiratory infections. Therefore, restorative procedures serve both local and systemic health objectives.
Core Objectives of Restorative Dentistry
The four main goals are restoring function, preserving natural teeth, preventing disease progression, and improving aesthetics.
Restorative dentistry pursues four primary clinical objectives:
Restore chewing and speaking function. Teeth play a critical role in mastication and phonation. When teeth suffer damage or loss, patients experience difficulty processing food and articulating speech sounds. Restorative treatments rebuild these functional capacities.
Preserve natural teeth whenever possible. Dental professionals prioritize conserving natural tooth structure. Research by Ericson (2017) confirms that retaining natural teeth supports periodontal health and maintains proper occlusal relationships. Extraction represents a last resort when preservation proves impossible.
Prevent further oral disease progression. Untreated dental caries and trauma create pathways for bacterial invasion. Restorative interventions seal these entry points and halt disease advancement. The procedure stops minor problems from becoming major complications.
Improve aesthetics as a secondary outcome. While function takes priority, modern restorative materials allow dentists to achieve natural-looking results. Patients regain confidence in their smiles alongside functional restoration.
Scope Within Modern Dentistry
Restorative dentistry overlaps with prosthodontics, endodontics, and periodontics.
Restorative treatment intersects with several dental specialties:
Prosthodontics covers crowns, bridges, and dentures. These appliances replace missing tooth structure or entire teeth.
Endodontics addresses root canal therapy. This procedure removes infected pulp tissue and seals the root canal system.
Periodontics manages supporting structures. Healthy gums and bone provide the foundation for successful restorations.
Who Needs Restorative Dental Treatment?
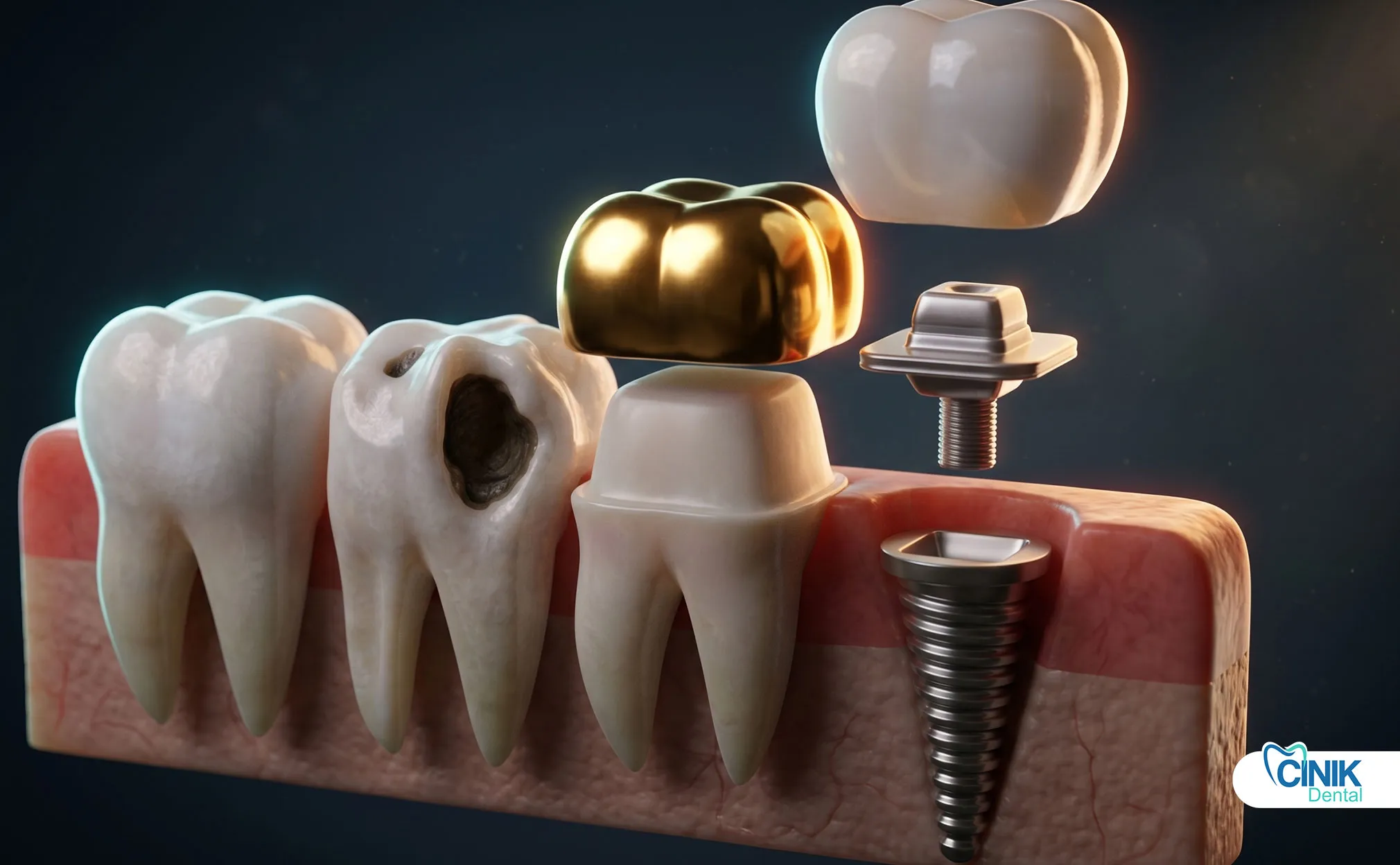
Patients with decayed, damaged, or missing teeth are primary candidates.
Dental professionals recommend restorative treatment for patients experiencing structural compromise of their dentition. The need arises from various pathological and traumatic conditions that affect tooth integrity. Research by Marcenes (2012) indicates that approximately 2.4 billion people worldwide suffer from untreated dental caries, making restorative intervention one of the most common dental procedures globally.
The decision to pursue restorative treatment depends on clinical examination findings, patient symptoms, and radiographic evidence. Dentists evaluate the extent of damage, remaining tooth structure, and overall oral health status before recommending specific interventions.
Main Clinical Indications
The five primary indications are dental caries, tooth fractures, tooth loss, enamel erosion, and failed old restorations.
Dental caries (cavities) represent the most common indication. Bacterial acid production demineralizes enamel and dentin, creating cavities that require filling. The World Health Organization (2017) identifies caries as the most prevalent non-communicable disease worldwide.
Tooth fractures or trauma necessitate immediate attention. Accidents, sports injuries, and biting hard objects can crack or break teeth. Traumatic dental injuries affect approximately 20% of the population according to Andreasen (2018).
Tooth loss requires replacement to maintain function and prevent adjacent tooth movement. Missing teeth create gaps that affect chewing efficiency and speech clarity.
Worn or eroded enamel develops from chemical or mechanical processes. Acidic foods, beverages, and gastric reflux erode enamel. Bruxism wears down occlusal surfaces through grinding.
Failed old restorations need replacement when they leak, fracture, or show marginal breakdown. No restoration lasts forever, and aging dental work requires periodic renewal.
Risk Factors
Poor oral hygiene, bruxism, acid erosion, and aging increase restorative treatment needs.
Certain conditions elevate the risk of requiring restorative procedures:
Poor oral hygiene allows plaque accumulation. Inadequate brushing and flossing permit bacterial colonization and acid production.
Bruxism (teeth grinding) generates excessive mechanical forces. Nocturnal grinding wears enamel and stresses restorations. Research by Manfredini (2013) links bruxism to temporomandibular disorders and tooth damage.
Acid erosion thins protective enamel layers. Frequent consumption of acidic beverages and foods accelerates tooth structure loss.
Aging dentition experiences cumulative wear. Older patients show higher rates of root caries and restoration failure.
Types of Restorative Dental Treatments (Complete Classification)
Treatments range from simple fillings to full-mouth rehabilitation.
Restorative procedures vary in complexity, materials, and clinical approach. Dental professionals classify treatments based on whether they involve direct placement in the mouth or laboratory fabrication. The classification system helps clinicians select appropriate interventions for specific clinical scenarios.
Direct Restorations
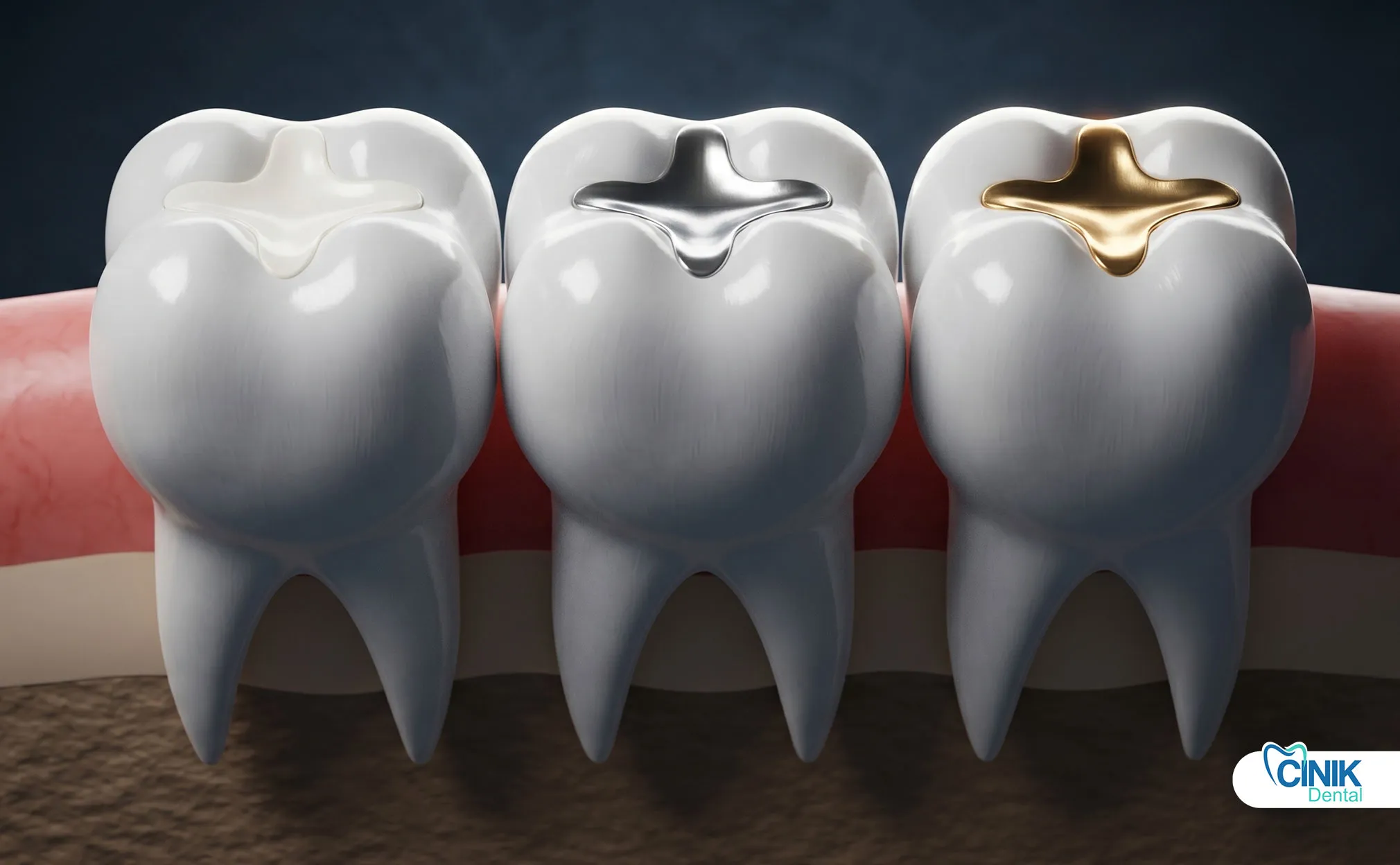
These include composite fillings, amalgam fillings, and glass ionomer restorations, applied in a single visit.
Direct restorations involve placing restorative material directly into prepared cavities during a single appointment. The dentist completes the entire procedure chairside without laboratory involvement.
Composite fillings use resin-based materials that bond chemically to tooth structure. These tooth-colored restorations offer excellent aesthetics and conservative preparation requirements. Research by Ferracane (2011) confirms composite resins provide durable restorations with proper technique.
Amalgam fillings employ silver-mercury alloys that have served dentistry for over 150 years. These restorations offer high strength and longevity, particularly for posterior teeth. Despite aesthetic limitations, amalgam remains a cost-effective option for large restorations.
Glass ionomer restorations release fluoride and bond chemically to enamel and dentin. These materials work well for root caries, pediatric applications, and temporary restorations. The fluoride release provides ongoing caries protection.
Key characteristic: Applied directly in a single visit without laboratory fabrication.
Indirect Restorations
These include crowns, bridges, inlays, onlays, and veneers, fabricated outside the mouth.
Indirect restorations require laboratory fabrication or CAD-CAM milling before cementation. These procedures typically require two appointments.
Crowns cover the entire clinical crown of a tooth. They protect weakened teeth and restore heavily damaged dentition. Materials include ceramic, metal, and porcelain-fused-to-metal.
Bridges replace missing teeth by spanning the gap with artificial teeth anchored to adjacent abutments. Traditional bridges require preparation of neighboring teeth.
Inlays and onlays restore specific portions of the occlusal surface. Inlays fit within cavity confines, while onlays extend over cusps. These conservative restorations preserve more tooth structure than full crowns.
Veneers are thin ceramic shells that cover facial surfaces. While primarily aesthetic, they also restore minor structural defects.
Key characteristic: Fabricated outside the mouth using laboratory or CAD-CAM technology.
Tooth Replacement Solutions
Options include dental implants, partial dentures, and full dentures.
When teeth require extraction or are already missing, replacement becomes necessary:
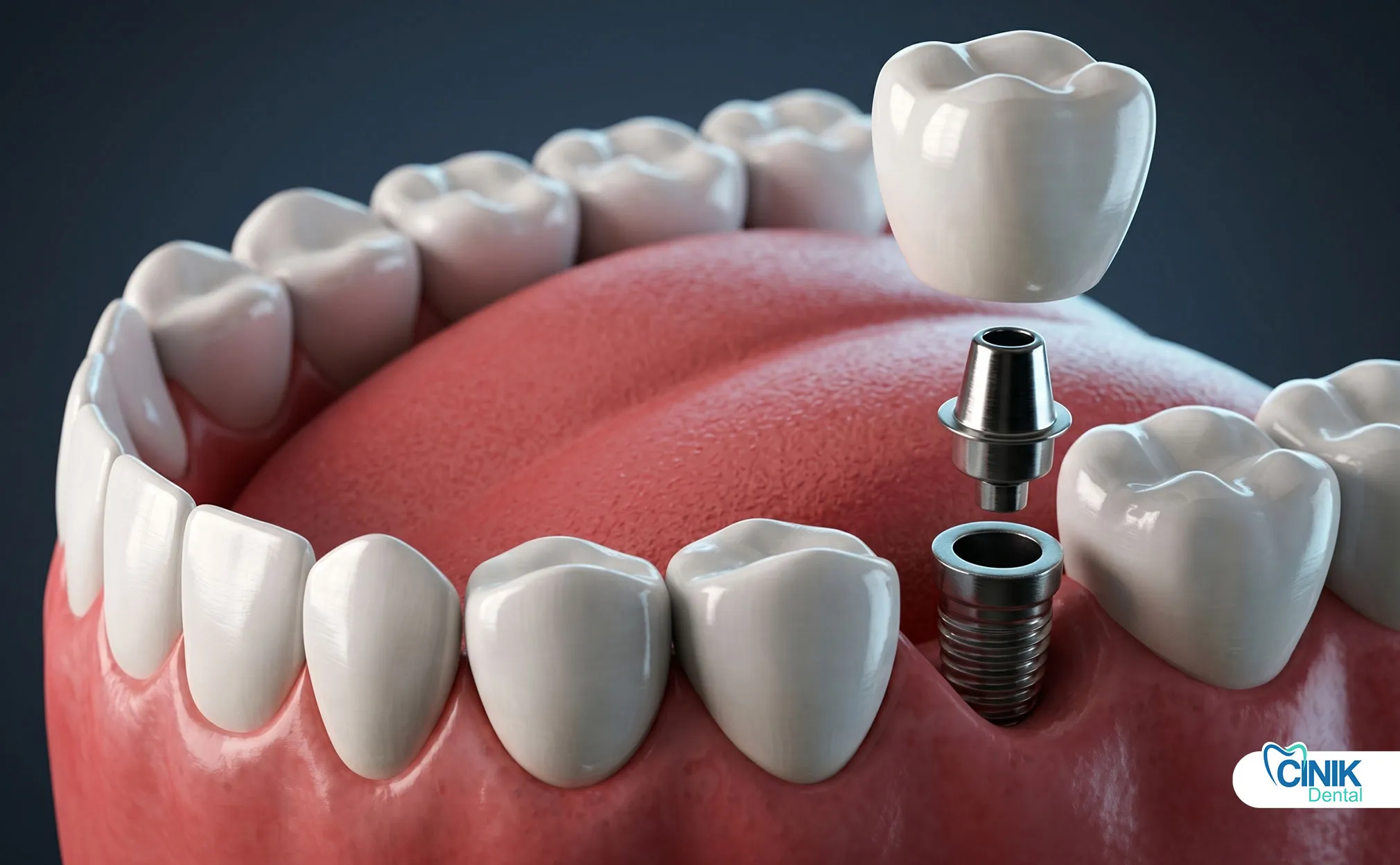
Dental implants serve as artificial tooth roots. Titanium posts integrate with jawbone through osseointegration. Research by Branemark (1983) established the scientific basis for modern implant dentistry. Implants support crowns, bridges, or dentures.
Partial dentures replace multiple missing teeth while remaining teeth provide support. Removable partial dentures use metal frameworks or flexible materials.
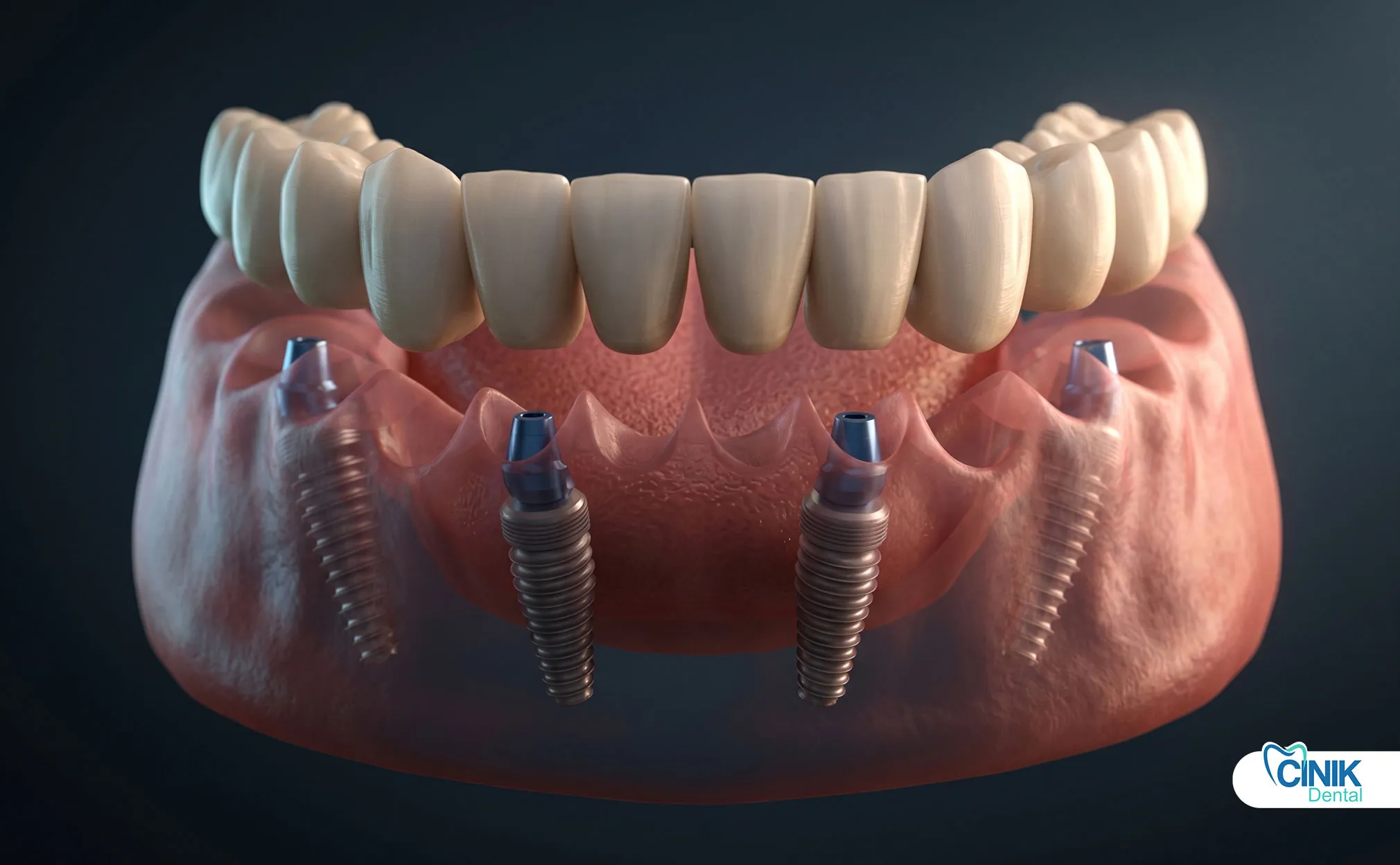
Full dentures replace entire arches of missing teeth. Conventional dentures rest on mucosal tissue, while implant-supported overdentures offer improved stability.
Advanced Restorative Procedures
These include root canal therapy, full-mouth reconstruction, and implant-supported prostheses.
Complex cases require advanced interventions:
Root canal therapy removes infected pulp tissue, disinfects the canal system, and seals the space. This procedure preserves teeth that would otherwise require extraction.
Full-mouth reconstruction addresses comprehensive dental rehabilitation. These cases involve multiple restorations across the entire dentition, often combining various treatment modalities.
Implant-supported prostheses include hybrid dentures and full-arch bridges. The All-on-4 concept popularized by Malo (2003) allows full-arch rehabilitation with minimal implants.
Step-by-Step Restorative Dental Treatment Process
The process involves diagnosis → planning → restoration → follow-up.
Successful restorative treatment follows a systematic clinical workflow. Each phase builds upon the previous one, ensuring optimal outcomes. The process requires patient cooperation, clinical expertise, and appropriate technology.
1. Clinical Examination & Diagnosis
This phase includes radiographs, caries risk assessment, and occlusion analysis.
The diagnostic phase establishes the foundation for treatment planning:
Radiographs (X-rays) reveal hidden pathology. Bitewing radiographs detect interproximal caries, while periapical films show periapical pathology and root morphology. Cone-beam computed tomography (CBCT) provides three-dimensional assessment for complex cases.
Caries risk assessment evaluates patient susceptibility. Dentists consider diet, oral hygiene, fluoride exposure, and previous caries history. Research by Featherstone (2004) established the CAMBRA (Caries Management By Risk Assessment) protocol.
Occlusion analysis examines bite relationships. Articulating paper identifies premature contacts, and study models allow detailed evaluation of occlusal schemes.
2. Treatment Planning
This phase involves material selection and prioritizing functional versus aesthetic needs.
Comprehensive planning addresses multiple factors:
Material selection depends on location, functional demands, and patient preferences. Posterior teeth require durable materials that withstand masticatory forces. Anterior restorations prioritize aesthetics and shade matching.
Functional versus aesthetic priority guides decision-making. Some patients require function restoration above all else, while others emphasize appearance. The treatment plan balances these competing demands.
3. Tooth Preparation
This involves removing decay and shaping the tooth for the restoration.
Preparation follows specific biomechanical principles:
Removal of decay or damaged tissue eliminates infected and affected dentin. Excavation extends to sound tooth structure. In deep caries, indirect pulp capping may preserve pulp vitality.
Shaping for restoration creates proper form and retention. Cavity design follows Black's principles of extension for prevention and resistance/retention forms. Modern minimally invasive techniques conserve tooth structure.
4. Restoration Placement
This involves direct placement or impression-taking followed by cementation.
The placement phase varies by restoration type:
Direct placement occurs for fillings. The dentist applies material in increments, shapes the anatomy, and polymerizes with light curing. Final polishing achieves smooth surfaces.
Impression-taking precedes indirect restorations. Traditional impressions use elastomeric materials, while digital scanning captures optical impressions for CAD-CAM fabrication.
Cementation/bonding secures the final restoration. Adhesive bonding provides retention for ceramic restorations, while conventional cements work for metal-based prostheses.
5. Recovery & Maintenance
This includes bite adjustment, oral hygiene protocols, and periodic check-ups.
Post-treatment care ensures longevity:
Bite adjustment verifies occlusal harmony. The dentist checks for high spots using articulating paper and adjusts accordingly. Proper occlusion prevents restoration fracture and patient discomfort.
Oral hygiene protocol educates patients on care specific to their restorations. Different materials and designs require tailored maintenance approaches.
Periodic dental check-ups monitor restoration integrity. Professional cleanings and examinations detect problems early. Research by Opdam (2007) shows that regular maintenance extends restoration longevity significantly.
Materials Used in Restorative Dentistry
Materials are chosen based on durability, aesthetics, and biocompatibility.
Material selection profoundly influences restoration success. Modern dentistry offers diverse options with varying properties. The ideal material balances strength, aesthetics, biocompatibility, and cost-effectiveness.
Common Materials
These include composite resin, ceramic/porcelain, metal alloys, and glass ionomer.
Composite resin dominates contemporary restorative practice. These materials contain Bis-GMA resin and filler particles. They offer excellent aesthetics, conservative preparation, and direct placement convenience. Nanofilled composites provide improved polishability and wear resistance.
Ceramic/porcelain provides superior aesthetics and biocompatibility. Feldspathic porcelain, lithium disilicate, and zirconia offer different strength and translucency profiles. Research by Lawn (2002) established ceramic fracture toughness criteria.
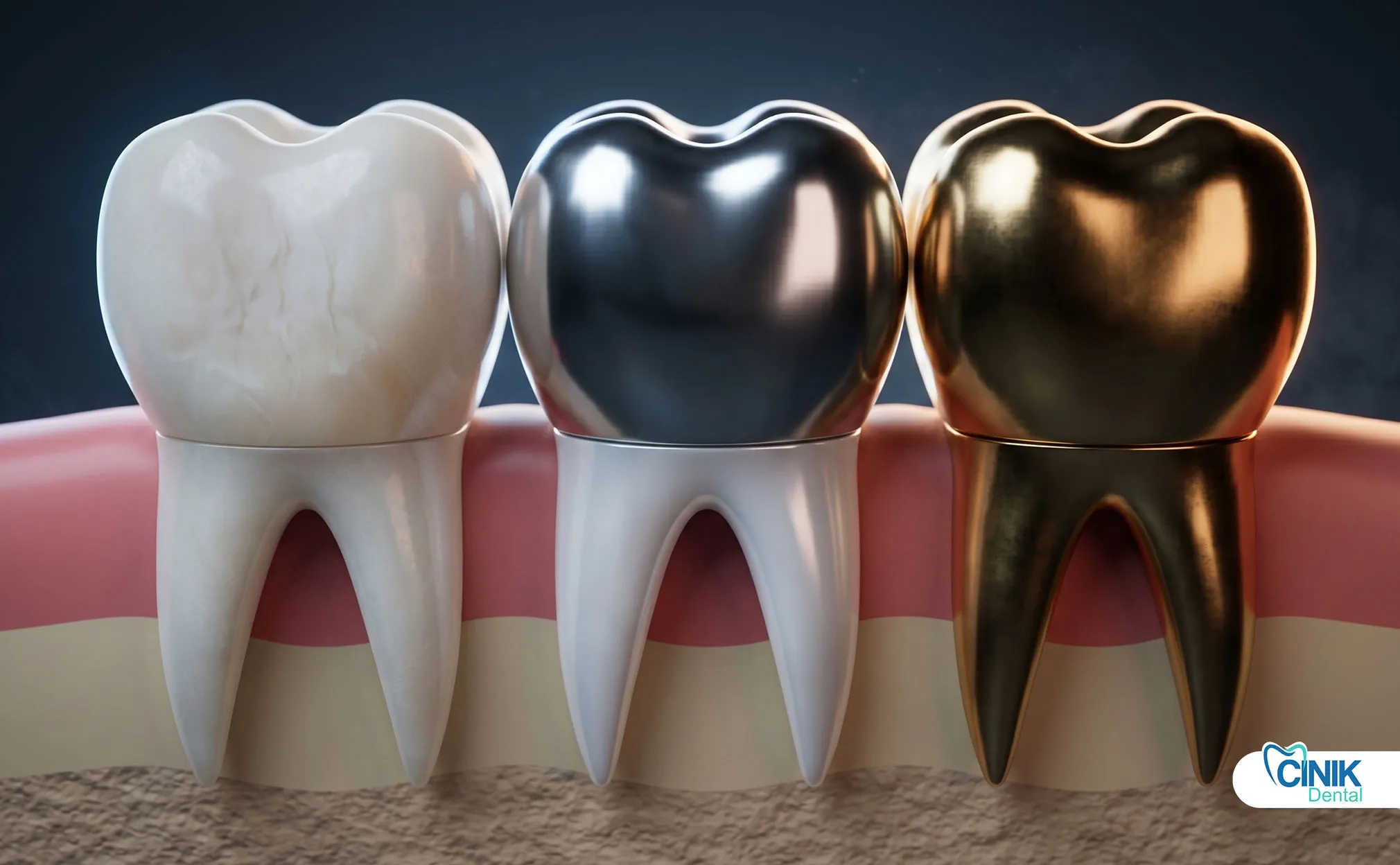
Metal alloys include gold, silver-palladium, and base metal alloys. These materials provide exceptional durability and wear characteristics. Cast metal restorations withstand high functional loads.
Glass ionomer serves specific clinical indications. These materials release fluoride, bond chemically to tooth structure, and exhibit biocompatibility. They work well for pediatric dentistry and root caries.
Modern Innovations
These include CAD/CAM restorations, zirconia prosthetics, and bioactive materials.
CAD/CAM restorations revolutionized indirect procedures. Computer-aided design and manufacturing enable same-day crowns and inlays. Chairside milling systems eliminate temporary restorations and second appointments.
Zirconia-based prosthetics offer metal-free durability. Yttria-stabilized tetragonal zirconia polycrystal (Y-TZP) provides flexural strength exceeding 900 MPa. These materials suit posterior crowns and implant abutments.
Bioactive materials represent the frontier of restorative science. These materials release ions that promote remineralization and inhibit bacterial growth. Research by Weir (2012) demonstrates bioactive glass potential for caries inhibition.
Benefits of Restorative Dental Treatment
It improves oral health, function, and quality of life.
Restorative treatment delivers multidimensional benefits that extend beyond the oral cavity. Patients experience improvements in physical health, psychological well-being, and social functioning. Research consistently demonstrates the positive impact of dental rehabilitation.
Functional Benefits
These include restored chewing, improved speech, and maintained bite alignment.
Restored chewing efficiency allows proper nutrition processing. Masticatory function directly impacts food selection and digestive health. Patients with restored dentition consume more diverse, nutritious diets.
Improved speech results from proper tooth positioning. Anterior teeth contribute to sibilant and fricative sound production. Missing or damaged anterior teeth cause speech impediments that restorations correct.
Maintained bite alignment prevents occlusal collapse. Missing teeth allow adjacent teeth to tilt and extrude. Restorations preserve arch integrity and occlusal stability.
Preventive Benefits
These include stopping decay progression, preventing bone loss, and reducing complication risks.
Stopping progression of decay eliminates infection sources. Sealed restorations prevent bacterial penetration and further demineralization.
Preventing bone loss occurs through implant placement. Tooth loss leads to alveolar ridge resorption. Implants maintain bone volume through functional stimulation.
Reducing risk of further complications addresses systemic connections. Research by Scannapieco (1999) links periodontal disease to respiratory infections. Restorations that improve periodontal health reduce these risks.
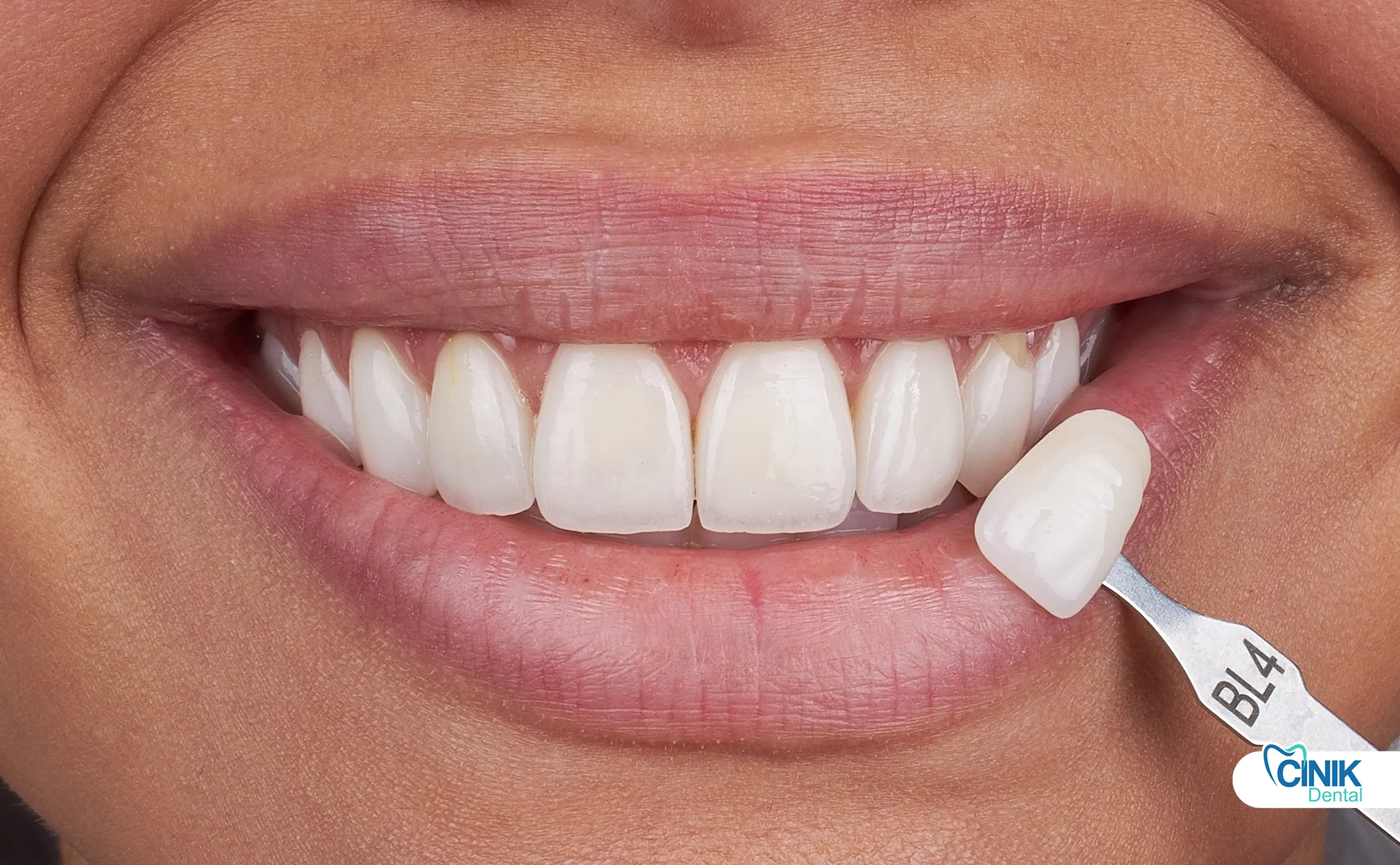
Aesthetic Benefits
These include natural-looking smiles and improved confidence.
Natural-looking smile restoration enhances facial aesthetics. Modern materials mimic natural tooth optical properties. Layering techniques create restorations indistinguishable from natural teeth.
Improved confidence affects social and professional interactions. Research by Kiyak (2008) demonstrates correlations between dental aesthetics and self-esteem. Patients report significant quality-of-life improvements after restorative treatment.
Restorative vs Cosmetic vs Preventive Dentistry
Restorative = function, Cosmetic = appearance, Preventive = disease avoidance.
Understanding the distinctions between dental disciplines helps patients set appropriate expectations. While overlap exists, each field maintains distinct primary objectives.
Type | Primary Goal | Examples | Insurance Coverage |
Restorative | Repair function | Crowns, implants, fillings | Usually covered |
Cosmetic | Enhance aesthetics | Whitening, veneers, bonding | Rarely covered |
Preventive | Avoid disease | Cleanings, fluoride, sealants | Usually covered |
Restorative dentistry prioritizes functional rehabilitation. The primary goal is restoring chewing ability and tooth integrity. Aesthetic improvements occur as secondary benefits.
Cosmetic dentistry focuses on appearance enhancement. These elective procedures improve smile aesthetics without necessarily addressing functional deficits. Teeth whitening represents a purely cosmetic intervention.
Preventive dentistry aims to avoid disease development. Regular cleanings, fluoride applications, and sealants prevent caries and periodontal disease. These services reduce the need for future restorative treatment.
Risks and Limitations of Restorative Treatments
Most treatments are safe but may involve minor complications.
While restorative dentistry enjoys high success rates, patients should understand potential complications. Informed consent requires discussing risks alongside benefits. Modern techniques minimize complications, but no procedure is entirely risk-free.
Possible Risks
These include post-treatment sensitivity, restoration failure, and rare infection.
Sensitivity after treatment commonly occurs following restorative procedures. Thermal and chemical sensitivity typically resolves within weeks. Persistent sensitivity may indicate pulp inflammation requiring additional intervention.
Restoration failure or wear develops over time. No restoration lasts indefinitely. Marginal leakage, fracture, and wear necessitate eventual replacement.
Infection remains rare but possible. Inadequate sterilization or post-operative contamination can introduce pathogens. Proper aseptic technique minimizes this risk.
Longevity Factors
Oral hygiene, material type, and bite forces determine restoration lifespan.
Multiple factors influence how long restorations last:
Oral hygiene practices directly impact restoration margins. Poor cleaning allows plaque accumulation and recurrent caries.
Material type determines wear characteristics. Gold restorations outlast composites, while ceramics offer intermediate durability.
Bite forces affect mechanical stress. Heavy bruxers experience faster restoration wear and failure.
How Long Do Restorative Treatments Last?
Longevity varies from 5 to 20+ years depending on the procedure.
Restoration longevity varies widely based on procedure type, material selection, and patient factors. Understanding expected lifespans helps patients plan for future maintenance and replacement.
Average Lifespan
Fillings last 5-10 years, crowns 10-15 years, and implants 20+ years.
Restoration Type | Average Lifespan | Range |
Composite fillings | 5-7 years | 3-10 years |
Amalgam fillings | 10-15 years | 8-20 years |
Ceramic crowns | 10-15 years | 7-20 years |
Gold crowns | 20+ years | 15-30 years |
Dental implants | 20+ years | 15-25+ years |
Bridges | 10-15 years | 7-20 years |
Research by Opdam (2007) in a 17-year longitudinal study found that 50% of amalgam restorations survived beyond 15 years, while composite restorations showed higher replacement rates. Implant survival rates exceed 95% at 10 years according to Jung (2012).
Cost of Restorative Dental Treatment (Global Perspective)
Costs vary widely depending on procedure complexity and location.
Restorative treatment costs present significant variation across geographic regions and clinical settings. Patients should consider multiple factors when budgeting for dental care. Insurance coverage and payment plans affect out-of-pocket expenses.
Key Cost Factors
These include restoration type, materials, dentist expertise, and location.
Type of restoration determines base cost. Simple fillings cost less than complex implant procedures. Full-mouth reconstruction represents the highest cost category.
Materials used affect pricing. Gold restorations cost more than amalgam. Premium ceramics command higher fees than standard materials.
Dentist expertise influences fees. Specialists such as prosthodontists charge premium rates for complex cases. Experience and advanced training justify higher costs.
Procedure | US Average Cost | UK Average Cost | India Average Cost | Turkey Average Cost | Thailand Average Cost | Mexico Average Cost |
Composite filling | $150-$400 | £60-£150 ($75-$190) | $20-$50 | $60-$100 | $60-$120 | $60-$120 |
Crown (porcelain) | $800-$1,500 | £400-$800 ($500-$1,000) | $150-$300 | $300-$400 | $300-$600 | $300-$600 |
Dental implant (single) | $3,000-$5,000 | £1,500-$2,500 ($1,900-$3,100) | $800-$1,500 | $400-$800 | $1,100-$2,000 | $750-$1,200 |
Full denture (per arch) | $1,000-$3,000 | £500-$1,500 ($625-$1,900) | $200-$500 | $700-$1,000 | $250-$450 | $350-$800 |
Geographic location creates significant variation. Urban areas and developed nations show higher fee schedules than rural or developing regions.Key findings for Turkey pricing:
Composite fillings: $60-$100
Porcelain crowns: $300-$400 (zirconia crowns range $160-$324)
Single dental implants: $400-$800 per implant (including implant + abutment + crown)
Full dentures: $700-$1,000 per arch
Turkey has become a major dental tourism destination, offering savings of 60-80% compared to US/UK prices while using internationally recognized implant brands like Straumann, Nobel Biocare, and high-quality materials .
Future Trends in Restorative Dentistry
Digital dentistry is transforming outcomes.
Restorative dentistry continues evolving through technological innovation. Emerging technologies promise improved precision, efficiency, and patient outcomes. The field stands at the intersection of materials science, digital technology, and biological understanding.
Emerging Technologies
These include AI-assisted diagnosis, 3D printing, and minimally invasive techniques.
AI-assisted diagnosis enhances detection accuracy. Machine learning algorithms analyze radiographs to identify caries and pathology. Research by Lee (2018) demonstrated AI systems matching or exceeding human diagnostic performance.
3D printing restorations enables chairside fabrication. Additive manufacturing produces crowns, bridges, and surgical guides with high precision. This technology reduces laboratory costs and treatment time.
Minimally invasive techniques preserve tooth structure. Air abrasion, chemomechanical caries removal, and partial caries excavation maintain healthy dentin. Research by Bjorndal (2010) supports selective caries removal in deep lesions.
Frequently Asked Questions (FAQs)
Is Restorative Dental Treatment Painful?
Most procedures use local anesthesia and cause minimal pain.
Modern anesthesia techniques ensure patient comfort during restorative procedures. Local anesthetics block nerve conduction completely. Patients feel pressure but not pain during treatment. Post-operative discomfort typically responds to over-the-counter analgesics.
How Do I Know If I Need Restorative Treatment?
Pain, visible cavities, or missing teeth indicate need.
Symptoms requiring evaluation include:
Persistent toothache or sensitivity
Visible holes or dark spots on teeth
Chipped or fractured teeth
Missing teeth
Difficulty chewing
Food impaction between teeth
Can Restorative Treatments Improve Aesthetics?
Yes, many treatments provide both functional and cosmetic benefits.
Modern restorative materials achieve excellent aesthetics. Tooth-colored composites and ceramics blend seamlessly with natural dentition. Patients receive functional restoration alongside smile enhancement.
Are Dental Restorations Permanent?
No, but they are long-lasting with proper care.
No dental restoration lasts forever. However, proper oral hygiene and regular dental visits maximize longevity. Implants can last decades, while fillings require periodic replacement.
What Is the Best Restorative Option?
The best option depends on damage severity and individual patient factors.
Treatment selection considers:
Extent of tooth damage
Remaining tooth structure
Patient oral hygiene
Budget constraints
Aesthetic priorities
Functional demands
Conclusion: Why Restorative Dental Treatment Matters
Restorative dental treatment is essential for maintaining oral health, preventing complications, and restoring quality of life through functional and durable dental solutions.
Restorative dental treatment represents a cornerstone of modern healthcare. The field addresses the universal problem of dental disease and trauma through scientifically validated interventions. Patients who pursue timely restorative care preserve their natural dentition, maintain systemic health, and enjoy improved quality of life.
The evidence supporting restorative dentistry continues growing. Research demonstrates clear connections between oral health and overall wellness. Functional dentition supports proper nutrition, clear speech, and social confidence. Modern materials and techniques deliver durable, aesthetic results that were impossible decades ago.
Patients should view restorative treatment as an investment in long-term health rather than an expense. Early intervention prevents costly complications and preserves treatment options. Regular dental examinations detect problems when they remain minor and easily treatable.
The future of restorative dentistry promises even better outcomes. Digital workflows, bioactive materials, and minimally invasive techniques will continue improving patient experiences. The fundamental goal remains unchanged: restoring health, function, and confidence through evidence-based dental care.
References:
Andreasen, J. O. "Traumatic Dental Injuries: A Manual." Wiley-Blackwell, 2018.
Bjorndal, L. "Indication and Outcomes of Different Caries Removal Techniques." Advances in Dental Research, vol. 22, no. 2, 2010, pp. 180-184.
Branemark, P. I. "Osseointegration and Its Experimental Background." Journal of Prosthetic Dentistry, vol. 50, no. 3, 1983, pp. 399-410.
Ericson, S. "The Role of Preservation of Natural Teeth in Oral Health." International Dental Journal, vol. 67, no. 1, 2017, pp. 22-28.
Featherstone, J. D. "The Caries Balance: The Basis for Caries Management by Risk Assessment." Oral Health & Preventive Dentistry, vol. 2, no. 1, 2004, pp. 259-264.
Ferracane, J. L. "Resin Composite: State of the Art." Dental Materials, vol. 27, no. 1, 2011, pp. 29-38.
Glick, M., Williams, D. M., and Kleinman, D. V. "A New Definition for Oral Health." Journal of the American Dental Association, vol. 146, no. 12, 2015, pp. 915-917.
Jung, R. E. "Long-Term Outcome of Dental Implants." Clinical Oral Implants Research, vol. 23, no. 1, 2012, pp. 93-96.
Kiyak, H. A. "Does Self-Perception of Dentition Predict Satisfaction with Facial Appearance?" Community Dentistry and Oral Epidemiology, vol. 36, no. 3, 2008, pp. 265-271.
Lawn, B. R. "Fracture of Brittle Solids." Cambridge University Press, 2002.
Lee, J. H. "Deep Learning in Dental Imaging." Journal of Dental Research, vol. 97, no. 9, 2018, pp. 942-949.
Malo, P. "All-on-4 Concept." Clinical Implant Dentistry and Related Research, vol. 5, no. 1, 2003, pp. 9-17.
Manfredini, D. "Bruxism: Definition, Epidemiology and Etiology." Dental Clinics of North America, vol. 57, no. 2, 2013, pp. 215-229.
Marcenes, W. "Global Burden of Oral Conditions in 1990-2010." Journal of Dental Research, vol. 92, no. 7, 2012, pp. 592-596.
Opdam, N. J. "Longevity of Restorations." Journal of Dentistry, vol. 35, no. 10, 2007, pp. 775-782.
Roberson, T. M. "Sturdevant's Art and Science of Operative Dentistry." Elsevier, 2019.
Scannapieco, F. A. "Role of Oral Bacteria in Respiratory Infection." Journal of Periodontology, vol. 70, no. 7, 1999, pp. 793-802.
Weir, M. D. "Bioactive Glass Composites." Dental Materials, vol. 28, no. 4, 2012, pp. 419-428.
World Health Organization. "Oral Health Fact Sheet." WHO, 2017.