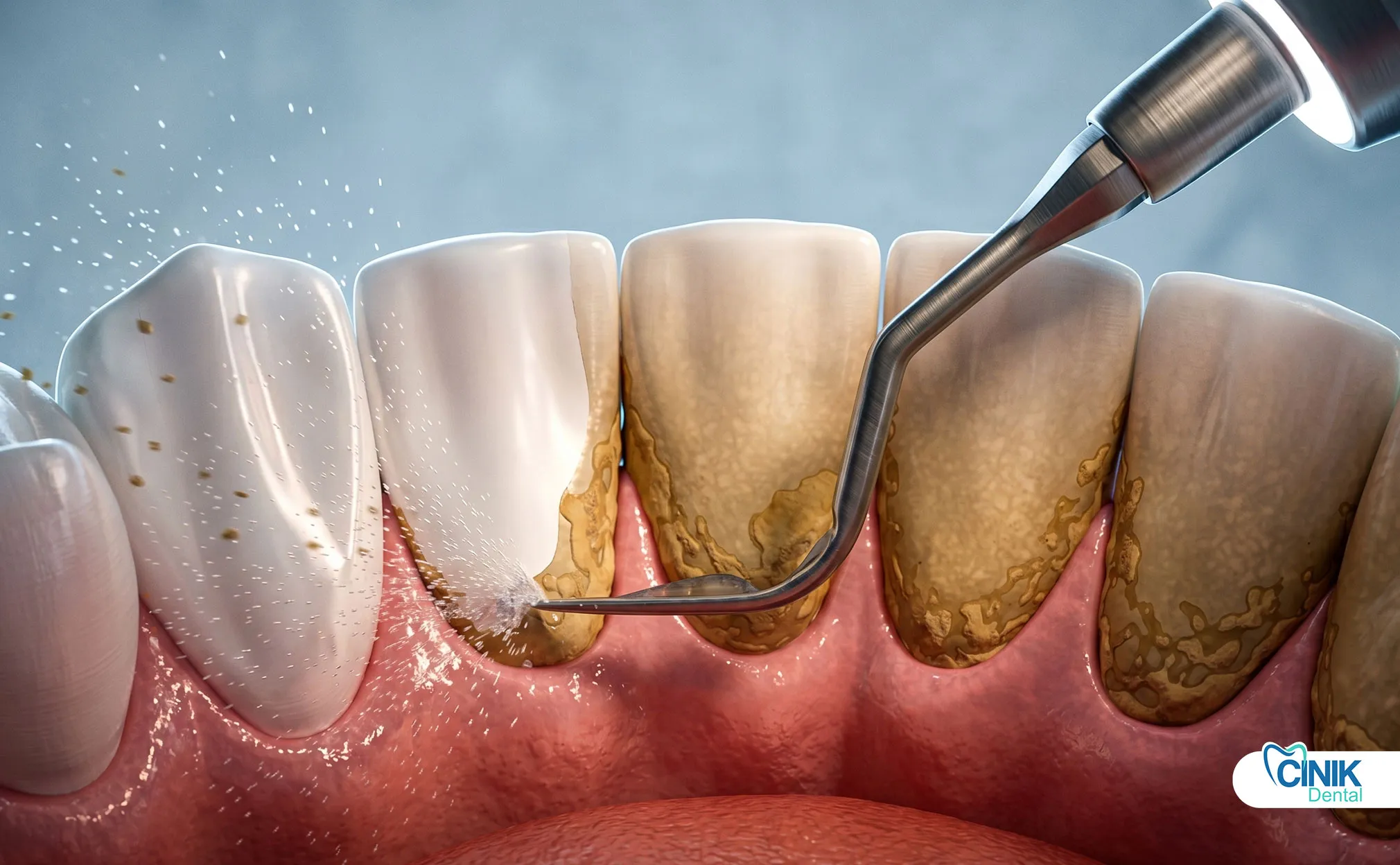
Tartar removal is the process of eliminating hardened dental plaque (calculus) from teeth, which can only be safely done through professional dental cleaning procedures. This article provides a comprehensive scientific analysis of tartar formation, removal methods, and prevention strategies based on current peer-reviewed research.
What Is Tartar (Dental Calculus)?
Tartar is mineralized plaque that hardens on teeth and cannot be removed by brushing alone.
Tartar, also known as dental calculus, represents one of the most common oral health challenges affecting the global population. Dental calculus is calcified bacterial plaque that forms throughout an individual's life on the subgingival and/or supragingival tooth surfaces underneath a layer of nonmineralized plaque (Hillson, 1996). The composition of dental calculus is primarily inorganic, consisting mainly of calcium and phosphorus, with minor components of carbonate, sodium, magnesium, silicon, iron, and fluoride. The minerals present include brushite, whitlockite, octacalcium phosphate, and hydroxyapatite (Hayashizaki et al., 2008; Lieverse, 1999; White, 1997). There is also an organic component (approximately 15%–20%) to calculus, consisting of microparticles such as phytoliths and starch granules, as well as biomolecules such as proteins, glycoproteins, lipids, DNA, carbohydrates, and bacteria (Lieverse, 1999; Warinner et al., 2014a,b).
The boundary between dental calculus and enamel or dentin is strong. There is bonding and sometimes complete fusion between the calculus and tooth apatite or enamel crystals (Rohanizadeh and Legeros, 2005), and residue may remain adhering to the teeth even after cleaning. This strong attachment explains why tartar cannot be removed through regular brushing once it has formed.
Plaque vs. Tartar: Key Differences
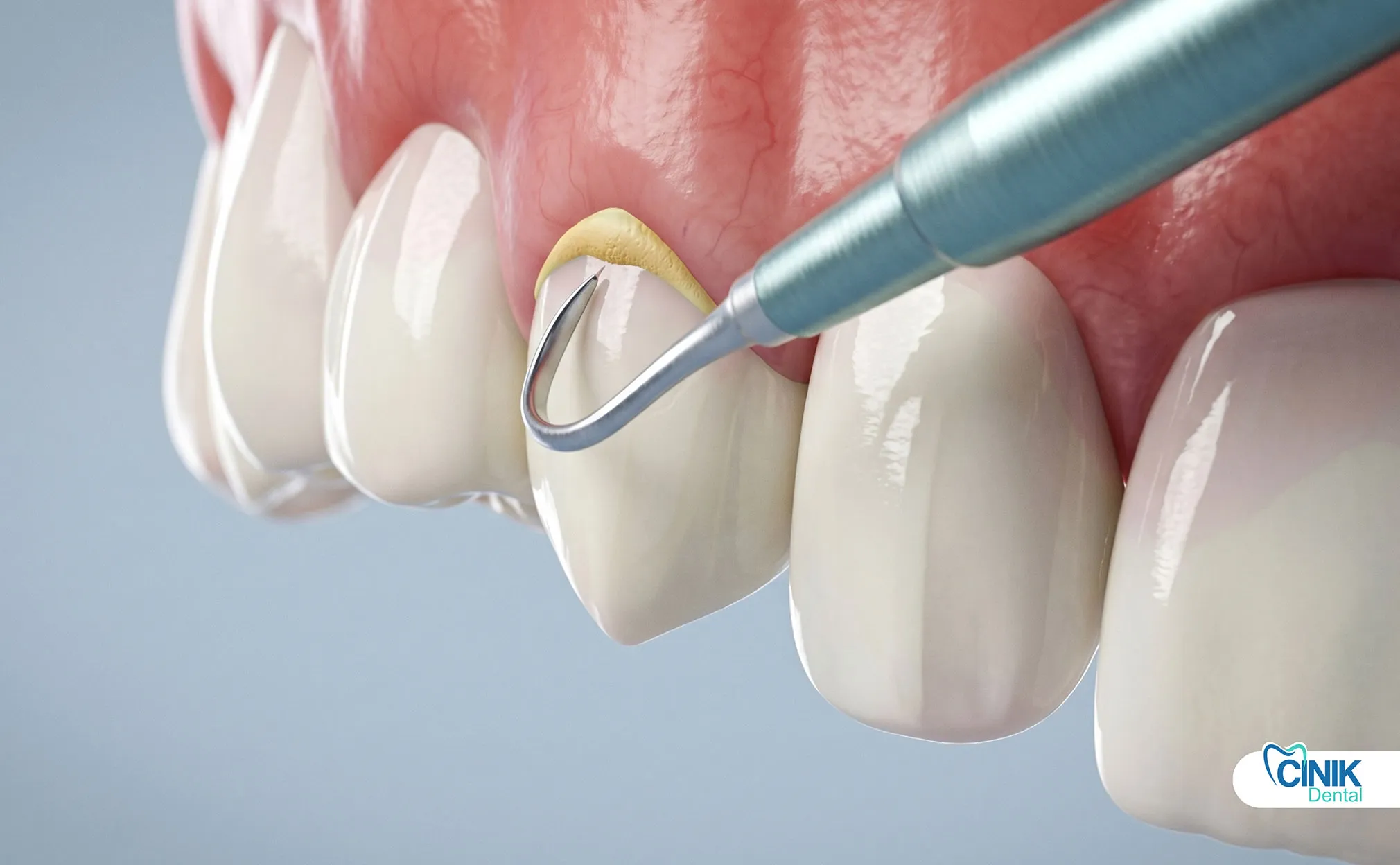
Understanding the distinction between plaque and tartar is essential for proper oral health management. The following table presents the critical differences:
Feature | Plaque | Tartar |
Texture | Soft, sticky biofilm | Hard, calcified deposit |
Color | Pale yellow or clear | Yellow to brown or black |
Removal Method | Brushing and flossing | Professional dental instruments |
Formation Time | Forms within hours | Hardens within 24–72 hours |
Composition | Bacteria, food debris, saliva | Mineralized calcium phosphate crystals |
Risk Level | Low (early stage, reversible) | High (advanced stage, requires intervention) |
Plaque represents a soft bacterial biofilm that accumulates on tooth surfaces throughout the day. This biofilm consists of bacteria, food particles, and saliva components. When plaque is not removed through regular brushing and flossing, it begins a mineralization process that transforms it into tartar. The microparticles and biomolecules in dental calculus originate from anything that comes in contact with the mouth, including food, animal and plant fibers, bacteria, parasites, protein, and DNA (Radini et al., 2017; Warinner et al., 2014b).
How Tartar Forms (Pathophysiology)
The formation of tartar follows a specific pathophysiological process that occurs in distinct stages. First, bacterial plaque accumulates on tooth surfaces. This plaque consists of bacteria and amorphous fluids. Second, mineralization occurs via calcium phosphate salts. Dental calculus forms as a result of the deposition of calcium phosphate crystals into this plaque (Lieverse, 1999). Third, hardening completes within 24–72 hours. Once this mineralization process finishes, the deposit becomes firmly attached to the tooth surface.
The rate of calculus formation, its microscopic structure, and how organic components are incorporated within it, are highly variable between individuals depending on diet, genetics, the bacterial microenvironment of the mouth (including pH and salivary flow), and dental care (Hanihara et al., 1994; Lieverse, 1999; White, 1997). Research suggests that relatively high alkaline conditions created by a high-protein diet may be associated with an increased calculus build-up; however, sugary or high-carbohydrate foods also have been linked to an increase in deposits (Hillson, 2005; Lieverse, 1999). Differences in the oral fluids of individuals may be more important for determining if one is more prone to calculus formation.
Types of Tartar
Dental professionals classify tartar into two main categories based on its location relative to the gumline:
Supragingival Calculus (Above Gumline): This type forms on the visible surfaces of teeth above the gumline. It typically appears yellow or tan in color and is easier to detect and remove. Supragingival calculus forms directly from saliva mineralization and tends to accumulate on the lingual surfaces of lower anterior teeth and buccal surfaces of upper molars.
Subgingival Calculus (Below Gumline): This type forms beneath the gumline within periodontal pockets. It appears darker (brown or black) due to blood pigments and is more harmful than supragingival calculus. Subgingival calculus contributes significantly to periodontal disease progression and requires specialized techniques for removal.
Why Is Tartar Removal Important?
Untreated tartar increases the risk of gum disease, cavities, and tooth loss.
The importance of tartar removal extends beyond cosmetic concerns. In 2021, global periodontal disease cases reached 951.3 million, with severe periodontal diseases estimated to affect more than 1 billion cases worldwide (WHO, 2025). The main risk factors for periodontal disease are poor oral hygiene and tobacco use. The global burden of periodontal diseases has increased substantially from 1990 to 2021, with the age-standardized prevalence rate rising by 8.44% worldwide (GBD Study, 2024).
Clinical Consequences of Tartar Build-Up
Tartar accumulation triggers several serious clinical conditions:
Gingivitis and Periodontitis: Tartar harbors bacteria that cause inflammation of the gums (gingivitis). If left untreated, this progresses to periodontitis, where the supporting bone and tissue deteriorate. Scaling and root planing has become the gold standard in gum disease treatment because it works well without being as intensive as alternatives. Scientists at the Journal of the American Dental Association looked at the result of 72 studies and found that deep cleanings improve the way the gums attach to the teeth by 0.5 millimeters (Holzinger Perio, 2022).
Halitosis (Bad Breath): The bacteria in tartar produce volatile sulfur compounds that cause persistent bad breath that cannot be eliminated through mouthwash or mints alone.
Tooth Discoloration: Tartar is porous and absorbs stains from food, beverages, and tobacco, leading to unsightly yellow or brown discoloration.
Gum Recession: As tartar accumulates below the gumline, it causes the gums to pull away from teeth, exposing sensitive root surfaces and creating deeper pockets for further bacterial accumulation.
Tartar as a Plaque Retention Factor
Tartar creates a vicious cycle of oral health deterioration. The rough surface of calculus traps more bacteria, creating a plaque-tartar cycle. Once tartar forms, its rough texture provides an ideal surface for new plaque accumulation. This new plaque then mineralizes into additional tartar, accelerating the deterioration process. The cycle continues until professional intervention breaks it.
Can Tartar Be Removed at Home?
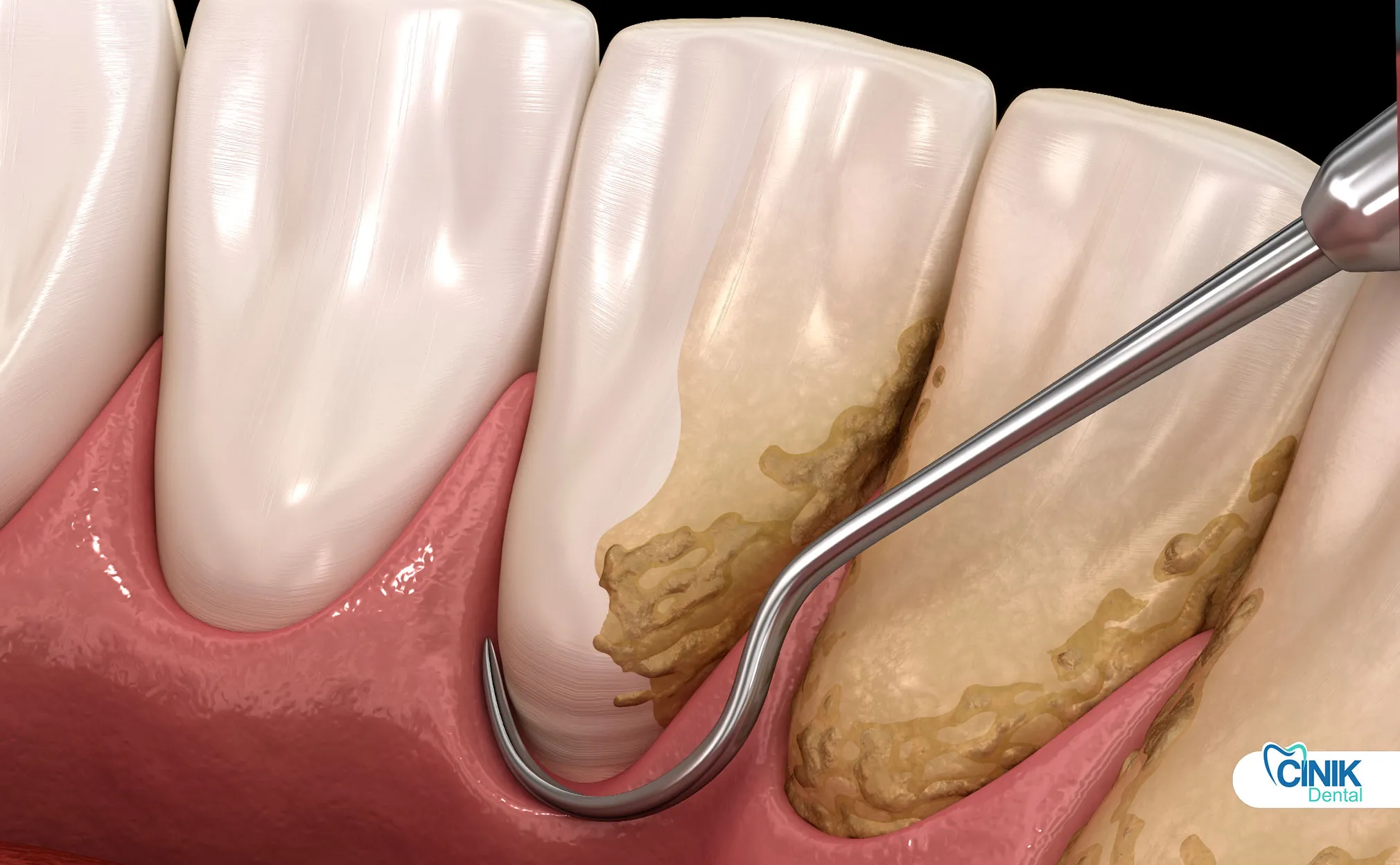
No, once tartar forms, it cannot be safely removed at home and requires professional treatment.
This is one of the most common misconceptions in oral health. While many products claim to dissolve or remove tartar at home, scientific evidence does not support these claims for existing calculus deposits.
Why Brushing and Flossing Are Not Enough
Tartar is strongly attached to enamel through a process of crystal fusion. Regular brushing and flossing cannot generate the mechanical force necessary to break this bond without damaging the tooth structure. The minerals in tartar (primarily calcium phosphate) form crystals that integrate with the tooth surface at the microscopic level.
Removing tartar requires mechanical scaling tools that dental professionals use. These instruments are specifically designed to fracture the calculus-tooth interface without damaging the underlying enamel or dentin.
Risks of DIY Tartar Removal
Attempting to remove tartar at home poses significant risks:
Enamel Damage: Metal picks, hard abrasives, or excessive force can scratch or remove enamel, leading to sensitivity and increased cavity risk.
Gum Injury: Sharp instruments can lacerate gum tissue, causing bleeding, infection, and potential gum recession.
Infection Risk: Improper technique can introduce bacteria into the bloodstream or damage tissue barriers that protect against infection.
A 2024 randomized clinical trial demonstrated that a novel enzyme-containing dentifrice (Tartarase) achieved approximately 40% reduction in calculus over 4 weeks, while control toothpaste users experienced 12% calculus increase (BMC Oral Health, 2024). However, this represents a reduction in accumulation rate, not removal of existing hardened deposits.
What Home Care Can Actually Do
While home care cannot remove existing tartar, it plays a crucial preventive role:
Prevent Plaque Buildup: Regular brushing and flossing remove plaque before it mineralizes into tartar.
Slow Tartar Formation: Anti-tartar toothpastes can reduce the rate of new calculus formation by 15-23% (Fairbrother et al., 1997).
Maintain Professional Results: Home care preserves the benefits of professional cleaning between visits.
Professional Tartar Removal Methods
Dentists remove tartar using scaling and polishing techniques with specialized instruments.
Professional tartar removal represents the only safe and effective method for eliminating existing calculus deposits. The procedures vary based on the severity and location of tartar accumulation.
Dental Scaling (Standard Cleaning)
Standard professional cleaning, also called prophylaxis, focuses on removing supragingival tartar. This procedure involves:
Removal of supragingival tartar from visible tooth surfaces
Use of hand scalers or ultrasonic devices
Polishing to smooth tooth surfaces
Application of fluoride for protection
The average cost for standard cleaning in the United States ranges from $75-$200 per visit, while deep cleaning (scaling and root planing) runs $150-$350 per quadrant, with full-mouth treatment costing $600-$1,400 or more (CWD Dental Group, 2025).
Deep Cleaning (Scaling and Root Planing)
Scaling and root planing (SRP) serves as the first line of treatment for chronic gum disease. This procedure removes subgingival tartar and smooths root surfaces. It can take between one and four visits to complete, depending on the severity of the gum disease (Holzinger Perio, 2022).
Clinical studies demonstrate that SRP significantly improves periodontal health. In pockets deeper than 6 mm, SRP provides a mean clinical attachment gain of 1.19 mm and a mean probing depth reduction of 2.19 mm. In pockets of moderate (4–6 mm) depth, the respective values are 0.55 mm and 1.29 mm. SRP also reduces clinical signs of inflammation, reducing bleeding on probing to approximately 43% of baseline levels (Cobb, 1996; ScienceDirect, 2024).
A three-arm randomized controlled trial by Qureshi et al. (2021) found that scaling and root planing improves glycemic control of type-2 diabetes mellitus patients independently of antibiotic use. Therefore, SRP after every 6 months may be suggested and included as a part of overall diabetes management for patients suffering with T2DM.
Ultrasonic vs. Manual Scaling
Dental professionals choose between ultrasonic and manual instruments based on clinical needs:
Feature | Ultrasonic Scaling | Manual Scaling |
Speed | Faster removal | Slower, more deliberate |
Comfort | Less patient discomfort | May cause more sensation |
Precision | Good for bulk removal | Superior for fine finishing |
Access | Excellent for deep pockets | Better for tight spaces |
Surface Finish | Requires follow-up polishing | Can provide smoother finish |
Research indicates that clinical outcomes are consistent regardless of instrument type used (chronic periodontitis patients, independent of the types of instruments used (power-driven or manual)) (ScienceDirect, 2024). However, patients with poor oral hygiene, smoking habits, or poor glycemic control exhibit a less favorable response to SRP.
Polishing and Fluoride Treatment
Following scaling, dentists polish teeth to smooth enamel surfaces. This polishing reduces plaque adhesion and makes future cleaning easier. Fluoride treatment then strengthens enamel and increases resistance to acid attacks.
Step-by-Step Tartar Removal Procedure
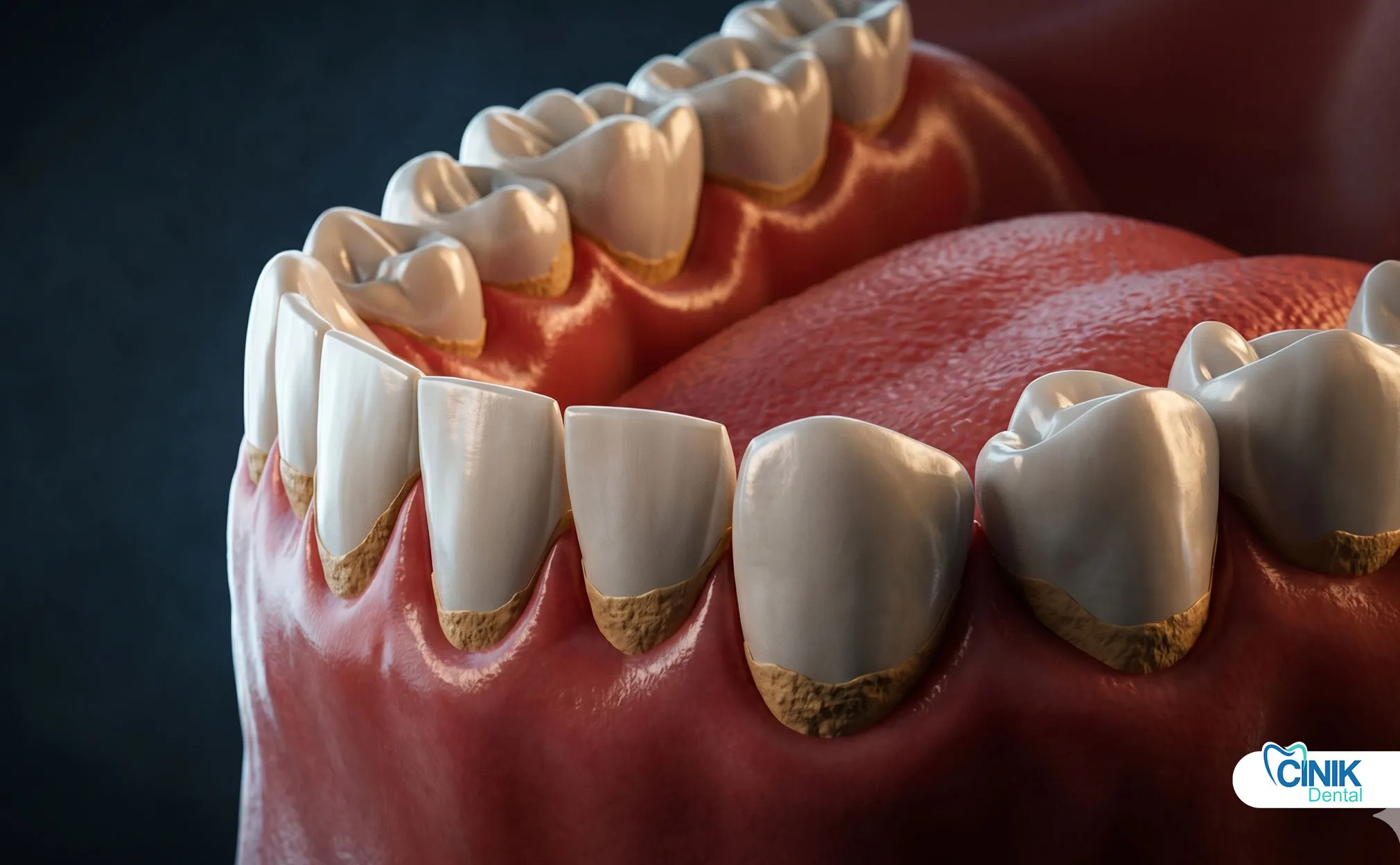
The process involves examination, scaling, polishing, and preventive guidance.
Understanding the clinical workflow helps patients prepare for tartar removal appointments and appreciate the thoroughness of professional care.
Clinical Workflow
Step 1: Oral Examination: The dentist or hygienist performs a comprehensive visual examination, often supplemented with periodontal probing to measure pocket depths and identify areas of concern.
Step 2: Plaque and Tartar Detection: Using dental explorers and sometimes disclosing agents, the clinician identifies all calculus deposits, both visible and hidden below the gumline.
Step 3: Scaling (Removal): The clinician uses ultrasonic scalers and hand instruments to fracture and remove calculus deposits. Ultrasonic devices use high-frequency vibrations to break up tartar while water spray cools the tip and flushes debris.
Step 4: Polishing: A rotating rubber cup with abrasive paste smooths tooth surfaces to reduce future plaque accumulation.
Step 5: Post-Treatment Care Advice: The dental professional provides specific instructions for home care, including brushing technique, interdental cleaning, and follow-up scheduling.
A 2024 randomized clinical trial demonstrated that twice-daily powered toothbrushing sustains the effects of SRP for bleeding on probing, probing pocket depth, and plaque significantly better than manual toothbrushing in Stage I/II periodontitis population, with differences evident 4 weeks following SRP and persisting for 24 weeks (Journal of Investigative and Clinical Dentistry, 2024).
Symptoms That Indicate You Need Tartar Removal
Visible deposits, bleeding gums, and bad breath are key warning signs.
Recognizing the signs of tartar accumulation enables timely intervention before serious damage occurs.
Early Signs
Yellow or Brown Deposits: Visible discoloration along the gumline or between teeth indicates calculus formation.
Rough Tooth Surfaces: When you run your tongue over teeth, tartar feels rough and hard compared to smooth enamel.
Persistent Film: A constant feeling of "fuzzy" or coated teeth that doesn't resolve with brushing suggests plaque mineralization.
Advanced Symptoms
Bleeding Gums: Gums that bleed during brushing or flossing indicate inflammation caused by bacterial accumulation in tartar.
Gum Recession: Teeth appear longer as gums pull away from the tooth crown due to chronic inflammation.
Persistent Bad Breath: Odor that remains despite oral hygiene efforts often signals bacterial overgrowth in calculus deposits.
Tooth Sensitivity: Exposed root surfaces from gum recession react painfully to temperature changes or sweet foods.
Cost of Tartar Removal (Global Comparison)
Costs vary by region, procedure type, and severity.
Dental care costs vary significantly across countries due to differences in labor costs, overhead, regulatory requirements, and healthcare systems.
Average Cost Table
Procedure | Turkey | UK | USA | Thailand | Mexico |
Basic Cleaning | €30–€100 | €60–€150 | $100–$300 | €25–€80 | €35–€90 |
Deep Cleaning (per quadrant) | €100–€300 | €200–€400 | $150–$350 | €80–€200 | €90–€250 |
Full Mouth Deep Cleaning | €400–€1,200 | €800–€1,600 | $600–$1,400 | €320–€800 | €360–€1,000 |
Note: Costs are approximate and vary by clinic location, technology used, and individual case complexity. Currency conversions are estimates.
Factors Affecting Cost
Severity of Tartar Buildup: Heavy calculus accumulation requires longer appointment times and more complex instrumentation.
Clinic Technology: Practices using advanced ultrasonic scalers, laser assistance, or digital imaging may charge higher fees.
Number of Sessions: Severe cases often require multiple appointments to complete full-mouth debridement safely.
Geographic Location: Urban centers typically have higher costs than rural areas due to increased overhead expenses.
Cost Comparison Analysis
Turkey offers competitive pricing for dental tourism, with costs 40-60% lower than US rates while maintaining high standards of care. The UK and USA represent higher-cost markets due to regulatory compliance, staff salaries, and facility overhead. Mexico provides an accessible option for North American patients seeking quality care at reduced costs.
How to Prevent Tartar Formation?
Consistent oral hygiene and professional cleanings are the most effective prevention methods.
Prevention is significantly more effective and less expensive than treatment. The guideline from the Ministry of Health Malaysia recommends that supportive periodontal treatment should be provided every three to six months (Ministry of Health Malaysia, 2017).
Daily Oral Hygiene Protocol
Brush Twice Daily: Use a soft-bristled brush and fluoride toothpaste for two minutes each session. Powered toothbrushes demonstrate superior plaque removal compared to manual brushing.
Floss Once Daily: Interdental cleaning removes plaque from areas brushes cannot reach. Failure to floss leaves approximately 40% of tooth surfaces uncleaned.
Use Fluoride Toothpaste: Fluoride strengthens enamel and increases resistance to acid demineralization.
Research shows that following SRP, use of a powered toothbrush may be an appropriate home hygiene strategy to help sustain the effects of in-office periodontal care in a non-surgical periodontitis population (Journal of Investigative and Clinical Dentistry, 2024).
Professional Prevention
Dental Check-ups Every 6 Months: Regular professional monitoring catches early calculus formation before it becomes problematic.
Early Plaque Removal: Professional cleanings remove plaque from areas patients miss, preventing mineralization.
Diet and Lifestyle Factors
Reduce Sugar Intake: Sugary foods feed oral bacteria that produce acids and accelerate plaque formation.
Avoid Tobacco: Smoking reduces saliva flow and alters oral bacteria, increasing calculus formation risk.
Stay Hydrated: Adequate water intake maintains saliva flow, which naturally cleanses teeth and neutralizes acids.
Best Toothpastes and Products for Tartar Control
Anti-tartar toothpaste and antimicrobial mouthwash help prevent buildup (not remove existing tartar).
Understanding the limitations and capabilities of anti-tartar products helps set realistic expectations.
Active Ingredients to Look For
Fluoride: Strengthens enamel and prevents decay. Essential for all toothpaste formulations.
Pyrophosphates: Inhibit calcium phosphate crystal formation, reducing tartar accumulation by 22-23% (Fairbrother et al., 1997).
Zinc Compounds: Zinc citrate and zinc chloride reduce calculus formation by 17-19% through crystal growth inhibition (Fairbrother et al., 1997).
A 2025 single-blind randomized controlled clinical trial found that a 5% pyrophosphate-containing dentifrice, used twice daily for 2 minutes for 3 months compared with a fluoridated dentifrice, showed better plaque index scores that were statistically significant (p = 0.006), though calculus reduction differences were not statistically significant (The Journal of Clinical Dentistry, 2025).
Limitations of Anti-Tartar Products
Preventive Only: These products cannot dissolve or remove existing hardened calculus.
No Effect on Hardened Calculus: Once mineralization completes, only mechanical removal works.
Variable Efficacy: Individual response varies based on saliva composition, diet, and genetic factors.
Tartar Removal vs. Plaque Removal
Plaque removal is preventive; tartar removal is corrective.
Understanding this distinction helps patients prioritize their oral health efforts appropriately.
Key Differences Table
Feature | Plaque | Tartar |
Physical State | Soft, sticky biofilm | Hard, mineralized deposit |
Formation Time | Continuous (hours) | 24-72 hours for initial hardening |
Removal Method | Brushing, flossing, rinsing | Professional scaling instruments |
Prevention/Treatment | Preventive daily care | Corrective professional procedure |
Reversibility | Fully reversible with hygiene | Irreversible without professional help |
Health Risk Level | Low (manageable) | High (requires intervention) |
Risks of Ignoring Tartar Removal
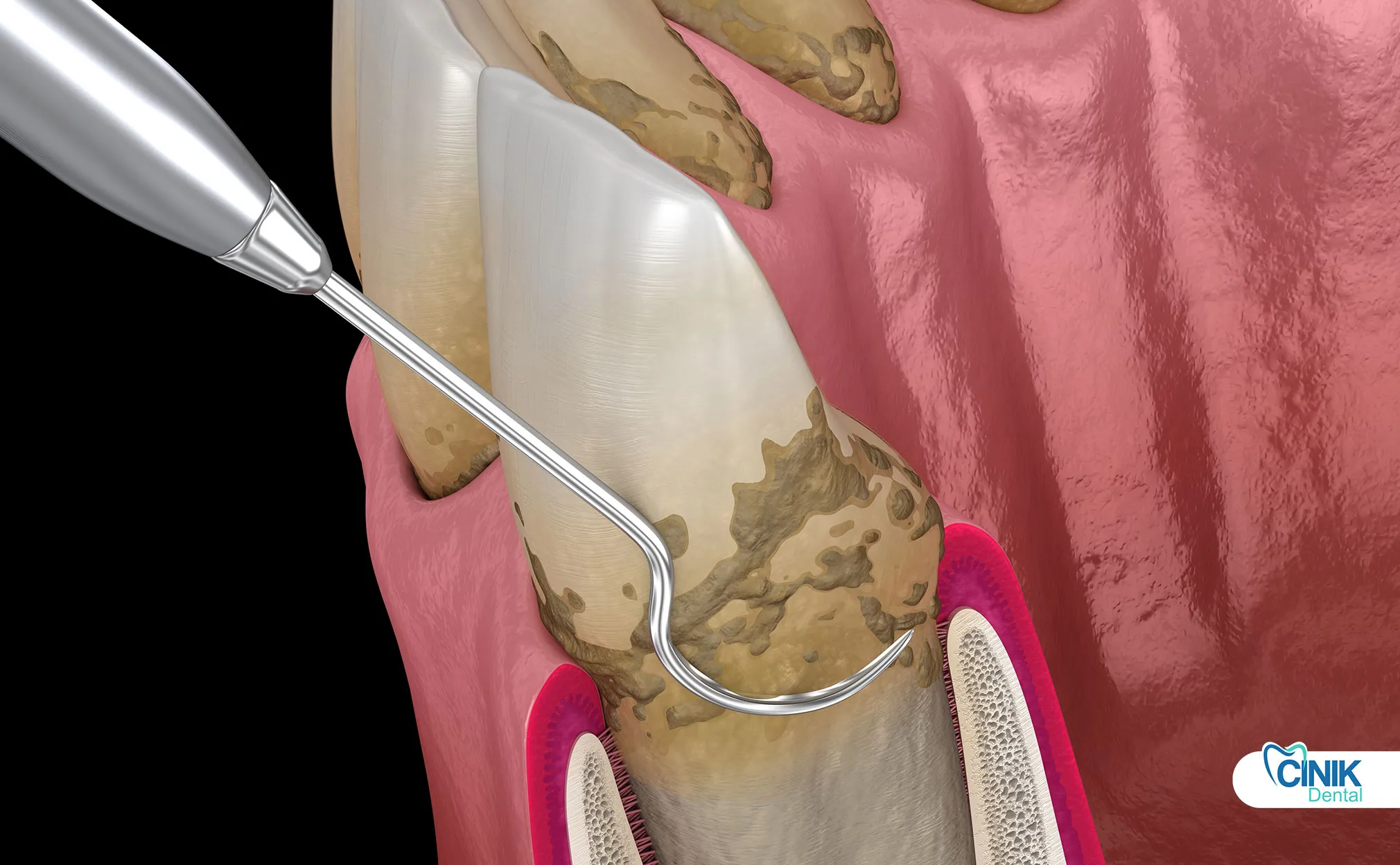
Untreated tartar can lead to irreversible gum disease and tooth loss.
The consequences of neglecting tartar removal extend far beyond cosmetic concerns.
Short-Term Risks
Gum Inflammation: Chronic bacterial irritation causes red, swollen, painful gums.
Bleeding: Gums bleed easily during brushing, flossing, or even spontaneous contact.
Discomfort: Patients experience persistent bad taste and oral malodor.
Long-Term Risks
Periodontitis: The supporting bone and ligaments deteriorate, leading to tooth mobility. By 2050, projections indicate over 1.56 billion people will be living with severe periodontitis, representing a 44.32% increase from 2021 (Frontiers in Oral Health, 2025).
Bone Loss: Alveolar bone resorption is irreversible without surgical intervention.
Tooth Mobility: Teeth become loose as supporting structures weaken.
Tooth Loss: Advanced periodontitis is the leading cause of adult tooth loss. The estimated global average prevalence of complete tooth loss is almost 7% among people aged 20 years or older. For people aged 60 years or older, a much higher global prevalence of 23% has been estimated (WHO, 2025).
Frequently Asked Questions (FAQ)
How Often Should Tartar Be Removed?
Every 6 months for most patients, or more frequently for high-risk individuals. The guideline from the Ministry of Health Malaysia recommends supportive periodontal treatment every three to six months (Ministry of Health Malaysia, 2017). Patients with a history of periodontal disease, smokers, or those with diabetes may require 3-4 month intervals.
Does Tartar Removal Hurt?
Usually painless for standard cleaning. Mild discomfort may occur during deep cleaning (scaling and root planing) for patients with sensitive gums or deep pockets. Local anesthesia is available for comfort during extensive procedures.
Can Tartar Come Back After Cleaning?
Yes, if oral hygiene is poor. Tartar formation is a continuous process. Without diligent home care and regular professional maintenance, new calculus will form on teeth.
Is Tartar Removal Safe?
Yes, when performed by dental professionals. The procedure is routine and safe. Evidence-based guidelines recommend that scaling and root planing should be considered as first-line therapy for patients with chronic periodontitis (Smiley et al., 2015; Tonetti et al., 2015).
Conclusion: The Role of Tartar Removal in Oral Health
Tartar removal is essential for preventing gum disease and maintaining long-term dental health.
Tartar removal stands as a cornerstone of preventive dentistry and overall health maintenance. The evidence is clear: tartar is irreversible at home, professional cleaning is mandatory for existing deposits, and prevention is more effective than treatment.
The global burden of periodontal diseases has reached unprecedented levels, affecting over 1 billion people worldwide. Population growth and aging are the primary drivers of increased disease burden, with low-middle SDI regions showing the highest rates (GBD Study, 2024). These statistics underscore the critical importance of regular tartar removal as part of comprehensive oral health strategy.
Professional tartar removal not only eliminates existing calculus but also interrupts the cycle of plaque accumulation and mineralization. When combined with diligent home care using proper technique and appropriate products, patients can maintain optimal oral health and prevent the progression from gingivitis to irreversible periodontitis.
The investment in regular professional cleaning, both financially and in terms of time, pales in comparison to the costs of treating advanced periodontal disease, tooth loss, and associated systemic health complications. As research continues to demonstrate connections between oral health and conditions such as diabetes, cardiovascular disease, and adverse pregnancy outcomes, the importance of tartar removal extends beyond the mouth to whole-body wellness.
Schedule your professional evaluation today and take the definitive step toward preserving your natural teeth for life.
References
Cobb, Charles M. "Non-surgical pocket therapy: mechanical." Annals of Periodontology 1.1 (1996): 443-490.
Fairbrother, K. J., et al. "The comparative clinical efficacy of pyrophosphate/triclosan, copolymer/triclosan and zinc citrate/triclosan dentifrices for the reduction of supragingival calculus formation." Journal of Clinical Dentistry 8.2 (1997): 62-66.
Frontiers in Oral Health. "Global Burden of Periodontal Diseases Analysis 2021." Frontiers in Oral Health, 2025.
GBD Study 2021. "Global burden of periodontal diseases among the working-age population from 1990–2021." PMC, 2024.
Hayashizaki, J., et al. "Mineral components of dental calculus." Archives of Oral Biology, 2008.
Hillson, Simon. Dental Anthropology. Cambridge University Press, 1996.
Holzinger Perio. "The Effectiveness of Scaling and Root Planing." Holzinger Periodontics, 2022.
Journal of Investigative and Clinical Dentistry. "The effects of scaling and root planing plus home oral hygiene maintenance in Stage I/II periodontitis population: A 24-week randomized clinical trial." Journal of Investigative and Clinical Dentistry, 2024.
Lieverse, A. R. "Diet and the etiology of dental calculus." International Journal of Osteoarchaeology, 1999.
Ministry of Health Malaysia. "Clinical Practice Guidelines for Periodontal Diseases." Ministry of Health Malaysia, 2017.
Pontis Biologics. "Clinical efficacy of novel enzyme formulation for dental calculus dissolution: 4-week randomized trial." BMC Oral Health, 2024.
Qureshi, Ambrina, et al. "Clinical efficacy of scaling and root planing with and without metronidazole on glycemic control: three-arm randomized controlled trial." BMC Oral Health, 2021.
Radini, Anita, et al. "Beyond food: The multiple pathways for inclusion of materials into ancient dental calculus." Archaeological and Anthropological Sciences, 2017.
Rohanizadeh, R., and R. Z. Legeros. "Ultrastructural study of calculus-enamel and calculus-root interfaces." Archives of Oral Biology, 2005.
Smiley, Christopher J., et al. "Evidence-based clinical practice guideline on the nonsurgical treatment of chronic periodontitis by means of scaling and root planing with or without adjuncts." Journal of the American Dental Association, 2015.
The Journal of Clinical Dentistry. "A Single-blind Randomized Controlled Clinical Trial of 5% Pyrophosphate Dentifrice." The Journal of Clinical Dentistry, 2025.
Tonetti, Maurizio S., et al. "Principles in the management of a periodontitis patient." Journal of Clinical Periodontology, 2015.
Warinner, Christina, et al. "Pathogens and host immunity in the ancient human oral cavity." Nature Genetics, 2014a.
Warinner, Christina, et al. "A robust framework for microbial archaeology." Annual Review of Genomics and Human Genetics, 2014b.
White, D. J. "Dental calculus: recent insights into occurrence, formation, prevention, removal and oral health effects of supragingival and subgingival deposits." European Journal of Oral Sciences, 1997.
World Health Organization. "Oral Health Fact Sheet." WHO, 2025.